Strategies for minimizing the planter fasciitis effectively condition’s impact is crucial, in the quest to tackle the challenges posed by plantar fasciitis. This comprehensive guide zeroes in on those strategies, offering a beacon of hope for individuals grappling with the persistent heel and foot pain associated with plantar fasciitis. With an emphasis on “Strategies for Minimizing Planter Fasciitis” we delve into a holistic approach that encompasses prevention, immediate relief measures, and long-term management techniques. From the outset, our focus is on educating readers about the root causes of plantar fasciitis, including overuse, unsuitable footwear, and poor foot posture, and then guiding them through a curated selection of interventions.
Table of Contents
We will try to focus on some key Strategies for minimizing the planter fasciitis. The plantar fasciitis, characterized by sharp pain in the heel or bottom of the foot, is a common condition that affects both athletes and non-athletes alike. This discomfort is due to inflammation of the plantar fascia, a thick band of tissue running across the bottom of your foot and connecting your heel bone to your toes. Fortunately, there are effective strategies to minimize the impact of plantar fasciitis, ensuring those affected can lead a pain-free life. This article delves into various methods to manage and potentially alleviate the symptoms of plantar fasciitis.

Understanding Plantar Fasciitis for Minimizing the pain
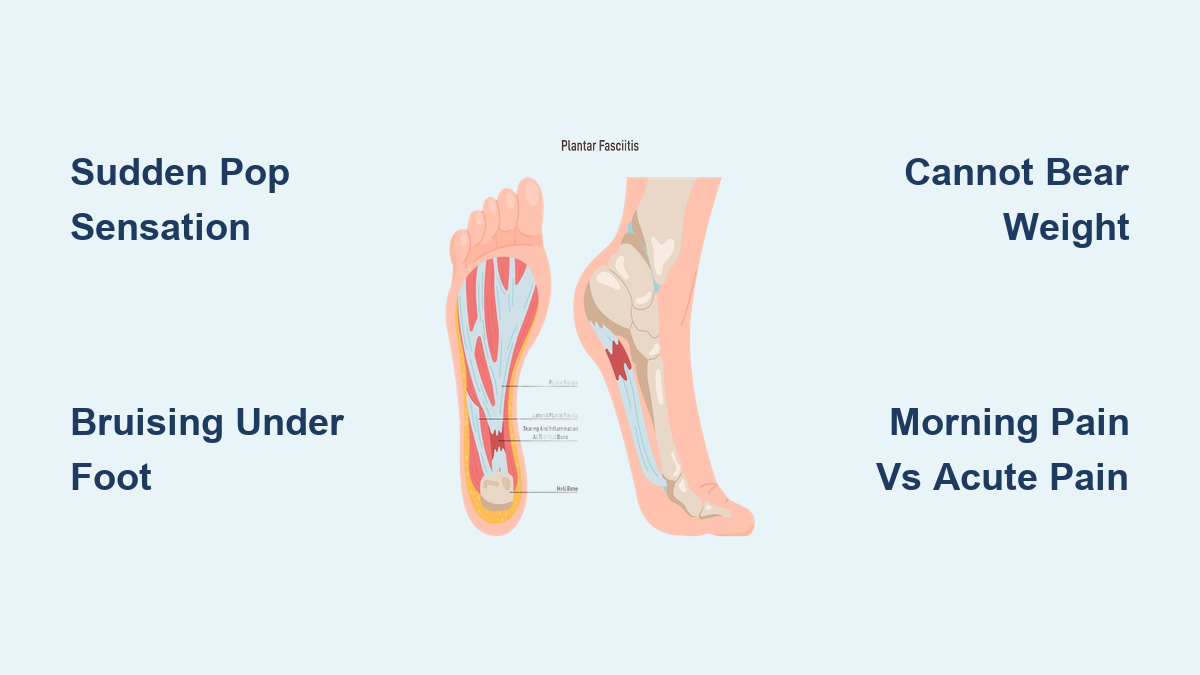
Plantar fasciitis is a common condition that affects the foot, specifically the plantar fascia—a thick, web like ligament that connects your heel to the front of your foot. This ligament acts as a shock absorber and supports the arch of your foot, helping you walk. However, too much pressure on your feet can damage or tear the plantar fascia, leading to a condition known as plantar fasciitis.
The onset of plantar fasciitis is often the result of excessive strain placed on the plantar fascia. This excessive strain can cause small tears in the ligament, leading to inflammation and pain in the heel or the bottom of the foot. The pain is usually most severe with the first steps after waking up, although it can also be triggered by long periods of standing or when getting up from a seated position.

