You step off a curb wrong, feel a sharp twist in your ankle, and suddenly you’re limping. Swelling starts to rise, pain flares—and you’re left wondering: Is this a sprain or a strain? While both injuries cause discomfort and limit movement, they affect different tissues and require distinct care. A sprained ankle means damaged ligaments—the tough bands connecting bones at the joint—while an ankle strain involves injury to muscles or tendons, the structures that power movement. Misidentifying one for the other can delay recovery, increase re-injury risk, or lead to long-term instability. This guide breaks down the key differences in symptoms, causes, and treatment so you can take the right action fast and get back on your feet safely.
Sprained Ankle or Strain? What’s Actually Injured
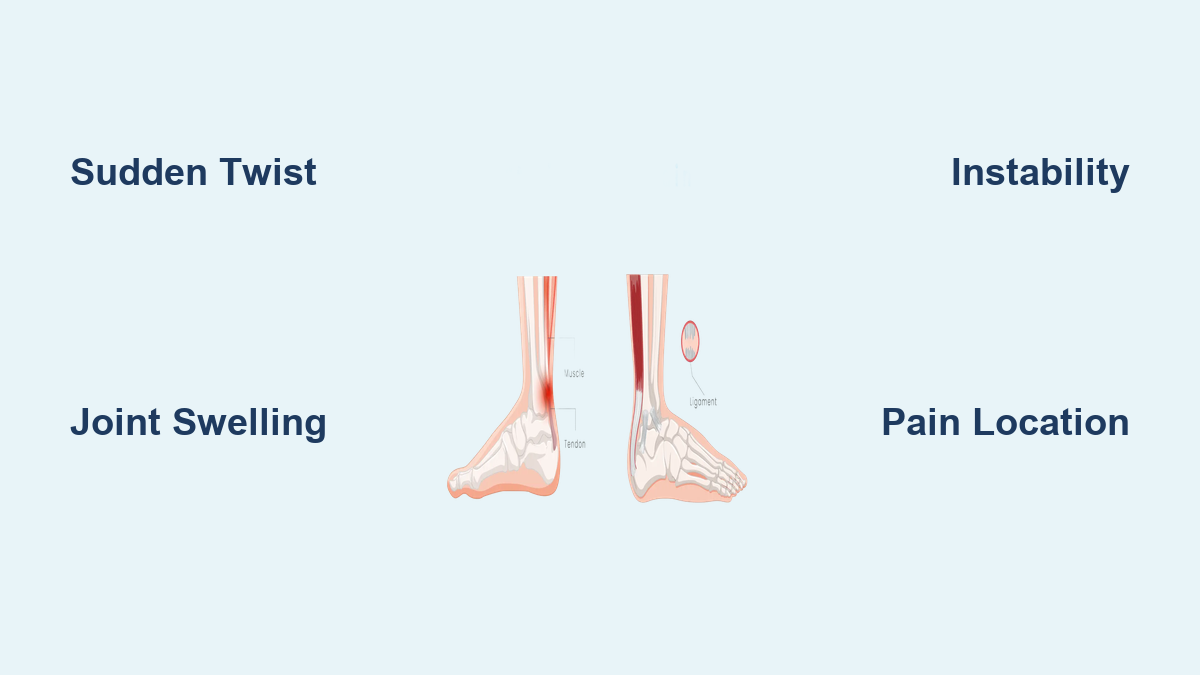
Ligaments vs Muscles: The Core Difference
Understanding the anatomy is the first step. A sprain damages ligaments, which stabilize joints by connecting bone to bone. These tissues have limited blood flow, meaning they heal slower and are more prone to chronic issues if not properly treated. The most common ankle sprain occurs when the foot rolls inward (inversion), stretching or tearing the lateral ligaments—especially the anterior talofibular ligament (ATFL).
In contrast, a strain affects muscles or tendons—the fibrous cords linking muscle to bone. These tissues are more vascular, allowing faster healing in mild cases. Ankle strains often involve the peroneal muscles on the outer calf or the tibialis posterior along the inner leg, typically from overuse, sudden sprinting, or repetitive stress rather than a single traumatic twist.
Pro Insight: If you felt a “pop” during a sudden twist, it’s likely a sprain. If pain built gradually after running or hiking, suspect a strain.
