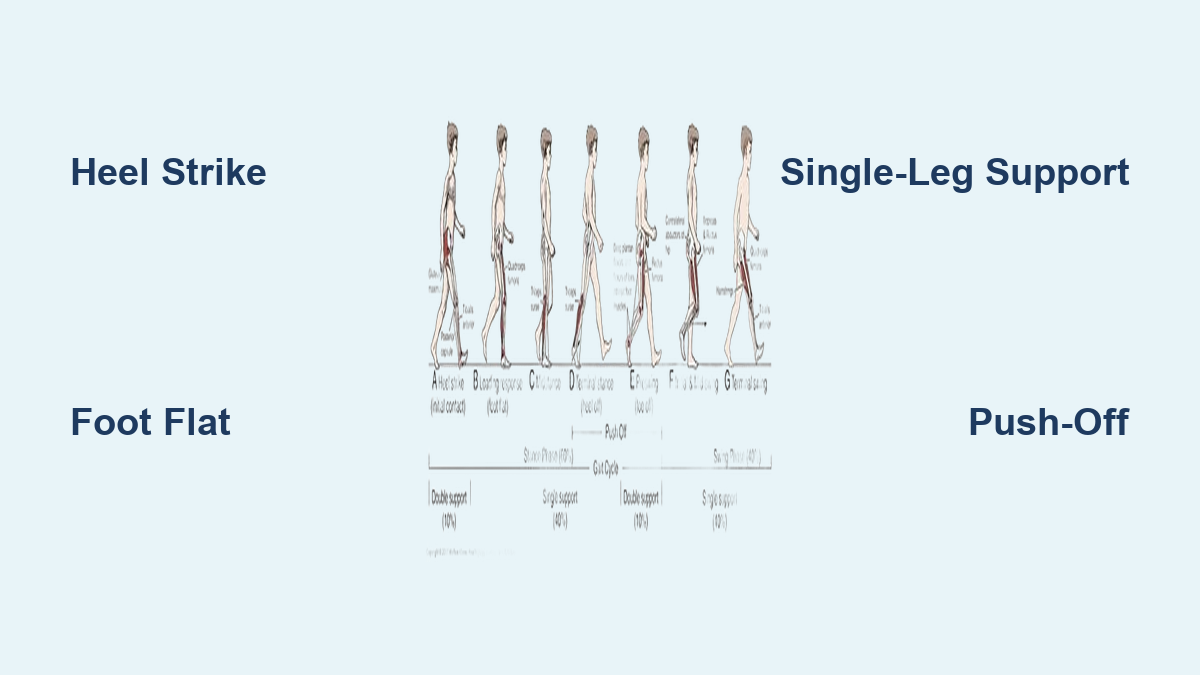
Walking may seem effortless, but behind every step is a highly coordinated sequence of movements known as the gait cycle—the complete motion from when one foot touches the ground to when that same foot strikes again. This cycle is essential for efficient, balanced, and energy-saving locomotion. At its core, the gait cycle is divided into two major phases: stance (when the foot is on the ground) and swing (when it’s in the air). However, to truly understand how we walk—and why problems arise—clinicians and biomechanists focus on four key functional phases: Initial Contact, Loading Response, Midstance, and Terminal Stance/Propulsion.
These four phases occur during the stance portion, which makes up about 60% of the gait cycle, and they handle the most critical tasks: absorbing impact, supporting body weight, maintaining balance, and generating forward movement. Whether you’re a physical therapist diagnosing an injury, a coach optimizing athletic performance, or someone recovering from surgery, knowing these phases helps identify inefficiencies, prevent falls, and restore natural movement.
Initial Contact (Heel Strike): The Moment Your Step Begins
The gait cycle starts with initial contact, commonly called heel strike, when the heel of the forward foot first touches the ground. This moment—just 0–3% into the cycle—sets the tone for everything that follows. It’s your body’s way of initiating forward motion while preparing to absorb the force of landing.
