If you’re managing diabetes, you may have heard your doctor mention “diabetic shoes”—but what exactly are they, and why do they matter so much? Unlike regular footwear marketed for comfort, diabetic shoes are medical-grade devices specifically engineered to protect your feet from severe complications like foot ulcers, infections, and even amputations. With around 15% of people with diabetes developing foot ulcers during their lifetime, these specialized shoes are not a luxury—they’re a vital part of preventive care.
Diabetic shoes—also known as therapeutic shoes, extra depth shoes, or informally as “sugar shoes”—are designed to combat two major diabetes-related threats: nerve damage (diabetic neuropathy) and poor blood circulation (peripheral artery disease, or PAD). Neuropathy dulls sensation in the feet, meaning blisters or pressure points from tight shoes can go unnoticed. Poor circulation slows healing, turning a small sore into a dangerous wound. Diabetic shoes break this cycle by eliminating friction, reducing pressure, and supporting healthy foot mechanics.
In this guide, you’ll discover the key design features that set diabetic shoes apart, who truly needs them, how to get them properly fitted, and how Medicare and insurance can help cover the cost. More importantly, you’ll understand how these shoes fit into a broader strategy to keep your feet safe, mobile, and healthy for years to come.
How Diabetes Damages Feet and Why Protection Is Critical

The Dangerous Combination of Neuropathy and Poor Circulation
Diabetes doesn’t just affect blood sugar—it can silently damage nerves and blood vessels, especially in the feet. Diabetic neuropathy causes numbness, tingling, or complete loss of sensation. That means you might not feel a pebble in your shoe, a blister forming, or even a deep cut. Meanwhile, peripheral artery disease (PAD) reduces blood flow to the extremities, making it harder for wounds to heal. When an unnoticed injury meets poor circulation, the result can be a chronic ulcer, serious infection, or worse—amputation.
In the U.S., over 100,000 diabetes-related amputations occur each year. Shockingly, 95% of these are preventable with proper foot care. Diabetic shoes are one of the most effective tools in this prevention strategy.
How Diabetic Shoes Prevent Complications
Think of diabetic shoes as protective armor for your feet—not treatment, but prevention. Just like wearing a seatbelt doesn’t stop car accidents but drastically reduces injury, diabetic shoes don’t cure neuropathy or PAD, but they shield your feet from harm during daily activities.
Research shows that properly fitted therapeutic footwear can reduce plantar pressure by up to 85% compared to regular shoes. A landmark study published in Diabetes Care (2013) found that custom diabetic footwear cuts ulcer recurrence by 50–70% when paired with daily foot checks. The International Working Group on the Diabetic Foot (IWGDF) now recommends these shoes as standard care for high-risk patients.
