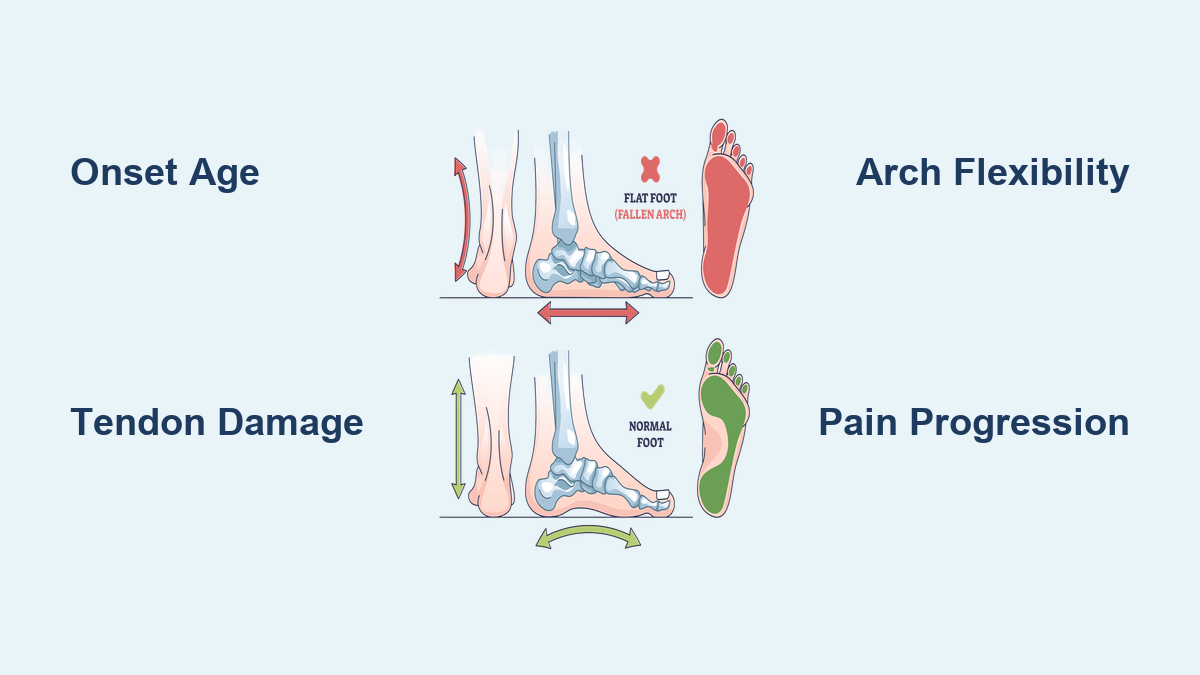
If you’ve ever looked down at your feet while standing and noticed that the arch seems to disappear—your entire sole pressing flat against the floor—you’re not alone. Millions of people live with flat feet, but what many don’t realize is that not all flat feet are the same. The difference between a fallen arch and naturally flat feet can mean the difference between needing no treatment at all and facing progressive foot collapse that may require surgery.
While both conditions result in a flattened appearance of the foot, they stem from entirely different causes. Naturally flat feet are typically a lifelong anatomical variation—something you’re born with or develop in childhood. In contrast, a fallen arch is a degenerative condition that develops later in life, often due to damage to a key tendon supporting the arch. Confusing one for the other can lead to delayed treatment—or unnecessary interventions.
Understanding this distinction is essential for proper diagnosis, effective treatment, and long-term foot health. This guide breaks down the critical differences between fallen arches and naturally flat feet, covering onset, causes, symptoms, diagnostic tests, and treatment options—so you can recognize which condition you may have and take the right steps toward relief and prevention.
Onset and Development: When It Starts Tells the Story
One of the most telling clues in identifying whether you have naturally flat feet or a fallen arch lies in when the flatness began.
Naturally Flat Feet: A Lifelong Foot Shape
Most people with naturally flat feet have had them since early childhood. It’s completely normal for infants and toddlers to appear flat-footed—their feet are cushioned with fat pads and their muscles and tendons haven’t fully developed. For many children, the medial longitudinal arch forms between ages 3 and 10 as the foot matures.