Why This Phase Matters
At heel strike, your body must immediately begin shock absorption. Even at a slow walk, ground reaction forces reach 1.2 times your body weight. Without proper control, this impact could travel up the leg, stressing joints and causing pain or injury.
- Ankle: Starts slightly dorsiflexed (toes up), then begins controlled plantarflexion to gently lower the foot.
- Knee: Bends slightly (5–10°) to act as a shock absorber.
- Hip: In slight extension, helping decelerate the swinging leg.
Key Muscles in Action
- Tibialis anterior: Works eccentrically (lengthens under tension) to prevent the foot from slapping down.
- Quadriceps: Stabilizes the knee to avoid buckling.
- Gluteus maximus: Slows the forward swing of the leg.
🔍 Visual cue: A normal gait shows the heel touching down first. If the whole foot or toes hit first, it may signal foot drop—a sign of nerve damage or neurological conditions like stroke.
Failure to control this phase results in foot slap, a telltale sign of weak dorsiflexors. Early intervention with strength training or ankle-foot orthoses (AFOs) can prevent long-term compensations.
Loading Response (Foot Flat): Accepting Your Full Weight

Right after heel strike (3–12% of the cycle), the foot rolls forward until the entire sole makes contact with the ground. This is the loading response, also known as foot flat, and it’s when your body begins shifting weight onto the stance leg.
Managing the Transition to Single-Leg Support
This brief phase is crucial for weight acceptance. Your leg transitions from double-leg support (briefly) to full single-limb loading. The knee flexes up to 15°, creating a “flexion wave” that helps dissipate impact forces.
- Ankle: Moves from plantarflexion to dorsiflexion—this is the ankle rocker in action.
- Knee: Flexes to absorb shock.
- Hip: Begins extending as the body moves forward.
Muscles That Keep You Stable
- Quadriceps: Eccentrically control knee flexion.
- Tibialis anterior and toe extensors: Continue lowering the foot smoothly.
- Gluteus medius and minimus: Fire to stabilize the pelvis and prevent the opposite hip from dropping.
⚠️ Red flag: A Trendelenburg sign—where the pelvis drops on the non-weight-bearing side—indicates weak hip abductors. This imbalance can lead to low back pain and inefficient walking.
Pain or stiffness in the knee, hip, or foot can shorten this phase, leading to an antalgic gait—a limp to avoid putting weight on the painful side.
Midstance: Balancing on One Leg
From 12% to 31% of the gait cycle, your body moves directly over the stance foot. This is midstance, the point of single-limb support, where 100% of your weight is balanced on one leg.
Stability Meets Forward Motion
During midstance, your foot transitions from a flexible shock absorber to a rigid lever, preparing for push-off. The center of mass passes over the foot, and the leg acts like a pillar supporting the trunk.
- Ankle: Progresses from dorsiflexion toward neutral.
- Knee: Fully extends.
- Hip: Reaches neutral and begins to extend.
Muscles That Maintain Balance
- Gluteus medius and minimus: Isometrically contract to keep the pelvis level.
- Soleus: Begins contracting to help propel the body forward.
- Tibialis anterior: Activity decreases as dorsiflexion demand drops.
💡 Pro tip: On uneven terrain, you’ll notice more ankle motion here—this is where balance training (like single-leg stands) makes a real difference.
Weakness in the gluteal muscles leads to Trendelenburg gait, where the trunk lurches over the stance leg to compensate. Over time, this alters spinal alignment and increases joint wear.
Terminal Stance (Heel-Off to Toe-Off): The Power Phase

From 31% to 50% of the cycle, your body enters terminal stance, also known as the propulsion phase. This is where forward drive happens—your heel lifts (heel-off), and your toes push off (toe-off) to launch you into the next step.
Generating Forward Momentum
This phase uses the forefoot rocker mechanism. As your body moves ahead of the foot, the forefoot acts as a pivot, and the calf muscles generate force for propulsion.
