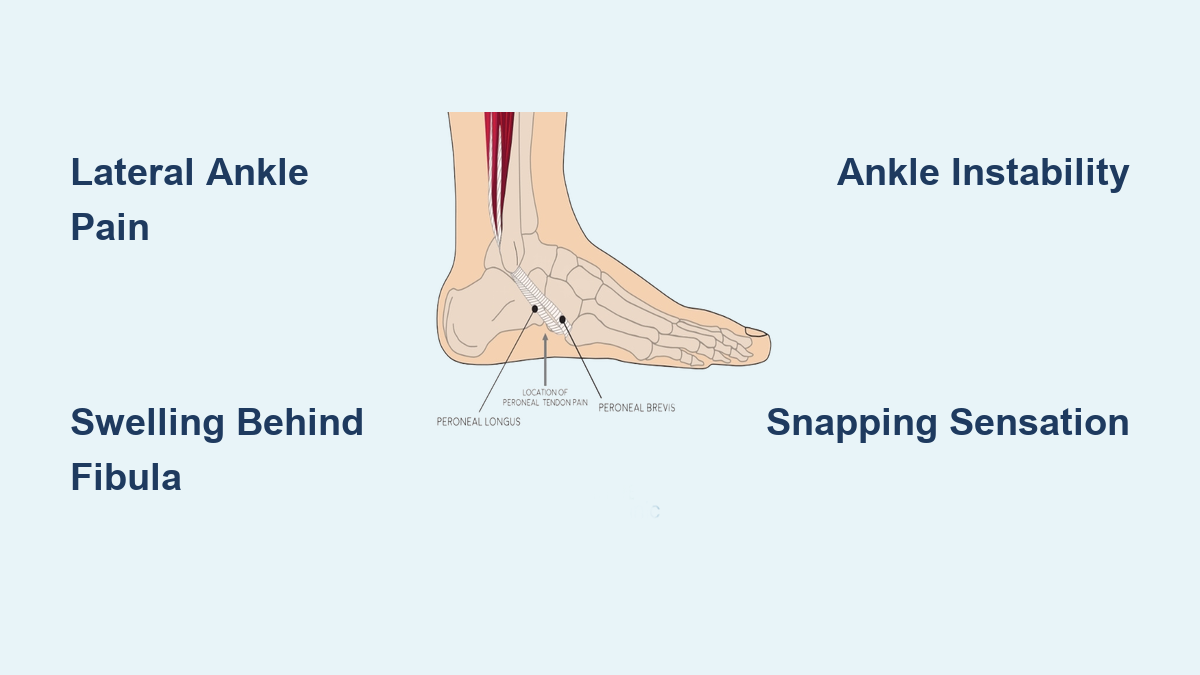
If you’ve ever rolled your ankle during a run or twisted it stepping off a curb, you might have unknowingly strained your peroneal tendon. While many dismiss lingering outer ankle pain as a simple sprain, it could actually signal a more specific and often overlooked injury: a strained peroneal tendon. These tendons—peroneus longus and brevis—run behind the fibula and are crucial for stabilizing the foot, preventing excessive inward rolling, and supporting the arch. When strained, they cause persistent pain, swelling, instability, and even a snapping sensation, significantly affecting mobility.
Unlike acute sprains that heal within days, peroneal tendon strains often linger or worsen without proper care. Because symptoms mimic those of common ankle injuries, this condition is frequently misdiagnosed, leading to prolonged discomfort and increased risk of chronic instability or tendon rupture. Recognizing the signs early—such as lateral ankle pain that flares with activity, warmth and swelling behind the fibula, or a popping feeling during movement—is essential for timely recovery. Whether you’re an athlete, dancer, or someone dealing with unexplained ankle discomfort, understanding these key indicators can help you seek the right treatment and prevent long-term damage.
Pain Along the Outer Ankle
One of the most consistent signs of a strained peroneal tendon is localized pain along the outer side of the ankle, specifically behind and below the lateral malleolus—the bony bump you can feel on the outside of your ankle. This isn’t generalized soreness; it follows the precise path of the peroneal tendons, making it distinct from typical ankle sprains that often affect the front or side of the joint.
