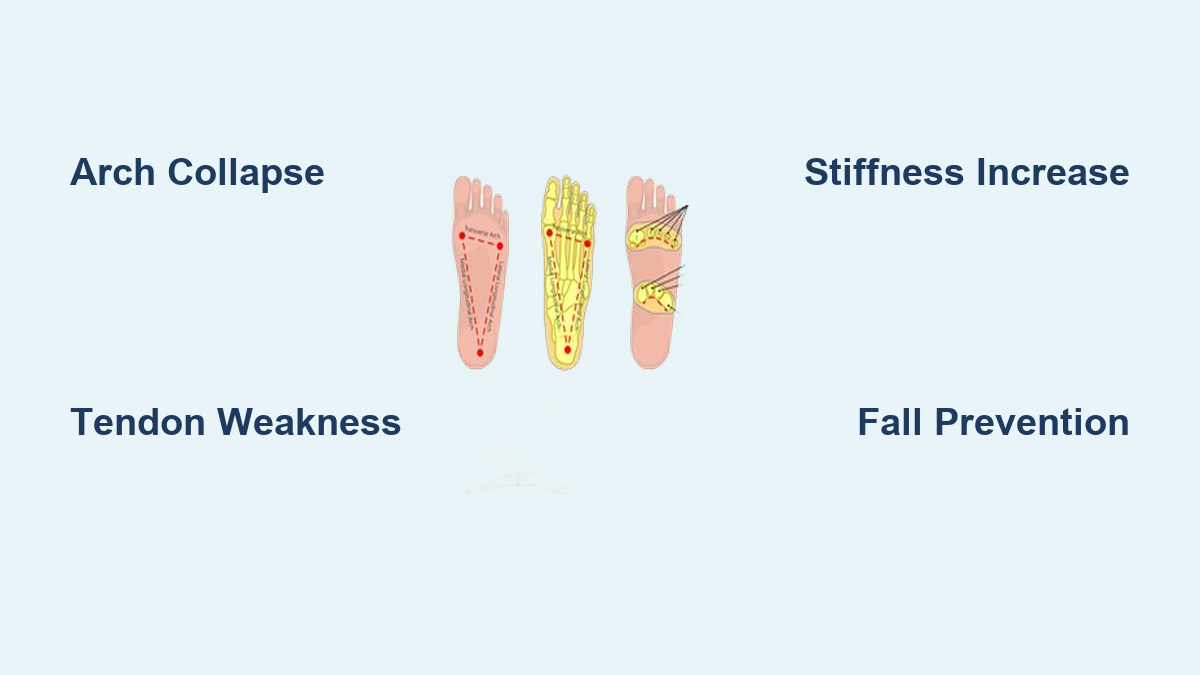
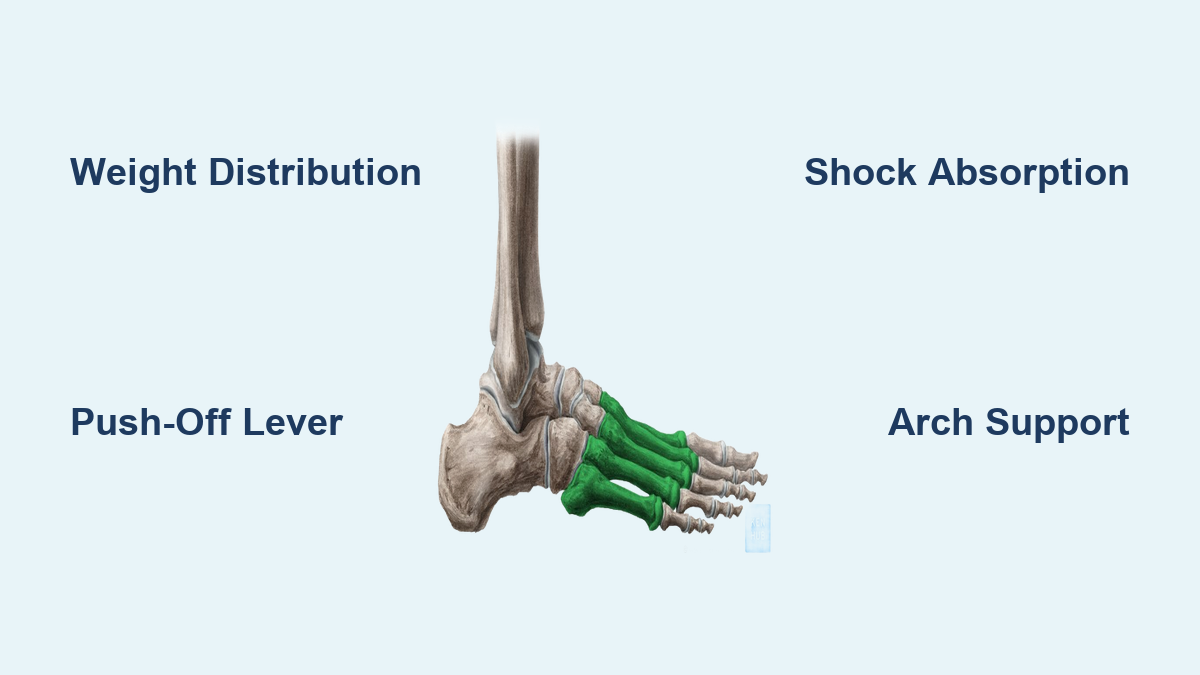
As the years pass, your feet silently bear the weight of time—carrying you through life while undergoing profound structural and functional changes. One of the most impactful yet underrecognized shifts is how age affects foot arch height and stability. The medial longitudinal arch, once a dynamic, spring-like support system, often weakens and flattens with age due to degenerating tendons, stiffening tissues, and loss of protective fat padding. This isn’t just about developing flat feet—it’s a biomechanical transformation that alters your gait, increases fall risk, and triggers pain that can travel from your heels all the way up to your lower back. Research confirms that while some decline is natural, many age-related foot changes can be slowed or corrected with early action. In this guide, you’ll discover exactly how aging reshapes your arches, why they become stiffer even as they collapse, and what you can do to maintain foot strength, balance, and mobility as you age.
