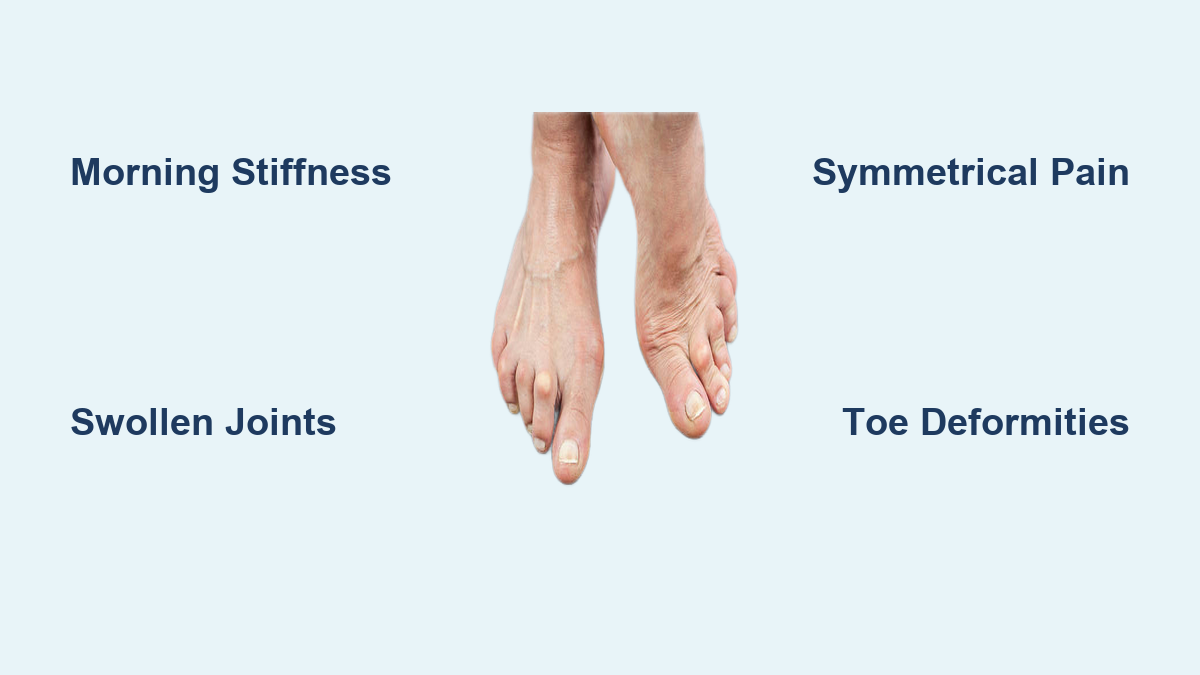
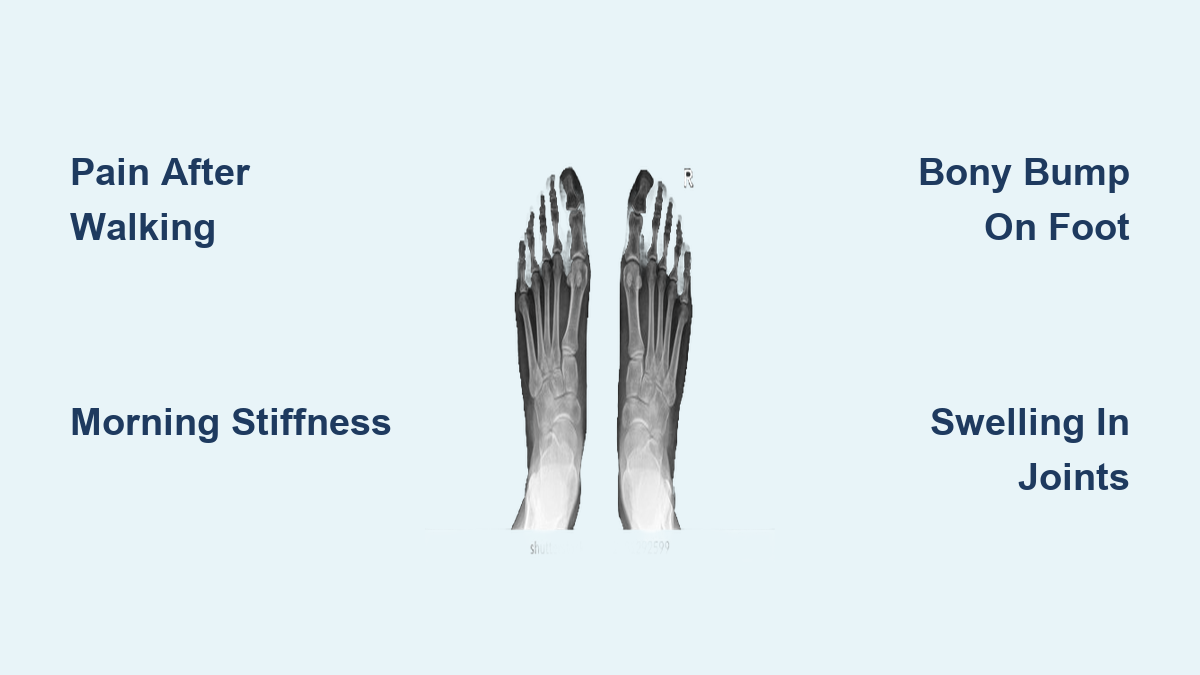
Waking up with stiff, aching toes that take minutes—or even hours—to loosen up could be more than just soreness from yesterday’s walk. For many, these subtle but persistent symptoms are the first warning signs of rheumatoid arthritis (RA) in the toes. Unlike osteoarthritis, which results from wear and tear, RA is an autoimmune disease that attacks the joints symmetrically, often starting in the small joints of the feet. In fact, about 20% of people with RA first notice symptoms in the toes or feet, and nearly 90% will experience foot involvement during their lifetime. Left undiagnosed, RA can lead to permanent joint damage, painful deformities, and difficulty walking. But catching it early—recognizing the signs before severe damage occurs—can dramatically improve outcomes. This guide breaks down the key symptoms, how RA affects toe joints, what to look for during flares, and when to seek help. Whether you’re struggling with toe pain or monitoring a recent diagnosis, understanding these signs is the first step toward effective management.
Early Warning Signs of RA in the Toes
Rheumatoid arthritis often begins quietly, with symptoms in the toes that may seem minor at first. Because RA typically affects both feet at once, symmetrical pain and stiffness are major red flags. These early changes can precede diagnosis by months or even years.
Morning Stiffness That Lasts Over 30 Minutes
