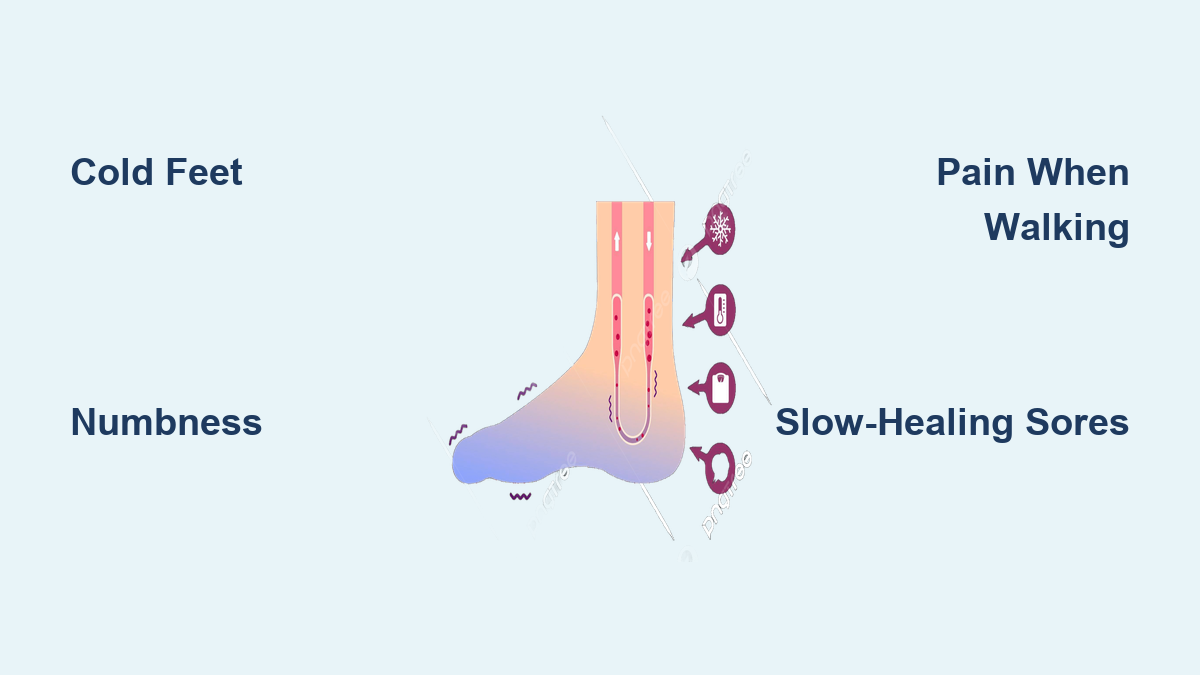
If your feet are always cold, tingle unexpectedly, or take forever to heal from minor scrapes, poor blood circulation could be the culprit. This condition occurs when blood flow to your lower limbs is restricted—often due to narrowed arteries, nerve damage, or chronic diseases like diabetes and peripheral artery disease (PAD). Because your feet are farthest from your heart, they’re usually the first to suffer when circulation falters.
Poor circulation isn’t a natural part of aging—it’s a warning sign of deeper health issues. Left unchecked, it can lead to chronic ulcers, severe infections, and even amputation, especially in people with diabetes. The good news? Recognizing the symptoms early can prevent complications and improve outcomes. In this guide, you’ll discover the most common signs of poor circulation in the feet, what’s causing them, when to seek help, and how to boost circulation through medical care and daily habits.
Cold and Discolored Feet
When blood flow drops, your feet lose warmth and may change color—two of the earliest and most noticeable signs of circulation problems.
Persistent Coldness in the Feet
Feeling cold in your feet—even indoors or during warm weather—is a classic red flag for poor circulation. With reduced blood flow, less warm, oxygen-rich blood reaches your toes and soles. You might notice one foot feels colder than the other, or that socks and blankets don’t help. This isn’t just uncomfortable—it means your tissues aren’t getting the oxygen they need to function properly.
Pro Tip: If you’re over 50, have diabetes, or smoke and experience persistently cold feet, talk to your doctor about an ankle-brachial index (ABI) test. It’s a simple, non-invasive way to check for PAD.
Skin Color Changes Due to Low Blood Flow
Poor circulation can cause visible shifts in skin tone:
– Pale or white skin: Often seen at rest, signaling low arterial inflow
– Bluish or purplish tint (cyanosis): Indicates oxygen-poor blood, commonly seen in venous insufficiency or severe PAD
– Redness when legs are lowered: Blood pools due to gravity, a sign of advanced arterial blockage
These color changes may come and go with position or temperature. For example, feet may turn bright red when dangled from the bed at night—a telltale sign of critical limb ischemia.
Numbness and Tingling in the Feet
Nerve damage from poor circulation or high blood sugar often leads to strange sensations in the feet.