Why Arches Flatten With Age

The Role of Posterior Tibial Tendon Dysfunction
One of the primary drivers of arch collapse in older adults is posterior tibial tendon dysfunction (PTTD)—a progressive weakening or tearing of the tendon that supports the inner arch. This tendon, running from the calf down to the inside of the foot, acts like a sling holding the arch in place. Over time, especially after age 40, repetitive stress, poor footwear, or underlying conditions like obesity or diabetes can cause it to stretch, fray, or rupture. As it fails, the arch gradually sags, leading to adult-acquired flatfoot (pes planus). This condition is more common in women and often begins with subtle symptoms: aching along the inner ankle, difficulty standing on one foot, or noticing that your shoes wear unevenly on the inside.
Unlike congenital flat feet, PTTD develops slowly and worsens without intervention. Early detection is key—once the tendon deteriorates significantly, the foot may require orthotics or even surgery to restore function.
Structural Breakdown Behind the Flattening
Arch collapse isn’t just about one failing tendon. It’s the result of multiple age-related changes working together:
- Ligament laxity: Connective tissues lose elasticity, causing the plantar fascia and spring ligament to stretch and sag.
- Fat pad atrophy: The natural cushion under the heel and ball of the foot thins, increasing pressure on bones and joints.
- Joint degeneration: Osteoarthritis in the midfoot or subtalar joints disrupts alignment and motion.
- Muscle weakening: Intrinsic foot muscles and calf muscles weaken, reducing dynamic support during walking.
These changes often go unnoticed until pain or instability interferes with daily activities. Even if static imaging shows minimal arch height loss, dynamic loading during walking reveals functional failure—the arch collapses under weight in ways that flat scans can’t capture.
Older Arches Are Stiffer—Not Softer

The Paradox of Increased Arch Stiffness
While your arch may be lowering, the tissues themselves are often becoming stiffer, not more flexible. A study of over 170 adults found a statistically significant increase in arch stiffness with age (p < .05), driven by collagen cross-linking, reduced elasticity, and fibrotic changes in tendons and ligaments. This stiffness impairs the foot’s ability to deform and recoil during walking—a critical function for shock absorption and propulsion.
A healthy arch should act like a spring: compressing slightly under load and then rebounding to help push you forward. When it’s too stiff, this energy-return mechanism fails, transferring excess force up the leg and increasing strain on the knees, hips, and spine.
Stiffness vs. Height: Not Always Linked
Interestingly, there’s only a weak positive correlation (r = 0.32, p < .01) between arch height and stiffness. This means someone can have a low, stiff arch—resulting in poor shock absorption and difficulty adapting to uneven terrain. This paradox explains why many older adults feel unsteady or fatigued when walking: their feet can’t adjust quickly, making every step less efficient and more tiring.
Women Face Higher Risk of Arch Collapse

Gender Differences in Arch Structure
Research shows women are significantly more likely to have low arches than men (p = .001). This disparity stems from anatomical and hormonal factors. Female feet tend to be narrower with more flexible ligaments, and hormones like relaxin—especially during pregnancy—can increase joint laxity, predisposing to arch flattening. Additionally, long-term use of high heels or narrow shoes shifts weight forward, weakens foot muscles, and alters biomechanics, accelerating arch decline.
Despite these structural differences, arch stiffness does not differ significantly between genders, suggesting that once loaded, both men and women experience similar mechanical behavior. However, women may benefit earlier from supportive footwear and orthotics to counteract their higher risk.
