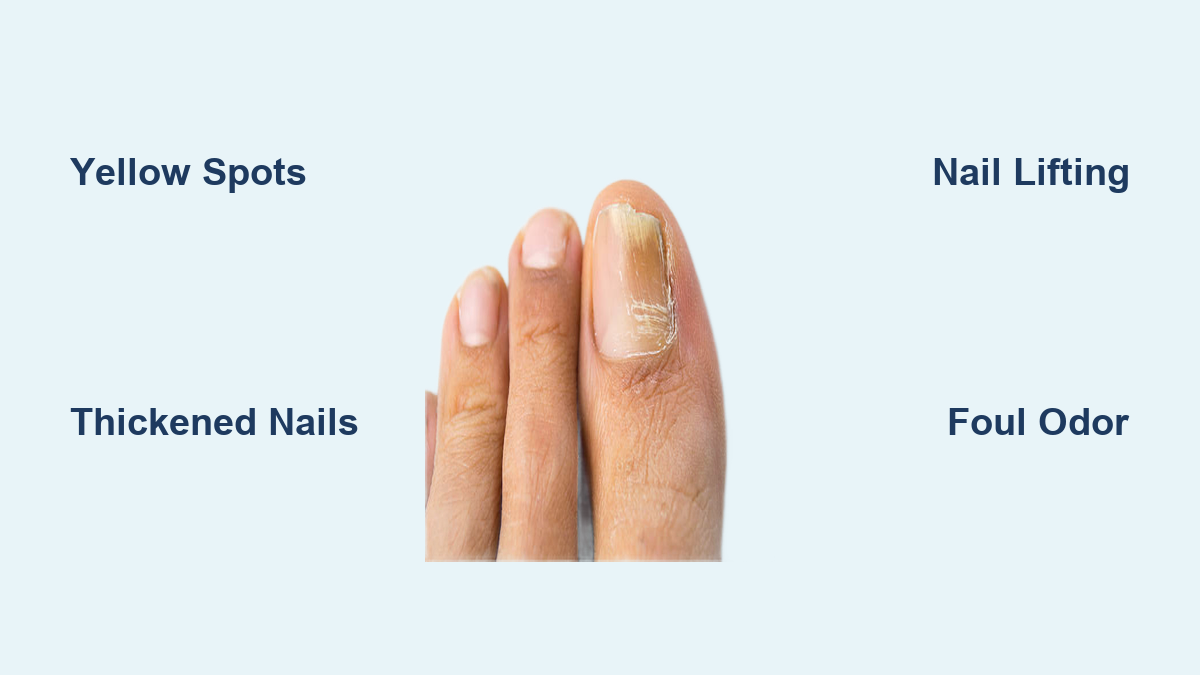
You trim your toenail and notice it’s yellow, thick, and crumbling at the edge. It doesn’t hurt—yet—but something feels off. You’ve seen this before in others: nails that look old, damaged, or stained. What you’re seeing could be onychomycosis, the medical term for a fungal nail infection. Affecting up to 13.8% of adults in North America and as many as 50% of people over 70, fungal nail infections are more than a cosmetic concern—they can lead to pain, disability, and complications, especially in those with diabetes or weakened immune systems.
Fungal nail infections develop slowly, often starting with a small discoloration that gradually worsens. Because symptoms mimic other conditions like psoriasis or trauma, proper identification is key. Left untreated, onychomycosis can destroy the nail, cause discomfort when walking, and even increase the risk of skin infections. The good news? Early recognition of the signs of a fungal nail infection allows for timely treatment and better outcomes. In this guide, we’ll walk through the visible and physical changes to watch for, how infections progress, and when to seek professional help.
Early Warning Signs of Onychomycosis
The first signs of a fungal nail infection are often subtle—so subtle that many people dismiss them as normal aging or minor injury. But catching these early clues can prevent the infection from spreading to other nails or causing irreversible damage.
Yellow or White Spots Under the Nail
One of the earliest indicators is a small yellow, white, or brown spot appearing under the tip or side of the nail. This discoloration typically begins at the distal (free) edge or lateral (side) border and slowly creeps toward the cuticle. In infections caused by dermatophytes—responsible for 70–90% of cases—the color is usually yellow-brown. If the discoloration is white and on the surface, it may indicate white superficial onychomycosis, where fungus invades the top layer of the nail and can sometimes be scraped away.