“Pins and Needles” Sensation
A tingling feeling, often described as “pins and needles,” is common with poor circulation—especially in people with diabetic neuropathy. It typically starts in the toes and moves upward. Unlike temporary numbness from sitting too long, this sensation lingers and may worsen at night, disrupting sleep.
Warning: Persistent tingling can mask injuries. Without proper sensation, you might not notice a cut, blister, or splinter until it becomes infected.
Loss of Feeling in Feet and Toes
As circulation worsens, nerves become increasingly damaged. You may:
– No longer feel hot or cold
– Step on sharp objects without pain
– Accidentally burn your foot in a hot bath
This numbness significantly increases the risk of unnoticed injuries and foot ulcers—especially in people with diabetes, where even minor wounds can escalate quickly.
Pain When Walking or at Rest

Circulation problems often reveal themselves through pain linked to activity—or worse, pain that doesn’t go away.
Leg Cramps While Walking (Intermittent Claudication)
Pain in the calf, thigh, or hip that starts during walking and eases with rest is called intermittent claudication, a hallmark symptom of PAD. It happens because your leg muscles aren’t getting enough oxygen during exertion.
- Onset: After a predictable distance (e.g., one block)
- Relief: Within minutes of stopping
- Progression: Worsens over time if untreated
Expert Note: Claudication affects up to 10% of people over 70. It’s not “just aging”—it’s a vascular red flag that demands attention.
Foot Pain at Rest
In advanced cases, pain occurs even when you’re not moving, especially in the toes or ball of the foot. It’s often worse at night and may force you to hang your leg over the bed to ease discomfort.
This type of pain is serious. It signals critical limb ischemia—so little blood is reaching the foot that tissue damage or death is imminent.
Skin and Nail Changes from Poor Circulation

Poor blood flow doesn’t just affect internal function—it visibly alters your skin and nails.
Dry, Shiny, or Tight Skin
Reduced blood flow leads to:
– Shiny, tight skin with loss of normal texture
– Extreme dryness and cracking, especially around the heels
– Hair loss on toes and lower legs
These changes happen because skin cells aren’t receiving the nutrients and oxygen needed to regenerate.
Thick, Brittle, or Discolored Toenails
Toenails may become:
– Thick and hard to trim
– Yellow or misshapen
– Slow-growing
These symptoms can mimic fungal infections but are often caused by poor blood supply. Similarly, reduced leg hair growth is a subtle but reliable sign of arterial insufficiency.
Slow-Healing Wounds and Foot Ulcers

One of the most dangerous signs of poor circulation is the inability to heal from minor injuries.
Non-Healing Sores on the Feet
Cuts, blisters, or pressure sores that:
– Take weeks to heal
– Get bigger or deeper
– Drain fluid or pus
are serious warning signs. Poor circulation means fewer immune cells reach the wound, increasing infection risk.
Fact: Up to 25% of people with diabetes develop foot ulcers. Over 85% of lower-limb amputations start with an untreated ulcer.
Risk of Infection and Gangrene
Without adequate blood flow, even small wounds can turn into:
– Cellulitis (skin infection)
– Abscesses
– Gangrene (tissue death)
Gangrene appears as blackened, foul-smelling tissue and is a medical emergency requiring immediate treatment.
Swelling and Fluid Buildup in Feet
Swelling isn’t always due to poor arterial flow—it can also signal venous problems.
Pitting Edema in the Feet and Ankles
Press your finger into the swollen area. If an indentation remains, it’s pitting edema, a sign of fluid buildup from:
– Chronic venous insufficiency
– Heart failure
– Kidney or liver disease
Swelling often worsens after standing or sitting for long periods.
Aching, Heavy Legs
Many people describe their legs as feeling:
– Heavy
– Achy
– “Full” or tight
This discomfort improves with elevation and is common in venous disease, where damaged valves fail to return blood efficiently.
Weak or Absent Foot Pulses
A key diagnostic clue—your doctor will check this, but you can learn to monitor it too.
How to Check Pedal Pulses
The dorsalis pedis (on the top of the foot) and posterior tibial (behind the inner ankle) pulses should be strong and equal on both sides. If you can’t feel them, it may indicate significant arterial blockage.
Self-Check Tip: Use two fingers (not your thumb) to press gently on the top of your foot or behind the ankle. Compare both sides.
Why Pulse Strength Matters
Absent or weak pulses are a major red flag for PAD. When combined with symptoms like claudication or rest pain, they prompt immediate testing—like ABI or Doppler ultrasound.
Underlying Causes and Risk Factors
Poor circulation is rarely random. It’s usually driven by chronic conditions.