Obesity Speeds Up Arch Degeneration

How Weight Strains the Foot
BMI significantly impacts arch height (p < .05). With every step, the force on your feet multiplies—up to 3–4 times body weight during walking. Excess weight overloads the posterior tibial tendon and plantar fascia, accelerating their breakdown. Obesity also promotes inflammation and metabolic dysfunction, which impair tissue repair.
While higher BMI strongly correlates with flatter, wider feet, it does not significantly alter arch stiffness, meaning the intrinsic tissue properties remain similar. However, the increased mechanical load still leads to earlier pain, instability, and mobility issues.
Lifestyle Choices Shape Arch Health
Activity Level and Footwear Matter
Your daily habits play a crucial role in how your arches age:
- Prolonged standing or high-impact activities can strain tendons over time.
- Sedentary behavior leads to muscle atrophy and poor circulation.
- Barefoot walking on hard surfaces without adequate strength may increase arch strain.
- Supportive, moderate activity—like walking or swimming—helps maintain tendon resilience.
Balance is essential: too much stress without recovery harms the foot, but too little activity leads to weakness.
The Right Shoes Make a Difference
Wearing flip-flops, high heels, or flimsy sneakers offers no arch support or shock absorption, speeding up collapse. Ideal footwear for aging feet includes:
- Firm heel counter (resists squeezing)
- Stiff midsole (resists bending at the arch)
- Cushioned sole (several millimeters thick)
- Wide toe box
- Removable insole for orthotics
Avoid shoes that twist easily—they lack structural integrity.
Arch Changes Disrupt Gait and Increase Fall Risk
How Flattening Alters Walking
A collapsing arch leads to:
- Overpronation: Excessive inward rolling destabilizes the knee and hip.
- Shuffling gait: Shorter steps and delayed push-off due to weakness.
- Widened stance: A balance compensation that increases energy cost.
- Reduced propulsion: Weak muscles impair forward movement.
These changes make walking feel labored and increase fatigue.
The Link to Falls
Foot problems are a major contributor to falls in older adults. The combination of:
- Structural instability (flat, stiff arches)
- Sensory loss (from fat pad atrophy or neuropathy)
- Muscle weakness
creates a perfect storm for tripping, especially on stairs or uneven ground. Studies show that improving foot support reduces fall rates, making arch health a critical part of fall prevention.
The Kinetic Chain: From Feet to Back Pain
How Arch Collapse Affects the Whole Body
When the arch fails, the body compensates:
- Ankle valgus: Heel rolls inward, tilting the leg.
- Knee valgus (knock-knees): Increases inner knee stress.
- Hip internal rotation and pelvic tilt: Strains glutes and lower back.
- Lumbar spine misalignment: Can lead to chronic back pain.
These adaptations may start small but become permanent, leading to conditions like IT band syndrome, hip bursitis, or degenerative disc disease.
Effective Treatments to Preserve Foot Function
Custom Orthotics for Targeted Support
Custom orthotics, made from a 3D scan or mold, provide:
- Arch support
- Overpronation correction
- Pressure redistribution
- Improved shock absorption
They’re most effective when paired with supportive shoes and help conditions like plantar fasciitis and PTTD.
Supportive Shoes That Work
Look for:
- Non-collapsible heel counter
- Resistant midsole
- Thick cushioning
- Secure fastening (laces/straps)
- Enough depth for orthotics
Replace shoes every 6–12 months or 500 miles.
Foot Strengthening Exercises
Daily exercises build resilience:
- Towel curls (3 sets of 10)
- Marble pickups
- Heel raises (3 sets of 15)
- Calf stretches (2–3 minutes, twice daily)
- Single-leg balance (30 seconds, progress to eyes closed)
These improve strength, proprioception, and dynamic arch support.
Medical and Surgical Options
When conservative care fails:
- Anti-inflammatory meds or corticosteroid injections reduce pain.
- Physical therapy offers gait training and manual therapy.
- Surgery (tendon repair, osteotomy, fusion) is for severe cases.
Surgery aims to restore function and requires extensive rehab.
When to See a Podiatrist
Warning Signs to Watch For
Seek help if you experience:
- Persistent arch or heel pain
- Visible foot flattening
- Inner ankle swelling
- Trouble rising onto toes
- Balance issues or frequent tripping
- Numbness or tingling
Early diagnosis of PTTD can prevent irreversible deformity.
High-Risk Monitoring for Diabetics
If you have diabetes, neuropathy, or vascular disease, regular foot exams are crucial. Include:
- Monofilament testing (sensation)
- Doppler ultrasound (blood flow)
- Gait analysis
- Deformity screening
Routine care prevents ulcers, infections, and amputations.
Final Note: Aging reshapes your foot arches through a mix of tendon weakening, tissue stiffening, and lifestyle factors. While arches tend to flatten and stiffen, proactive care—custom orthotics, supportive shoes, strength training, and timely medical care—can preserve mobility and reduce fall risk. Understanding how age affects your feet empowers you to take action before pain or instability limits your life.