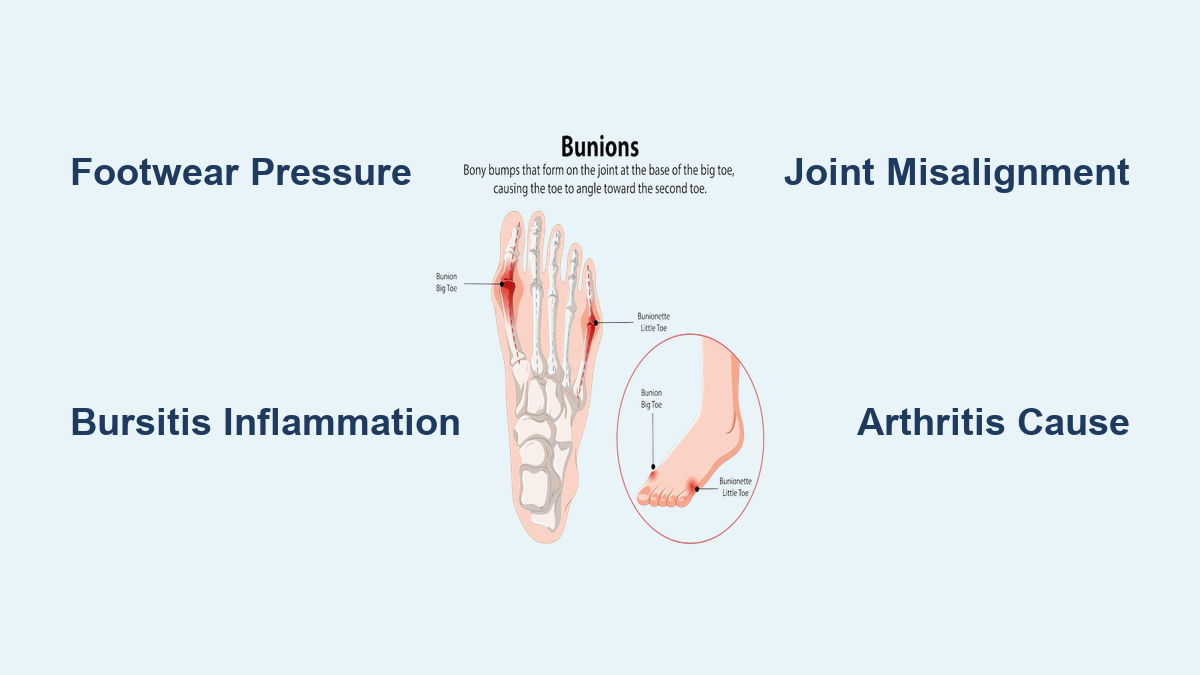
If you’ve noticed redness, warmth, or swelling around the base of your big toe, you’re likely dealing with more than just a bump — you’re experiencing active inflammation at the first metatarsophalangeal (MTP) joint, commonly known as a bunion. While many people view bunions as purely cosmetic, the redness and swelling that accompany them signal real tissue stress, irritation, or joint damage. These symptoms are not random; they stem from a mix of mechanical pressure, structural instability, and sometimes deeper systemic conditions.
Understanding what triggers redness and swelling is essential for effective management. Whether it’s from tight shoes rubbing against the joint, an inflamed bursa, or an underlying condition like arthritis, each factor activates your body’s inflammatory response. This article breaks down the primary causes, risk factors, and complicating conditions behind bunion-related inflammation—so you can identify the root of your discomfort and take targeted steps to reduce pain, prevent progression, and preserve foot function.
Mechanical Pressure from Footwear
Tight or poorly designed shoes are one of the fastest ways to trigger redness and swelling around a bunion.
How Shoes Irritate the Bunion Joint
Narrow toe boxes and high heels force the forefoot into a compressed space, pressing the bony prominence of the bunion directly against the shoe material. This constant friction and pressure irritate the skin and soft tissues, leading to:
- Localized redness and warmth
- Tenderness to touch
- Soft tissue swelling
- Calluses or blisters from repeated rubbing
High heels are especially problematic because they shift up to 75% of your body weight onto the ball of the foot, dramatically increasing load on the already compromised MTP joint. Even minor pressure, when repeated over time, can cause micro-inflammation that accumulates into visible swelling and chronic discomfort.
When Symptoms Flare
Redness and swelling often appear after:
– Wearing dress shoes or heels for several hours
– Standing or walking for extended periods
– Switching from barefoot activity to restrictive footwear
Pro tip: If your symptoms improve when barefoot or in wide-toe-box shoes, footwear is very likely a major contributor to your inflammation. Choosing supportive, low-heeled shoes with ample room in the toe box can provide immediate relief.
