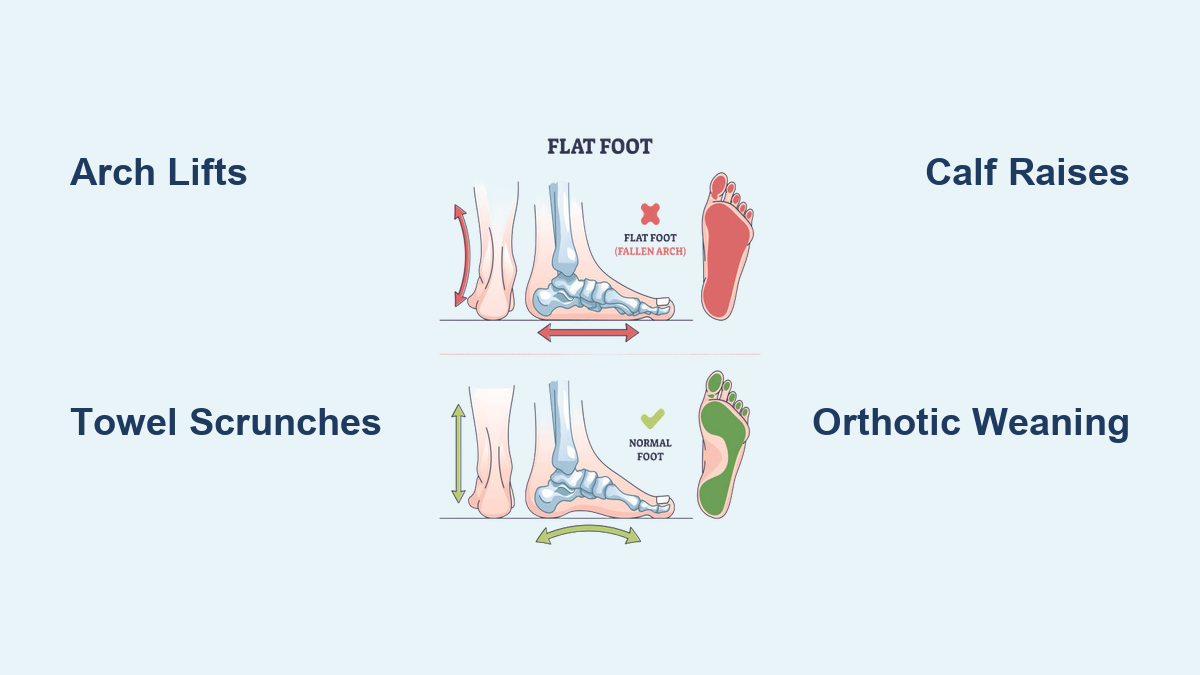
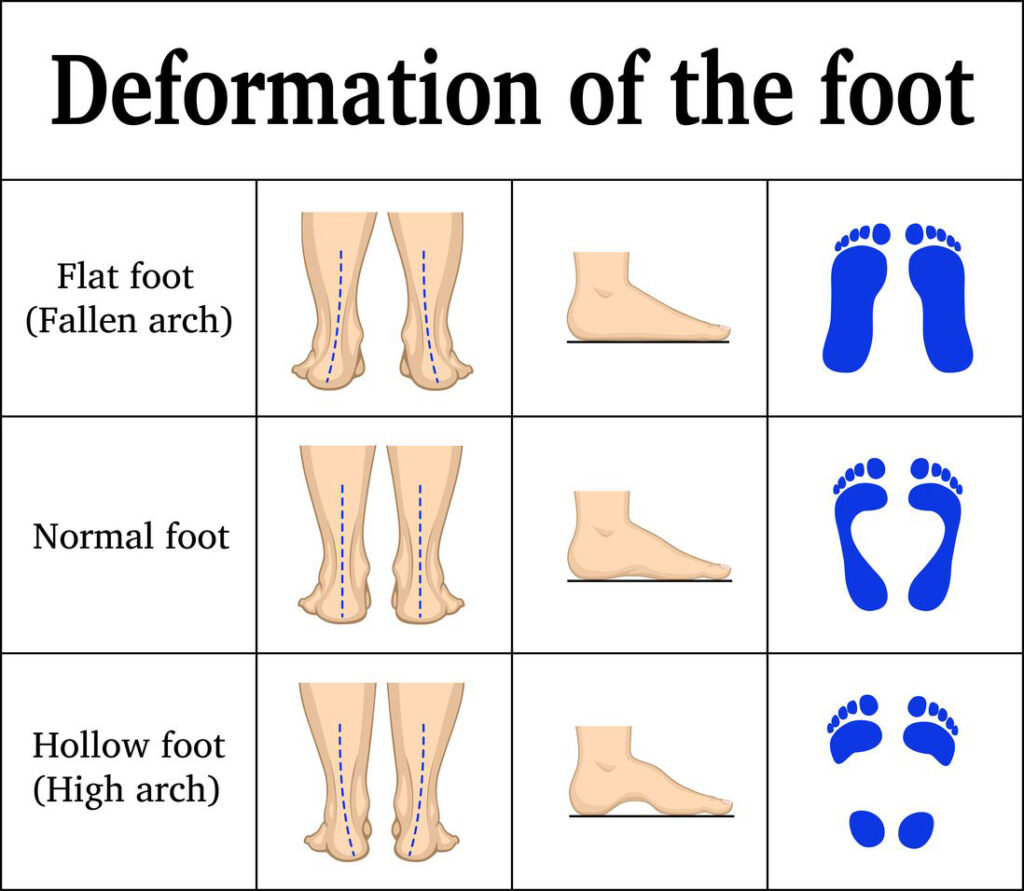
If you wince with every step, feeling a deep ache in your arches or inner ankles after just a short walk, flat feet pain while walking could be the culprit. This common condition—medically known as pes planus—affects millions, including an estimated 18 million Americans who experience discomfort from collapsed or low arches. When the medial longitudinal arch flattens, your entire sole presses into the ground, altering your gait, increasing strain on tendons, and often leading to pain that radiates up into the calves, knees, and even the lower back.
The good news? You don’t have to live with this discomfort. Most cases of flat feet pain are treatable without surgery using a combination of targeted exercises, supportive footwear, orthotics, and lifestyle changes. Whether your flat feet are flexible, rigid, or developed later in life (adult-acquired), the right approach can restore foot strength, correct alignment, and eliminate pain—helping you walk farther, stand longer, and move more freely.
Choose the Right Shoes to Reduce Arch Strain
Wearing proper footwear is the most immediate way to relieve flat feet pain. Shoes that lack structure or arch support allow your feet to overpronate—rolling inward excessively—which places stress on the posterior tibial tendon, the key stabilizer of the arch.
Features of the Best Shoes for Flat Feet
- Firm heel counter: Prevents excessive motion in the rearfoot.
- Motion control or stability design: Limits overpronation during walking.
- Built-in arch support: Mimics a natural arch and redistributes pressure.
- Low heel-to-toe drop (0–8mm): Encourages a neutral foot position.
- Wide toe box: Allows toes to spread naturally, improving balance and shock absorption.
Top picks: Look for athletic shoes labeled “stability” or “motion control,” such as Brooks Adrenaline GTS, ASICS Gel-Kayano, or New Balance 860 series.
What to Avoid
- High heels: Shorten the Achilles tendon and shift weight forward, worsening arch collapse.
- Flat, unsupportive footwear: Flip-flops, ballet flats, and worn-out sneakers offer zero stability.
- Old shoes: Replace every 300–500 miles or when the midsole shows visible wear—even if the outer sole looks fine.
Pro Tip: Try on shoes in the evening when feet are slightly swollen for the most accurate fit.
