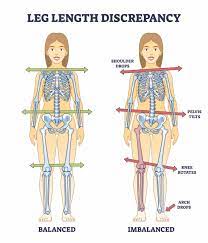
If you’ve been struggling with unexplained back pain, hip soreness, or a persistent limp, the root cause might not be where you think. A hidden imbalance—leg length discrepancy (LLD)—affects over 90% of people to some degree. While many live with minor differences without symptoms, even a 3 mm variation between legs can trigger postural shifts, joint stress, and long-term wear on your spine and lower limbs. The solution? Often starts with a simple, non-invasive tool: the heel lift.
A heel lift is an orthopedic insert placed under the heel of the shorter leg to restore balance, improve alignment, and reduce pain caused by biomechanical asymmetry. By elevating the shorter side, it levels the pelvis, corrects spinal curvature, and promotes even weight distribution across the hips, knees, and feet. Whether your LLD stems from childhood injury, joint replacement surgery, or muscle imbalances, untreated discrepancies can lead to chronic pain, gait abnormalities, and early joint degeneration. This guide breaks down how heel lifts work, who needs them, and how to use them safely and effectively as part of a comprehensive treatment strategy.
Structural vs Functional Leg Length Discrepancy: Know the Difference

Understanding the Two Main Types of LLD
Leg length discrepancy falls into two distinct categories: structural and functional—and identifying which type you have is crucial to effective treatment.
Structural LLD means there’s an actual anatomical difference in bone length, usually in the femur or tibia. Causes include congenital conditions, childhood fractures that healed improperly, or joint surgeries like hip or knee replacements. Research shows up to 83% of knee replacements result in measurable leg length changes. Because this is a physical shortening, it requires mechanical correction—typically through a heel lift.
Functional LLD, on the other hand, occurs when bones are equal in length but posture, muscle tightness, or joint restrictions create the appearance of a short leg. Common triggers include tight hip flexors, weak gluteus medius, pelvic tilt, scoliosis, or excessive foot pronation. Unlike structural LLD, this type often improves with stretching, manual therapy, and gait retraining. However, a heel lift may still be used temporarily while the underlying imbalance is corrected.
Signs You Might Have Leg Length Discrepancy
Don’t ignore subtle clues. Watch for uneven shoe wear, a noticeable limp, one shoulder sitting lower than the other, or hip hiking—where you lift one hip while walking to compensate. You may also experience one-sided back pain, knee discomfort, or fatigue during walking. If you’ve had hip or knee surgery, post-op LLD is surprisingly common and should be evaluated. Left unchecked, even a small discrepancy can accelerate joint degeneration and lead to conditions like osteoarthritis or chronic muscle strain.
How Heel Lifts Restore Posture and Reduce Pain

Correcting Pelvic Tilt and Spinal Misalignment
At the heart of LLD-related pain is pelvic tilt. When one leg is shorter, the pelvis drops on that side, forcing the spine to curve sideways in a compensatory scoliosis. This misalignment increases pressure on spinal discs and facet joints, especially in the lower back. Studies show that a 6 mm discrepancy can alter lumbar lordosis, while a 9 mm difference affects facet joint angles. A heel lift counters this by elevating the shorter leg, leveling the pelvis, and reducing the need for spinal compensation. The result? A more neutral spine, reduced disc stress, and relief for overworked muscles like the quadratus lumborum and piriformis.
Preventing Joint Overload and Muscle Strain
Without correction, LLD leads to asymmetric weight distribution, placing excessive force on the longer leg. The hip, knee, and ankle on that side endure higher compressive loads, increasing the risk of osteoarthritis, particularly in the knee’s inner compartment. Meanwhile, the foot on the shorter side may overpronate to touch the ground, contributing to plantar fasciitis or metatarsalgia. A properly fitted heel lift helps distribute weight evenly, reduces joint stress, and allows overstretched muscles to return to their optimal length and function.
Choosing the Right Heel Lift: Material, Fit, and Type