Bursitis: Inflamed Fluid Sac Over the Joint

Bursitis is a leading cause of sudden or persistent swelling and redness in bunion cases.
What Is Bursitis?
A bursa is a small, fluid-filled sac that cushions bones and tendons near joints. In bunions, the protruding metatarsal head creates constant pressure, causing the overlying bursa to become inflamed — a condition called bunion bursitis.
An inflamed bursa leads to:
– Puffy, red, warm swelling directly over the bunion
– Sharp or throbbing pain when pressed
– Tenderness that makes wearing any closed shoe unbearable
Unlike general soft tissue puffiness, bursitis often appears as a distinct, soft bulge rather than diffuse swelling, and it may feel warm to the touch.
Acute vs. Chronic Bursitis
| Type | Triggers | Symptoms |
|---|---|---|
| Acute | Sudden increase in activity, new shoes | Rapid onset, intense redness, warmth, pain |
| Chronic | Long-term shoe pressure | Persistent swelling, thickened tissue, recurrent flare-ups |
In rare cases, the bursa can become infected (septic bursitis), especially if there’s a cut, blister, or crack in the skin nearby. Signs include fever, pus, or redness spreading beyond the joint — all of which require urgent medical attention and possible antibiotic treatment.
Hallux Valgus: Joint Misalignment and Deformity

The structural root of all bunion-related inflammation is hallux valgus — a progressive deformity where the big toe angles inward and the first metatarsal drifts outward.
How Deformity Causes Inflammation
As the MTP joint shifts out of alignment:
– A bony prominence forms on the side of the foot
– The joint capsule and ligaments stretch and inflame
– Synovitis (inflammation of the joint lining) develops
– Abnormal motion causes microtrauma with every step
This creates a self-perpetuating cycle: the larger the bunion, the more it sticks out, the more it gets rubbed and irritated — leading to worsening redness and swelling.
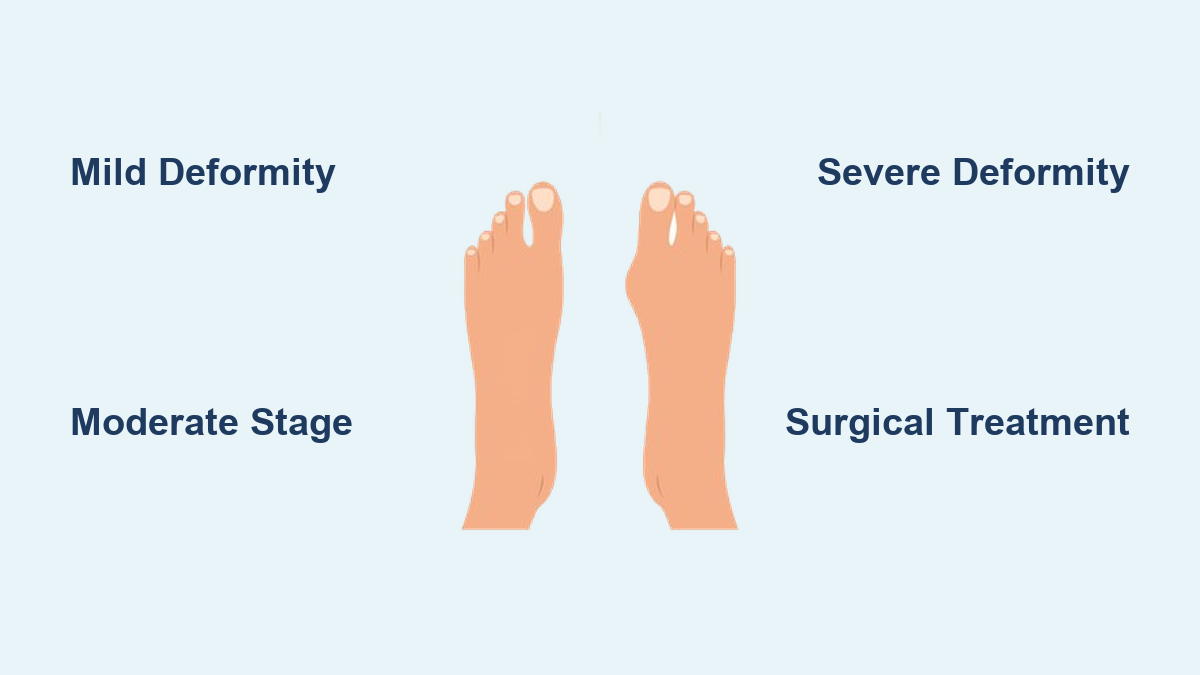
Signs of Progressive Joint Damage
Watch for:
– Increasing bump size over time
– Pain even without shoes
– Joint stiffness or crunching (crepitus)
– Difficulty finding comfortable footwear
Weight-bearing X-rays can confirm the degree of misalignment and help determine whether conservative care or surgical correction is needed.
