Up to 14% of people are born with an extra bone in the foot known as the accessory navicular, a small ossicle that develops beside the navicular bone on the inner side of the midfoot. While it causes no issues for most, in some individuals this additional bone leads to pain, swelling, and shoe irritation—especially during physical activity. The condition becomes problematic when the bone disrupts the function of the posterior tibial tendon, a key stabilizer of the foot’s arch, leading to a painful condition called accessory navicular syndrome.
Medically referred to as os tibiale externum or os naviculare, this extra bone is congenital, meaning it forms before birth due to abnormal ossification during fetal development. Although present from infancy, symptoms typically emerge in adolescence or early adulthood, often triggered by increased physical demands, flat feet, or trauma. Despite being the most common accessory bone in the foot, many people live their entire lives unaware of its presence.
This guide explores why some individuals develop an accessory navicular, how it’s classified and diagnosed, and what treatment options exist when pain arises. From conservative therapies like orthotics and physical therapy to surgical solutions such as the Kidner procedure, you’ll gain a clear understanding of this unique anatomical variation and how to manage it effectively.
How the Accessory Navicular Forms During Development
The accessory navicular develops due to abnormal persistence of a secondary ossification center near the navicular bone during fetal growth. Normally, bones form from cartilage templates that gradually harden through ossification. In some cases, an extra center of bone formation fails to fully fuse with the main navicular, resulting in a distinct, additional bone.
Genetic Factors Behind the Extra Bone
There is strong evidence of a hereditary component in accessory navicular development. If one biological parent has the condition, their children are more likely to inherit it. While no single gene has been identified, researchers believe multiple genetic factors influence skeletal patterning and tendon attachment sites. This explains why the trait often appears in families, even if symptoms don’t manifest until later in life.
Anatomical Position and Its Impact on Foot Function
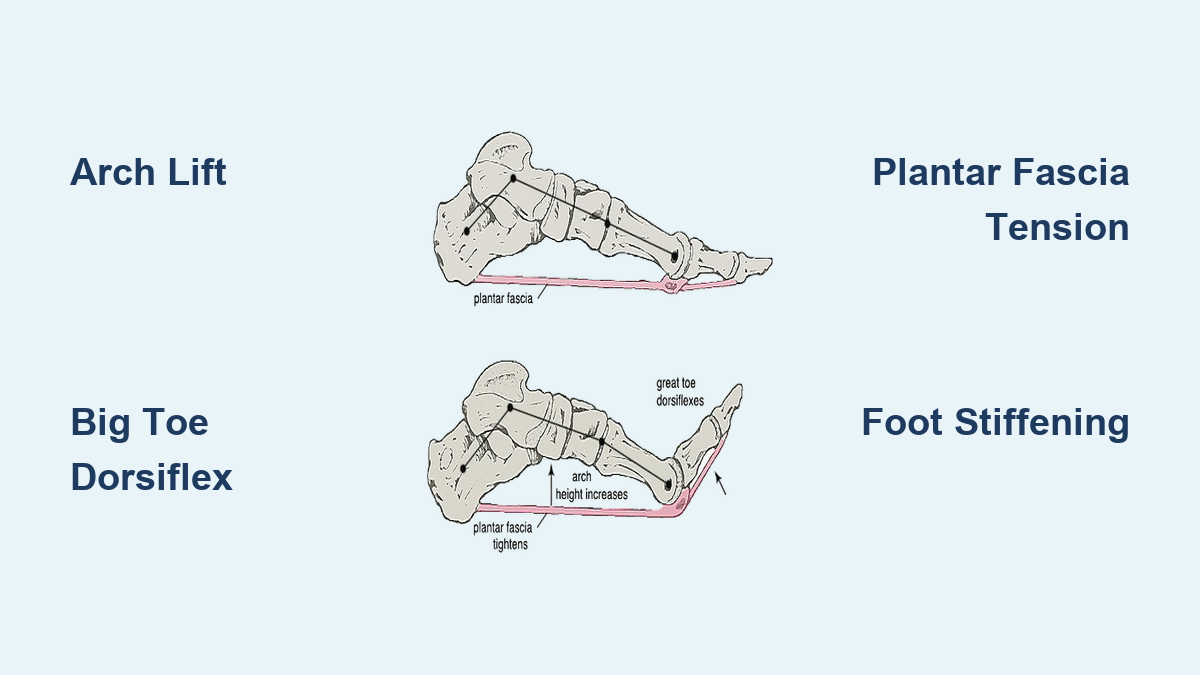
The accessory navicular sits on the medial (inner) side of the foot, just above the arch and slightly forward of the ankle. It lies directly within or adjacent to the insertion point of the posterior tibial tendon, which plays a crucial role in maintaining the foot’s arch and enabling inward foot motion.
