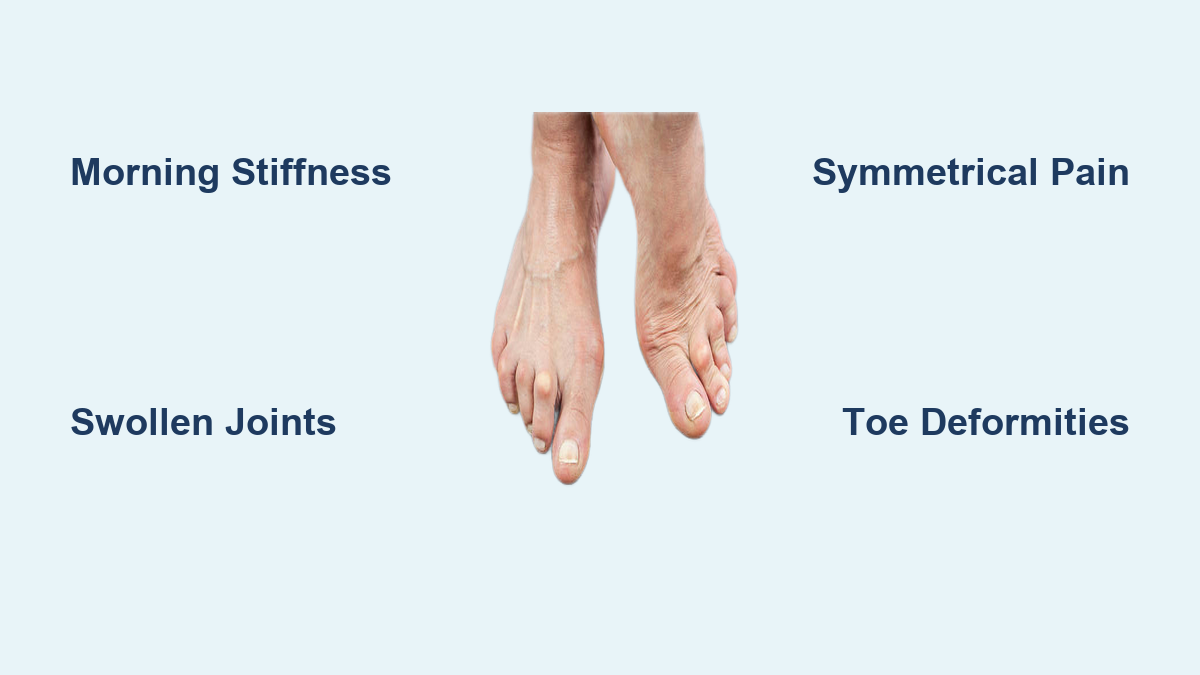
If you’ve started to feel pain when walking, notice stiffness in your toes after sitting, or see a hard bump forming on the top of your foot, you may be experiencing early signs of osteoarthritis (OA) in the foot joints. Osteoarthritis is the most common type of arthritis, and despite often being associated with knees and hips, it frequently affects the complex network of over 30 joints in each foot. Unlike inflammatory arthritis, OA develops gradually due to wear and tear, primarily targeting weight-bearing joints like the base of the big toe, midfoot, and ankle. Left unchecked, it can lead to joint deformity, chronic pain, and reduced mobility. Recognizing symptoms early—such as activity-related discomfort, morning stiffness, swelling, or visible bone spurs—can help you take action before irreversible damage occurs. This guide outlines the key signs, affected areas, progression patterns, and effective strategies for managing foot OA.
Early Warning Signs of Foot OA
Pain After Activity
One of the earliest indicators of foot osteoarthritis is joint pain that flares up after standing, walking, or other weight-bearing activities. This discomfort is typically localized to the top of the foot, especially near the big toe or midfoot. Unlike nerve pain or plantar fasciitis, OA-related pain improves with rest and worsens with use. In the early stages, it may come and go—easily mistaken for fatigue or overuse—making it easy to ignore. However, recurring pain after routine activities like climbing stairs or walking on hard surfaces should not be dismissed.
Morning Stiffness That Fades Quickly
Stiffness in the foot joints—especially after waking or sitting for long periods—is a hallmark of OA. However, unlike rheumatoid arthritis, morning stiffness in OA typically lasts less than 30 minutes and eases as you start moving. If your foot feels “locked” at first but loosens up within a few minutes of walking, osteoarthritis could be the cause. This temporary stiffness results from joint fluid redistribution after inactivity and is a key clue differentiating OA from inflammatory conditions.