Sharp or Dull Pain With Activity
The pain typically worsens during movement, especially with activities that stress the outer ankle:
– Walking on uneven ground
– Pushing off the toes while running or climbing stairs
– Making quick cuts or pivots in sports
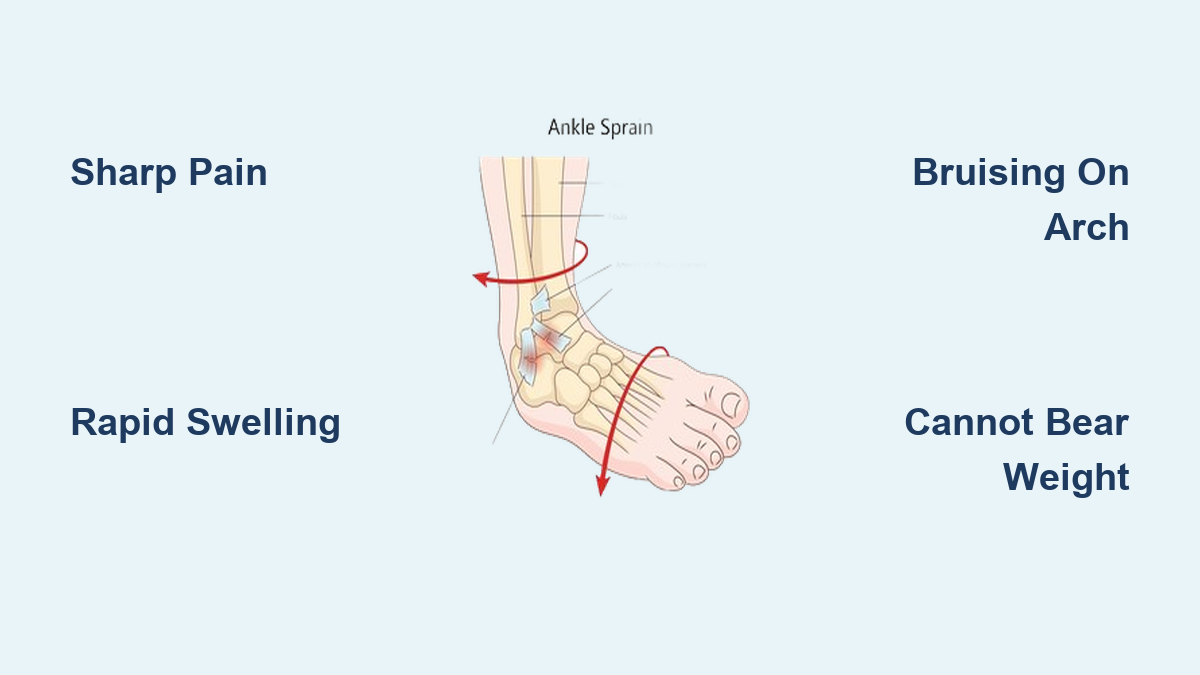
In acute cases, the pain starts suddenly after an ankle roll or twist, often accompanied by a pop. In chronic strains, it develops gradually and may only appear after prolonged activity. Some people describe a sharp, stabbing sensation during movement, while others experience a deep, aching throb that persists even at rest. The discomfort may be mild at first but intensifies with continued use, especially in runners or athletes who don’t modify their training.
Pain That Radiates Down the Foot
As the injury progresses, pain may radiate along the outer edge of the foot or slightly up the lower leg. This occurs because the two peroneal tendons follow different paths: the peroneus longus travels under the foot to the base of the big toe, while the peroneus brevis attaches to the fifth metatarsal on the outer midfoot. Damage to either tendon can refer pain beyond the ankle.
Key signs to watch for:
– Tenderness when pressing along the tendon sheath
– Increased pain when the foot is stretched inward (passive inversion)
– Discomfort that lingers after exercise or returns quickly upon resuming activity
This radiating pain is often mistaken for plantar fasciitis or nerve issues, but its connection to ankle movement and lateral tenderness points strongly to peroneal involvement.
Swelling and Tenderness Behind the Ankle
Visible or palpable swelling behind the outer ankle is a hallmark of peroneal tendon irritation. Unlike the diffuse puffiness seen with a mild sprain, this swelling is localized, often appearing as a defined bulge along the tendon’s path. It may develop immediately after an injury or build up gradually with overuse.
Localized Inflammation and Warmth
The area may feel warm to the touch, signaling active inflammation—a common sign of peroneal tendinitis. This is especially noticeable after physical activity and may be accompanied by redness or mild skin sensitivity.
Check for:
– Swelling that increases with activity and decreases with rest
– Persistent tenderness when touching the back of the lateral malleolus
– Discomfort when wearing tight shoes that press on the area
If swelling occurs without a clear injury, consider overuse as the likely cause—common in runners, dancers, or individuals who recently increased their physical activity. Ignoring this sign can lead to chronic inflammation and tendon degeneration.
Ankle Instability and Weakness
A strained peroneal tendon compromises your ankle’s dynamic stabilizers, leading to a sensation that the joint might “give way.” This isn’t just discomfort—it’s functional weakness that affects balance, coordination, and confidence in movement.
Feeling of Ankle Collapse
You may feel unsteady, especially when:
– Walking on slopes or uneven surfaces
– Making quick directional changes
– Standing on one foot
This instability happens because the peroneal tendons help control inversion (inward rolling) of the ankle. When they’re injured, the ankle loses critical support, increasing the risk of repeated sprains and falls.
Weakness During Foot Eversion
Try this simple test: Sit with your leg extended and press the outside of your foot outward against resistance (like a hand or wall). If it feels weak or painful, the peroneal tendons are likely compromised.
