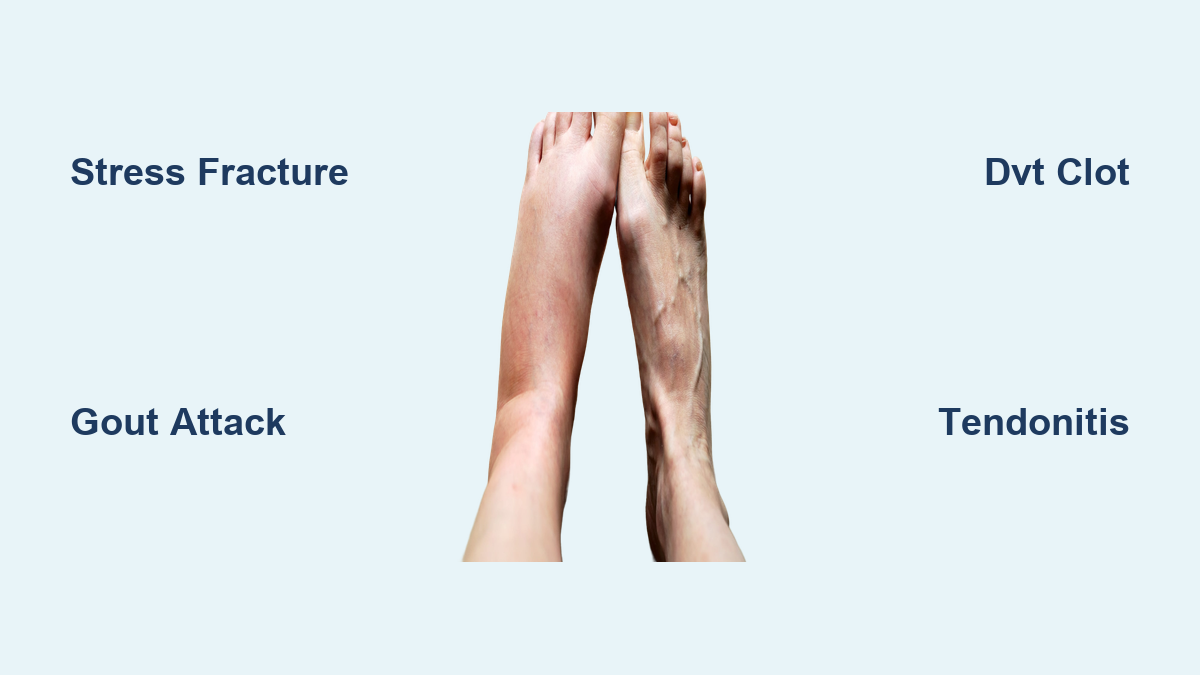
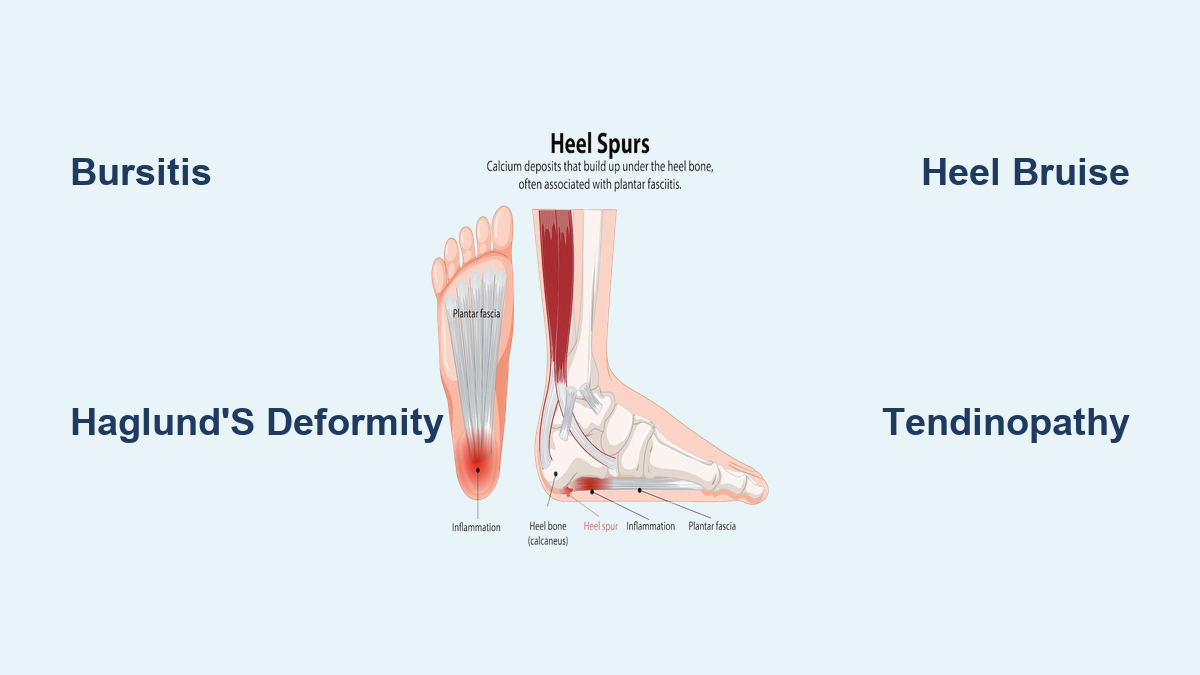
Swelling on the top of the foot isn’t just a minor annoyance—it’s often your body’s way of signaling something’s wrong. Whether it creeps in after a long day on your feet or flares up overnight with intense pain, dorsal foot swelling can stem from a wide range of causes, from simple strain to life-threatening conditions like blood clots or organ failure. The top of the foot contains delicate tendons, joints, blood vessels, and lymphatic channels—all potential sources of inflammation and fluid buildup.
