You’re relaxing on the couch, feet up, muscles unwinding—when out of nowhere, a sharp, burning, or throbbing pain jolts through your arch. No injury. No recent workout. Just stillness—followed by pain. This isn’t normal. Sudden arch pain while resting is a warning sign. Unlike discomfort from overuse, rest-triggered pain often points to deeper issues like nerve irritation, microtrauma, or chronic inflammation that only become apparent when movement stops.
This kind of pain isn’t just “wear and tear.” It’s your body signaling that something is wrong—whether it’s a strained tendon, compressed nerve, or even a hidden stress fracture. The absence of activity makes internal changes more noticeable, turning quiet moments into painful alerts.
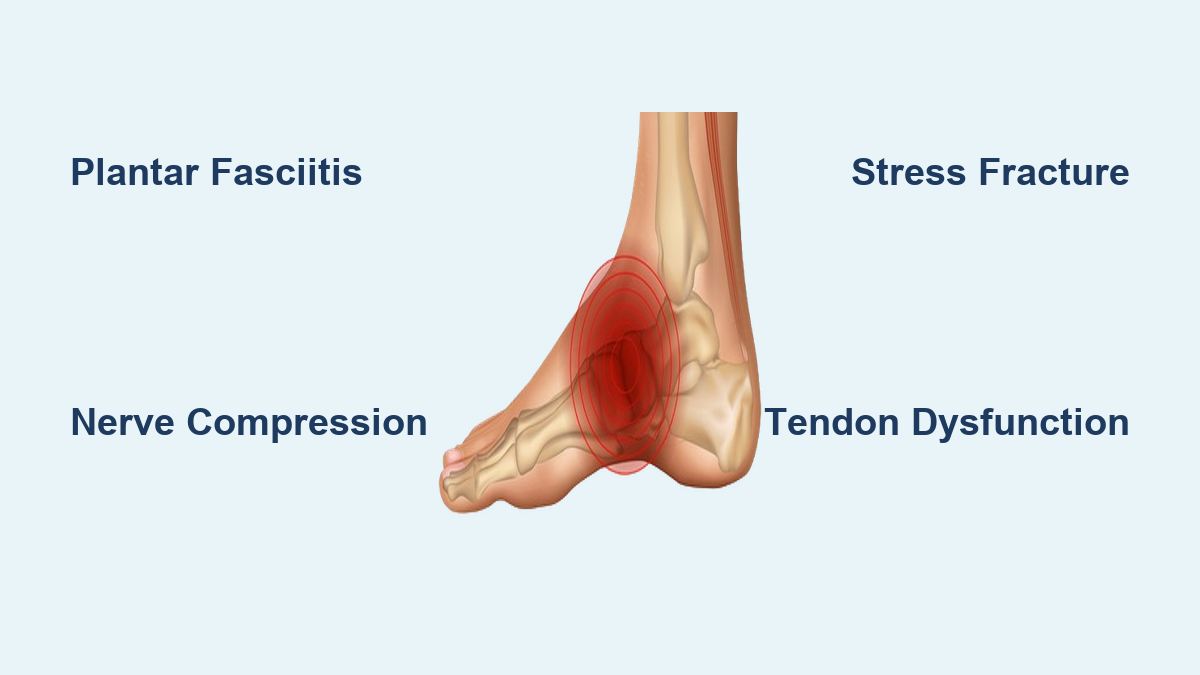
In this guide, we’ll break down the real causes of sudden arch pain at rest, based on clinical evidence and patient patterns. You’ll learn how to distinguish between plantar fasciitis flare-ups, nerve compression, tendon damage, and other serious but often overlooked conditions. Most importantly, you’ll discover how to assess your symptoms, when to act, and when to seek professional help—before temporary discomfort becomes long-term disability.
Plantar Fasciitis: Why It Hurts When You’re Not Moving

Despite being linked to walking, plantar fasciitis is one of the most common causes of sudden arch pain at rest. The secret lies in what happens when you stop moving.
When you sit or lie down for long periods, the inflamed plantar fascia tightens and shortens. Even minor shifts—like flexing your toes or adjusting your foot—can pull on this already damaged ligament, triggering a sharp, stabbing pain in the arch or heel. This explains why many people feel a jolt of pain upon waking or after hours of sitting, even without stepping down.
Key Signs It’s Plantar Fasciitis
- Pain type: Sharp, stabbing, or burning under the medial arch or inner heel
- Timing: Flares after rest, especially first thing in the morning
- Improves slightly with walking as the fascia stretches
- Worsened by tight calf muscles or flat feet
How to Self-Check
- Tenderness when pressing on the inside of the heel
- Pain increases when you passively stretch your big toe upward
- Relief from rolling a frozen water bottle under the foot
Pro tip: If extending your big toe causes arch pain while seated, you’re likely experiencing the Windlass effect—a telltale sign of plantar fasciitis.