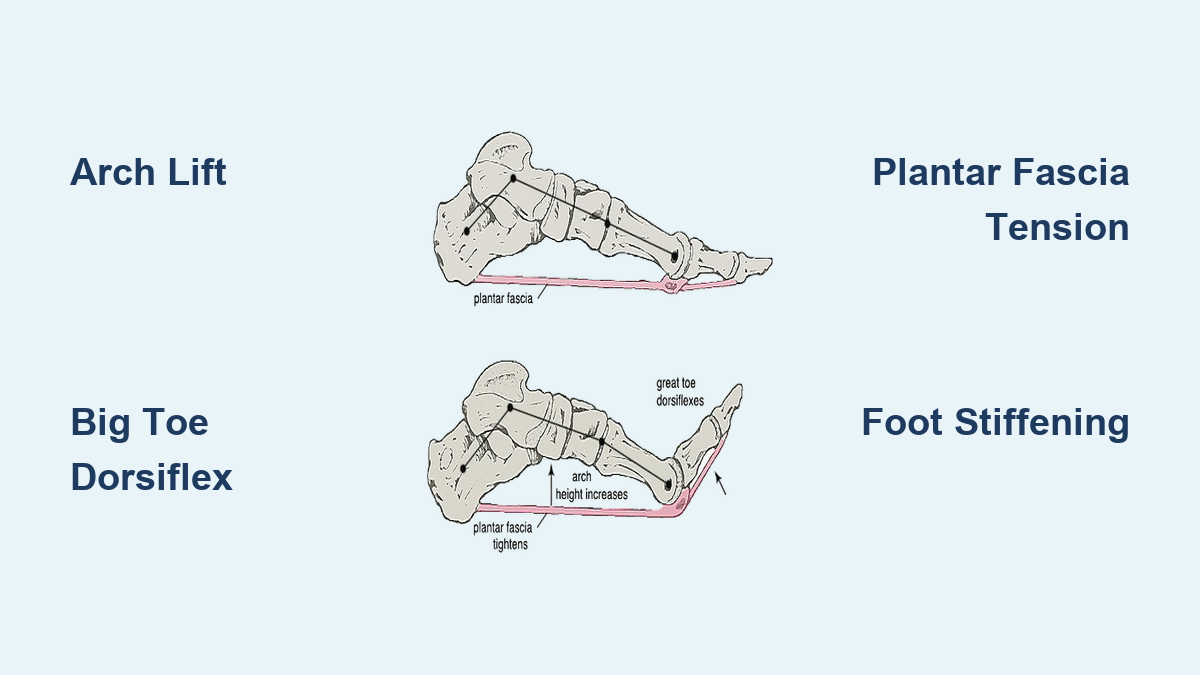
- Ankle: Strong plantarflexion via the windlass mechanism—tightening of the plantar fascia stiffens the arch for a rigid lever.
- Knee: Slight flexion as the body advances.
- Hip: Extends beyond neutral (hyperextension) to maximize forward reach.
Muscles That Drive You Forward
- Gastrocnemius and soleus: Concentric contraction powers push-off.
- Hamstrings and gluteus maximus: Aid hip extension.
🚨 Warning: Weak calf muscles or tight Achilles tendons reduce propulsion, leading to a shortened stride and slower walking speed.
Patients with diabetes, peripheral neuropathy, or post-stroke weakness often show reduced push-off, resulting in shuffling or reliance on arms for stability. Gait analysis can detect these issues early, allowing for interventions like strength training or orthotics.
Swing Phase: Preparing for the Next Step
Although not part of the “four phases,” the swing phase (40% of the cycle) completes the loop. It begins at toe-off and ends at the next heel strike, ensuring the leg swings forward safely and clears the ground.
Three Subphases of Smooth Advancement
Pre-Swing (50–62%)
- Heel lifts, knee flexes rapidly.