Unlike ankle swelling, which is common and often linked to systemic issues, swelling specifically on the dorsum (top) of the foot tends to point to localized mechanical problems—or, in some cases, serious circulatory or inflammatory disorders. Is the swelling tender and red, or painless and firm? Did it start after wearing tight shoes, or does it appear without any obvious trigger? These details matter. Sudden, one-sided swelling could be a deep vein thrombosis (DVT), while recurrent fiery-red flares might signal gout. Bilateral swelling that worsens by evening may reflect heart, kidney, or liver disease, especially if you’re on certain medications.
In this guide, we’ll break down the most common and dangerous causes of swelling on the top of the foot, how to recognize warning signs, and when to seek urgent care. From stress fractures and tendonitis to infections, medication side effects, and systemic illnesses, you’ll learn what each symptom pattern means—and what steps to take next.
Common Injury-Related Causes

Mechanical trauma or overuse is one of the top reasons for dorsal foot swelling, especially in active individuals or those who’ve recently increased physical activity.
Stress Fractures and Acute Breaks
Small cracks in the foot bones—particularly the metatarsals, navicular, or cuneiforms—can cause visible swelling on the top of the foot. Stress fractures develop gradually from repetitive impact, common in runners or soldiers, while acute fractures result from falls or direct blows.
- Symptoms: Pain that worsens with walking, pinpoint tenderness, swelling, and sometimes bruising.
- Risk factors: High-impact sports, poor footwear, osteoporosis.
- Visual clue: A firm bulge along the midfoot or forefoot, often mistaken for a soft tissue injury.
Left untreated, stress fractures can progress to complete breaks. Diagnosis usually requires an X-ray or MRI, as early-stage fractures may not show up on initial imaging.
Extensor Tendon Inflammation
The extensor tendons, including the extensor digitorum longus and hallucis longus, run across the top of the foot and help lift the toes. Overuse or pressure from tight shoes can inflame these tendons, leading to extensor tendinitis.
- Symptoms: Dorsal swelling, tenderness along the tendon path, pain when lifting the toes.
- Triggers: Running uphill, sudden increases in activity, narrow or rigid footwear.
- Common mistake: Continuing activity despite discomfort, which can lead to chronic tendon damage.
Treatment includes rest, ice, proper footwear, and stretching. Severe cases may require physical therapy.
Arthritis in Midfoot Joints
Joint inflammation—whether from wear-and-tear or autoimmune disease—can cause persistent dorsal swelling.
Osteoarthritis vs Autoimmune Arthritis
- Osteoarthritis (OA): Caused by aging or prior injury. Swelling is usually mild, intermittent, and worsens after activity.
- Rheumatoid arthritis (RA): An autoimmune disorder causing symmetric swelling, morning stiffness, warmth, and redness in midfoot joints.
- Psoriatic arthritis: May affect one or both feet, often with skin or nail changes.
Blood tests and imaging help distinguish between types. Early diagnosis prevents irreversible joint damage.
Gout: Sudden and Severe Swelling

Gout is a form of inflammatory arthritis triggered by uric acid crystal deposits in joints. While it typically affects the big toe, it can strike any joint—including those on the top of the foot.
Signs of a Gout Attack
- Sudden, severe pain and swelling, often starting at night
- Skin over the area becomes red, hot, and shiny
- Flares may follow heavy meals, alcohol, or dehydration
- Occurs without injury
Even mild swelling during remission can indicate underlying hyperuricemia. Recurrent attacks lead to joint erosion if untreated.
Confirming the Diagnosis
Doctors may:
– Check serum uric acid levels
– Perform joint aspiration to identify urate crystals
– Use imaging to rule out infection or fracture
Treatment includes NSAIDs, colchicine, or corticosteroids during flares, plus long-term uric acid-lowering therapy.
Infections That Cause Dorsal Swelling
Infections can mimic gout or injury but require urgent treatment to prevent complications.
Cellulitis: Skin Infection Danger
Bacterial infection (commonly Staph or Strep) enters through tiny cuts, especially in older adults or diabetics.
- Symptoms: Expanding redness, warmth, swelling, fever
- Mistaken for gout: But doesn’t respond to gout medications
- Urgency: Can spread to bloodstream—requires antibiotics
Any unexplained hot, red swelling needs immediate medical evaluation.
