Dry, cracked heels are more than just a cosmetic issue—they’re a common yet often misunderstood foot problem affecting millions. Known medically as heel fissures, this condition begins when the skin around the heel becomes excessively dry, thickened, and inflexible. As you walk or stand, the fat pad beneath the heel expands outward, placing stress on the surrounding skin. When that skin lacks moisture and elasticity, it splits—forming painful, sometimes bleeding cracks.
Left untreated, these fissures can deepen into open wounds, increasing the risk of bacterial infections, cellulitis, or even diabetic foot ulcers in high-risk individuals. The root causes are rarely simple. Instead, cracked heels stem from a complex mix of biomechanical pressure, environmental exposure, medical conditions, and lifestyle habits. Understanding these underlying factors is key to effective treatment—and long-term prevention.
In this guide, we’ll break down the 8 major causes of dry and cracked heels, from overlooked fungal infections to hidden nutrient deficiencies. You’ll learn how everyday choices—like your footwear or shower routine—can silently worsen the problem, and when to seek medical help before complications arise.
Why Heels Crack: The Science Behind Fissure Formation
Cracked heels don’t happen overnight. They develop through a predictable cycle: dryness → callus buildup → loss of elasticity → splitting under pressure.
The heel’s skin is uniquely vulnerable. Unlike other areas of the body, it has no sebaceous (oil) glands, meaning it can’t naturally lubricate itself. Over time, repeated pressure from walking or standing leads to thickened skin (calluses), especially along the outer rim of the heel. When this callused skin dries out, it becomes brittle. The moment the fat pad expands during weight-bearing activities, the rigid outer layer cracks.
Severity depends on three key factors:
– How dry and thick the skin has become
– How much pressure the heel endures daily
– Whether underlying health issues impair healing or moisture retention
Small, superficial cracks may only look unsightly. But deep fissures can expose nerve endings, bleed, and become infected—especially in people with diabetes or poor circulation.
Dry Skin and Lack of Moisture
The most common starting point for cracked heels is xerosis cutis, or abnormally dry skin. Without adequate hydration, the skin loses its ability to stretch and repair.
Feet are naturally prone to dryness because:
– No oil glands in the heel area
– Constant exposure to air, friction, and hard surfaces
– Low humidity environments, especially in winter
– Hot showers and harsh soaps that strip natural oils
Even brief daily habits—like using a high-pH soap or skipping moisturizer—can accelerate moisture loss. Over time, the skin turns ashy, rough, and flaky, setting the stage for fissures.
How to Prevent Moisture Loss
- Moisturize within 10 minutes of bathing to trap water in the skin
- Use thick creams or ointments with urea, lactic acid, or petroleum jelly
- Avoid long, hot showers—opt for lukewarm water instead
- Install a humidifier in dry indoor environments
Ignoring early dryness allows calluses to build up, making the skin even more likely to split.
Excessive Pressure on the Heels

Even well-moisturized skin can crack under too much mechanical stress. The heel absorbs up to 1.5 times your body weight with each step—more during running or prolonged standing.
When pressure forces the fat pad to expand sideways, dry or thickened skin can’t accommodate the stretch and splits open.
Who’s at Risk?
- People with obesity (BMI >25): Increased load on the heel
- Healthcare workers, teachers, retail staff: Long hours on hard floors
- Athletes: High-impact activities increase force
- Those with heel spurs or flat feet: Altered foot mechanics
Podiatrist insight: Deep fissures are common in people who stand for 8+ hours daily without supportive footwear.
