Unlock the secrets to overcoming shin splints with our expert guide. Discover groundbreaking treatments, prevention strategies, and insights to get back on track, pain-free. Dive in now!

Introduction
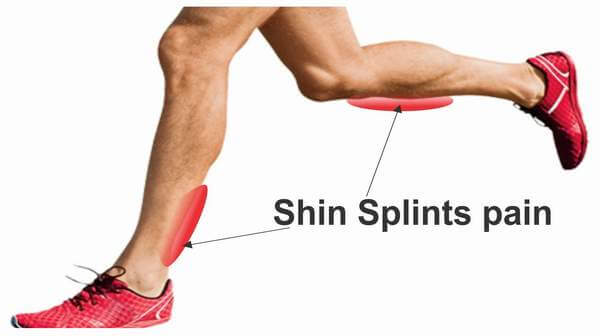
Shin splints, medically termed as medial tibial stress syndrome (MTSS), represent a prevalent ailment that predominantly impacts athletes and individuals engaged in high-impact physical activities, such as running, jumping, and dynamic sports. This condition manifests as pain along the inner side of the shinbone (tibia), a consequence of excessive stress on the bone and its surrounding muscular and connective tissues. The objective of this article is to offer an exhaustive exploration of shin splints, delving into the multifaceted aspects of its etiology, symptomatology, diagnostic methodologies, a variety of treatment modalities, and effective prevention strategies.
Table of Contents
Causes of Shin Splints
Shin splints occur when there is excessive stress on the shinbone (tibia) and the surrounding tissues. Some common causes of shin splints include:
1. Excessive Physical Activity
The primary culprit behind shin splints is often the overuse of the leg muscles, tendons, and bone tissue. This condition predominantly affects individuals who engage in high-impact sports or activities involving substantial leg work, such as running, dancing, and military training. When these activities are performed repetitively without sufficient rest intervals, it places undue stress on the lower legs, leading to the onset of shin splints. The issue is exacerbated if there is a sudden increase in the intensity or duration of these activities without allowing the body adequate time to adapt.
2. Inadequate Footwear
Footwear plays a pivotal role in cushioning and supporting the feet during physical activities. Shoes that lack proper support or are not designed for the specific demands of the activity can significantly contribute to the development of shin splints. This includes shoes with insufficient cushioning for absorbing impact or those that fail to correct biomechanical imbalances in foot alignment. Proper footwear is crucial in distributing the force exerted during movement, thereby reducing the load on the shinbone and surrounding tissues.

