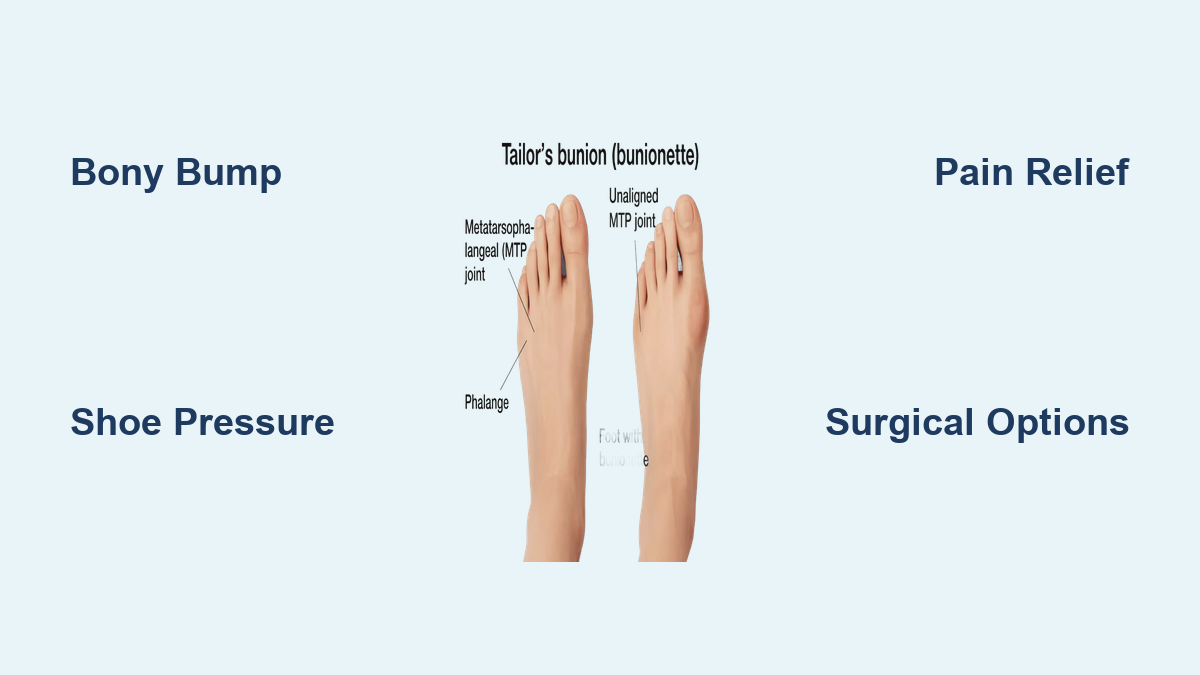
You slip on your favorite pair of shoes, take a few steps, and feel a sharp, persistent ache along the outer edge of your foot—right below your little toe. You glance down and notice a red, swollen bump forming where it never used to be. This could be a tailor’s bunion, also known as a bunionette, a common yet often overlooked foot condition that mirrors the more familiar bunion but develops on the opposite side of the foot.
A tailor’s bunion is a bony protrusion at the base of the little toe, specifically at the fifth metatarsophalangeal (MTP) joint. It occurs when the fifth metatarsal bone shifts outward or the little toe drifts inward, creating a prominent bump that becomes irritated by shoe pressure. While not dangerous, it can lead to chronic pain, skin irritation, and difficulty wearing everyday footwear. Without treatment, the deformity typically worsens over time.
In this guide, you’ll learn the causes, symptoms, and treatment options for a tailor’s bunion—both non-surgical and surgical. Whether you’re noticing early discomfort or struggling with persistent pain, understanding your condition is the first step toward lasting relief.