- Hamstrings control hip extension; tibialis anterior activates for dorsiflexion.
Initial Swing (62–75%)
- Leg accelerates forward.
- Hip flexes ~30°, knee ~60°.
- Ankle fully dorsiflexed to prevent toe drag.
❗ Risk: Foot drop—inability to lift the foot—causes tripping and high-stepping gait (steppage gait).
Terminal Swing (87–100%)
- Leg decelerates before heel strike.
- Knee extends; hip reaches peak flexion.
- Hamstrings eccentrically slow the limb.
A smooth swing phase ensures proper foot placement and rhythm. Neurological conditions like Parkinson’s or stroke often disrupt this timing, requiring gait retraining or assistive devices.
Whole-Body Coordination: It’s Not Just Your Legs
Walking is a full-body effort. While the legs do the work, other parts contribute to balance and efficiency:
- Pelvis: Rotates forward (~5°) with the swing leg, increasing step length.
- Spine and thorax: Rotate opposite the pelvis (~3–5°), counteracting twisting forces.
- Arms: Swing contralaterally (left arm with right leg), aiding rhythm and momentum.
- Trunk: Minimal side-to-side or up-down motion (~5 cm)—excess indicates instability.
Reduced arm swing, as seen in Parkinson’s disease, or trunk sway in older adults, signals impaired coordination and higher fall risk.
How Gait Analysis Reveals Hidden Problems

Gait analysis—the science of measuring walking patterns—helps detect abnormalities invisible to the naked eye. It’s used in clinics, rehab centers, and sports labs to guide treatment.
Common Assessment Tools
- Observational analysis: Trained eyes spot limping, asymmetry, or compensations.
- Motion capture: Reflective markers track joint angles.
- Force plates: Measure pressure and ground reaction forces.
- EMG: Records muscle timing.
- Wearable sensors: Track real-world movement.
Key Metrics Clinicians Watch
| Parameter | Normal Range | Why It Matters |
|---|---|---|
| Stance time | ~60% of cycle | Shortened? Could mean pain or weakness |
| Cadence | 100–120 steps/min | Slow? May indicate neurological issues |
| Walking speed | 1.2–1.4 m/s | Below 1.0? Higher fall risk |
| Step length | 70–80 cm (adults) | Short? Suggests weak propulsion |
| Double support time | 28–40% | Increases with age or instability |
Data is normalized to 0–100% of the cycle, allowing precise comparison. Advanced tools like Statistical Parametric Mapping (SPM) analyze full movement patterns, not just snapshots.
Common Gait Abnormalities and What They Mean
Even small disruptions alter your walk. Recognizing these patterns leads to faster diagnosis and better outcomes.
- Antalgic Gait: Limping due to pain—shortened stance on the painful side.
- Trendelenburg Gait: Weak hip abductors—pelvis drops on swing side.
- Foot Drop Gait: Nerve damage—high stepping to avoid toe drag.
- Hemiplegic Gait: Stroke—leg swings outward (circumduction).
- Parkinsonian Gait: Shuffling, small steps, reduced arm swing.
- Ataxic Gait: Cerebellar issues—wide base, staggering, poor coordination.
Each pattern points to a specific cause, guiding targeted rehab.
Final Note: Why the Four Phases Matter
The gait cycle’s four core phases—Initial Contact, Loading Response, Midstance, and Terminal Stance/Propulsion—form the foundation of efficient walking. They manage weight-bearing, balance, and power generation. While the swing phase completes the cycle, these stance-phase stages do the heavy lifting.
Understanding them allows you to:
– Diagnose musculoskeletal or neurological issues.
– Design effective rehabilitation programs.
– Improve athletic performance.
– Prevent falls in older adults.
✅ Takeaway: Efficient gait = stability + smooth transitions + strong propulsion. Monitor each phase, address weaknesses early, and keep moving safely.