3. Biomechanical Imbalances
The structure and mechanics of an individual’s feet and legs can greatly influence the risk of developing shin splints. Biomechanical factors such as abnormal foot arches—either flat feet (overpronation) or excessively high arches (supination)—can lead to an uneven distribution of weight and stress across the leg, placing additional strain on the shinbone. Moreover, improper techniques in running, jumping, or walking can further aggravate the risk by imposing abnormal stress on the lower leg. These biomechanical inefficiencies disrupt the natural alignment and functioning of the leg, thereby predisposing individuals to shin splints.
4. Muscular Imbalances and Flexibility Issues
In addition to the aforementioned causes, muscular imbalances and a lack of flexibility in the lower leg can also precipitate shin splints. Tight calf muscles, weak ankle muscles, and inadequate flexibility can alter gait and running patterns, leading to increased stress on the shinbone. Regular stretching and strengthening exercises targeting the lower leg muscles can help mitigate these risks by promoting better muscle balance and flexibility.
5. Surface and Environmental Factors
Engaging in activities on hard or uneven surfaces can exacerbate the likelihood of developing shin splints due to the increased impact forces transmitted to the shinbone. Similarly, training in poor environmental conditions without appropriate adjustments to equipment or intensity can also elevate stress on the lower legs.
Symptoms
The primary symptom of shin splints is pain along the inner edge of the shinbone. Other common symptoms include:
Pain Along the Inner Edge of the Shinbone
The hallmark symptom of shin splints is a sharp, aching, or throbbing pain felt along the inner side of the shinbone (tibia). This pain is indicative of stress and inflammation in the area surrounding the bone, primarily affecting the connective tissues that attach muscles to the bone.
Tenderness and Soreness
The affected region often exhibits a heightened sensitivity to touch, with tenderness and soreness palpable along the inner aspect of the shin. This soreness can vary in intensity, sometimes presenting as a mild discomfort, but can escalate to severe pain that hinders daily activities.
Swelling and Inflammation
In response to the stress exerted on the shinbone and surrounding tissues, there may be visible swelling and signs of inflammation. While the swelling is typically mild, it further contributes to the discomfort and can be an indicator of the severity of the condition.
Dull or Throbbing Pain During Physical Activity
Individuals with shin splints usually report a dull, aching, or throbbing pain that intensifies during physical activities, especially those involving significant leg work such as running or jumping. The pain might initially appear only during the start of an activity but can become constant as the condition worsens.
Pain That Worsens With Pressure or Impact
Applying pressure to the shinbone or engaging in impact activities can exacerbate the pain. This symptom is particularly noticeable when pressing on the affected area or performing actions that place additional stress on the legs, such as walking or jogging on hard surfaces.
Additional Symptoms
In some cases, individuals may experience muscle stiffness and a reduced range of motion in the affected leg. The pain may also radiate to surrounding areas, contributing to an overall feeling of discomfort in the lower leg.
Progression of Symptoms
Initially, shin splint symptoms might only occur during or immediately after physical activity. However, without proper management and rest, the symptoms can progress to the point where pain is present even at rest, significantly affecting an individual’s mobility and quality of life.
Diagnosis
The diagnostic process for shin splints is comprehensive, aiming to accurately identify the condition while excluding other potential causes of lower leg pain. This multifaceted approach ensures that the treatment plan is appropriately targeted to address the underlying issues contributing to the symptoms. Below is an overview of how shin splints are diagnosed:
Medical History Assessment
- Initial Consultation: The diagnosis begins with a detailed discussion regarding the patient’s medical history, focusing on any previous incidents of leg pain, injury, or conditions that could influence lower leg health. This conversation also covers the patient’s current exercise regimen, recent changes in physical activity levels, and any prior treatments for leg pain.
- Symptom Analysis: Understanding the nature of the symptoms—such as the onset of pain, its duration, and any specific activities that exacerbate or alleviate the discomfort—is crucial. This helps in distinguishing shin splints from other conditions with similar symptoms.
Physical Examination
- Visual and Tactile Assessment: The examining physician will inspect the affected leg for signs of swelling, redness, or anatomical abnormalities. Palpation (the action of touching and feeling the leg) helps in identifying areas of tenderness along the shinbone, which is a key indicator of shin splints.
- Functional Tests: Simple exercises or movements may be requested to observe the leg’s biomechanics, evaluate muscle strength and flexibility, and pinpoint pain triggers. This can include walking, hopping, or flexing the feet.
Advanced Imaging Tests
While the initial diagnosis of shin splints can often be made based on medical history and a physical exam, further testing might be necessary to rule out other conditions:
- X-rays: Although shin splints themselves do not show up on X-rays, this imaging can help exclude bone fractures, which can present with similar symptoms.
- MRI Scans: Magnetic Resonance Imaging (MRI) offers a more detailed view of the soft tissues, including muscles and connective tissues. This can help in identifying stress reactions to the bone or distinguishing shin splints from soft tissue injuries.
- Bone Scans: In cases where stress fractures are a concern, a bone scan might be recommended. This test involves injecting a small amount of radioactive material, which highlights areas of bone remodeling indicative of fractures or severe stress.
Differential Diagnosis
An essential part of diagnosing shin splints is the differential diagnosis process, where similar conditions such as compartment syndrome, stress fractures, and muscle strains are considered and ruled out. This ensures that the treatment plan is accurately tailored to address shin splints rather than another underlying issue.
Treatment
The treatment of shin splints depends on the severity and underlying cause of the condition. Common treatment options include:
1. Rest and Recovery
- Essential Downtime: The cornerstone of treating shin splints involves taking a hiatus from any activities that exacerbate the condition. This period of rest is critical to allow the inflamed tissues around the shinbone to heal. Depending on the severity of the shin splints, this could mean a complete break from certain forms of exercise or a modification of activity levels to avoid further strain on the legs.
- Gradual Resumption: Once symptoms begin to improve, activities can be gradually resumed, ensuring that intensity and duration are carefully managed to prevent recurrence.
2. Ice Therapy
- Pain and Inflammation Reduction: The application of ice packs to the affected area for 20-30 minutes several times a day can significantly help in reducing pain and inflammation. This cold therapy constricts blood vessels, which can decrease swelling and provide temporary pain relief.

3. Compression Techniques
- Supportive Compression: The use of compression sleeves or elastic bandages around the lower leg can offer support and reduce swelling. These compression devices are designed to apply gentle pressure, improving circulation and stabilizing the area, which can aid in the healing process.
4. Medication for Symptom Relief
- NSAIDs for Pain and Inflammation: Nonsteroidal anti-inflammatory drugs, such as ibuprofen or naproxen, may be recommended to help alleviate pain and reduce inflammation. These medications should be used as directed by a healthcare professional to avoid potential side effects.

5. Physical Therapy and Exercises
- Customized Rehabilitation Programs: Physical therapy plays a pivotal role in the treatment of shin splints. A physical therapist can design a personalized program that includes stretching and strengthening exercises to improve the flexibility and strength of the muscles around the shinbone.
- Preventative Strategies: Beyond immediate rehabilitation, physical therapy can also teach patients techniques to prevent future occurrences of shin splints, such as proper warm-up routines and adjustments in exercise form.
6. Orthotic Support
- Custom Orthotics for Added Support: For individuals with biomechanical issues such as flat feet or high arches, custom-made shoe inserts or orthotic devices can be beneficial. These orthotics provide additional support and cushioning, helping to distribute weight more evenly and reduce the stress on the shinbone and surrounding tissues.