Swelling Around Joints
Swelling in foot OA is usually mild and confined to the affected joint. You might notice puffiness on the top of the foot, often accompanied by warmth or tenderness. This results from low-grade inflammation in the joint lining or fluid buildup due to cartilage breakdown. Unlike the widespread swelling seen in gout or rheumatoid arthritis, OA-related swelling tends to be localized and increases after prolonged activity.
Visible and Structural Changes

Bony Bump on Top of Foot
A telltale sign of foot OA is a hard, bony protrusion on the top of the foot, most commonly at the base of the big toe. This bump is caused by osteophytes (bone spurs)—abnormal bone growths that form as the joint tries to stabilize itself amid cartilage loss. Over time, this prominence can rub against shoes, leading to redness, skin irritation, or calluses. In some cases, a soft tissue cyst may also develop, creating a “bubble-like” appearance over the joint.
Joint Deformity and Toe Stiffness
As OA progresses, the joint may lose its normal shape. The big toe (hallux) can become stiff and difficult to bend—a condition known as hallux rigidus. In advanced stages, the joint may fuse, making it painful to push off while walking. You might also begin to notice your arch flattening or your foot collapsing inward, altering your gait and increasing strain on other joints.
Crepitus: Crunching Sensation
When moving the affected joint, you may hear or feel a grating, cracking, or crunching noise. This is called crepitus and occurs when damaged cartilage causes bones to rub together. While not always painful, crepitus is a clear sign of joint degeneration and is commonly reported by patients with midfoot or big toe OA.
Commonly Affected Foot Joints

Big Toe Joint (First MTP)
The first metatarsophalangeal (MTP) joint—where the big toe meets the foot—is the most frequent site for foot OA. Due to constant pressure during walking, this joint wears down over time. Symptoms include:
– Pain when pushing off with the toe
– Difficulty wearing tight or high-heeled shoes
– Dorsal (top-side) bone spurs
– Progressive stiffness (hallux rigidus)
This joint bears up to twice your body weight with each step, making it highly susceptible to degeneration.
Midfoot Arthritis
OA in the midfoot joints—such as the tarsometatarsal and naviculocuneiform joints—often follows trauma or arch collapse. Pain is typically felt on the top of the midfoot and worsens on uneven surfaces or after prolonged standing. Over time, this can lead to a “rocker-bottom” foot, where the arch flattens and the sole bulges downward, increasing pressure on the ball and heel of the foot.
Ankle Joint Involvement
While less common, the ankle joint can develop OA after fractures or severe sprains. Symptoms include:
– Deep joint pain during movement
– Swelling and stiffness after activity
– Instability or wobbliness when standing
– Reduced range of motion in up-and-down motion
Post-traumatic ankle OA is a leading cause of chronic ankle pain in active adults.
Stages of Osteoarthritis Progression

Stage 1: Mild Joint Wear
In the earliest stage, cartilage begins to thin but symptoms are minimal. You may experience occasional stiffness or mild pain after long walks. X-rays may show slight joint space narrowing, but no bone spurs or deformities.
Stage 2: Noticeable Symptoms
Cartilage damage becomes more evident. Pain and swelling occur more frequently, especially after activity. Bone spurs start to form, and joint motion begins to stiffen. Daily tasks like walking or climbing stairs become uncomfortable.
Stage 3: Severe Cartilage Loss
Pain is now constant, even at rest or during the night. Joint space is significantly narrowed on imaging, and bone-on-bone contact begins. The foot may appear deformed, and movement is limited. Walking becomes increasingly difficult.
Stage 4: End-Stage Degeneration
At this point, cartilage is nearly or completely gone. The joint is stiff, deformed, and extremely painful. Bone spurs are large, and mobility is severely restricted. Assistive devices like canes or braces may be needed to walk.
Risk Factors You Should Know
Age and Gender
OA risk increases after age 45. Women are more likely than men to develop foot OA, especially after menopause, due to hormonal changes affecting joint health.
Prior Foot Injuries
A history of ankle sprains, fractures, or dislocations significantly raises the risk of post-traumatic OA. Even injuries that healed well can lead to joint degeneration years later.
Obesity and Joint Load
Excess body weight dramatically increases pressure on foot joints. Each pound of body weight exerts about 4 pounds of force on the feet during walking. Weight loss can reduce pain and slow OA progression.
Foot Structure Issues
Abnormal foot mechanics increase joint stress. Conditions like:
– Flat feet (pes planus)
– High arches (pes cavus)
– Bunions or hammertoes
…can all contribute to early OA development by altering weight distribution.
Complications of Untreated OA
Hallux Rigidus
This is the end-stage of big toe OA, where the joint becomes stiff or fused. It severely limits gait and often requires surgery to relieve pain.