Why the Tendon Is at Risk
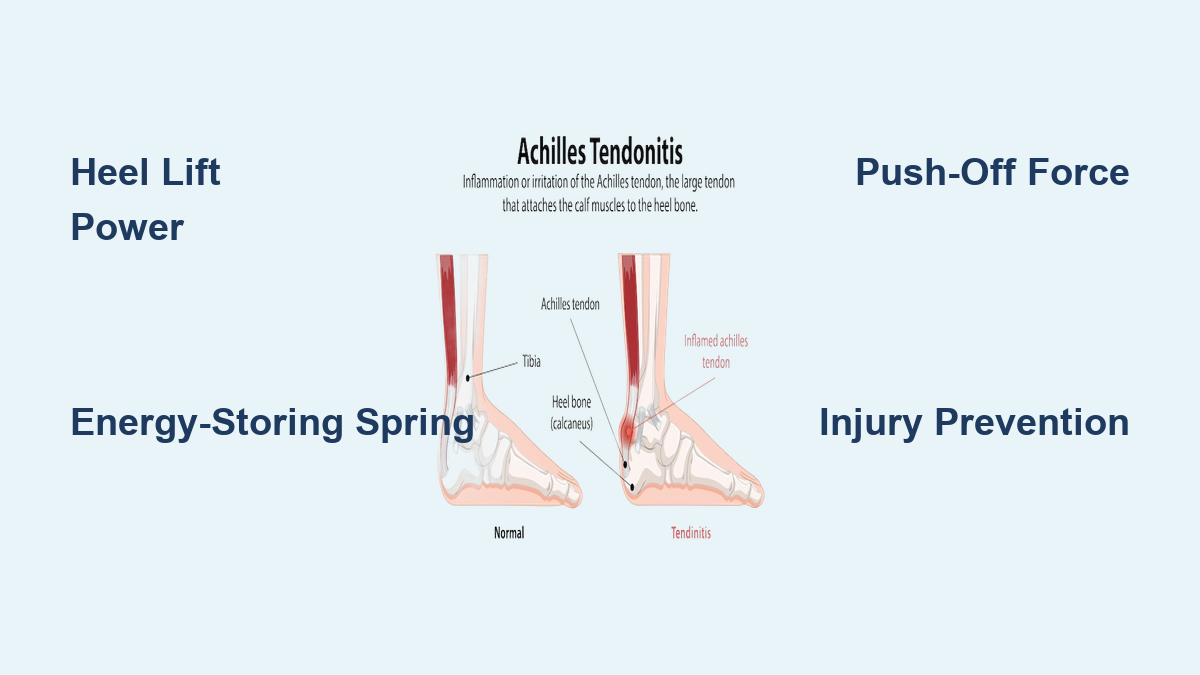
Because the posterior tibial tendon either wraps around or inserts into the accessory bone, any abnormal movement or pressure can lead to tendon strain, inflammation, or degeneration. Over time, chronic irritation may contribute to posterior tibial tendinopathy or even progressive flatfoot deformity, particularly in individuals with pre-existing biomechanical weaknesses.
Three Types of Accessory Navicular: Structure Determines Symptoms

Not all accessory naviculars are the same. Radiographic imaging classifies them into three distinct types, each with different clinical implications.
Type I: A Harmless Sesamoid Within the Tendon
- Small, round bone embedded within the posterior tibial tendon
- No connection to the navicular bone
- Found in about 30% of cases
- Rarely causes symptoms due to minimal mechanical impact
Type I is often discovered incidentally on X-rays and typically requires no treatment.
Type II: The Most Common Source of Pain
- Triangular or heart-shaped ossicle
- Connected to the navicular via a cartilaginous joint (synchondrosis)
- Allows slight movement, making it prone to irritation and inflammation
- Accounts for the majority of accessory navicular syndrome cases
This type is vulnerable to stress, especially during physical activity, and is the most likely to require intervention.