Use Orthotics to Restore Arch Support

Orthotics act like internal scaffolding for your feet, lifting the collapsed arch and correcting your foot’s alignment with every step.
Over-the-Counter Insoles
- Affordable and effective for mild to moderate symptoms.
- Look for:
- Deep heel cup for stability
- Firm arch contour that matches your foot shape
- Shock-absorbing materials like EVA foam
- Trusted brands: PowerSteps, SuperFeet BLUE, or Sof Sole Airr
Custom Orthotics
- Designed by a podiatrist after gait analysis and foot scanning.
- Ideal for rigid flat feet, severe overpronation, or chronic pain.
- Can last years and are often covered by insurance.
Warning: Don’t rely solely on orthotics. Over time, they can weaken intrinsic foot muscles if not paired with strengthening exercises. Use them as a support tool, not a permanent fix.
Stretch Tight Muscles That Pull on the Arch
Tight calves and plantar fascia increase tension on the arch, making pain worse with every step. Regular stretching reduces this strain and improves foot flexibility.
Calf Stretch at the Wall
- Stand facing a wall, hands at shoulder height.
- Step one foot back, keeping the heel flat and knee straight.
- Lean forward until you feel a stretch in the upper calf.
- Hold 20–30 seconds, repeat 3 times per leg.
- For deeper stretch: Slightly bend the back knee to target the soleus muscle.
Plantar Fascia Stretch
- Sit with one ankle crossed over the opposite knee.
- Gently pull the toes back toward the shin.
- You’ll feel a stretch along the arch.
- Hold 20 seconds, repeat 2–3 times per foot.
Heel Drop Stretch
- Stand on a step with heels hanging off.
- Slowly lower heels below the step level.
- Hold 30 seconds, do 4 sets daily.
- Best done barefoot in the morning to ease first-step pain.
Strengthen the Muscles That Support Your Arch
Weak intrinsic foot muscles contribute to arch collapse. Strengthening them builds dynamic arch support—your body’s natural defense against flat feet pain.
Short Foot Exercise
- Sit or stand barefoot, feet hip-width apart.
- Slide the ball of your foot toward your heel without curling your toes.
- This activates the arch muscles.
- Hold 5 seconds, relax, repeat 3 sets of 10 reps.
- Visual cue: Think of “shortening your foot” like a monkey gripping a branch.
Towel Scrunches
- Place a small towel on the floor.
- Use only your toes to pull it toward you.
- Perform 2–3 sets of 10–15 reps per foot.
- Progression: Pick up marbles or coins with your toes.
Arch Lifts
- Stand barefoot with feet flat.
- Lift the arch upward while keeping your heel and toes on the ground.
- Hold 2–3 seconds, lower slowly.
- Do 2–3 sets of 15 reps.
Build Ankle and Calf Strength for Stability

Strong lower leg muscles improve balance, reduce overpronation, and support the arch during walking.
Heel Raises (Calf Raises)
- Stand on flat ground or a step.
- Rise onto your toes, hold 5 seconds, lower slowly.
- Perform 3 sets of 15–20 reps.
- Advanced: Try single-leg raises or add small pulses at the top.
Heel and Toe Walking
- Toe walking: Walk on tiptoes for 30 seconds—strengthens calves.
- Heel walking: Walk on heels with toes lifted—engages the shin muscles.
- Repeat each 2–3 times.
Stair Arch Raises
- Stand sideways on a step, one foot on, one hanging off.
- Raise the arch of the hanging foot while keeping heel and ball grounded.
- Do 2–3 sets of 10 reps per side.
- Why it works: Isolates the muscles that actively lift the arch.
Reduce Pain and Inflammation Quickly
Even with exercise and good shoes, flare-ups happen. Address pain early to prevent chronic issues.
Ice Therapy
- Apply an ice pack (wrapped in cloth) to the inner arch or ankle for 10–20 minutes.
- Use after walking or standing for long periods.