How It Happened: Clues from the Injury Mechanism
Sprain Triggers: Sudden Twisting or Rolling
Sprains usually result from acute trauma:
– Rolling the ankle inward on uneven ground
– Landing awkwardly from a jump
– Sudden change in direction during sports like basketball or soccer
These movements overstress the ligaments, especially on the outer ankle. The injury is often immediate and unmistakable—sharp pain, swelling, and instability follow within minutes.
Strain Causes: Overuse and Repetitive Stress
Strains develop differently:
– Pushing through fatigue during long runs or hikes
– Sprinting without proper warm-up
– Repeated ankle motion in jumping or cutting sports
Unlike sprains, strains often start subtly. You might notice tightness or soreness during activity that worsens over time. There’s rarely a single “moment of injury”—instead, the pain accumulates.
Red Flag: A single traumatic event points to a sprain. Gradual onset after activity suggests a strain.
Where It Hurts: Pain Location Tells the Story

Sprained Ankle: Joint-Line Tenderness
Pain from a sprain is localized around the joint, especially the bony outer ankle (lateral malleolus). Pressing directly over the ligaments—just in front of and below the ankle bone—will trigger sharp tenderness. Pain intensifies when you try to turn your foot inward or bear weight.
Ankle Strain: Muscle-Specific Discomfort
With a strain, pain runs along the muscle belly or tendon, such as the outer calf (peroneals) or back of the lower leg. It’s tender to touch along the soft tissue, not directly over the joint. The discomfort increases when you contract the muscle—like pushing your foot outward against resistance—or stretch it.
Self-Test: Gently press around your ankle. Deep, joint-level pain? Likely sprain. Pain along the calf or side of the leg? Think strain.
Swelling and Bruising: What the Patterns Reveal

Sprain: Rapid, Joint-Centered Swelling
Swelling from a sprain appears quickly—often within minutes—and centers around the ankle joint, particularly the outer side. The area may feel warm and puffy. Bruising (ecchymosis) is common and can spread down toward the sole of the foot as blood pools.
Strain: Slower, Localized Swelling
Strains cause milder, delayed swelling, usually confined to the muscle or tendon area. The skin may feel tight, but the joint itself remains relatively unaffected. Bruising is less common unless there’s a significant muscle tear.
Visual Cue: Puffy, discolored ankle within an hour? Think sprain. A sore, tight calf with swelling the next day? Likely a strain.
Stability and Function: Is Your Ankle Loose or Tight?
Sprain: Joint Instability and “Giving Way”
One hallmark of a sprain is joint instability. You might feel your ankle “give out” when walking or standing on uneven surfaces. Try balancing on one foot—if your injured ankle wobbles excessively, it could mean ligament damage has compromised stability.
Strain: Muscle Spasms and Tightness
Strains often trigger muscle cramps or spasms in the affected area. You might feel sudden, involuntary tightening in the calf or along the outer ankle. This twitching is rare in pure sprains but common with muscle overexertion or micro-tears.
Expert Note: Instability = sprain. Spasms = strain.
Can You Bear Weight? A Key Diagnostic Clue
Sprain: Weight-Bearing Often Limited
- Grade 1 (mild): Mild pain, full or near-full weight-bearing possible
- Grade 2 (moderate): Limping, may need crutches
- Grade 3 (severe): Unable to stand due to pain and instability
Severe sprains often prevent walking altogether.
Strain: Weight-Bearing Usually Possible
Even with discomfort, most people can walk on a strained ankle. Pain increases with push-off, uphill walking, or running, but the joint remains stable. Only severe (Grade 3) strains—like a complete tendon rupture—significantly impair function.
Rule of Thumb: If you can’t take four steps without severe pain, seek medical evaluation—this meets the Ottawa Ankle Rules for potential imaging.
What Doctors Check: Clinical Tests That Diagnose the Injury
For Suspected Sprains
- Anterior drawer test: The doctor pulls the foot forward to check ATFL integrity.
- Talar tilt test: Assesses lateral ligament laxity by tilting the ankle.
- Tenderness over specific ligaments confirms sprain location.
For Suspected Strains
- Resisted muscle testing: Pain when you push your foot outward against the doctor’s hand indicates peroneal strain.
- Palpation along tendons reveals tender spots.
- Weakness or a palpable gap suggests a severe tear.
Reality Check: These tests require training. At home, rely on swelling pattern, pain location, and stability cues.
When You Need Imaging: X-Ray, Ultrasound, or MRI?