- Flexible flatfoot is the most common form in kids
- The arch becomes visible when sitting or standing on tiptoes
- Often resolves without intervention by adolescence
- If it persists into adulthood, it’s usually painless and stable
This condition, known medically as congenital pes planus, may be inherited or linked to loose ligaments. As long as the foot remains flexible and functional, it rarely causes problems—even elite athletes can perform at high levels with naturally flat feet.
Fallen Arches: A Change in Adulthood
A fallen arch, on the other hand, develops when a once-normal arch begins to collapse—typically after age 40. This is not a birth trait but an acquired deformity, often caused by weakening or tearing of the posterior tibial tendon.
- Usually starts in one foot before affecting both
- Marked by a noticeable change in foot shape over time
- Associated with aging, overuse, obesity, or injury
- Progresses if untreated, leading to increasing pain and instability
Signs include shoes feeling tighter, feet appearing wider, or ankles rolling inward more than before. If you once had an arch and now it’s gone, you likely have a fallen arch, not naturally flat feet.
Structural Cause: Anatomy vs Degeneration

The root cause separates these two conditions at a fundamental level.
Naturally Flat Feet: A Genetic or Developmental Trait
Naturally flat feet are primarily a structural variation, not a disease. The arch simply never fully forms due to:
- Family history of flat feet
- Ligamentous laxity (loose joints)
- Delayed maturation of foot bones and tendons
There’s no tendon failure. The foot functions differently but isn’t breaking down. Many individuals with naturally flat feet go their entire lives without pain or limitations.
Fallen Arches: Posterior Tibial Tendon Dysfunction (PTTD)
Fallen arches are most commonly caused by posterior tibial tendon dysfunction (PTTD)—a condition where the tendon that supports the arch becomes inflamed, stretched, or torn.
Contributing factors include:
– Overuse: Long periods of standing, walking, or running
– Obesity: Increases mechanical load on the tendon
– Diabetes or hypertension: Impairs blood flow and healing
– Rheumatoid arthritis: Causes inflammatory joint and tendon damage
– Pregnancy: Hormones like relaxin loosen ligaments
– Poor footwear: Lacking arch support, leading to chronic strain
As the tendon weakens, the arch drops, the heel tilts outward (heel valgus), and the forefoot drifts laterally. This alters your entire lower limb alignment and can lead to pain far beyond the foot.
Flexibility and Arch Behavior: How Your Foot Responds
How the arch behaves under different conditions is a key diagnostic clue.
Naturally Flat Feet: Often Flexible
In flexible flat feet:
– The arch collapses when standing but reappears when sitting or rising onto toes
– Joints move normally
– Typically causes no pain or only mild fatigue
This flexibility means the foot can still function well biomechanically. Most children outgrow this type, but some adults retain it without issues.
Rigid flat feet, though rare, show no arch in any position and may stem from tarsal coalition (abnormal bone fusion) or severe arthritis—often requiring imaging and possible surgery.
Fallen Arches: Start Flexible, May Become Rigid
Early-stage PTTD presents as a flexible flatfoot—the arch can still be manually corrected. But as the tendon deteriorates, the foot becomes stiff and fixed.
- Stage 1: Painful tendon, arch still present
- Stage 2: Arch collapses, deformity is flexible
- Stage 3: Joints stiffen, arthritis develops
- Stage 4: Ankle joint becomes involved
Once rigidity sets in, conservative treatments become less effective, and surgical correction may be necessary.
Key Diagnostic Tests: How Doctors Tell the Difference

Diagnosis goes beyond appearance—it involves functional testing and imaging.
Single-Limb Heel Rise Test
This critical test assesses posterior tibial tendon function:
– Stand on one foot and try to rise onto your toes
– Normal or naturally flat feet: Arch forms, heel turns inward
– Fallen arch (PTTD): Can’t rise, or heel stays neutral/tilted outward
Failure to complete this motion strongly suggests tendon damage.