One of the most telling signs of RA is morning stiffness lasting more than 30 minutes. Unlike typical soreness that eases quickly, RA-related stiffness in the toes can take hours to improve. You might find it hard to wiggle your toes or walk normally when you first get out of bed. This prolonged stiffness results from overnight joint inflammation and is a hallmark of autoimmune arthritis. If you need to “warm up” your toes before walking comfortably each morning, this isn’t normal wear-and-tear—it could be early RA.
Swelling and Warmth Around Toe Joints
Swelling in the ball of the foot or around the base of the toes—especially the big toe—is common. The metatarsophalangeal (MTP) joints are frequent early targets. Affected joints may appear puffy, feel warm to the touch, and be tender when pressed. This inflammation isn’t just cosmetic; it signals active synovitis, where the immune system attacks the joint lining. You might notice your socks feel tighter in the forefoot area, or your shoes no longer fit comfortably—even if they haven’t changed size.
Pain That Increases With Standing or Walking
Toe pain in RA often worsens with standing or walking and improves with rest. You might feel a sharp or burning sensation under the ball of the foot when pushing off during a step. Early on, pain may come and go during flare-ups, alternating with periods of relief. Over time, without treatment, the pain becomes more constant and harder to ignore. Activities like climbing stairs, walking on hard surfaces, or wearing tight shoes can trigger or intensify discomfort.
Visible and Functional Changes in RA-Affected Toes

As RA progresses, subtle symptoms evolve into noticeable physical changes. These deformities not only affect appearance but also make walking painful and wearing regular shoes difficult.