8 Must-Have Features of True Diabetic Shoes

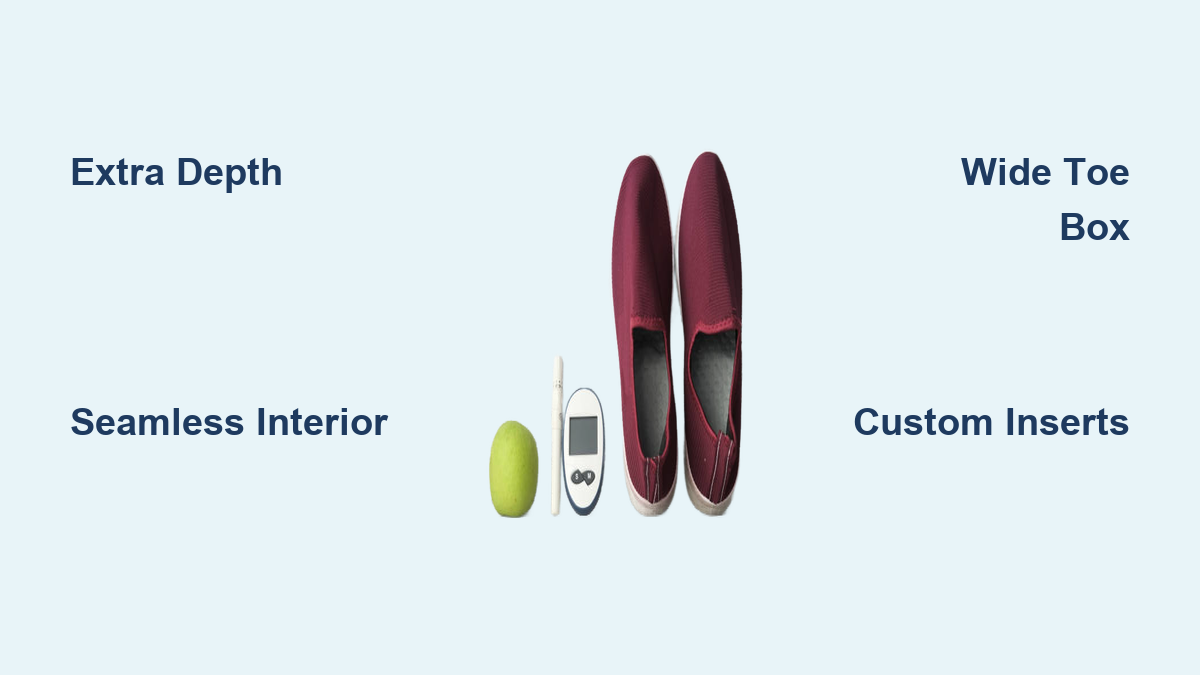
Extra Depth to Fit Medical Inserts
Diabetic shoes are built ¼ to ½ inch deeper than standard footwear to accommodate custom orthotics, AFO braces, or shoe lifts. This extra space prevents crowding and ensures your foot isn’t compressed by added inserts.
- Required for Medicare-covered shoes
- Essential for people with foot deformities or leg length differences
- Prevents new pressure points caused by ill-fitting insoles
Without this depth, even a supportive insert can cause more harm than good.
Seamless Interior to Prevent Blisters
Internal seams in regular shoes can rub against numb skin, causing friction wounds that go unnoticed. Diabetic shoes use soft, seamless linings made from microfiber or moisture-wicking fabric to eliminate this risk.
- Stops blisters before they start
- Protects insensate feet from microtrauma
- Reduces infection risk from broken skin
This feature is non-negotiable—any stitching inside the shoe increases the risk of ulcers.
Wide and High Toe Box for Natural Movement
A roomy toe box gives toes space to spread and move without being squeezed. This is crucial for people with bunions, hammertoes, or swelling.
- Prevents worsening of foot deformities
- Reduces callus and corn formation
- Distributes pressure evenly across the forefoot
Unlike fashion shoes that taper at the front, diabetic models maintain width from heel to toe.
Removable Insoles for Custom Orthotics
All diabetic shoes have removable insoles, allowing space for custom-molded orthotics. These are created using 3D scanning, foam casting, or pressure mapping to match your foot’s exact shape.
- Offloads pressure from high-risk zones (ball of foot, heel)
- Corrects gait imbalances
- Supports flat feet or collapsed arches
The insole is often the most critical component—without it, even the best shoe won’t provide full protection.
Cushioned, Supportive, and Non-Slip Soles
The soles are engineered to absorb shock, distribute weight, and prevent falls.
- Extra padding at pressure points (ball, heel)
- Arch support for flat feet
- Non-slip rubber outsoles for better traction
Many models include rocker-bottom soles that reduce push-off pressure—ideal for those with ulcers or stiffness.
Adjustable Closures for a Secure, Custom Fit
Diabetes can cause foot swelling, deformities, or limited hand strength, so diabetic shoes feature adjustable closures:
- Laces for precise fit control
- Velcro straps for easy on/off and swelling accommodation
- Elastic panels for flexible fit
- Hands-free entry (e.g., spring-loaded heels)
These allow daily customization, especially important for fluctuating foot size.