Genetic and Hereditary Risk Factors
You may be more prone to bunion inflammation simply due to your genes.
Inherited Foot Structure
Over 70% of people with bunions have a family history of the condition. Common inherited traits include:
- Flat feet (pes planus) – leads to overpronation and forefoot instability
- Ligamentous laxity – allows excessive joint motion
- Metatarsus primus varus – abnormal inward alignment of the first metatarsal
These structural issues increase mechanical stress on the MTP joint, making it more likely to deform and inflame.
Why Some People Develop Symptoms Earlier
Even with similar footwear habits, genetically predisposed individuals may:
– Develop bunions in their 20s or 30s
– Experience swelling with minimal shoe pressure
– Have faster progression of deformity
If your parent or sibling has painful bunions, you’re at higher risk — and should consider preventive measures like proper footwear and foot strengthening exercises early.
Hormonal Influences on Joint Stability

Women are up to 10 times more likely than men to develop bunions and related inflammation — and hormones may be why.
Estrogen and Ligament Laxity
Higher estrogen levels, especially during reproductive years or pregnancy, can:
– Loosen ligaments in the feet
– Reduce stability of the MTP joint
– Allow greater deviation of the big toe
This increased joint mobility, combined with wearing heels or narrow shoes, creates a perfect storm for bunion formation and flare-ups.
Pregnancy-Related Swelling
During pregnancy, hormonal changes and fluid retention can cause:
– Temporary increase in bunion redness and swelling
– Worsening discomfort, even in mild bunions
– Need for wider, supportive footwear
Symptoms may improve postpartum, but structural changes often remain and can accelerate long-term progression.
Underlying Arthritic Conditions
Redness and swelling around the bunion joint aren’t always due to mechanical irritation — sometimes, an underlying arthritis is to blame.
Rheumatoid Arthritis (RA)
RA is an autoimmune disease that attacks joint linings. It can:
– Mimic or accelerate bunion deformity
– Cause symmetrical swelling in both feet
– Lead to severe pain, warmth, and stiffness, especially in the morning
Unlike mechanical bunion pain, RA-related inflammation often improves with activity.
Osteoarthritis (OA)
Long-standing bunions can lead to secondary OA from cartilage wear. This causes:
– Joint stiffness
– Bone spurs
– Grating sensation during movement
OA-related swelling tends to be chronic and worsens with use.
Gout Attacks
Gout commonly affects the first MTP joint and can be mistaken for a bunion flare.
Gout symptoms include:
– Sudden, intense pain (often at night)
– Bright red, hot, swollen joint
– Extreme tenderness—even bed sheets hurt
A blood test for uric acid and joint fluid analysis can confirm gout.
Foot Injuries and Repetitive Stress
Trauma or overuse can initiate or worsen bunion inflammation.
Acute Injuries
Sprains, fractures, or stubbing the big toe can:
– Disrupt joint alignment
– Trigger inflammation in the MTP joint
– Accelerate bunion development
Even after healing, the joint may remain unstable and prone to swelling.
Chronic Overuse
Activities that overload the forefoot increase risk, including:
– Running or jumping sports
– Dancing (especially ballet)
– Jobs requiring long hours on your feet
This repetitive stress leads to microtrauma, which fuels chronic inflammation and tissue breakdown.
Secondary Complications That Worsen Swelling
Redness and swelling aren’t always from the bunion itself — secondary issues can amplify inflammation.
Hammertoes
As the big toe shifts toward the smaller toes, it can push the second toe into a bent position (hammertoe). This:
– Alters weight distribution
– Increases pressure on the bunion
– Creates friction points that inflame surrounding tissue
Calluses and Corns
Chronic rubbing between toes or against shoes leads to thickened skin (hyperkeratosis). These areas:
– Become painful and inflamed
– Trap heat and moisture, increasing redness
– May break down into ulcers in severe cases
Altered Gait and Forefoot Overload
To avoid bunion pain, you might unconsciously shift your weight to the outer foot or ball of the foot. This antalgic gait leads to:
– Increased pressure on the MTP joint
– Development of metatarsalgia
– Secondary inflammation and swelling
Over time, this can affect knees, hips, and lower back.
How Doctors Diagnose the Cause of Swelling
Not all redness and swelling are the same. A proper diagnosis ensures you get the right treatment.
Physical Examination
Your doctor will look for:
– Redness, warmth, swelling over the joint
– Skin changes (calluses, blisters, ulcers)
– Joint tenderness and bursal thickening
– Range of motion and stability
They may also check for nerve symptoms like numbness or burning.