X-Ray: Rule Out Fracture First
Used when you can’t bear weight or have bony tenderness. Follows Ottawa Ankle Rules: X-ray only if pain in the malleolar zone and inability to walk four steps. Can detect avulsion fractures—tiny bone fragments pulled by ligaments—confirming sprain severity.
Ultrasound or MRI: For Soft Tissue Clarity
- Ultrasound: Real-time imaging of ligaments and tendons; useful for dynamic assessment.
- MRI: Best for detailed views—used if symptoms persist beyond 1–2 weeks or surgery is considered.
Telehealth Tip: Mild cases can be assessed via video. Severe pain, instability, or deformity needs in-person care.
Healing Time: How Long Until You’re Back?
| Injury | Grade | Recovery Duration |
|---|---|---|
| Ankle Sprain | 1 | 1–2 weeks |
| 2 | 4–6 weeks | |
| 3 | 8–12+ weeks; possible surgery | |
| Ankle Strain | 1 | 3–7 days |
| 2 | 2–6 weeks | |
| 3 | 3–6 months; may need surgery |
Fact: Up to 30% of people with ankle sprains still have pain or instability one year later—often due to incomplete rehab.
Immediate Care: Use the PRICE Protocol
P – Protect
Stop activity. Use a brace or supportive shoe. Consider a walking boot for moderate to severe sprains.
R – Rest
Avoid weight-bearing if painful. Use crutches if limping. Don’t immobilize completely—early motion aids healing.
I – Ice
Apply cold pack for 15–20 minutes every 2–3 hours for first 48 hours. Wrap in cloth to prevent burns.
C – Compression
Wrap with elastic bandage (ACE wrap) from toes up. Snug but not tight—check for numbness or discoloration.
E – Elevation
Keep foot above heart level as much as possible. Reduces swelling and speeds recovery.
Myth Busting: Swelling isn’t the enemy. It’s part of healing. The goal is to manage—not eliminate—it.
When to See a Doctor
Seek urgent care if:
– Can’t bear weight
– Heard a “pop” or “crack”
– Severe pain, deformity, or numbness
– Rapid swelling or bruising
See a provider if:
– Pain lasts more than 48–72 hours
– Recurrent injuries or instability
– Returning to sports
In the UK, self-referral to NHS physio is available in many areas.
Recovery Tips: Heal Stronger and Prevent Re-Injury
For Sprains: Restore Stability
- Start alphabet tracing with toes for range of motion
- Progress to balance training: single-leg stands, wobble board
- Strengthen peroneal muscles to prevent recurrence
For Strains: Rebuild Flexibility and Strength
- Begin gentle stretching after 48 hours
- Use heat therapy after swelling subsides
- Perform eccentric exercises (e.g., slow heel drops) to rebuild tendon strength
Pro Tip: Balance training cuts re-injury risk by up to 50% in athletes.
Prevent Future Injuries
- Warm up with dynamic stretches (leg swings, high knees)
- Strengthen calf, peroneals, tibialis anterior
- Improve balance with single-leg stands or foam pads
- Wear supportive, well-cushioned shoes
- Follow the 10% rule: Increase activity by no more than 10% per week
Final Checklist: Sprained Ankle or Strain?
| Feature | Likely Sprain | Likely Strain |
|---|---|---|
| Cause | Sudden twist or roll | Overuse or repetitive motion |
| Pain Spot | Outer joint line | Calf or muscle belly |
| Swelling | Around joint, rapid | Along muscle, slower |
| Bruising | Common, spreads fast | Less common |
| Stability | Feels loose | Stable |
| Spasms | Rare | Frequent |
| Weight-Bearing | Often impaired | Usually possible |
| Pop Sound | Common in severe sprains | Only in full tendon rupture |
| Recovery (Mild) | 1–2 weeks | 3–7 days |
Bottom Line: Know the Difference, Heal Faster
Telling a sprained ankle from a strain comes down to what’s injured, how it happened, and how it feels. Ligament damage (sprain) follows a twist, causes joint swelling, instability, and bruising. Muscle or tendon injury (strain) builds from overuse, causes localized pain, spasms, and allows better weight-bearing. Use the PRICE method immediately, monitor symptoms, and seek medical help if you can’t walk, hear a pop, or see deformity. With proper care and rehab, most mild injuries heal in days to weeks—but skipping recovery steps risks long-term problems. Stay smart, listen to your body, and protect your mobility for the long run.