Type III: Fused Bony Prominence
- Appears as a smooth, continuous extension of the navicular bone
- No cartilaginous joint—likely a fused Type II
- Can still cause discomfort due to shoe pressure and prominence
Though structurally stable, Type III may mimic a prominent navicular and lead to chronic shoe rubbing.
Confirming the Diagnosis: Clinical and Imaging Evaluation
Diagnosing an accessory navicular begins with a thorough physical exam but requires imaging for accurate classification.
Physical Signs Doctors Look For
During evaluation, clinicians assess:
– A visible or palpable bony bump on the inner midfoot
– Localized tenderness and swelling over the navicular area
– Pain that worsens with activity
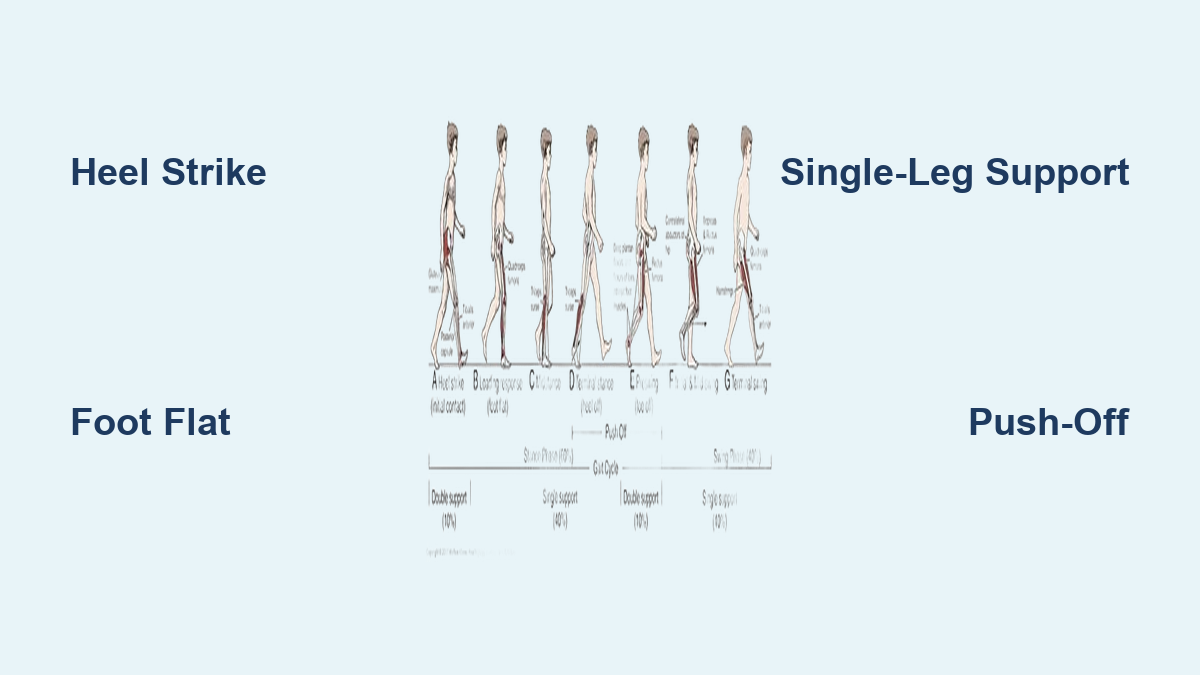
– Foot alignment, arch height, and gait abnormalities
Patients often report discomfort after walking, running, or wearing tight shoes.
Imaging to Identify the Type and Severity

X-Ray: The First Step
Weight-bearing X-rays (AP, oblique, lateral views) clearly show the size, shape, and connection of the accessory bone. They help differentiate between Type I, II, and III and rule out fractures or arthritis.
MRI: Assessing Soft Tissue Damage
When tendon involvement is suspected, MRI provides detailed views of:
– Posterior tibial tendon integrity
– Bone marrow edema
– Inflammation at the synchondrosis
– Fluid accumulation indicating active irritation
MRI is especially valuable before surgery to evaluate tendon health.
CT Scans: For Complex Surgical Planning
While less routine, CT scans offer 3D bony detail, aiding in preoperative planning when additional reconstruction is anticipated.
What Triggers Accessory Navicular Syndrome?
Most people with an accessory navicular never experience symptoms. But when pain develops, it’s usually due to irritation of the bone, tendon, or cartilage junction—a condition known as accessory navicular syndrome.