Redness and Localized Joint Tenderness
Active inflammation can cause redness over the toe joints, especially during flares. Combined with warmth and swelling, this “hot joint” appearance helps distinguish RA from other foot conditions. Tenderness is often localized to the MTP joints but can spread to the midfoot as the disease advances. Pressing on the ball of the foot may elicit pain, and you might avoid putting weight on the front of your foot altogether.
Difficulty Walking or Altered Gait Patterns
Even mild swelling in the forefoot can disrupt normal gait. You may start limping or shifting weight to the outer edges of your feet to avoid pressure on painful toe joints. Standing for long periods becomes exhausting, and you might need to sit down frequently. This altered walking pattern can lead to secondary issues like knee, hip, or lower back pain due to uneven weight distribution.
Systemic Symptoms That Accompany Toe Pain
RA is a whole-body disease. Toe symptoms often appear alongside fatigue, low-grade fever, and unexplained weight loss. You may feel generally unwell, even when joint pain seems mild. These systemic signs, combined with symmetrical toe involvement, strongly suggest an autoimmune process rather than mechanical injury or overuse.
Common Toe Deformities Caused by Rheumatoid Arthritis

Without treatment, chronic inflammation weakens ligaments, tendons, and joint structures, leading to permanent changes in toe alignment and foot shape.
Severe Bunions (Hallux Valgus)
RA often causes severe bunions—a bony bump at the base of the big toe. Unlike typical bunions from ill-fitting shoes, RA-related bunions develop due to joint instability and inflammation. The big toe drifts inward, sometimes crossing over the second toe, making shoe fit nearly impossible. This deformity is not only painful but also alters balance and increases pressure on other toes.
Claw and Hammer Toes
Claw toes occur when toes curl downward at both the middle and end joints, creating pressure points on the top and tip. Hammer toes are bent at the middle joint only. These deformities result from muscle imbalances and tendon damage. The knuckles become prominent, leading to painful calluses or even skin breakdown from constant shoe friction.
Metatarsalgia and Forefoot Collapse
As ligaments weaken, the transverse arch of the forefoot collapses, causing the front of the foot to splay outward. This shifts weight to the metatarsal heads, leading to metatarsalgia—sharp, burning pain under the ball of the foot. Over time, these bones become prominent and may ulcerate, especially in people with reduced sensation or poor circulation.
Crossed and Overlapping Toes
With joint instability, one toe may cross over or under another, most commonly the second toe overlapping the big toe. This is not just cosmetic—it can cause friction, corns, and difficulty finding shoes that fit. The condition worsens as RA progresses and joint support deteriorates.
When to See a Doctor for Toe Pain
Early diagnosis is critical. The sooner RA is identified, the better your chances of slowing joint damage and preserving function.
Symmetrical Joint Pain Is a Major Red Flag
If you have pain, swelling, or stiffness in the same toes on both feet, especially with morning stiffness lasting over 30 minutes, see a healthcare provider. Symmetry is a key clue that points to RA rather than injury or gout.
Persistent Symptoms Despite Rest and Home Care
If toe pain doesn’t improve after days of rest, ice, and over-the-counter pain relievers, it’s time to get evaluated. RA symptoms don’t resolve with simple measures because the underlying cause is systemic inflammation, not mechanical strain.
Signs of Systemic Inflammation Should Not Be Ignored
Fatigue, low-grade fever, or unexplained weight loss alongside toe pain should prompt immediate medical attention. These are not foot problems—they’re signs of whole-body immune activation that require blood testing and specialist care.
How RA in the Toes Is Diagnosed
Diagnosing RA involves more than just a physical exam. A combination of clinical findings, blood tests, and imaging helps confirm the condition and rule out other causes.
Physical Exam Findings
Doctors check for:
– Tenderness in the MTP joints
– Swelling and warmth in toe joints
– Range of motion—early RA may still allow movement, but pain limits it
– Foot shape changes like bunions or clawing
– Calluses or pressure points indicating abnormal weight distribution
Blood Tests That Confirm Autoimmune Activity
No single test diagnoses RA, but these are key:
– Rheumatoid Factor (RF): Positive in 70–80% of cases
– Anti-CCP antibodies: More specific than RF; strongly predicts erosive disease
– CRP and ESR: Markers of inflammation; often elevated during flares
A positive anti-CCP test with symptoms is highly predictive of RA and helps guide early treatment.