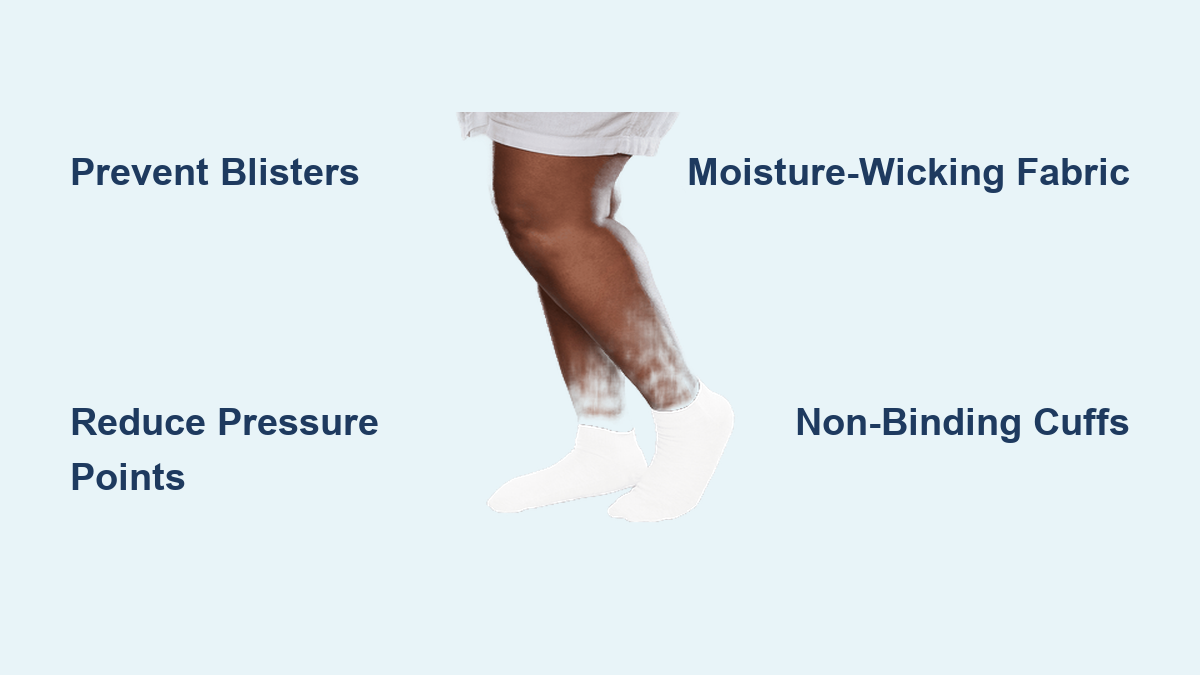
Breathable, Non-Binding Uppers
Diabetic shoes use soft, breathable materials like leather, mesh, or canvas to prevent moisture buildup and fungal infections.
- Avoids plastic or vinyl that traps sweat
- Stretches slightly to conform to foot shape
- Doesn’t constrict ankles or calves
Non-binding uppers prevent pressure on swollen legs and reduce skin breakdown.
Closed-Toe Design for Full Protection
All true diabetic shoes are closed-toe to shield feet from debris, temperature extremes, and injury.
- Even indoor diabetic slippers maintain closed structure
- Prevents cuts, burns, and puncture wounds
Open sandals or backless shoes offer no medical protection and are not considered therapeutic.
Who Really Needs Diabetic Shoes?
Medical Conditions That Require Therapeutic Footwear
Diabetic shoes are medically necessary for people with diabetes who have one or more of these conditions:
- Neuropathy (with or without calluses)
- History of foot ulcers or amputation
- Pre-ulcerative lesions
- Foot deformities (e.g., Charcot foot, bunions)
- Poor circulation (PAD)
- Swollen or fluctuating foot size
- Need for custom orthotics or braces
Even without current wounds, long-term diabetics or those with poor blood sugar control are high-risk and benefit from early use.
Who Else Can Benefit from Diabetic Shoes?