Imaging Tests
Weight-bearing X-rays are essential to:
– Measure the hallux valgus angle
– Assess joint alignment and arthritis
– Rule out fractures or bone spurs
X-rays help determine if surgery is needed or if conservative care can help.
Blood Tests
If arthritis is suspected, your doctor may order:
– Rheumatoid factor (RF), ESR, CRP – for RA
– Serum uric acid – for gout
These are especially important if swelling is sudden, severe, or not clearly linked to shoe wear.
Prevention and Early Intervention
You can reduce redness and swelling by addressing the causes early.
Wear Proper Footwear
- Choose wide-toe-box shoes with low heels
- Avoid pointed or rigid styles
- Use cushioned insoles or orthotics for support
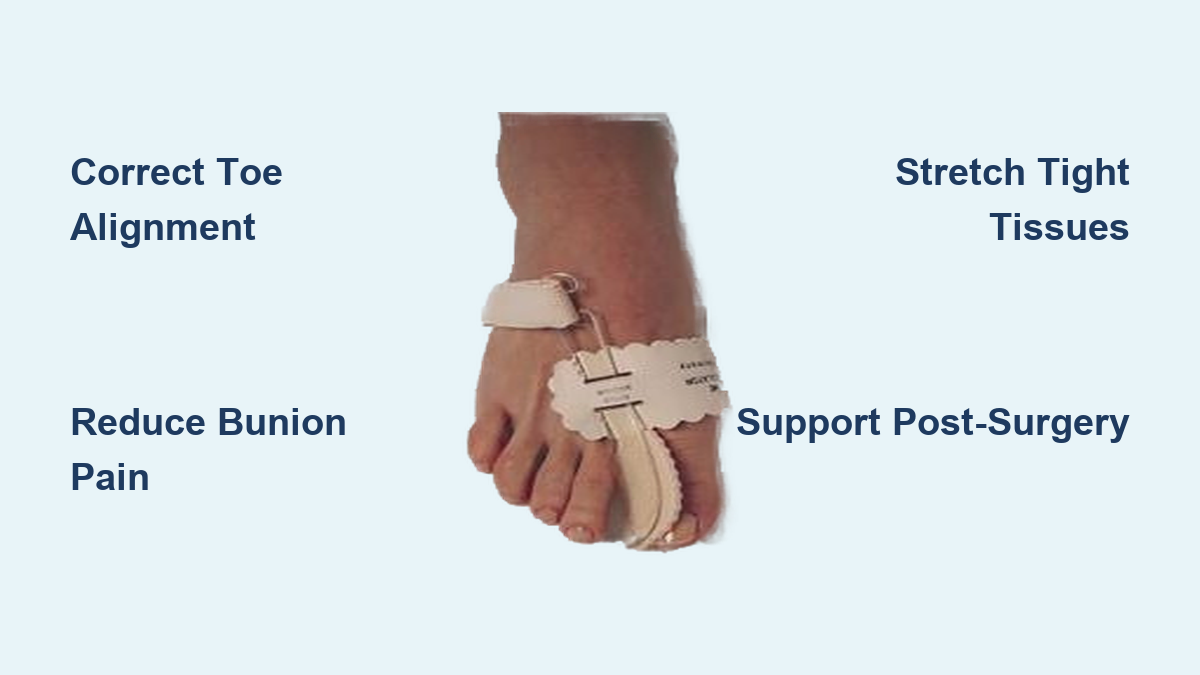
Use Protective Padding
- Apply bunion sleeves or gel pads to reduce friction
- Try moleskin or felt pads to offload pressure
Modify Activity
- Limit time in high heels or tight shoes
- Take breaks during prolonged standing
- Ice the area after activity to reduce swelling
When to See a Doctor
Seek professional help if you have:
– Swelling that doesn’t improve with rest or shoe changes
– Severe pain or redness that wakes you at night
– Signs of infection (fever, pus, spreading redness)
– Difficulty walking or wearing any shoes
Treatment options include:
– Custom orthotics to correct biomechanics
– Anti-inflammatory medications (oral or injected)
– Bursal aspiration for severe swelling
– Surgery for advanced deformity
Final Note: Redness and swelling around the bunion joint are not just cosmetic — they’re signs of active inflammation and tissue stress. The causes are multifactorial, ranging from shoe pressure and bursitis to genetic predisposition and arthritis. By identifying the specific triggers behind your symptoms, you can take targeted steps to reduce swelling, prevent progression, and preserve foot function. Early intervention is key: don’t ignore persistent redness — it’s your body’s way of asking for help.