How to Reduce Pressure
- Wear shoes with cushioned heels and arch support
- Use gel heel pads or custom orthotics
- Avoid barefoot walking on tile, concrete, or hardwood
- Maintain a healthy weight to reduce load
Wearing the Wrong Shoes
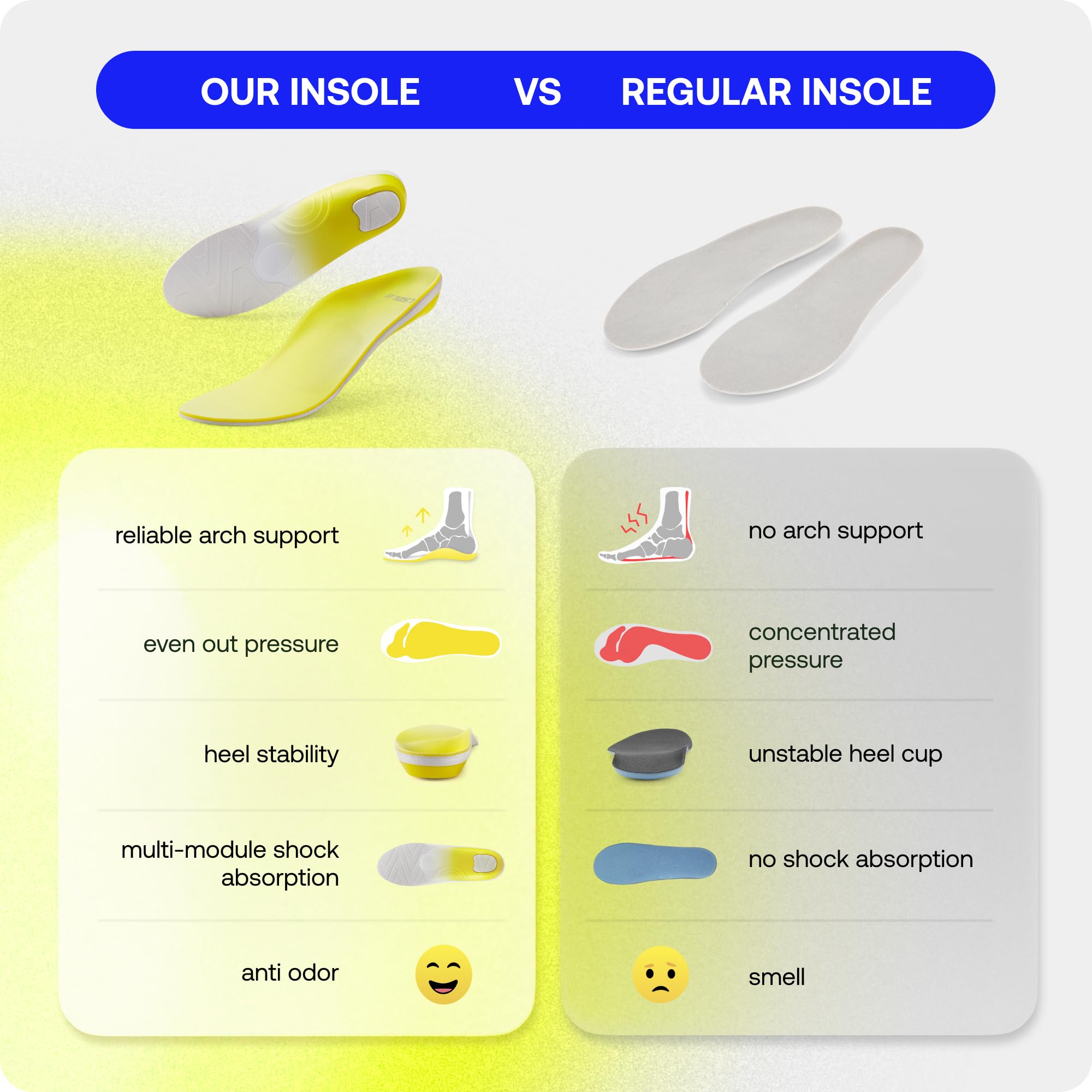
Your footwear plays a critical role in heel health. The wrong shoes can expose, over-stress, and dry out the skin.
Worst Footwear Choices
Open-Back Shoes and Sandals
- Allow the heel to bulge with every step
- Offer no support or containment
- Increase friction and exposure to dry air
Thin-Soled or Flat Shoes
- Provide minimal shock absorption
- Transfer full impact to the heel
- Promote callus formation over time
High Heels
- Shift weight forward but still stress the outer heel
- Cause uneven skin thickening
Ill-Fitting Shoes
- Too tight: cause rubbing and irritation
- Too loose: lead to sliding and friction
Pro tip: Flip-flops are a top culprit in seasonal heel cracking—especially in summer.
Best Shoes for Heel Protection
- Closed-back designs with heel counters
- Cushioned insoles and shock-absorbing soles
- Wide toe boxes to support natural gait
- Moisture-wicking linings to reduce sweat
Fungal Infections (Athlete’s Foot)

Not all cracked heels are caused by dryness. Tinea pedis, commonly known as athlete’s foot, is a fungal infection that mimics and worsens xerosis.
Fungi thrive in warm, moist environments—like sweaty shoes and gym floors—and often start between the toes before spreading to the heels.
Signs of Fungal Involvement
- Itching, burning, or scaling
- White, soggy skin between toes
- Redness or swelling
- Foul odor
- Yellow, thickened toenails (sign of nail fungus)
Red flag: If cracks don’t improve with moisturizers, consider a fungal cause.
Treatment Steps
- Apply antifungal creams (clotrimazole, terbinafine)
- Use antifungal powder daily
- Wear breathable, moisture-wicking socks
- Disinfect shoes regularly
Untreated fungal infections can lead to secondary bacterial infections if fissures bleed.