Bunions (Hallux Valgus)
OA can destabilize the big toe joint, causing it to drift toward the second toe. This creates a bony prominence that rubs against shoes, leading to inflammation and pain.
Corns and Calluses
As joints protrude, shoes press against them, causing thickened skin. Calluses form over wide pressure areas, while corns develop on bony points. Both can be painful and lead to skin breakdown.
Arch Collapse
Degeneration in the midfoot can cause the medial arch to flatten, altering gait and increasing strain on other joints. This acquired flatfoot deformity worsens OA and may require orthotics or surgery.
How Diagnosis Works
Physical Exam Findings
A doctor will check for:
– Tenderness when pressing on joints
– Swelling or warmth
– Range of motion in the toes and midfoot
– Gait abnormalities
– Comparison between both feet
They may also observe how you walk to detect joint stiffness or compensatory movements.
X-Ray Detection
X-rays are the primary diagnostic tool for foot OA. They reveal:
– Joint space narrowing
– Bone spurs (osteophytes)
– Subchondral sclerosis (bone hardening)
– Cysts near the joint
These changes confirm OA and help determine its stage.
MRI for Early or Complex Cases
If X-rays are inconclusive or surgery is being considered, an MRI can detect:
– Early cartilage damage
– Bone marrow lesions
– Soft tissue inflammation
It’s especially useful for assessing midfoot or ankle OA before structural changes appear on X-ray.
When to See a Doctor
Persistent Pain Beyond One Week
If foot pain lasts more than 7 days without improvement, it’s time to get evaluated. Early intervention can prevent irreversible joint damage.
Difficulty Wearing Shoes
Pain or pressure from shoes—especially over a bony bump—suggests structural changes. A podiatrist can recommend proper footwear or orthotics.
Trouble Walking Normally
If you’re limping, avoiding stairs, or needing to rest frequently while walking, OA may be impacting your function. Don’t wait—early treatment improves outcomes.
Effective Management Strategies
Low-Impact Exercise Routine
Regular movement keeps joints lubricated and muscles strong. The CDC recommends:
– 150 minutes of moderate aerobic activity weekly (e.g., walking, swimming)
– Strength training 2+ days per week
– Daily stretching to maintain joint flexibility
Avoid high-impact activities like running that accelerate joint wear.
Weight Management for Joint Relief
Losing even 5–10% of body weight can significantly reduce foot pain. Every pound lost removes 4 pounds of pressure from your joints during walking.
Supportive Footwear Essentials
Wear shoes that:
– Have a low heel (≤1 inch)
– Offer a wide toe box
– Provide firm heel support
– Include cushioned soles
– Feature arch support
Rocker-bottom shoes are ideal—they reduce pressure on the top of the foot by allowing smooth roll-off during walking.
Custom Orthotics and Insoles
Over-the-counter or custom-made insoles can:
– Cushion painful joints
– Support collapsing arches
– Improve foot alignment
– Reduce strain on OA-affected areas
A podiatrist can prescribe or mold orthotics to your foot shape.
Medical and Surgical Options
Pain Relief Medications
- Acetaminophen (paracetamol): First choice for mild pain
- Topical NSAIDs (e.g., diclofenac gel): Reduce inflammation with minimal side effects
- Oral NSAIDs (e.g., ibuprofen): Use short-term due to stomach and heart risks
- Steroid injections: Provide temporary relief (weeks to months) but shouldn’t be repeated often
Surgical Interventions
Surgery is considered when pain persists despite conservative care.
Arthroscopy and Debridement
Minimally invasive procedure to:
– Remove bone spurs
– Clean out damaged cartilage
– Smooth joint surfaces
Used for early to moderate OA, especially in the big toe.
Arthrodesis (Joint Fusion)
Fuses bones to eliminate painful motion. Commonly used for:
– Advanced midfoot OA
– Severe hallux rigidus
– Ankle arthritis
It’s effective for pain relief but reduces joint flexibility.
Joint Replacement (Arthroplasty)
Replaces damaged joint surfaces with implants. Most common in ankles, less so in toes. Lasts about 10 years and may require revision.
Bunion Correction
If OA leads to hallux valgus, surgery can realign the toe, remove the bony bump, and improve function.
Osteoarthritis in the foot joints is a progressive but manageable condition. Recognizing early signs—like activity-related pain, stiffness, swelling, or a bony bump on the foot—can help you take control before joint damage becomes severe. With proper footwear, exercise, weight management, and medical care, most people maintain mobility and reduce pain. Don’t ignore persistent foot symptoms—early diagnosis and treatment are key to preserving function and quality of life.