Nerve Compression: Burning, Tingling Pain at Night

If your arch pain feels like electric shocks, numbness, or “pins and needles,” especially at night, nerve entrapment could be the culprit.
Tarsal Tunnel Syndrome: The Silent Nighttime Agony
Compression of the posterior tibial nerve behind the inner ankle can send radiating pain into the arch—without any movement required. Similar to carpal tunnel syndrome, symptoms worsen at rest, when external sensations fade and nerve signals become more prominent.
Symptoms of Nerve Involvement
- Burning or tingling in the arch, sole, or toes
- Foot cramps while lying down
- Numbness spreading across the bottom of the foot
- Pain intensifies at night or after leg elevation
How to Test at Home
- Tinel’s Test: Tap gently behind your inner ankle. If you feel tingling or shooting pain in the arch, the nerve is irritated.
- Risk factors: Flat feet, diabetes, ankle swelling, or prior sprains
Expert insight: Nerve pain doesn’t need activity to flare. Inflammation around the nerve can cause spontaneous firing, leading to sudden pain even while resting.
Posterior Tibial Tendon Dysfunction (PTTD): The Hidden Arch Collapse
The posterior tibial tendon is your arch’s main support. When it weakens, the arch begins to collapse—leading to aching pain that lingers after activity and often flares during rest.
Early-Stage PTTD: The Quiet Progression
In Stage I, damage is reversible. But pain often appears hours after walking, including during evening rest. Why? Inflammation continues even when you’re off your feet.
Warning Signs of PTTD
- Dull ache along the inner arch and ankle
- Foot fatigue or a “dragging” sensation
- Arch flattens when standing, partially recovers when sitting
- Pain or weakness during a single heel raise
Why It Hurts at Rest
- Swollen tendon sheath presses on nearby nerves
- Micro-instability in foot joints becomes noticeable when muscles relax
- Inflammatory chemicals build up post-activity, causing delayed pain
Critical note: Untreated PTTD leads to permanent flatfoot deformity. Early diagnosis is essential.
Stress Fractures: Throbbing Pain Without Weight

A stress fracture usually hurts with walking—but in cases of insufficiency fractures (due to osteoporosis or metabolic issues), pain often builds at rest, especially at night.
The Rest Pain Paradox
When bone micro-damage occurs, edema and bleeding inside the bone increase pressure in the marrow. This pressure becomes more noticeable when you’re still—similar to a toothache that worsens when lying down.
How to Spot a Stress Fracture
- Deep, throbbing, localized pain in the arch
- Point tenderness over a specific bone (navicular, cuboid, cuneiform)
- Heel tap test: Pain flares when you gently tap the heel
- Imaging: X-rays may miss early fractures; MRI or bone scan is needed
Red flag: If you have osteoporosis, take steroids, or have a history of low-impact injuries, even minor strain can cause a fracture.
Cavus Foot: High Arches, Hidden Cramps
High arches (cavus foot) create instability, concentrating pressure on the heel and ball of the foot. But pain isn’t just from walking—tight plantar structures can spasm at rest.
Why High Arches Hurt While Still
- Chronic shortening of the plantar fascia and foot muscles
- Muscle cramps or spasms in the arch while lying down
- Reduced blood flow to overstressed tissues during inactivity
Signs You Have Cavus Foot
- Visibly high arch, even when sitting
- Calluses under the ball of the foot
- Hammertoes or claw toes
- Associated with neurological conditions (e.g., Charcot-Marie-Tooth, stroke)
Note: If your pain includes muscle twitching or weakness, a neurological evaluation may be needed.
Tendonitis: Delayed Aching in the Arch
Flexor hallucis longus and flexor digitorum longus tendons run under the arch. When inflamed, they cause aching or sharp pain that may flare hours after activity, including during rest.
Why Inflammation Lingers
- Tendons have poor blood supply, slowing healing
- Inflammatory fluid accumulates in the sheath, causing delayed pain
- Pain worsens with toe flexion or resisted movement
How to Test at Home
- Resist toe curling: If it causes arch pain, tendonitis is likely
- Look for swelling or crepitus (grinding) under the arch
Common in: Runners, dancers, or those who suddenly increase activity
Arthritis: Stiffness That Flares After Rest
Osteoarthritis, rheumatoid arthritis (RA), or post-traumatic arthritis in the midfoot joints can cause aching, throbbing arch pain that worsens after inactivity.