Comparing Heel Lift Materials and Firmness
Heel lifts come in several materials, each with unique benefits:
- EVA foam: Lightweight and cushioned, ideal for daily wear and mild discrepancies (up to 6 mm). May compress over time.
- Rubber: Durable and firm, excellent for active users or lifts over 6 mm.
- Silicone or gel: Soft and conforming, reduces pressure—great for sensitive or diabetic feet.
- Cork: Naturally moldable and stable, often used in custom orthotics for long-term support.
Firmness is measured on the Shore A durometer scale (0 = soft, 100 = hard). Softer lifts (30–50 Shore A) offer comfort; firmer ones (60–80 Shore A) provide better biomechanical control.
Custom vs Off-the-Shelf Heel Lifts
Off-the-shelf lifts are affordable and available in standard heights (3 mm, 6 mm, 9 mm). They work well for mild, stable discrepancies but may not fit all shoes or address additional foot issues.
Custom orthotics with built-in lifts are molded to your foot and can combine heel elevation with arch support or metatarsal padding. These are ideal for moderate to severe LLD, athletes, or those with complex biomechanics. Though more expensive, they offer precision and better long-term outcomes.
Proper Fitting and Gradual Use: Avoid Common Mistakes
Determining the Correct Lift Height
Accurate measurement is non-negotiable. X-ray imaging is the gold standard for structural LLD, while block testing helps assess functional imbalances. Once the discrepancy is known:
- Start with half the measured difference for long-standing cases. For example, a 12 mm short leg begins with a 6 mm lift.
- For recent-onset LLD (e.g., after surgery), full correction may be appropriate immediately.
- Adjust based on comfort—1–2 mm changes can make a real difference.
Never guess the height. Self-prescribed lifts can worsen pain or create new imbalances.
Gradual Adaptation Protocol
Your body needs time to adjust. Follow this step-by-step approach:
- Increase lift height by 2–3 mm per week.
- Use adjustable heel lifts (like Clearly Adjustable) for fine-tuning.
- Monitor for discomfort, new pain, or gait changes.
This slow progression allows muscles, ligaments, and joints to adapt without strain.
When In-Shoe Lifts Aren’t Enough: External Shoe Modifications
Limits of Internal Heel Lifts
Most shoes can fit up to 10–12 mm (about 1/2 inch) of internal lift. Beyond that, you risk foot slippage, poor fit, instability, and altered mechanics. Narrow shoes, dress footwear, or high heels offer even less space.
External Sole Build-Ups for Larger Discrepancies
For discrepancies over 12 mm, external modifications are essential. A cobbler can build up the sole and heel of the shoe on the shorter side. Full-foot lifts raise the entire shoe, preserving natural foot posture. These are durable, stable, and discreet under clothing. Combining a moderate in-shoe lift (6–8 mm) with an external build-up allows for greater correction without sacrificing comfort.
Maximizing Results: Integrate Heel Lifts Into a Full Treatment Plan
Wear Lifts in All Shoes for Consistent Correction
Using a heel lift only in your running shoes or work boots creates intermittent correction, confusing your neuromuscular system. Apply the same elevation across all footwear—athletic shoes, dress shoes, slippers, and even sandals if possible. Use low-profile lifts for shallow shoes and consider multiple pairs tailored to different footwear. Skipping correction at home undermines progress made elsewhere.
Combine With Therapy and Exercise
Heel lifts are not a standalone fix—they work best alongside:
- Manual therapy: Chiropractic adjustments, soft tissue release, and joint mobilization to correct pelvic tilt.
- Stretching: Target tight hip flexors, hamstrings, and calf muscles.
- Strengthening: Focus on gluteus medius, core stabilizers, and foot intrinsics.
- Gait retraining: Learn to walk symmetrically to reinforce proper mechanics.
This integrated approach addresses both the structural imbalance and the functional adaptations that have developed over time.
Avoiding Risks: Common Errors and How to Prevent Them
Key Mistakes That Can Worsen Your Condition
Improper use of heel lifts can backfire. Avoid these pitfalls:
- Starting too high: Jumping to full correction causes muscle strain and joint pain.
- Using lifts in both shoes: Only the shorter leg should be elevated unless directed otherwise.
- Ignoring symptoms: New or worsening pain means the lift may be too high or poorly fitted.
- Poor shoe fit: Wearing lifts in tight or narrow shoes leads to instability and discomfort.
Always follow professional guidance—never “tough it out.”
Monitoring for Adverse Effects
Watch for:
– Skin irritation or pressure sores
– Foot slippage inside the shoe
– Balance issues or coordination changes
– Increased back or knee pain
If any occur, remove the lift and consult your provider. Regular check-ins ensure your treatment stays on track.
Evidence-Based Benefits and Long-Term Value
Proven Improvements in Pain and Function
Research confirms heel lifts improve outcomes for LLD-related conditions:
- Low back pain: Reduced intensity and disability (measured via VAS and Oswestry scores)
- Knee osteoarthritis: Less medial compartment loading and pain (WOMAC, KOOS)
- Hip and foot pain: Improved joint mechanics and gait symmetry
- Plantar fasciitis: Reduced strain due to normalized foot strike
Patients report higher quality of life (SF-36) and greater satisfaction (QUEST scale) with properly prescribed lifts.
Preventing Long-Term Damage
Beyond pain relief, heel lifts help prevent secondary conditions:
- Slows joint degeneration
- Reduces risk of stress fractures
- Prevents chronic muscle imbalances
- Minimizes progression of scoliosis
For active individuals and athletes, early intervention preserves performance and joint health.
Final Note: Heel lifts are a simple, powerful solution for leg length discrepancy when used correctly. They restore alignment, reduce pain, and enhance mobility—but success depends on accurate diagnosis, proper fitting, and integration with other therapies. Always consult a qualified professional such as a podiatrist, physical therapist, or chiropractor. With the right approach, a small lift can make a big difference in your long-term musculoskeletal health.