Several factors can contribute to the strain on the plantar fascia and increase the risk of developing plantar fasciitis:
Obesity: Extra weight puts more stress on the plantar fascia, especially if the weight gain happens suddenly.
Inadequate Footwear: Shoes that do not provide proper support, especially in the arch and heel area, can lead to increased strain on the plantar fascia. Worn-out shoes can also be a problem because they no longer cushion the foot effectively.
Prolonged Standing: Occupations that require long hours on your feet can increase the risk of plantar fasciitis due to the constant pressure on the plantar fascia.
Abnormal Walking Pattern: Also known as abnormal gait, this can include issues like excessive pronation (rolling inwards of the foot), which puts additional stress on the plantar fascia.
Age: Plantar fasciitis is most common in people between the ages of 40 and 60, possibly due to the wear and tear on the plantar fascia over time.
Exercise: Activities that place a lot of stress on the heel and attached tissue, like long-distance running, ballet dancing, and aerobic dance, can contribute to an earlier onset of plantar fasciitis.
The diagnosis of plantar fasciitis typically involves a physical examination, with the doctor checking for tenderness in the foot and the exact location of the pain to make sure that it’s not the result of a different foot problem. Imaging tests like X-rays or MRIs may be used to rule out other conditions, such as bone fractures.

Treatment for plantar fasciitis aims to relieve pain and reduce inflammation. Options include rest, ice, over-the-counter pain relievers, physical therapy, and wearing supportive shoes or orthotics. In more severe cases, your doctor might suggest steroid injections, shock wave therapy, or even surgery as a last resort.
Preventive measures can also be taken to avoid plantar fasciitis, such as choosing footwear with adequate support, avoiding sudden weight gain, and doing exercises to strengthen the foot muscles and ligaments. Stretching the Achilles tendon and plantar fascia before activities can also help reduce the risk.
Key Strategies for Relief from the planter fasciitis
Here we will discuss some key Strategies for Minimizing Plantar Fasciitis problem in our daily life.
1. Wear Proper Footwear
Footwear plays a crucial role in managing plantar fasciitis. Shoes with adequate arch support, cushioning, and a flexible sole can help distribute pressure more evenly across your foot, reducing strain on the plantar fascia. It’s advisable to avoid flat shoes and high heels as these can exacerbate the problem.
2. Incorporate Stretching and Strengthening Exercises
Specific exercises can help relieve the pain associated with plantar fasciitis and prevent future occurrences. Stretching exercises aimed at the Achilles tendon and plantar fascia can increase flexibility, while strengthening exercises for the lower leg muscles can improve foot support.
Plantar Fascia Stretch: Sit with your affected leg crossed over your other leg. Use your hand to gently pull your big toe back towards you until you feel a stretch along the bottom of your foot. Hold for 15-30 seconds and repeat 2-3 times.
Calf Stretch: Stand facing a wall with your hands on the wall at eye level. Place the leg with plantar fasciitis behind you, keeping your heel on the ground, and lean forward, bending your front knee until you feel a stretch in the back leg. Hold for 15-30 seconds and repeat 2-3 times.
3. Maintain a Healthy Weight
Excess weight can put additional pressure on your plantar fascia, exacerbating the pain. Losing weight through a balanced diet and regular exercise can significantly reduce the strain on your feet.
4. Apply Ice and Rest
Applying ice to the affected area for 15-20 minutes several times a day, especially after activities that exacerbate your symptoms, can help reduce inflammation and pain. Additionally, giving your feet a rest from high-impact activities can allow the inflammation to subside.
5. Consider Over-the-Counter Supports
Orthotic inserts available over the counter can provide extra cushioning and support for your arch, reducing the strain on the plantar fascia. For more severe cases, custom orthotics prescribed by a podiatrist may be necessary.
6. Physical Therapy
A physical therapist can tailor a treatment plan to your specific needs, incorporating techniques such as manual therapy, taping, and exercises to improve flexibility, strength, and foot mechanics.
7. Use of Night Splints
For chronic plantar fasciitis, wearing a night splint can help. These devices stretch your calf and the arch of your foot while you sleep, preventing the plantar fascia from tightening overnight.
8. Consider Professional Treatment Options
If conservative measures do not bring relief, professional treatments such as corticosteroid injections, shock wave therapy, or in rare cases, surgery, may be considered. These treatments should only be pursued after consulting with a healthcare provider.
Lifestyle Adjustments
In addition to the strategies mentioned above, making simple lifestyle adjustments can also contribute to managing plantar fasciitis effectively:
- Avoid walking barefoot on hard surfaces, which can increase stress on the plantar fascia.
- Incorporate low-impact exercises such as swimming or cycling into your routine to maintain fitness without putting excessive strain on your feet.
- Practice good posture and foot mechanics during activities to reduce unnecessary stress on your feet.
Conclusion
While plantar fasciitis can be a painful and frustrating condition, adopting a comprehensive approach that includes proper footwear, targeted exercises, weight management, and professional guidance can significantly reduce symptoms and improve quality of life. By understanding the underlying causes and implementing these strategies, individuals suffering from plantar fasciitis can take proactive steps towards recovery and prevention. Remember, if your symptoms persist or worsen, it’s important to seek advice from a healthcare professional to explore further treatment options.