Wet Foot Test
A simple at-home screening:
– Wet your soles and step on paper
– A full or nearly full footprint indicates flat feet
– Doesn’t distinguish cause—but confirms arch absence
Useful for parents monitoring children’s foot development.
Imaging for Confirmation
When symptoms suggest progression:
– Weight-bearing X-rays: Show bone alignment, heel valgus, joint degeneration
– MRI: Gold standard for detecting tendon tears or inflammation
– Ultrasound: Dynamic view of tendon during movement, detects partial tears
These tools help differentiate stable flat feet from progressive PTTD.
Symptoms: Pain Patterns Reveal the Truth
Both can cause discomfort—but the timing, location, and progression differ.
Naturally Flat Feet: Often Painless
Most people with naturally flat feet experience no symptoms. When pain occurs, it’s usually:
– Mild arch or heel fatigue after standing
– Occasional swelling after activity
– Improved with rest or supportive shoes
Children may complain of tired feet but often outgrow it.
Fallen Arches: Progressive and Debilitating
Symptoms develop gradually and worsen:
– Inner ankle pain along the posterior tibial tendon
– Swelling that increases with activity
– Difficulty standing on tiptoes
– Outer ankle pain (due to heel shift)
– Burning or sharp arch pain
– Foot widening—shoes feel tight
– Limping or instability
Pain often starts in one foot and spreads. Without treatment, daily activities become difficult.
Risk Factors: Who’s Most Affected?
Naturally Flat Feet
- Family history
- Connective tissue disorders (Ehlers-Danlos, Marfan)
- Neuromuscular conditions (cerebral palsy)
- Children with delayed motor milestones
Fallen Arches
- Age over 40
- Female gender (especially post-pregnancy)
- Obesity (BMI >30)
- Diabetes, hypertension, or arthritis
- History of ankle injuries
- Prolonged standing (e.g., teachers, nurses)
Over 80% of adult-acquired flatfoot cases are due to PTTD.
Treatment: Support vs Repair

Naturally Flat Feet: Supportive Care
Most need no treatment. If symptomatic:
– Custom orthotics for arch support
– Stable shoes with firm heel counters
– Stretching and strengthening exercises
– Activity modification during flare-ups
Surgery is rare and reserved for rigid, painful cases.
Fallen Arches: Early Intervention Is Critical
Goal: halt progression and preserve function.
Non-Surgical Options
- Walking boot or cast (6–8 weeks) to rest the tendon
- Custom orthotics with medial posting
- Physical therapy to strengthen the posterior tibial muscle
- NSAIDs and ice for pain and swelling
- Weight loss to reduce stress
Surgical Options (if conservative care fails)
- Tendon transfer (e.g., flexor digitorum longus)
- Osteotomy to realign the heel
- Lateral column lengthening
- Arthrodesis for rigid joints
Surgery is most successful when performed before joint damage occurs.
Prevention and Long-Term Foot Health
For Naturally Flat Feet
- Encourage barefoot play on varied surfaces in children
- Use supportive shoes only if pain occurs
- Avoid unnecessary orthotics in pain-free kids
For Preventing Fallen Arches
- Maintain a healthy weight
- Wear arch-supportive shoes daily
- Strengthen posterior tibial muscle:
- Heel raises (double-leg → single-leg)
- Towel scrunches
- Resistance band inversion exercises
- Stretch tight calves and Achilles regularly
- Replace worn-out shoes every 6–12 months
See a podiatrist at the first sign of inner ankle pain or difficulty on tiptoes.
Footwear and Orthotics: What Works Best
Look for:
– Firm heel counter
– Supportive midsole
– Removable insole
– Extra depth
– Stable outsole
Brands like Brooks, ASICS, New Balance, and Dansko offer excellent models.
Custom orthotics are often worth the investment—they correct overpronation, reduce tendon strain, and improve alignment from foot to back.