By employing a combination of these treatment options, individuals suffering from shin splints can find relief and work towards a full recovery, eventually returning to their regular activities with greater awareness and preventive measures in place.
Prevention
Preventing shin splints is key, especially for athletes who are prone to this condition. Here are some strategies to reduce the risk of shin splints:
1. Progressive Training Adaptation
- Incremental Intensity Adjustments: It’s essential to gradually increase the intensity, distance, and duration of physical activities. This methodical approach allows the muscles, bones, and connective tissues in the lower legs to adapt progressively, reducing the risk of overuse injuries. Setting realistic goals and timelines can help in managing the escalation of activity levels without overwhelming the body.
- Scheduled Rest Periods: Integrating rest days into the training schedule ensures that the body has adequate time to recover. These breaks are vital for preventing the accumulation of stress on the shinbone and surrounding tissues.
2. Optimal Footwear Selection
- Activity-Specific Shoes: Selecting footwear that offers sufficient support and cushioning tailored to the specific demands of your activity can significantly impact the prevention of shin splints. Shoes should be replaced regularly to ensure they provide the necessary protection, as worn-out shoes lose their ability to absorb impact effectively.
- Professional Fitting: Consider consulting a specialist for a professional fitting, as they can recommend shoes based on your foot type and gait, further reducing the risk of shin splints.
3. Diverse Training Regimens
- Cross-Training Incorporation: Engaging in a variety of physical activities can help distribute the stress exerted on the body more evenly. Alternating high-impact activities like running with low-impact exercises such as swimming, cycling, or yoga can prevent overloading the shinbone and muscles.
4. Effective Warm-up and Cool-down Routines
- Dynamic Stretching Pre-Exercise: Starting your workout with dynamic stretches prepares the body for physical activity, increases blood flow, and enhances muscle flexibility, thereby reducing the likelihood of injuries.
- Static Stretching Post-Exercise: Implementing static stretches after exercising helps in cooling down the body, relaxing the muscles, and improving flexibility, which can mitigate the risk of shin splints.
5. Targeted Strengthening and Flexibility Exercises
- Lower Leg Strengthening: Exercises that focus on strengthening the muscles around the shinbone, such as the calves and the anterior tibialis, can improve leg stability and support, reducing the stress on the shinbone.
- Flexibility Enhancement: Regular flexibility exercises for the lower leg muscles help maintain an adequate range of motion, preventing tightness that can contribute to shin splints.
FAQ Section
Q: What exactly are shin splints? A: Shin splints, medically known as medial tibial stress syndrome (MTSS), are a condition characterized by pain along the inner edge of the shinbone due to excessive stress on the shinbone and surrounding tissues.
Q: Who is most at risk for developing shin splints? A: Athletes, dancers, military recruits, and anyone involved in high-impact activities are at a higher risk due to the repetitive stress on their lower legs.
Q: Can improper footwear contribute to shin splints? A: Yes, shoes that lack proper support or cushioning can significantly increase the risk of developing shin splints by failing to absorb impact or correct biomechanical imbalances.
Q: Are there effective treatments for shin splints? A: Absolutely. Treatments range from rest and ice therapy to physical therapy and custom orthotics, all aimed at reducing inflammation, correcting biomechanical issues, and strengthening the surrounding muscles.
Q: How can I prevent shin splints? A: Prevention strategies include gradual training increases, selecting the right footwear, incorporating cross-training, and performing targeted strengthening and flexibility exercises.
Q: What role does diet play in the recovery from shin splints? A: Nutrition plays a crucial role in the healing process of shin splints. A diet rich in calcium and vitamin D can support bone health, while anti-inflammatory foods like omega-3 fatty acids (found in fish, flaxseeds, and walnuts) can help reduce inflammation. Staying hydrated and maintaining a balanced diet can also support overall muscle and bone health, aiding in quicker recovery.
Q: Can shin splints lead to more serious injuries if left untreated? A: Yes, if shin splints are not properly treated, they can lead to more severe conditions, such as stress fractures. Ignoring the symptoms and continuing to engage in high-impact activities without allowing adequate time for recovery can exacerbate the stress on the shinbone, potentially leading to small cracks or fractures in the bone. It’s crucial to address shin splints early and follow a comprehensive treatment plan to prevent progression to more serious injuries.
Q: How often should I replace my running shoes to prevent shin splints? A: The lifespan of running shoes can vary depending on your running style, weight, and the shoe’s quality, but a general guideline is to replace them every 300 to 500 miles. Worn-out shoes lose their ability to absorb shock effectively, which can increase the risk of shin splints. Pay attention to signs of wear in the midsole and tread and consider getting professionally fitted for new shoes to ensure they provide the appropriate support and cushioning for your activities.
Conclusion
Shin splints don’t have to be a roadblock on your path to fitness and athletic excellence. With the right knowledge, treatment plan, and preventive measures, you can navigate through this challenge and emerge stronger. Remember, understanding your body’s signals and responding with care is key to overcoming shin splints and achieving your physical activity goals. Embrace the journey to recovery with patience and perseverance, and let this guide be your first step towards a pain-free lifestyle.