Pro Tip: Shine a flashlight or phone light from beneath the nail. Early subungual (under-nail) changes are easier to spot with backlighting.
Surface Patches That Can Be Scraped Off
In white superficial onychomycosis, the infection stays confined to the outermost layer of the nail plate. You might notice chalky, white patches that look like powder. Unlike deeper infections, these areas can often be lightly scraped off with a nail file. This form is less common in adults but more frequent in children and swimmers exposed to damp environments.
Avoid aggressive scraping, which can damage the nail and spread infection. Instead, monitor changes and consult a healthcare provider for confirmation.
Progressive Nail Changes in Fungal Infections

As the fungus spreads deeper into the nail bed and matrix, structural damage becomes more apparent. These changes are hallmarks of moderate to advanced onychomycosis.
Thickened, Woody Nails
One of the most recognizable signs is nail thickening. The nail becomes hard, dense, and difficult to cut—often requiring heavy-duty clippers or professional trimming. This results from subungual hyperkeratosis, a buildup of keratin debris underneath the nail.
- In lighter skin tones, thickened nails often appear yellow or brown.
- In darker skin tones, the discoloration may present as dark brown or gray, sometimes mistaken for trauma or melanoma.
Thickening impairs nail function and increases pressure inside shoes, leading to discomfort over time.
Brittle, Crumbly, or Split Nails
Infected nails lose their strength and elasticity. They become brittle, ragged, or crumble easily when pressed or trimmed. You may notice:
– Longitudinal splitting (cracks from base to tip)
– Transverse breaks (across the nail)
– Jagged edges or flaking at the surface
This fragility occurs because fungi digest the keratin that gives nails their structure. The more extensive the infection, the greater the breakdown.
Warning: Never attempt to pull off loose pieces. This can cause bleeding, pain, or secondary bacterial infection.
Structural and Positional Changes in Infected Nails

Fungal invasion doesn’t just alter color and texture—it can distort the entire shape and position of the nail.
Nail Lifting From the Bed (Onycholysis)
Onycholysis is when the nail separates from the underlying nail bed, starting at the tip and moving backward. The gap created is often opaque, yellow, or greenish, and may trap dirt, sweat, and microbes.
- Separation allows moisture to accumulate, creating a perfect environment for fungal and bacterial growth.
- If the space turns green, suspect Pseudomonas aeruginosa—a common bacterium that thrives in moist, oxygen-poor spaces.
Onycholysis is common in distal lateral subungual onychomycosis (DLSO), the most prevalent form of the infection.
Distorted or Claw-Like Nails
As the infection advances, the nail may lose its natural flat shape and become misshapen, curved, or excessively thickened. In neglected cases, onychogryphosis develops—a claw-like deformity where the nail grows long, twisted, and horn-shaped.
This condition results from:
– Chronic fungal damage
– Lack of trimming
– Abnormal pressure from shoes
It’s more common in elderly individuals or those with mobility issues who can’t care for their nails properly.
Sensory and Secondary Symptoms of Onychomycosis
While early onychomycosis is usually painless, advanced stages can cause noticeable discomfort and lead to complications.
Pain When Walking or Wearing Shoes
Thickened, distorted nails press against footwear, causing soreness, tenderness, or sharp pain with each step. The pressure can also lead to:
– Ingrown toenails
– Calluses under the nail
– Reduced mobility, especially in older adults
Patients often report changing shoe size or switching to open-back footwear to relieve pressure.
Foul, Musty Odor From the Nail
A persistent, unpleasant smell—often described as sour, cheesy, or musty—can emanate from the infected nail. This odor comes from metabolic byproducts of fungal growth and trapped debris beneath the nail.
Regular washing won’t eliminate the smell, as it originates deep within the nail unit.
Note: Strong odor combined with green discoloration suggests bacterial co-infection, which may require antibiotics.
Swollen, Tender Skin Around the Nail
Inflammation of the nail fold—called paronychia—is a red flag, especially if:
– The skin is red, swollen, and painful
– There’s pus or drainage
– The nail lifts away
Paronychia is particularly common in Candida onychomycosis, which affects fingernails more often and is seen in people with:
– Frequent hand immersion in water
– Diabetes
– Immunosuppression
Unlike bacterial paronychia, fungal versions tend to be chronic and recurrent.