- Cold ball roll: Freeze a tennis ball and roll under your foot for 2–3 minutes—great for plantar fascia.
NSAIDs for Short-Term Relief
- Ibuprofen (Advil) or naproxen (Aleve) can reduce inflammation and pain.
- Use sparingly—long-term use may affect gut or kidney health.
Corticosteroid Injections
- For severe posterior tibial tendonitis.
- Administered by a doctor; provides temporary relief.
- Not a cure—must be combined with rehab exercises.
Make Lifestyle Changes That Reduce Foot Stress
Small daily adjustments can have a big impact on flat feet pain.
Maintain a Healthy Weight
- Every extra pound multiplies to 3–4 times the force on your feet when walking.
- Losing weight reduces arch strain and improves mobility.
Limit Prolonged Standing
- Take sitting breaks every 30 minutes.
- Use anti-fatigue mats if you work on hard floors.
Choose Low-Impact Activities
- Replace running with:
- Swimming
- Cycling
- Elliptical training
- These keep you fit without pounding your arches.
Try Controlled Barefoot Walking
- Walk barefoot on grass, sand, or soft carpet.
- Strengthens foot muscles and improves balance.
- Avoid hard surfaces until your feet adapt.
Caution: If you have diabetes or neuropathy, consult a doctor before going barefoot.
See a Physical Therapist for Personalized Care
For persistent or worsening pain, physical therapy (PT) delivers targeted rehab that accelerates healing.
What PT Includes
- Gait analysis: Identifies overpronation and imbalance.
- Manual therapy: Releases tight tissues and improves mobility.
- Custom exercise program: Tailored to your foot type and goals.
- Balance and proprioception drills: Improve foot control.
Expert Insight: “Physical therapists can correct subtle imbalances before they lead to knee or back pain.” – Clinical Podiatry Review
Know When to See a Doctor
Most flat feet pain improves with self-care, but see a podiatrist or orthopedic specialist if you have:
– Severe or worsening pain
– Swelling that doesn’t go down
– Numbness or tingling
– Trouble standing on tiptoe
– Pain spreading to knee, hip, or back
Diagnostic Tools
- Wet footprint test: Shows lack of arch imprint.
- X-rays or MRI: Check bone alignment and tendon health.
- Gait analysis: Evaluates walking pattern.
Red flag: Pain on the outside of the ankle may signal advancing deformity and bone impingement.
Consider Advanced Treatments as Last Resorts
When conservative methods fail, medical intervention may be needed.
Immobilization
- A walking boot or cast may be used to rest the foot, especially for acute posterior tibial tendon dysfunction (PTTD).
Surgery
- Reserved for severe, disabling cases.
- Options include tendon repair, bone realignment (osteotomy), or joint fusion.
- Recovery: 3–6 months, including physical therapy.
Fact: Over 90% of flat feet cases improve without surgery. Always exhaust non-invasive options first.
Prevent Long-Term Problems With Daily Habits
Flat feet don’t have to mean lifelong pain. With consistent care, you can prevent progression and maintain foot health.
Daily Prevention Tips
- Wear supportive shoes—even at home.
- Replace worn footwear regularly.
- Continue foot exercises even after pain resolves.
- Use compression socks during long walks or workouts.
Monitor for Changes
- Watch for:
- Increased foot fatigue
- New pain areas
- Visible flattening of the arch
- Early action stops minor issues from becoming major ones.
Final Tips for Pain-Free Walking
- Start slow: Begin exercises gently—no sharp pain.
- Focus on form: Better quality beats high reps.
- Combine strategies: Shoes + orthotics + exercises = best results.
- Be patient: Real improvement takes 6–12 weeks.
- See a pro: If pain lasts more than 4–6 weeks, get evaluated.
Remember: Flat feet pain while walking is not normal—but it is fixable. With the right mix of support, strength, and smart habits, you can walk comfortably again—step after step.