Peripheral Artery Disease (PAD)
PAD is the leading cause of poor foot circulation. It results from atherosclerosis—plaque buildup in leg arteries. Risk factors include:
– Smoking
– Diabetes
– High cholesterol
– Hypertension
– Age over 50
Did You Know? 8.5 million Americans have PAD, yet only 1 in 4 receive treatment.
Diabetes and Neuropathy
High blood sugar damages both nerves and blood vessels. Diabetic neuropathy reduces sensation, while vascular damage limits blood flow—creating a dangerous combo.
- Foot ulcers are 15x more likely in diabetics
- Amputation risk is 10–40x higher
Blood Clots and Raynaud’s Disease
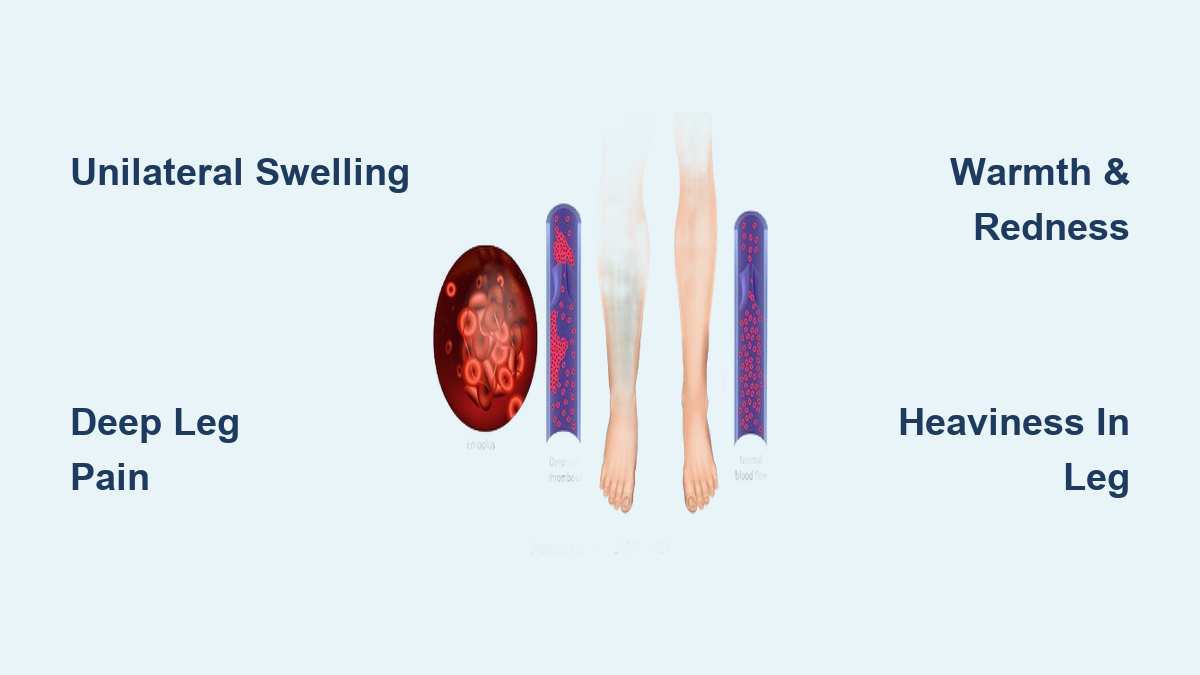
- Deep Vein Thrombosis (DVT): A leg clot causes sudden swelling, pain, and warmth. It can break off and cause a pulmonary embolism.
- Raynaud’s Disease: Cold or stress triggers artery spasms, turning toes white or blue. Episodes last minutes to hours.
When to See a Doctor
Don’t wait. Early diagnosis saves limbs and lives.
Schedule an Appointment If You Have:
- Cold, numb, or discolored feet lasting more than a few days
- Leg pain when walking
- Slow-healing cuts or sores
- Swelling in one or both legs
- Skin changes like shininess or hair loss
Your doctor may order an ABI test, Doppler ultrasound, or blood work to check for diabetes, cholesterol, or inflammation.
Seek Emergency Care for:
- Sudden, severe leg pain or swelling
- Blue or black toes
- No pulse in the foot
- Chest pain or trouble breathing (possible clot in lungs)
- Signs of stroke (facial droop, slurred speech)
These could indicate a life-threatening blockage or embolism.
Treatment and Management Options
The right treatment depends on the cause and severity.
Medications That Improve Circulation
- Statins: Lower cholesterol and stabilize plaque
- Aspirin or clopidogrel: Prevent blood clots
- ACE inhibitors: Improve blood vessel function
- Diabetes medications: Control blood sugar
Caution: Never start or stop blood thinners without medical advice.
Procedures for Severe Blockages
- Angioplasty and stenting: Opens narrowed arteries
- Bypass surgery: Reroutes blood around a blockage
- Atherectomy: Removes plaque from artery walls
These are used when symptoms are severe or ulcers aren’t healing.