Advanced and Severe Cases of Fungal Nail Infection

When onychomycosis goes untreated for months or years, it can lead to irreversible damage.
Complete Nail Loss or Dystrophy
In end-stage infection, the nail may:
– Detach partially or fully
– Crumble into fragments
– Fail to regrow properly
This condition, known as total dystrophic onychomycosis (TDO), represents the final stage of long-standing infection. Even after successful antifungal treatment, the nail matrix may be permanently damaged, resulting in abnormal or absent nail growth.
Black or Green Discoloration
While yellow-brown is typical of dermatophyte infections, black, green, or blue-green hues suggest other causes:
– Green: Pseudomonas infection under a lifted nail
– Black: Mixed fungal-bacterial infection or, rarely, subungual melanoma (a serious skin cancer)
Urgent: A new, dark streak in a single nail—especially with pigmentation on the skin around it (Hutchinson’s sign)—requires immediate dermatologic evaluation to rule out melanoma.
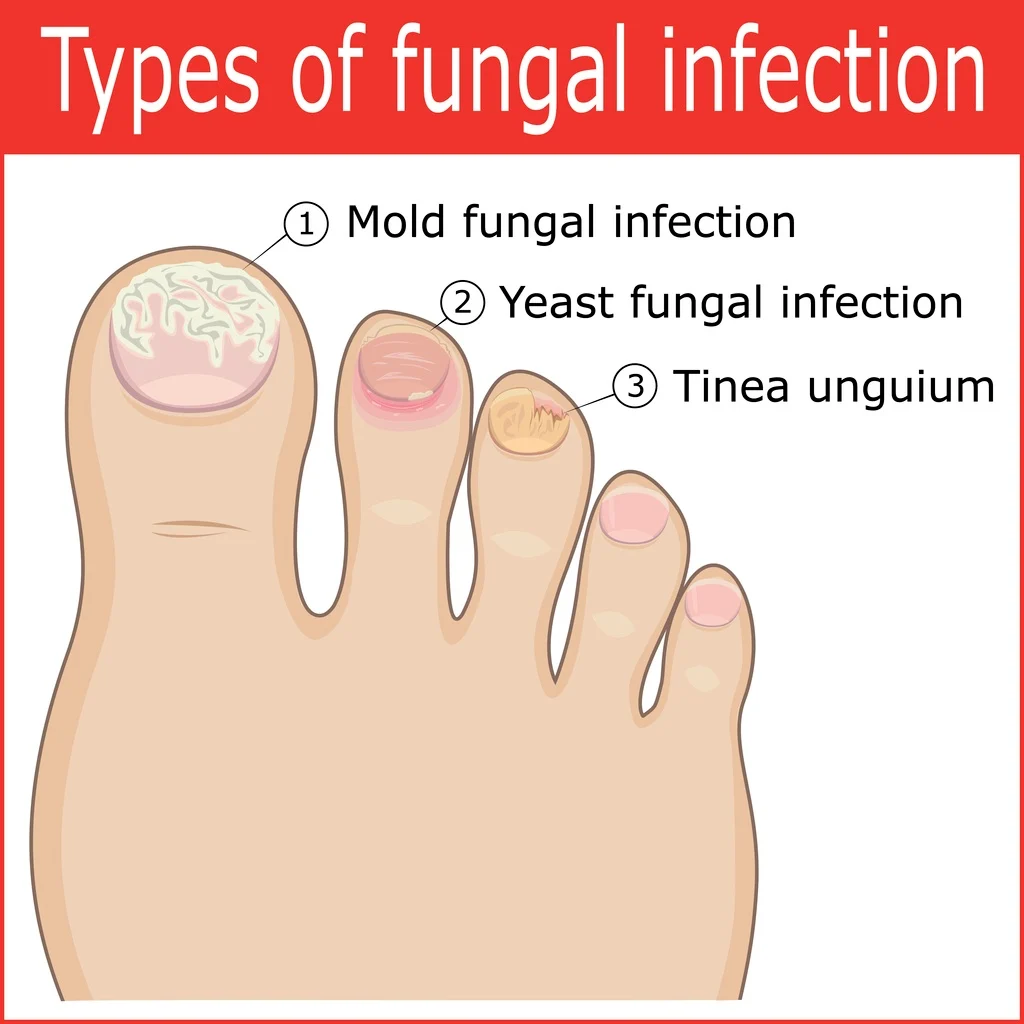
How Onychomycosis Differs by Infection Type

Not all fungal nail infections look the same. The appearance depends on the subtype of onychomycosis.