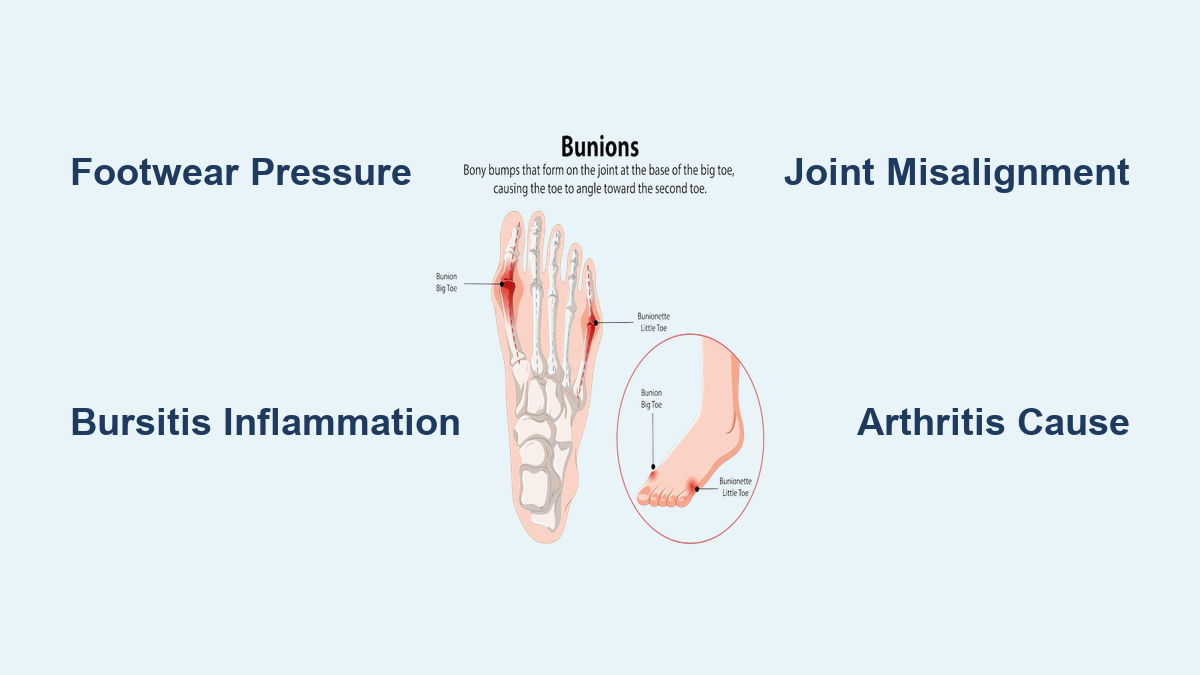
Fifth MTP Joint Misalignment Causes the Bump
The root of a tailor’s bunion lies in the structure and alignment of the outer foot, particularly at the fifth metatarsophalangeal joint.
How the Bony Prominence Forms
The fifth metatarsal is the long bone that connects your midfoot to your little toe. When this bone’s head shifts outward—often due to pressure or structural imbalance—it creates a visible bump on the outside of the foot. At the same time, the little toe may begin to drift inward toward the fourth toe, a condition called adductovarus deformity. This misalignment increases pressure on the joint, leading to inflammation, soft tissue irritation, and over time, bony remodeling.
Bony Enlargement vs. Exostosis: Two Types of Bunionettes
Not all tailor’s bunions are the same. Some result from general hypertrophy—a broad enlargement of the metatarsal head due to long-term stress. Others stem from a distinct bony spur (exostosis) growing off the side of the bone. X-rays are essential to determine which type you have, as this affects treatment options. An exostosis may be removed more easily, while angular deformities often require bone realignment.
Why Do Tailor’s Bunions Develop?

Tailor’s bunions don’t appear overnight. They’re usually the result of a mix of genetic, mechanical, and lifestyle factors that gradually alter foot structure.
Genetics and Inherited Foot Shape
Over 70% of people with bunionettes have a family history of foot deformities. Inherited traits like a wide forefoot (splayfoot), flat feet (pes planus), or high arches (pes cavus) change how weight is distributed across the foot. A longer fifth metatarsal compared to the fourth increases pressure on the outer edge, making you more prone to developing a bunionette.
Shoes That Worsen or Trigger the Condition
Tight, narrow, or high-heeled shoes are among the biggest external triggers. Pointed toes squeeze the forefoot, forcing the little toe inward and pushing the metatarsal head outward. Heels over 2 inches shift your body weight forward, intensifying pressure on the ball of the foot. This constant friction irritates the joint, leading to inflammation and eventual bony changes—especially if worn daily.
Biomechanical Stress and Gait Problems
Abnormal foot mechanics—like excessive pronation (rolling inward)—can overload the lateral column of the foot. People who stand for long hours, athletes, or dancers may experience repetitive stress that destabilizes the joint. Even sitting cross-legged for prolonged periods—like tailors did centuries ago—can press the outer foot against the floor, accelerating irritation and earning the condition its name.
Medical and Traumatic Causes
- Arthritis (osteoarthritis or rheumatoid) can erode cartilage, leading to joint instability and deformity.