Other signs include:
– Difficulty performing a single-leg heel raise
– Noticeable strength difference between ankles
– Fatigue in the outer calf during prolonged standing
This weakness often goes unnoticed until daily activities become challenging, but it’s a key indicator of tendon dysfunction.
Popping or Snapping Sensation

A snapping or popping feeling along the outer ankle is a red flag for peroneal tendon subluxation—where the tendon slips out of its groove behind the fibula. While not always painful, this sensation should never be ignored.
Audible Snap During Movement
You might hear or feel a pop when rotating the ankle, pushing off the foot, or rising onto your toes. In acute injuries, a loud pop at the moment of trauma may indicate a partial or complete tendon tear. In chronic cases, the snap recurs with certain motions and may eventually become visible as the tendon dislocates.
Associated With Acute Trauma or Overuse
Subluxation often follows:
– A sudden inversion injury (rolling the ankle inward)
– Repetitive strain from sports like basketball, tennis, or dancing
– Anatomical variations like a shallow fibular groove
Repeated subluxation can lead to permanent tendon damage, chronic dislocation, or degenerative changes over time.
Difficulty Bearing Weight
When the peroneal tendons are strained, weight-bearing becomes painful and inefficient. This isn’t just about discomfort—it reflects a breakdown in normal gait mechanics.
Pain During Push-Off Phase
The most intense pain often occurs during the push-off phase of walking or running, when the peroneal tendons are most active. You may notice:
– Limping to avoid full weight on the foot
– Shortened stride on the affected side
– Avoidance of jogging, climbing stairs, or standing for long periods
Altered Gait to Compensate
To protect the injured tendon, your body adapts—sometimes unconsciously. You might walk on the inner foot, shift weight to the other leg, or reduce ankle motion. These compensations can lead to secondary issues in the knee, hip, or lower back over time.
Risk Factors for Peroneal Tendon Strain

Certain conditions increase your likelihood of developing this injury:
– High arches (pes cavus): Place more stress on the outer ankle
– Hindfoot varus: Heel tilts inward, forcing tendons to work overtime
– Previous ankle sprains: Lead to chronic instability and tendon overuse
– Tight calf muscles: Limit ankle motion and increase load on peroneals
– Sports with repetitive lateral motion: Tennis, basketball, running, dancing
Wearing unsupportive shoes or suddenly increasing training intensity also raises the risk.
Diagnostic Challenges and Misdiagnosis
Peroneal tendon injuries are commonly misdiagnosed as lateral ankle sprains because symptoms overlap. Standard X-rays appear normal since they don’t show soft tissue damage, leading many to believe the injury is minor. However, persistent pain beyond 1–2 weeks suggests a deeper issue.
Key Differentiators
To distinguish a peroneal strain:
– Pain location: Behind and below the lateral malleolus (not just in front)
– Pain with resisted eversion: Reproduces symptoms
– Snapping sensation: Suggests subluxation
– Chronicity: Persists beyond typical sprain recovery
If your “sprain” isn’t healing, a peroneal tendon evaluation is crucial.
When to See a Doctor
Seek medical attention if:
– Pain lasts more than 7–10 days
– You can’t bear weight or walk normally
– You notice visible deformity or tendon shifting
– There’s no improvement with rest, ice, and elevation
Immediate evaluation is needed for suspected ruptures or subluxation.
Imaging and Professional Diagnosis

Accurate diagnosis requires more than a physical exam:
– Ultrasound: Real-time imaging that detects swelling, tears, and subluxation
– MRI: Gold standard for soft tissue detail, showing tendinosis, partial tears, and surrounding pathology
A healthcare provider will also assess tenderness, strength, gait, and perform dynamic tests like the dressage maneuver (forced dorsiflexion and eversion) to reproduce symptoms.
Potential Complications
Untreated strains can lead to:
– Chronic ankle instability
– Tendon rupture
– Development of ankle arthritis
– Long-term mobility issues
Prevention and Recovery Tips
Immediate Self-Care
- Rest: Avoid aggravating activities
- Ice: 15–20 minutes every 2–3 hours
- Compression: Use a supportive wrap
- Elevation: Keep foot above heart level
Physical Therapy
- Eccentric strengthening
- Balance and proprioception training
- Calf stretching
- Gait retraining
Footwear and Orthotics
- Wear shoes with firm heel counters and lateral support
- Consider custom orthotics if you have high arches or hindfoot varus
Final Note: A strained peroneal tendon is more than just lingering ankle pain—it’s a sign of compromised stability and function. Recognizing the key signs—lateral ankle pain, swelling, weakness, and snapping—can prevent misdiagnosis and long-term damage. Early intervention with rest, proper diagnosis, and targeted rehab offers the best chance for full recovery. If your ankle pain persists beyond a typical sprain, don’t wait—see a foot and ankle specialist for an accurate assessment.