Common Causes of Pain
- Trauma or ankle sprains that injure the synchondrosis or strain the tendon
- Overuse from sports like running, basketball, or dancing
- Flat feet (pes planus), which increase stress on the posterior tibial tendon
- Tight or rigid footwear that rubs against the bony prominence
Adolescents are especially susceptible due to rapid growth, increased activity levels, and hormonal changes affecting connective tissue.
Recognizing the Symptoms
Key signs include:
– A noticeable bump on the inner foot
– Localized pain and tenderness, especially after activity
– Swelling and warmth around the area
– Difficulty wearing certain shoes
– Throbbing or aching that improves with rest
In severe cases, chronic irritation can weaken the posterior tibial tendon, potentially leading to progressive flatfoot.
Non-Surgical Treatment: The First Line of Defense
For most patients, conservative care successfully relieves symptoms without surgery.
Step-by-Step Conservative Management
- Rest and activity modification to reduce tendon strain
- Ice therapy (15–20 minutes, 3–4 times daily) to reduce inflammation
- NSAIDs like ibuprofen for pain and swelling
- Footwear changes—choose soft, flexible shoes with wide toe boxes
- Custom orthotics or arch supports to offload the tendon
- Bracing or supportive footwear to limit motion
- Physical therapy focusing on foot strength, gait correction, and tendon resilience
- Immobilization in a walking boot or cast for 4–6 weeks in severe cases
Corticosteroid Injections: Short-Term Relief Only
In persistent cases, image-guided corticosteroid injections into the synchondrosis may reduce inflammation. However, they carry risks like tendon weakening and do not address structural issues.
When Surgery Becomes Necessary
Surgery is considered only after 3–6 months of failed conservative treatment.
Indications for Surgical Intervention
- Persistent pain despite non-surgical care
- Inability to perform daily or athletic activities
- Progressive flatfoot or tendon dysfunction
- Recurrent swelling and functional limitation
The Kidner Procedure: Standard Surgical Solution
The Kidner procedure is the most common surgical fix:
– Removes the accessory navicular bone
– Detaches, trims, and reattaches the posterior tibial tendon to the navicular using sutures or bone anchors
Key Details:
- Duration: 45–60 minutes
- Anesthesia: General or regional
- Hospital stay: None (outpatient)
- Incision: Small cut over the medial bump
Note: This procedure does not correct flatfoot—additional surgery may be needed if arch collapse is present.
Recovery Timeline After Surgery

0–2 Weeks: Initial Healing Phase
- Non-weight-bearing on crutches or scooter
- Wear a backslab cast or splint
- Keep foot elevated above heart level 95% of the time
- Protect wound with waterproof cover (e.g., Limbo bag)
2 Weeks: First Follow-Up
- Wound check and dressing removal
- Transition to removable walking boot if healing well
- Begin scar massage with E45 cream
- Start gentle non-weight-bearing movement
6 Weeks: Begin Weight-Bearing
- Gradual full weight-bearing in the boot
- Start physical therapy for strength, flexibility, and balance
- Swelling may last 3–4 months
3–6 Months: Return to Activity
- Clinical review at 3 months
- Begin low-impact activities (swimming, cycling) at 3–4 months
- Full return to sports and running by 6 months
- Some report complete normalization only after 12 months
Returning to Daily Life
Driving After Surgery
- Left foot: Resume automatic driving at ~6 weeks if emergency braking is pain-free
- Right foot: Wait 6–8 weeks minimum
- Always ensure safe pedal control
Returning to Work
- Sedentary jobs: Return in 2–4 weeks
- Standing/manual jobs: Need 8–12 weeks off
- Employer accommodations can allow earlier return
Potential Risks and Complications
Non-Surgical Risks
- Worsening pain
- Chronic tendon damage
- Medial foot ulcers from shoe friction
Surgical Risks
- Infection, bleeding, blood clots
- Painful scar, stiffness, altered foot mechanics
- Tendon injury during reattachment
Despite risks, 80–90% of patients report excellent outcomes, including significant pain relief.
Long-Term Outlook: Most Patients Do Well
- Asymptomatic cases require no treatment and pose no long-term issues
- Treated cases—both non-surgical and surgical—typically achieve full recovery
- After Kidner surgery, pain resolves in 80–90% of patients
- Recurrence is rare
- Long-term disability is extremely uncommon
With proper diagnosis and management, nearly all individuals regain pain-free function and return to normal activities.