Underlying Medical Conditions
Persistent or severe heel fissures may signal a hidden health issue.
Diabetes
- Neuropathy reduces sensation, so cracks go unnoticed
- Poor circulation slows healing
- Dry skin from autonomic nerve damage
- High risk of foot ulcers and infections
Action: Diabetics should inspect their feet daily.
Hypothyroidism
- Slows skin cell turnover
- Causes coarse, dry skin
- Reduces sweating
Psoriasis (Palmoplantar Type)
- Thick, silvery scales on soles
- Deep, painful fissures
- Often symmetrical
Eczema
- Chronic inflammation
- Itchy, red, cracked skin
- Scratching worsens fissures
Sjögren’s Syndrome
- Autoimmune dryness of skin, eyes, and mouth
- Fissures resist moisturizers
Palmoplantar Keratoderma
- Genetic thickening of soles
- Requires high-dose urea creams (20–40%)
Clinical advice: If fissures are deep, bilateral, or treatment-resistant, see a doctor.
Age and Hormonal Shifts
Skin changes with age—and after menopause—make heels more vulnerable.
Aging Effects
- Thinner skin
- Slower healing
- Less natural oil and sweat
- Cumulative damage from years of pressure
People over 50 are at significantly higher risk.
Postmenopausal Women
- Estrogen decline reduces skin hydration and elasticity
- Increased callus formation
- Some studies suggest topical estrogen may help restore skin quality
Prevention: Prioritize daily foot care and regular podiatry visits.
Nutritional Deficiencies
Your diet directly affects skin strength and repair.
Key Nutrients for Healthy Skin
- Vitamin B3 (Niacin): Supports skin barrier (found in poultry, peanuts)
- Vitamin C: Essential for collagen (citrus, peppers)
- Vitamin E: Antioxidant (nuts, seeds)
- Zinc: Aids wound healing (oysters, pumpkin seeds)
- Iron: Prevents anemia-related poor healing (red meat, lentils)
When to test: If cracks persist despite good care, ask your doctor about blood tests.
Environmental and Lifestyle Triggers
Even healthy skin can crack due to habits and surroundings.
Winter Dryness
- Cold air = low humidity
- Indoor heating dries the air
- Hot showers strip oils
- Result: “Winter heel” syndrome
Fix: Use a humidifier and apply occlusive moisturizers nightly.
Summer Risks
- Bare feet in pools and gyms
- Sweaty shoes = fungal breeding ground
- Sandals increase pressure
Prevention: Wear shower shoes and rotate footwear.
Poor Foot Habits
- Not drying feet thoroughly
- Using harsh soaps
- Skipping moisturizer
- Over-scrubbing with pumice stones
Best practice: Wash, dry, and moisturize feet every night—just like your face.
Who’s Most at Risk?
| High-Risk Group | Why They’re Vulnerable |
|---|---|
| Over 50 | Age-related skin thinning |
| Diabetics | Poor healing, dry skin |
| Overweight | Increased heel pressure |
| Healthcare workers | Long hours on hard floors |
| Athletes | Sweaty shoes, public areas |
| Postmenopausal women | Hormonal skin changes |
| Psoriasis/eczema patients | Chronic skin defects |
If you’re in one of these groups, proactive care is essential.
Complications of Untreated Cracks
Ignoring heel fissures can lead to:
– Painful walking
– Bleeding
– Bacterial infections (cellulitis)
– Fungal superinfections
– Foot ulcers (especially in diabetics)
– Reduced mobility
Seek urgent care if you notice redness, warmth, pus, or fever.
When to See a Doctor
Consult a healthcare provider if:
– Cracks are deep, bleeding, or painful
– No improvement after 2–3 weeks
– You have diabetes or poor circulation
– Signs of infection
– Suspected fungal or skin disorder
Possible Diagnostics
- Skin scraping for fungus
- Blood tests for thyroid, diabetes, or nutrients
- Dermatology referral for psoriasis
- Podiatry assessment for orthotics
Final Takeaways: Prevent Cracked Heels Before They Start
Cracked heels are preventable. Key strategies:
– Moisturize daily with thick creams (urea, lactic acid)
– Wear supportive, closed-back shoes
– Avoid hot showers and harsh soaps
– Dry feet completely
– Treat fungal infections early
– Manage medical conditions
– Eat nutrient-rich foods
– Inspect feet regularly
Quick Action Plan
- Tonight: Wash, dry, and moisturize your feet.
- This week: Replace worn shoes and buy moisture-wicking socks.
- This month: Schedule a foot check if you’re diabetic or have persistent cracks.
By addressing the real causes—not just surface dryness—you can keep your heels smooth, pain-free, and healthy year-round.