- Injury to the fifth metatarsal or MTP joint—such as a fracture or dislocation—can disrupt alignment and initiate bunionette formation.
Recognizing the Symptoms of a Bunionette

Early detection is key to preventing progression. Symptoms often start mild but worsen without intervention.
Visible Bump and Skin Changes
The most obvious sign is a hard bump on the outer edge of the foot at the base of the little toe. Over time, this area may become:
– Red, swollen, and warm to the touch
– Covered in calluses or corns from constant shoe rubbing
– Raw or irritated, especially after wearing tight shoes
Pain and Mobility Issues
Pain typically flares when wearing shoes and eases when barefoot. You may experience:
– Sharp or aching pain over the bump
– Tenderness when touched
– Stiffness in the little toe joint
– Difficulty walking or standing for long periods
– Altered gait to avoid pressure
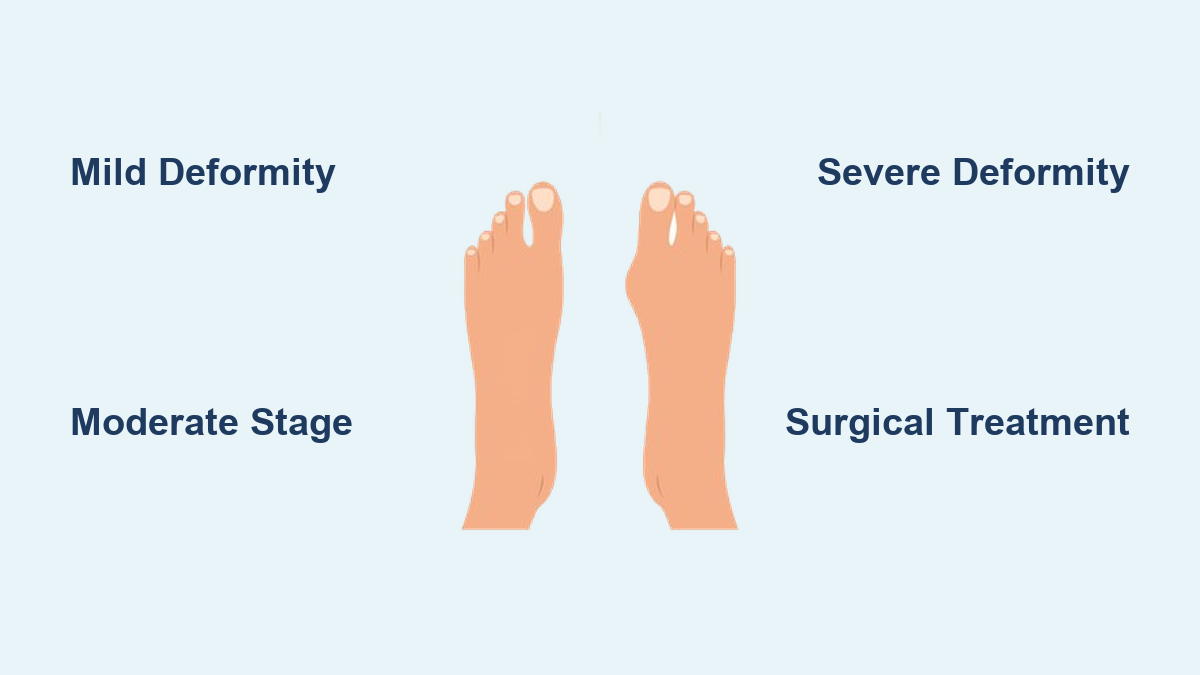
Progressive Toe Deformity
As the condition advances, the little toe may:
– Drift toward the fourth toe
– Overlap or underlap adjacent toes
– Develop a hammertoe due to crowding and muscle imbalance
When to See a Podiatrist
Don’t ignore persistent symptoms. Seek professional help if you notice:
– A growing bump that interferes with shoe wear
– Ongoing pain despite changing footwear
– Redness, warmth, or skin breakdown
– Changes in toe alignment
– Swelling that doesn’t improve with rest
A podiatrist or foot and ankle surgeon can diagnose your condition through physical exam and imaging.
How a Tailor’s Bunion Is Diagnosed
Accurate diagnosis ensures the right treatment—especially when surgery is being considered.