While designed for diabetics, these shoes help anyone with foot pain or instability:
- Plantar fasciitis sufferers
- People with metatarsalgia (ball-of-foot pain)
- Those with flat feet or bunions
- Post-surgical recovery patients
- Seniors with balance issues
Brands like Orthofeet, New Balance, and Propét offer styles that blend medical function with everyday appeal.
How to Get Diabetic Shoes Properly Fitted
Why Professional Fitting Is Essential
You can’t just buy diabetic shoes online and expect protection. Improper fit increases ulcer risk, even in therapeutic models. A certified fitter ensures the shoe and insert work together to offload pressure.
Who Can Fit Diabetic Shoes?
- Podiatrist
- Pedorthist
- Orthotist
- Certified therapeutic shoe fitter
Only prescriptions from a doctor (MD or DO) or podiatrist qualify for insurance coverage.
The Two-Appointment Fitting Process
-
Initial Assessment
– Foot exam (pulse check, monofilament testing)
– Gait analysis
– 3D scan or foam cast for custom inserts -
Final Fit Verification
– Try on shoes with inserts
– Pressure mapping to confirm offloading
– Adjustments made if needed
This process ensures the footwear is truly protective—not just comfortable.
Medicare and Insurance Coverage

Does Medicare Cover Diabetic Shoes?
Yes. Medicare Part B covers one pair of therapeutic shoes per year for eligible patients.
Eligibility Requirements:
You must have:
– A diabetes diagnosis
– AND at least one of:
– History of foot amputation
– Previous foot ulcer
– Pre-ulcerative callus
– Neuropathy with callus
– Foot deformity
– Poor circulation
Patients pay 20% coinsurance (typically $160–$280). Many Medigap plans cover this, making shoes free out-of-pocket.
What’s Covered Annually?
- 1 pair of extra-depth shoes
- 3 pairs of custom-molded inserts
—OR—
2 pairs of inserts + shoe modifications (e.g., rocker soles, heel wedges)
Shoes must be prescribed and fitted by approved professionals.
Real-World Benefits and Patient Outcomes
Patients consistently report life-changing results:
“After years of foot pain, these shoes changed my life. I can walk without fear.” — Donald R.
“Without my Orthofeet shoes, I wouldn’t be able to walk. Neuropathy and plantar fasciitis made every step agony.” — Manny K.
“Most comfortable shoes I’ve ever owned. I recommend them to everyone.” — Ellen D.
Common Misconceptions Debunked
| Misconception | Reality |
|---|---|
| “Any wide, comfortable shoe is good enough” | ❌ Lacks seamless lining, custom inserts, and pressure redistribution. Not clinically proven. |
| “I can buy diabetic shoes online without fitting” | ❌ Without custom molds and professional fitting, protection is compromised. |
| “Diabetic shoes cure neuropathy” | ❌ They are protective, not curative—like eyeglasses for your feet. |
| “Medicare covers all diabetics” | ❌ Only those with existing complications qualify. |
How to Maintain Your Diabetic Shoes
When to Replace Them
- Shoes: Annually (or when soles are worn, cushioning flattens)
- Inserts: Every 6–12 months, depending on weight and activity
Signs it’s time for new shoes:
– Flattened midsole
– Cracked or smooth outsole
– Inserts losing shape
– Shoes no longer feel supportive
Medicare allows one new pair per year—use it.
Daily Foot and Shoe Checks
- Inspect feet daily for redness, swelling, or wounds
- Check inside shoes for debris, rough spots, or moisture
- Never walk barefoot, even indoors
Even the best shoes can’t protect against neglect.
Final Note: Diabetic Shoes Are Medical Devices, Not Just Footwear
Diabetic shoes are life-preserving tools in diabetes care. Every 30 seconds, someone loses a limb to diabetes. But 95% of amputations are preventable with proper foot care.
These shoes work best as part of a full protection plan:
– Daily foot inspections
– Blood sugar control
– Seamless, moisture-wicking socks
– Regular podiatrist visits
– Never walking barefoot
When prescribed, properly fitted, and worn consistently, diabetic shoes help maintain mobility, independence, and quality of life. If you’re at risk, don’t wait for a wound to act—protect your feet now.