Nighttime Arthritis Pain
- Joint swelling and synovial fluid buildup increase pressure
- Pain flares after rest, improves slightly with gentle movement
- Morning stiffness lasting over 30 minutes suggests RA
Diagnostic Clues
- X-ray: Shows joint narrowing, bone spurs, or erosions
- Blood tests: Elevated CRP, ESR, or rheumatoid factor (RF) if RA suspected
- Pain localized to midfoot joints (naviculocuneiform, tarsometatarsal)
Key insight: Arthritis pain isn’t just weight-bearing. Capsular distension at rest can trigger deep aching.
Lisfranc Injury: The Missed Midfoot Crisis

A Lisfranc injury involves ligament tears or fractures in the midfoot. While typically painful with walking, minor or chronic cases may cause intermittent arch pain at rest due to joint instability.
Subtle Signs You Might Miss
- Central midfoot pain, often mistaken for a sprain
- Bruising on the sole of the foot (a major clue)
- Pain lingers after activity, flares when sitting
How to Diagnose
- Weight-bearing X-ray: Shows bone separation (diastasis)
- Piano key test: Upward movement of metatarsal heads indicates instability
- MRI or CT: Confirms ligament or bone damage
Urgency: Undiagnosed Lisfranc injuries lead to arthritis and chronic disability.
Peroneal Tendon Issues: Lateral Arch Pain
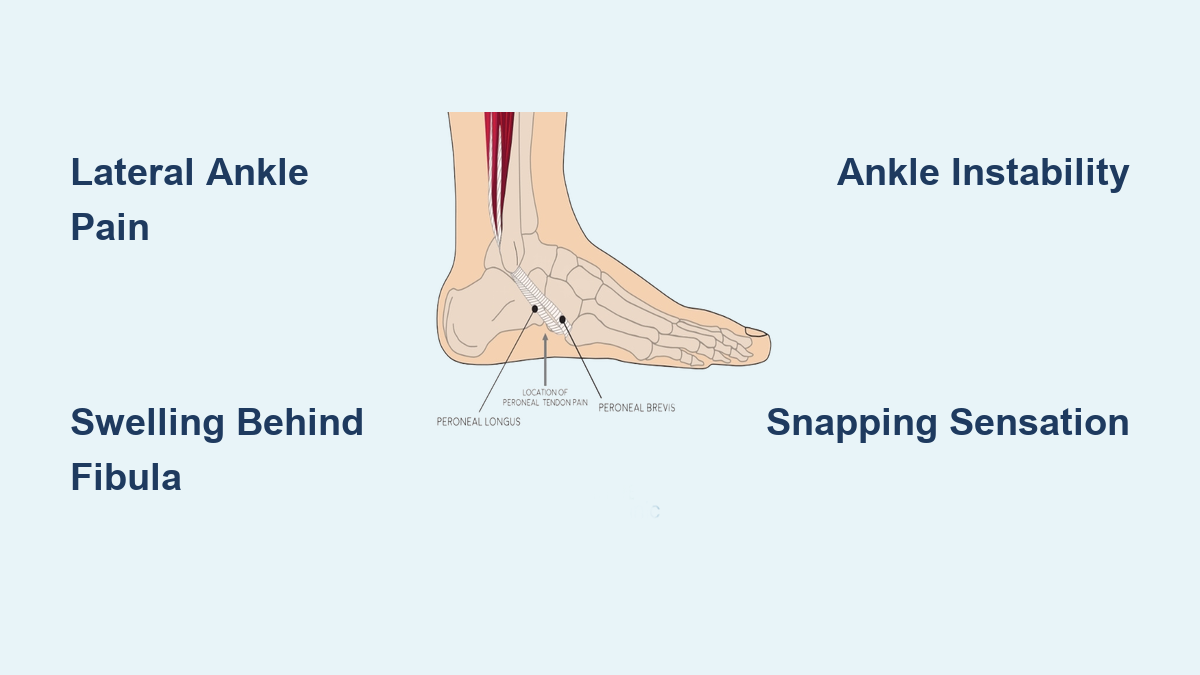
Though peroneal tendons run behind the outer ankle, peroneus longus crosses the foot and can refer pain to the lateral arch. Inflammation may cause aching at rest, especially after activity.
Key Indicators
- Pain on the outer side of the arch
- Swelling behind the lateral malleolus
- History of ankle instability or sprains
Confirmation
- MRI: Shows tendinopathy, tears, or subluxation
- Pain worsens with resisted eversion of the foot
Risk Factors That Trigger Rest Pain
Certain factors increase your risk of sudden arch pain at rest:
| Risk Factor | How It Contributes |
|---|---|
| Weight gain | Increases load on arch structures |
| Poor footwear | Lack of support leads to microtrauma |
| Flat feet | Overpronation strains tendons and fascia |
| Age > 40 | Connective tissue degeneration |
| Diabetes | Nerve damage and poor healing |
| Sedentary lifestyle | “Weekend warrior” syndrome causes micro-injuries |
Prevention tip: Supportive shoes and daily calf stretching reduce risk across all causes.