Distal Lateral Subungual Onychomycosis (DLSO)
- Most common type
- Begins with yellow-brown discoloration at the tip or side
- Progresses to thickening, debris, and onycholysis
- Affects toenails, especially the big and little toes
Proximal Subungual Onychomycosis (PSO)
- Starts near the cuticle with white or yellow spots
- Nail lifts from the base forward
- Often seen in immunocompromised individuals, including those with HIV
White Superficial Onychomycosis (WSO)
- White, powdery patches on the surface
- Can be scraped off
- More common in children and swimmers
Candida Onychomycosis
- Affects fingernails more than toenails
- Causes swollen nail folds, pain, and lifting
- Often follows chronic paronychia
When to See a Doctor for a Suspected Fungal Nail Infection
Don’t wait for pain or nail loss. Seek medical advice if you notice:
– Two or more nails showing changes
– No improvement with over-the-counter treatments
– Diabetes, poor circulation, or immune issues
– Signs of infection: redness, swelling, pus, fever
– Uncertainty about the cause—many conditions mimic fungus
A dermatologist or podiatrist can confirm the diagnosis with lab tests and recommend effective treatment.
Why Lab Testing Is Essential for Accurate Diagnosis
Over 50% of nail disorders aren’t fungal—they may be psoriasis, trauma, or cancer. That’s why lab testing is crucial before starting treatment.
KOH Test: Quick Office Check
A potassium hydroxide (KOH) preparation dissolves keratin so fungal elements can be seen under a microscope. It’s:
– Fast (results in minutes)
– Inexpensive
– Moderately sensitive (55–80%)
But it requires an experienced technician and may miss low-level infections.
Fungal Culture: Identifies the Organism
A nail clipping is grown in a lab to identify the exact fungus. Benefits:
– High specificity (99%)
– Can detect yeasts and molds
– Guides targeted therapy
Downside: Takes 2–6 weeks, and false negatives are common.
PAS Stain: Most Sensitive Histology Test
Periodic acid–Schiff (PAS) staining of nail tissue is the gold standard for detecting fungal elements in the nail plate.
– Sensitivity: 81–92%
– Detects dead or non-culturable fungi
– Often used when other tests are negative but clinical suspicion remains
Prevention Tips to Reduce Risk of Fungal Nail Infections
You can’t eliminate risk entirely, but you can significantly lower your chances.
Wear Protective Footwear in Public Areas
Always wear flip-flops or shower shoes in:
– Locker rooms
– Public pools
– Gyms
– Hotel bathrooms
These damp, warm environments are breeding grounds for fungi.
Keep Feet Dry and Clean
Moisture fuels fungal growth. To stay dry:
– Wash and dry feet daily, especially between toes
– Use antifungal powders or sprays in shoes
– Change socks daily—opt for moisture-wicking materials like wool or synthetic blends
Avoid Sharing Personal Items
Fungi spread through contact. Never share:
– Nail clippers or files
– Socks or shoes
– Towels or nail polish
Disinfect tools with 70% alcohol or bleach solution after use.
Trim Nails Properly
Cut nails straight across, not too short. Avoid digging into corners, which can cause trauma and invite infection.
Use clean, dedicated tools—and consider bringing your own to salons.
Final Note: Recognizing the signs of a fungal nail infection early—like yellow spots, thickening, or crumbling—can prevent long-term damage. While common, onychomycosis isn’t harmless. It can cause pain, limit mobility, and lead to serious complications in vulnerable individuals. If you suspect a fungal nail infection, don’t self-diagnose. See a healthcare provider for lab-confirmed diagnosis and personalized treatment. With proper care, most cases can be resolved, and recurrence reduced through consistent prevention.