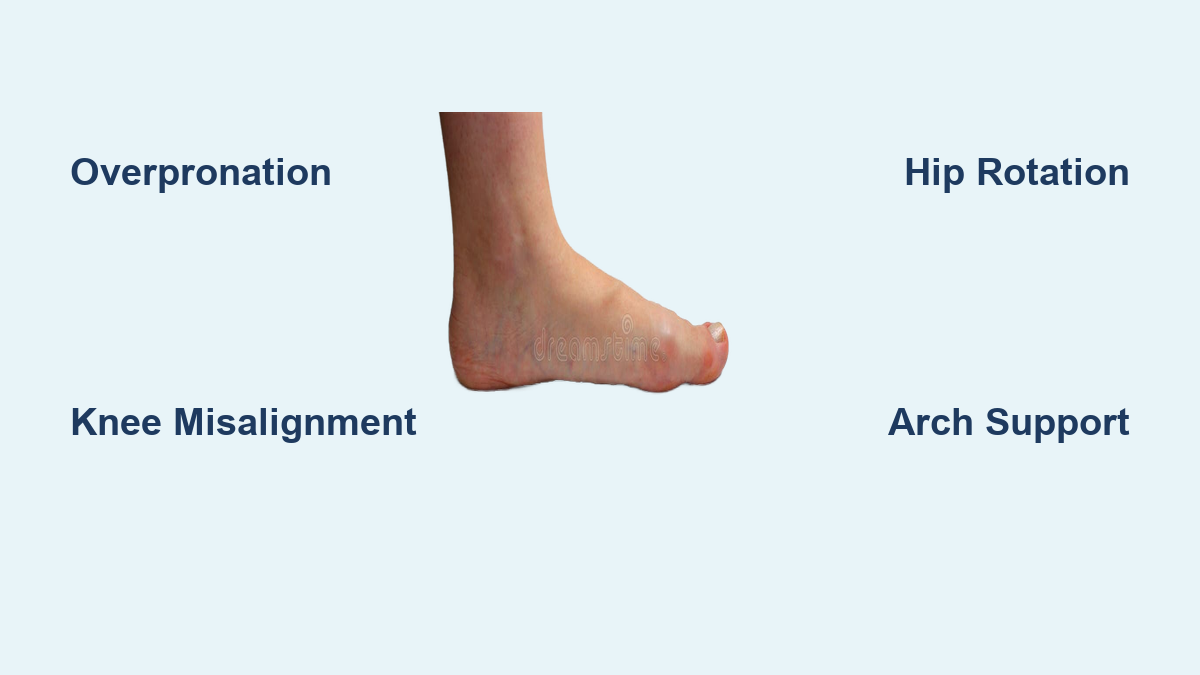
Impact on the Body: Beyond the Foot
Both conditions can cause overpronation, leading to:
– Knee pain (runner’s knee)
– IT band syndrome
– Hip pain
– Lower back pain
– Increased joint stress
Patients often seek help for knee or back pain—without realizing the root cause is their feet.
When to See a Podiatrist
Seek professional care if you notice:
– New arch or ankle pain
– Inability to rise onto your toes
– Foot shape changing (wider, flatter)
– Shoes wearing unevenly
– Pain that limits daily activities
Early diagnosis of fallen arches can prevent surgery. For naturally flat feet, a podiatrist can confirm stability and recommend support if needed.
Summary: Key Takeaways
| Factor | Naturally Flat Feet | Fallen Arches |
|---|---|---|
| Onset | Childhood | Adulthood (>40) |
| Cause | Genetic/anatomical | Tendon failure (PTTD) |
| Progression | Stable | Progressive |
| Pain | Often none or mild | Gradual, worsening |
| Flexibility | Arch returns off-weight | Starts flexible, may become rigid |
| Tendon Function | Normal | Impaired (fails heel rise test) |
| Treatment | Orthotics if symptomatic | Immobilization, PT, possible surgery |
| Prevention | Foot exercises, monitoring | Weight control, supportive shoes |
While both naturally flat feet and fallen arches result in a flat footprint, they are fundamentally different. One is a stable anatomical variation; the other is a degenerative process requiring action. Recognizing the difference empowers you to take the right steps—whether that’s wearing better shoes or seeking early treatment to prevent irreversible damage. Your feet carry you every day. Understanding what’s happening beneath them is the first step toward lasting comfort and mobility.