Physical Examination
Your doctor will:
– Inspect the size and location of the bump
– Check for tenderness, redness, and swelling
– Assess range of motion in the little toe
– Evaluate toe alignment and gait
– Look for calluses or skin damage
They’ll also ask about:
– Shoe habits
– Family history
– Occupational or lifestyle factors
X-Ray Evaluation
Weight-bearing X-rays are essential to:
– Measure angles between the fourth and fifth metatarsals
– Determine the degree of metatarsal deviation
– Identify joint arthritis or bony spurs
– Assess overall foot alignment
These images help classify severity and guide treatment decisions.
Non-Surgical Treatment Options
Most tailor’s bunions can be managed without surgery, especially when caught early.
Wear Proper Footwear
Switching to shoes that fit well is the most effective step:
– Wide and deep toe box
– Low heels (under 2 inches)
– Soft, stretchable uppers (mesh, knit)
– Adjustable closures (laces, straps)
– 3–5 mm (1/8 to 1/4 inch) between longest toe and shoe end
Try shoes on in the evening when feet are slightly swollen.
Stretch Shoes for Relief
If you love a pair of shoes but they rub, consider:
– Shoe stretchers (available at drugstores)
– Professional stretching by a cobbler
– Heat-molding services for leather shoes
This creates extra space over the bunionette.
Use Protective Padding
Cushioning reduces friction:
– Gel pads or silicone sleeves over the bump
– Bunionette shields inside the shoe
– Toe spacers to maintain alignment
These don’t correct the bone but protect soft tissues.
Try Orthotics for Support
Custom or over-the-counter insoles can:
– Correct overpronation (flat feet)
– Cushion high arches
– Offload pressure from the fifth metatarsal
Look for orthotics with a lateral forefoot post to reduce lateral loading.
Reduce Inflammation
For flare-ups:
– Ice the area 15–20 minutes every 2–3 hours
– Use NSAIDs like ibuprofen or naproxen
– In severe cases, a doctor may give a corticosteroid injection to calm bursitis
Avoid repeated injections to prevent tissue damage.
Modify Activities
- Limit time in tight shoes
- Avoid cross-legged sitting
- Alternate footwear throughout the day
- Take breaks during prolonged standing
Can You Reverse a Bunionette Without Surgery?
No Natural Bone Reduction
There is no way to shrink or eliminate the bony bump naturally. Once the bone has remodeled, it won’t revert without surgery.
Conservative Care Slows Progression
While it won’t reverse the deformity, proper footwear, padding, and orthotics can:
– Relieve pain
– Prevent worsening
– Avoid surgery
Early action is crucial—once the joint is significantly misaligned, non-surgical options become less effective.
Surgical Treatment Options
Surgery is considered when pain persists despite conservative care.
When Surgery Is Recommended
Indications include:
– Chronic pain limiting activities
– Inability to wear most shoes
– Severe toe deviation
– Bursitis or hammertoe development
Common Surgical Procedures

| Procedure | Best For | Outcome |
|---|---|---|
| Exostosectomy | Mild cases with bump but no angular deformity | Removes bump; quick recovery |
| Osteotomy | Moderate to severe misalignment | Repositions bone; uses screws/pins |
| Resection Arthroplasty | Older patients or arthritis | Removes metatarsal head; may reduce stability |
| Soft Tissue Repair | Joint imbalance | Realigns ligaments and tendons |
| Arthrodesis | Severe arthritis or recurrence | Fuses joint; eliminates motion but adds stability |
Minimally Invasive vs. Open Surgery
- Minimally invasive surgery (MIS): Smaller incisions, faster recovery. Requires specialized training.
- Open surgery: Full visualization, better for complex cases.
Both aim to correct alignment and relieve pain.
Recovery After Surgery
Healing time depends on the procedure.
First 6 Weeks: Protect and Heal
- Non-weight-bearing or partial weight-bearing using crutches
- Wear a surgical shoe, boot, or cast
- Elevate the foot to reduce swelling
- Attend follow-ups for X-rays and suture removal
Weeks 6–12: Gradual Return
- Begin weight-bearing as tolerated
- Start physical therapy
- Transition to supportive, wide-toe-box shoes
Swelling may persist for months.
Full Recovery Timeline
- Most resume normal activities in 3–6 months
- Bone healing can take up to 12 months
Preventing Tailor’s Bunions
You can’t change your genetics, but you can reduce your risk.
Choose Foot-Friendly Shoes
- Avoid pointed toes and high heels
- Prioritize width and depth
- Try brands like New Balance, Brooks, Drew, Propet, Orthofeet
Use Orthotics Early
If you have flat feet or high arches, custom orthotics can correct imbalances before they lead to deformity.