Imaging to Detect Joint Damage Early

| Test | What It Shows |
|---|---|
| X-ray | Bone alignment, joint space narrowing, erosions, deformities |
| MRI | Early synovitis, tendon inflammation, bone edema—often before X-ray changes |
| Ultrasound | Real-time imaging of joint fluid and soft tissue inflammation |
MRI is especially valuable when symptoms are present but X-rays look normal. It can detect inflammation long before structural damage appears.
Treatment Options for RA Toe Symptoms
While there’s no cure, early and aggressive treatment can control inflammation, relieve pain, and prevent deformities.
Medications That Slow Disease Progression
- DMARDs (e.g., methotrexate): First-line treatment; slows joint damage
- Biologics (e.g., adalimumab): Target specific immune pathways; used when DMARDs fail
- NSAIDs (e.g., ibuprofen): Reduce pain and swelling but don’t stop joint destruction
- Corticosteroids: Provide fast relief during flares; injections into toe joints can also help diagnose pain sources
Early use of DMARDs within six months of symptom onset is linked to better long-term outcomes.
Supportive Footwear and Orthotics
Proper shoes are essential:
– Wide toe boxes to accommodate bunions and claw toes
– Stiff soles to reduce joint motion during walking
– Arch support to stabilize the foot
– Rocker soles to ease pressure on the forefoot
Avoid soft, floppy shoes—they may feel comfortable at first but increase strain over time.
Custom orthotics made from soft, cushioned materials help redistribute pressure away from painful areas. Hard inserts can worsen pain in RA due to thinning skin and bony prominences.
Bracing, Padding, and Toe Spacers
- Toe spacers reduce friction between overlapping toes
- Metatarsal pads lift and cushion the ball of the foot
- Lace-up braces support the midfoot and ankle
- Custom-molded inserts provide maximum comfort for severe deformities
These tools can delay or even prevent the need for surgery.
Surgical Options for Severe RA Toe Deformities
When conservative treatments fail, surgery can restore function and relieve pain.
When Surgery Is Needed
Consider surgery if you have:
– Severe pain that limits daily activities
– Fixed, rigid deformities (e.g., clawed toes)
– Skin ulcers from bony pressure
– Inability to wear shoes or walk normally
Common Procedures
- Fusion (Arthrodesis): Most common; fuses damaged joints to eliminate motion and pain
- Metatarsal Head Resection: Removes part of the bone to reduce pressure under the ball of the foot
- Tendon Releases or Transfers: Corrects alignment in early deformities
- Lesser Toe Corrections: Includes bone cuts (Weil osteotomy), joint removal, or fusion for toes 2–5
Recovery takes 6+ weeks, often with non-weight-bearing restrictions. Risks include infection, poor healing, and nerve damage—especially in patients on immunosuppressants.
Long-Term Management and Prevention
RA is lifelong, but proactive care can preserve foot function and prevent complications.
Daily Foot Care Tips
- Inspect your feet daily for redness, swelling, or skin breaks
- Wear supportive shoes at all times, even indoors
- Avoid walking barefoot to prevent injury
- Maintain a healthy weight to reduce joint stress
- Perform gentle toe stretches to preserve mobility
Regular Medical Monitoring
- See your rheumatologist regularly to adjust medications
- Schedule foot check-ups with a podiatrist every 6–12 months
- Get periodic X-rays or MRIs to monitor joint changes
- Report new or worsening toe pain immediately
Final Note: Recognizing the signs of rheumatoid arthritis in the toes—from early stiffness to visible deformities—can make a critical difference in long-term joint health. With prompt diagnosis, appropriate treatment, and consistent foot care, many people with RA maintain mobility and independence for years. If you’re experiencing persistent toe pain, swelling, or stiffness, don’t wait. Early action is your best defense against irreversible damage.