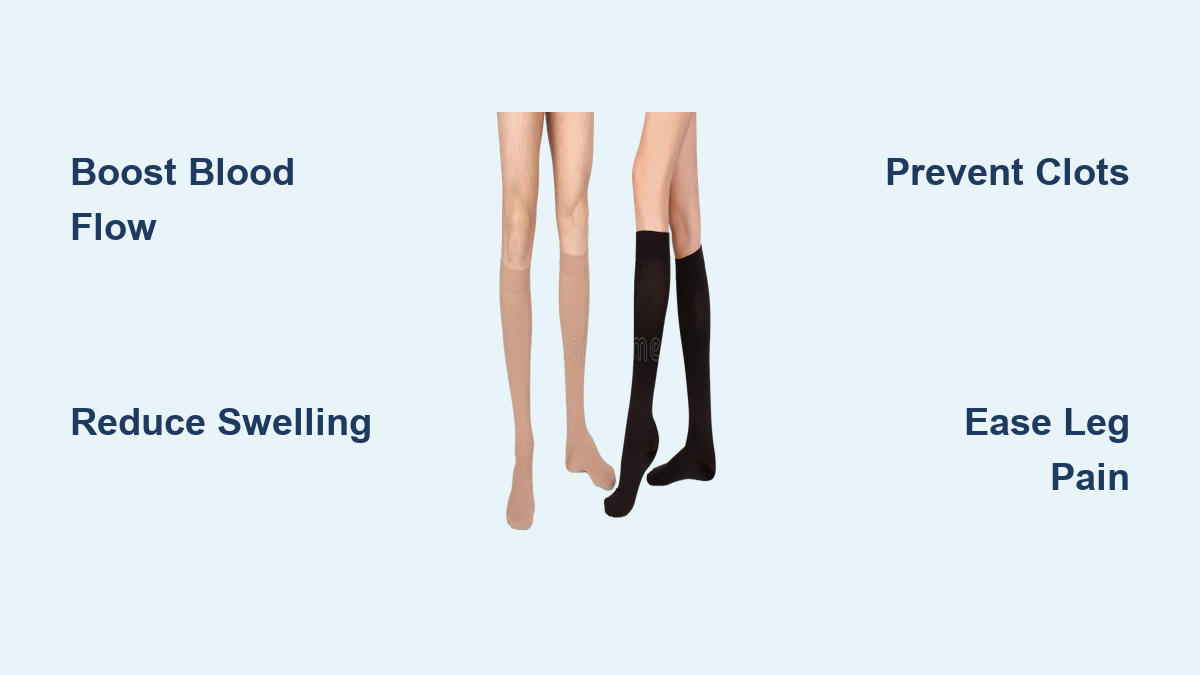
Lifestyle Changes That Improve Circulation
You have more control than you think.
Walk Regularly
Walking is the #1 recommended exercise for PAD. It promotes collateral circulation—natural bypass routes that improve blood flow.
- Goal: 30–60 minutes most days
- Start slow: Walk until pain begins, rest, then resume
- Supervised programs increase walking distance by 50–100%
Eat a Circulation-Friendly Diet
Focus on:
– Leafy greens (nitrates dilate blood vessels)
– Fatty fish (omega-3s reduce inflammation)
– Citrus fruits (flavonoids support vessel health)
– Nuts and seeds (vitamin E improves flow)
Avoid processed foods, excess salt, and sugary drinks.
Stop Smoking Immediately
Smoking is the most modifiable risk factor. It:
– Narrows blood vessels
– Damages artery linings
– Speeds up plaque buildup
Within weeks of quitting, circulation begins to improve.
Daily Foot Care Tips
Prevention is your best defense—especially if you have diabetes.
Inspect Feet Every Day
Check for:
– Cuts, blisters, redness
– Swelling or warmth
– Ingrown toenails
Use a mirror or ask for help—you might not feel injuries.
Moisturize and Protect
- Apply lotion to dry skin (not between toes)
- Trim nails straight across
- Wear cushioned, well-fitting shoes
- Avoid walking barefoot
Warning: Never use heating pads on numb feet—burns can occur without you feeling them.
Prevention and Long-Term Health
You can’t change your age—but you can control most risk factors.
Key Prevention Strategies
- Exercise 150 minutes/week
- Keep blood pressure under 130/80
- Maintain HbA1c <7% if diabetic
- Lower LDL cholesterol to <100 mg/dL
- Avoid alcohol excess and manage stress
Routine checkups with your doctor or podiatrist can catch problems early.
Final Note: Poor blood circulation in the feet is not something to ignore. From cold toes to non-healing wounds, the signs are clear—and treatable. By recognizing symptoms early, managing underlying conditions, and adopting healthy habits, you can protect your feet, your mobility, and your long-term health. If you’re at risk, start today: take a walk, check your feet, and talk to your doctor about your circulation.