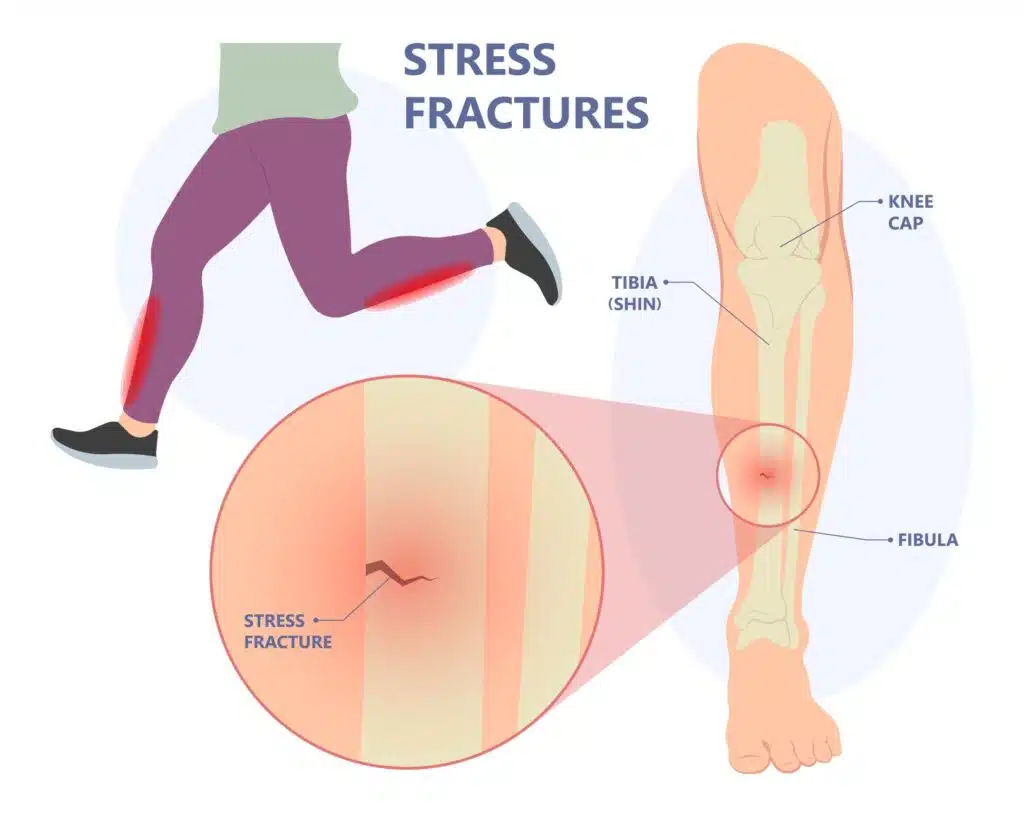
That nagging ache in your shin after a run—could it be more than just soreness? If the pain is focused in one spot, flares during activity, and lingers longer each day, you may be experiencing a stress reaction, the silent precursor to a stress fracture. Unlike muscle fatigue, which fades with rest, a stress reaction signals that your bone is struggling to keep up with repetitive strain. This early stage of bone injury occurs when microdamage accumulates faster than your body can repair it—long before a crack forms. The good news? With early detection, most stress reactions heal in just 2–6 weeks without immobilization. But ignore the warning signs, and recovery time jumps to 6–12 weeks or more. This guide breaks down the key red flags, physiological changes, and diagnostic tools to help you catch a stress reaction in time—plus science-backed strategies to prevent it from turning into a full fracture.
How to Spot a Stress Reaction Early
Pain That Gets Worse with Each Workout
The first sign of a stress reaction is often subtle: a dull ache that starts late in your workout—maybe at mile 4 or after a hard set. At first, it disappears quickly with rest, making it easy to dismiss. But over days or weeks, the pain starts earlier in activity and lasts longer afterward. If you’re now feeling discomfort at mile 1 instead of mile 5, and the pain sticks around for hours post-exercise, your bone is sending an SOS. This progressive pattern is a hallmark of bone stress—unlike muscle soreness, which improves with training, stress reaction pain escalates.
Watch for:
– Pain onset shifting earlier in each session
– Discomfort lasting more than 30 minutes after stopping
– Needing longer recovery between workouts
This worsening cycle means your bone’s repair system is overwhelmed. Without intervention, it’s only a matter of time before a microcrack forms.
Pinpoint Tenderness Over the Bone
One of the most telling signs is focal tenderness—so precise you can press one finger on the exact spot and reproduce the pain. This isn’t a broad muscle ache; it’s a sharp, deep sensation directly on the bone. For example, pressing on the mid-shin (tibia) or the top of the foot (metatarsals) triggers pain that mirrors what you feel while running.
High-risk areas include:
– Tibia (shin)
– Metatarsals (long bones in the foot)
– Femoral neck (hip)
– Navicular (midfoot)
– Fibula (outer lower leg)
– Calcaneus (heel)
If pressing on the bone hurts more than stretching or moving the joint, suspect a bone stress injury—not a strain or tendon issue.
Swelling and Warmth Without Bruising
Mild swelling may develop over the affected bone, especially in the foot or lower leg. The area might feel puffier than the other side, and the skin could be slightly warm to the touch due to internal inflammation. Unlike an ankle sprain, there’s no bruising or discoloration—because no acute injury occurred. This subtle swelling is often overlooked, but comparing both limbs side-by-side can reveal asymmetry that points to early bone stress.
Pain That Lingers—or Wakes You Up
Early-stage stress reactions resolve within minutes of stopping activity. But as damage builds, the pain lasts longer—into the evening, and eventually, at rest. A major red flag is night pain, especially in the shin, foot, or hip. This type of discomfort, felt while lying down or during the night, signals significant bone inflammation and possible progression to a microfracture.
Clinical alert: Night pain is not normal. It’s a strong indicator that your bone is in crisis and needs immediate attention.
Limping or Changing Your Running Form
Your body instinctively protects injured areas. You might shorten your stride, avoid pushing off on one foot, or shift weight to your other leg. These gait changes are often subtle but can be spotted by a coach or physical therapist. Over time, altered mechanics increase stress on your knees, hips, or opposite limb, raising the risk of secondary injuries.
Warning signs:
– Limping after runs
– Feeling “off” or unbalanced
– Avoiding heel strike or toe-off on one side
Even minor changes in movement suggest your body is trying to offload a stressed bone.
A Positive Hop Test Signals Trouble
The single-leg hop test is a quick functional check for lower limb bone stress. Stand on the affected leg and hop forward 6–12 inches, landing and holding for 2 seconds. If this causes sharp, localized pain, the test is positive—and strongly suggests a stress reaction.
Best for: Tibial, metatarsal, and calcaneal injuries.
Caution: Do this only once or twice. Repeated hopping can worsen microdamage.
Why a Stress Reaction Turns Into a Fracture