Strengthen Your Feet
Simple exercises help:
– Toe spreads: Fan toes apart and hold 5 seconds
– Towel scrunches: Use toes to pull a towel toward you
– Calf stretches: Improve ankle mobility
Do these daily.
Inspect Feet Regularly
Check for:
– Small bumps
– Red spots
– Calluses on the outer foot
Address issues early.
Frequently Asked Questions
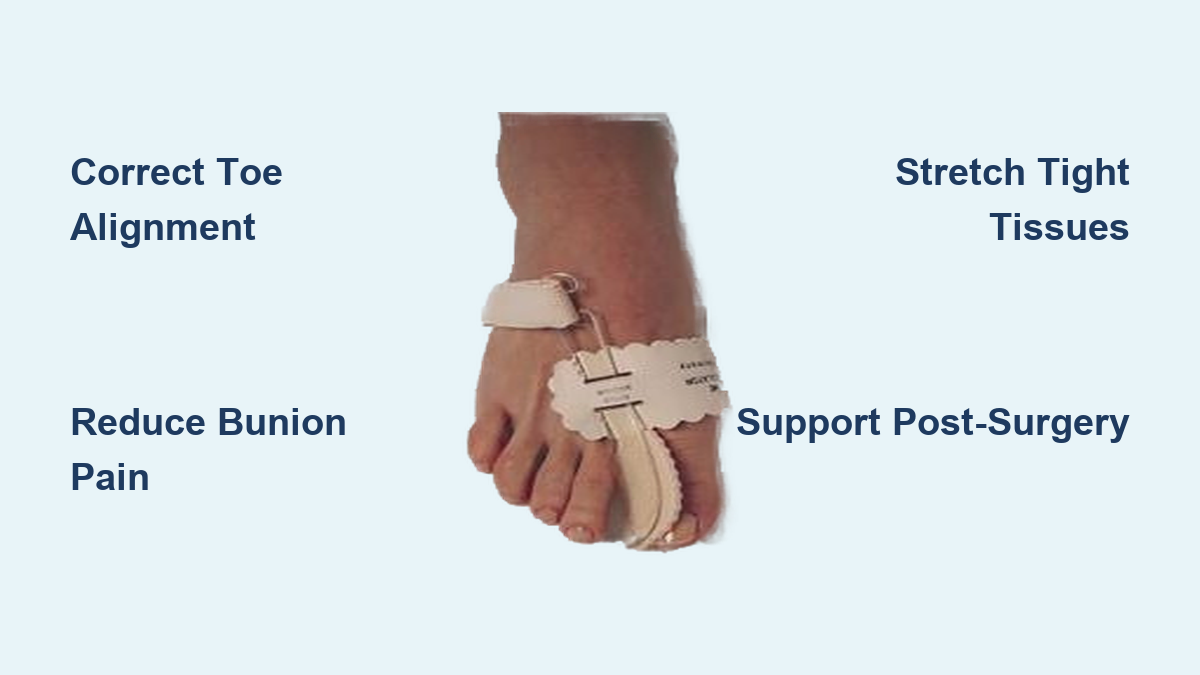
Do bunionette correctors work?
No—they don’t correct the bone. But pads, sleeves, and splints can reduce pain and friction, making them useful for symptom management.
Are tailor’s bunions hereditary?
Yes. A strong genetic link exists. If family members have bunions or foot deformities, you’re more likely to develop one.
Why are women more affected?
Women wear narrow, high-heeled, or pointed shoes more often. Hormonal factors and ligament laxity may also play a role.
How to treat a callus on a bunionette?
- Soak in warm water
- Gently file with a pumice stone
- Apply moisturizer with urea or salicylic acid
- Use padding to prevent recurrence
Never cut calluses—risk of infection is high.
Can a tailor’s bunion go away on its own?
No. The bony bump will not resolve spontaneously. Without treatment, it usually gets worse over time.
Final Thoughts
A tailor’s bunion (bunionette) is more than just a bump—it’s a structural issue that can impact your mobility and comfort. Caused by a mix of genetics, foot mechanics, and shoe pressure, it won’t disappear on its own. But with early action, most people can manage symptoms without surgery.
From choosing the right shoes to using padding and orthotics, conservative treatments are highly effective. When pain persists, surgical options can correct alignment and restore function.
The key is not to ignore the signs. If you’re experiencing pain, swelling, or a growing bump on the outer edge of your foot, see a podiatrist. With proper care, you can walk comfortably—without sacrificing style or mobility.