When to See a Doctor Immediately
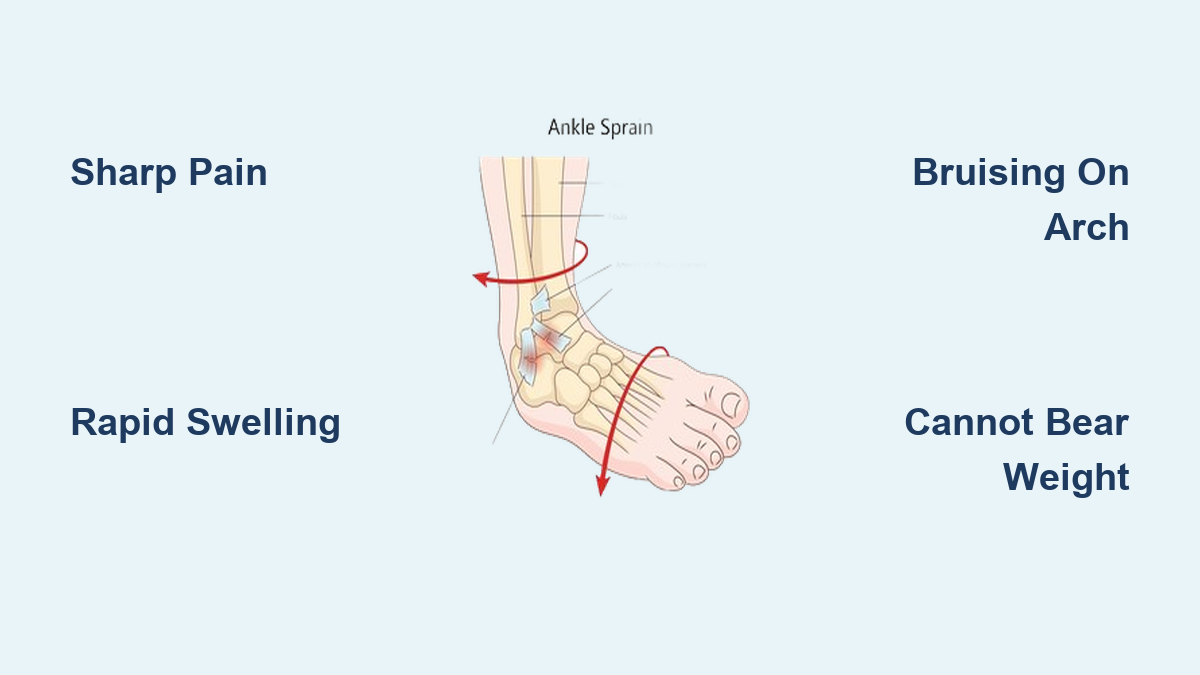
Don’t wait if you have:
- Inability to bear weight or walk normally
- Visible swelling, bruising, or deformity
- Numbness, tingling, or loss of sensation
- History of trauma (fall, twist)
- Pain lasting >1–2 weeks despite rest
- Fever or redness (possible infection)
Go to the ER If:
- Suspected Lisfranc injury
- Tendon rupture (heard a “pop,” sudden weakness)
- Open wound or signs of infection
How Doctors Diagnose Resting Arch Pain
Step 1: Medical History
- Onset: Sudden or gradual?
- Timing: Worse at rest, night, or morning?
- Associated conditions: Diabetes, arthritis, neuropathy?
Step 2: Physical Exam
- Palpation: Tenderness at plantar fascia, navicular, tendons
- Arch assessment: Wet test or visual inspection
- Special tests:
- Windlass test (big toe extension)
- Tinel’s sign (nerve tapping)
- Single heel raise (PTTD check)
Step 3: Imaging
- X-ray: Rule out fractures, arthritis, bone spurs
- MRI: Best for soft tissue (tendons, ligaments, nerves)
- Ultrasound: Dynamic view of tendons and fascia
- Bone scan: If stress fracture is suspected but X-ray is normal
Step 4: Neurological Tests
- EMG/NCS: Confirms tarsal tunnel syndrome or nerve damage
Sudden arch pain while resting is not normal—and it’s not just “wear and tear.” It’s a signal. Whether it’s plantar fasciitis tightening overnight, a nerve firing at rest, or a hidden stress fracture, the cause must be identified early. Ignoring it risks chronic pain, foot deformity, or long-term disability.
Start with rest, ice, and supportive footwear. Stretch your calves and arches daily. If pain persists beyond a week, see a podiatrist or orthopedic specialist. With the right diagnosis, most causes are treatable—often without surgery.
Don’t let your feet pay the price of inaction. Your arch pain has a cause. Find it. Fix it. Move freely again.