The 5-Stage Bone Injury Timeline
Bone damage follows a predictable path:
1. Normal loading: Microdamage occurs during activity; bone repairs itself.
2. Fatigue accumulation: Damage outpaces repair.
3. Stress reaction: Inflammation and edema appear—no crack yet.
4. Stress fracture: A microcrack forms; structural integrity fails.
5. Complete fracture: The crack extends fully through the bone.
The critical window for intervention is Stage 3—the stress reaction. At this point, healing takes 2–6 weeks with proper management. Once a crack forms (Stage 4), recovery jumps to 6–12 weeks or more.
X-Rays Miss Early Stress Reactions—MRI Doesn’t
Standard X-rays often come back normal in the early stages because they can’t detect bone marrow edema—the key sign of a stress reaction. MRI, however, can spot inflammation within days of overuse. By the time an X-ray shows a stress fracture, the injury has been developing for weeks.
Bottom line: If you have localized bone pain that worsens with activity, get an MRI. It’s the only way to confirm a stress reaction before a crack forms.
Risk Factors You Can’t Ignore

Sudden Training Increases
The #1 trigger? Ramping up too fast. Doubling your mileage, adding speedwork, or switching surfaces without adaptation overwhelms bone remodeling. Follow the 10% rule: never increase weekly volume or intensity by more than 10%.
Poor Biomechanics
Flat feet, high arches, leg length discrepancies, or weak glutes alter how force travels through your body, concentrating stress on bones instead of muscles. A gait analysis can identify these issues before they cause injury.
Nutritional Deficiencies
Bone health depends on:
– Calcium (1,000–1,300 mg/day)
– Vitamin D (600–2,000 IU/day)
– Adequate calories
Low energy availability, especially in female athletes, can lead to the Female Athlete Triad—a dangerous combo of low calories, missed periods, and weak bones—that triples fracture risk.
Worn-Out Shoes
Running shoes lose cushioning after 300–500 miles. Worn soles transfer more impact to bones. Replace them every 3–6 months if you run regularly.
When It’s Not Just Soreness
Stress Reaction vs. Muscle Soreness

| Feature | Stress Reaction | Muscle Soreness |
|---|---|---|
| Onset | Gradual, worsens over weeks | 24–72 hrs post-exercise |
| Location | Focal, on bone | Diffuse, muscle belly |
| Tenderness | Sharp with bone pressure | Dull, broad ache |
| Pain Pattern | Worse with loading | Improves with movement |
| Rest Response | Incomplete relief | Resolves in 3–5 days |
If pain persists beyond a few days and correlates with activity, don’t assume it’s DOMS.
When to See a Doctor
Seek evaluation if you have:
– Pain worsening over 3–5 days despite rest
– Tenderness on a specific bone spot
– Swelling or warmth over bone
– Limping or gait changes
– Pain at rest or night pain
Urgent care needed if you can’t bear weight or feel sudden severe pain.
Prevent and Treat Before It’s Too Late
Immediate Action Steps
- Stop high-impact activity (running, jumping)
- Switch to pool running, cycling, or elliptical
- Use a walking boot or stiff-soled shoe for foot/shin injuries
- Consider crutches if walking causes pain
Recovery Timeline
- Stress reaction: 2–6 weeks
- Stress fracture: 6–12 weeks
- High-risk fractures (navicular, femoral neck): 3–6 months
Gradual Return to Running
Only restart when:
– Pain-free during daily activities
– Cleared by imaging (if done)
– Strength and mobility are restored
Start with 1-minute run / 3-minute walk intervals, increasing run time by 10% per week.
Final Note: Pain is your body’s alarm. Localized, activity-related bone pain isn’t “normal”—it’s a stress reaction until proven otherwise. Recognize the signs: worsening pain, pinpoint tenderness, lingering discomfort, and gait changes. Act fast with rest, proper diagnosis, and smart rehab. With the right steps, you’ll avoid a fracture and get back to doing what you love—faster and safer.