Deep Abscess or Osteomyelitis
A pus-filled abscess may appear as a swollen, painful lump. If infection reaches bone (osteomyelitis), it becomes harder to treat.
- Risk groups: Diabetics, people with poor circulation
- Clues: Persistent swelling, deep pain, fever, history of puncture wound
- Diagnosis: MRI or bone scan often needed
These require drainage and prolonged antibiotics.
Blood Flow and Clotting Disorders
Impaired circulation can cause fluid leakage—and some vascular causes are life-threatening.
Deep Vein Thrombosis (DVT)
A blood clot in a deep leg vein causes unilateral leg and foot swelling, including the dorsal aspect.
Red Flags for DVT
- Swelling in one leg only
- Pain, warmth, redness along the calf or foot
- Worsens with standing
- Risk of pulmonary embolism—a medical emergency
Immediate testing (Doppler ultrasound) and anticoagulation are essential.
Who’s at Risk?
- Long flights or immobility
- Recent surgery
- Cancer
- Birth control or hormone therapy
- Personal history of clots
Never ignore one-sided foot swelling.
Chronic Venous Insufficiency
Weak vein valves cause blood to pool, increasing pressure and fluid leakage.
- Symptoms: Bilateral swelling that worsens during the day, improves with elevation
- Skin may darken or thicken over time
- Often linked to varicose veins or prior DVT
Compression stockings and leg elevation help manage symptoms.
Superficial Phlebitis
Inflammation of a surface vein causes tender, red, cord-like swelling.
- Less dangerous than DVT but must be evaluated
- Can occur after IV lines or spontaneously
Treated with heat, NSAIDs, and monitoring.
Systemic Diseases Behind Foot Swelling

When both feet swell without injury, systemic disease may be the culprit.
Heart Failure and Fluid Backup
Weak heart pumping leads to fluid backing up into the lungs and legs.
- Symptoms:
- Bilateral foot and ankle swelling
- Worsens with activity, improves with rest
- Shortness of breath, fatigue, nighttime cough
- Swelling often extends to calves
Treated with diuretics, medication, and lifestyle changes.
Kidney Disease and Protein Loss
Damaged kidneys retain sodium and water, causing edema.
- Signs:
- Generalized swelling, starting in feet
- Morning eye puffiness
- Foamy urine (proteinuria)
- Elevated creatinine on blood tests
Early detection via urinalysis is key.
Liver Cirrhosis and Low Albumin
The liver produces albumin, which keeps fluid in blood vessels. In cirrhosis, low albumin causes leakage.
- Swelling pattern: Legs, feet, hands, and abdomen (ascites)
- Skin may appear yellow (jaundice)
- History of alcohol use or hepatitis
Requires specialist care and nutritional support.
Lymphedema: Chronic Non-Pitting Swelling
When lymphatic drainage fails, lymphedema causes progressive, firm swelling.
Identifying Lymphedema
- Non-pitting edema: Pressing the skin leaves no indentation
- “Box-like” or dorsal mound appearance
- May follow cancer surgery, radiation, or infection
- Skin thickens over time; infection risk increases
Unlike venous swelling, it doesn’t improve much with elevation.
Management Strategies
- Compression garments
- Manual lymphatic drainage
- Skin care to prevent infection
- Early intervention slows progression
Medications That Cause Foot Swelling
Many common drugs list peripheral edema as a side effect.
Top Drug Culprits
| Medication | How It Causes Swelling |
|---|---|
| Amlodipine, nifedipine | Dilate vessels → capillary leakage |
| Pioglitazone, rosiglitazone | Promote fluid retention |
| Prednisone | Increases sodium retention |
| NSAIDs | Reduce kidney function over time |
| Estrogen therapy | Hormonal fluid retention |
Talk to your doctor before stopping any medication.
Pregnancy and Hormonal Swelling
Mild foot swelling is common in pregnancy due to increased blood volume and uterine pressure.
Normal vs Dangerous Swelling
- Normal: Bilateral, gradual, improves with rest
- Dangerous: Sudden, severe, one-sided, or with high blood pressure, headache, vision changes
These could signal preeclampsia, which endangers both mother and baby.
All new swelling in pregnancy should be monitored.
Lifestyle and Mechanical Triggers
Sometimes, the cause isn’t medical—just how you move or what you wear.
Prolonged Sitting or Standing
Long hours reduce calf pump action, slowing blood return.
- Swelling pattern: Bilateral, worse by evening
- Fix: Walk every 30–60 minutes, elevate feet
Common in travelers and office workers.
Tight or Poor-Fitting Shoes
Shoes that compress the top of the foot restrict blood flow.
- Symptoms: Localized swelling, redness, numbness
- High heels increase dorsal pressure
- Solution: Wear wide-toe-box, supportive shoes
Simple changes can prevent recurrence.
Final Note: Swelling on the top of the foot is not normal if it persists, recurs, or appears without cause. While some triggers are harmless, others—like DVT, infection, or heart failure—require urgent attention. Use symptom patterns to guide concern, but always consult a healthcare provider for unexplained swelling. Early diagnosis means better outcomes, fewer complications, and faster recovery. Your feet are telling you something—listen carefully.