If you wince with every step or feel a sharp ache in your big toe when pushing off the ground, you’re likely dealing with excessive pressure on the first metatarsophalangeal joint (1st MTPJ)—the technical name for the big toe joint. This small but mighty joint supports up to 8 times your body weight with each stride, making it one of the most stressed joints in the body. Over time, conditions like hallux rigidus, bunions, gout, or turf toe can turn everyday walking into a painful ordeal. Left unchecked, the strain worsens, alters your gait, and accelerates joint damage. The good news? You don’t need to suffer. With the right footwear, orthotics, exercises, and lifestyle changes, you can significantly reduce pressure on the big toe joint, ease pain, and restore mobility. This guide delivers a science-backed, step-by-step plan to protect your feet and keep you moving pain-free.
Wear Shoes That Offload the Big Toe Joint

Choose Rocker-Soled Shoes for Smoother Walking
Rocker-soled shoes are a game-changer for reducing big toe strain. Their curved, scooped-out sole mimics a rocking motion, allowing your foot to roll forward instead of forcing the big toe to bend upward during push-off. This is especially beneficial for people with hallux rigidus or arthritis, where joint motion is already limited. Brands like Hoka One One, Altra, and Skechers GOwalk offer models with built-in rocker profiles. Look for shoes labeled “rocker bottom” or “motion control” to ensure they support natural gait mechanics and reduce stress on the 1st MTPJ.
Add Stiff Forefoot Inserts to Limit Joint Motion
A rigid forefoot plate—often made of carbon fiber—can prevent excessive bending of the big toe joint. By restricting hyperextension, it protects against turf toe and repetitive sprains. Performance running shoes like the Nike Alphafly or Adidas Adizero include these plates, but you can also add aftermarket stiff insoles to your existing shoes. This is especially helpful for athletes or anyone returning to activity after an injury. The stiff insert acts like a splint, stabilizing the joint and reducing shear forces during movement.
Opt for Wide, Deep Toe Boxes to Prevent Compression
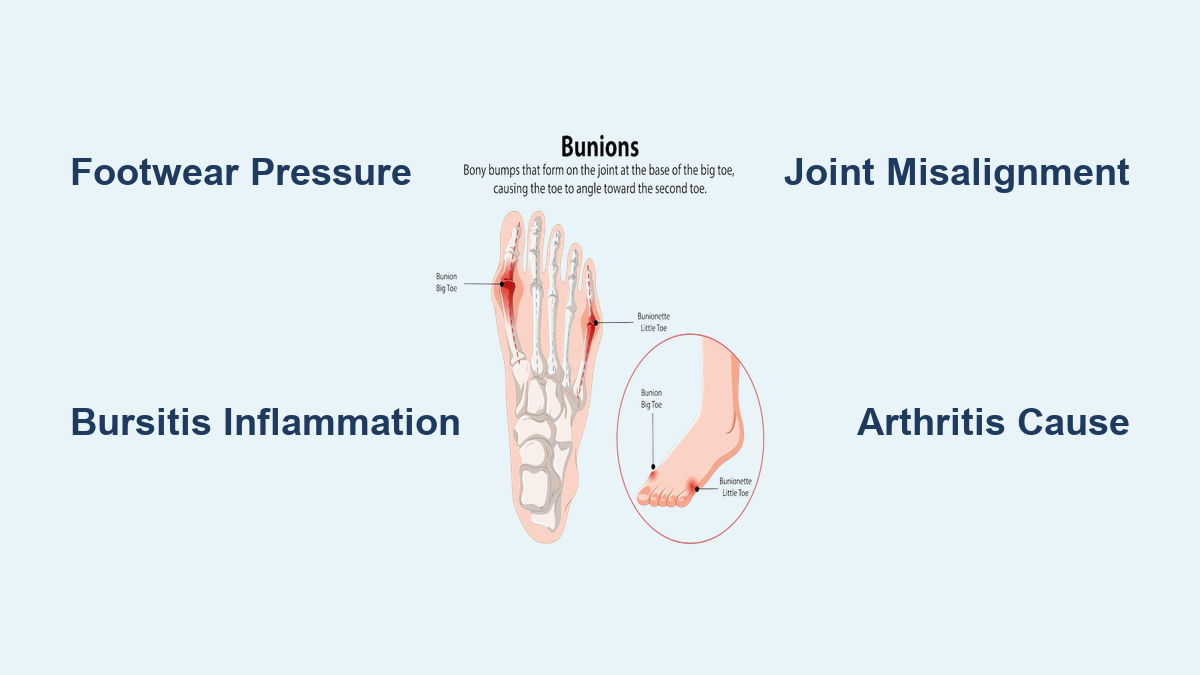
Tight shoes squeeze the big toe joint, worsening bunions, gout flares, or swelling. A wide, deep toe box allows your toes to splay naturally, reducing pressure on the medial bony bump and preventing irritation of inflamed tissues. This simple change can bring immediate relief, especially for those with hallux valgus or arthritic changes. Avoid narrow or pointed shoes—your toes should lie flat without crowding.
Ditch High Heels and Tight Footwear
Heels shift your weight forward, increasing forefoot pressure by up to 75%. Even low heels (1–2 inches) can overload the big toe joint over time. Tight shoes compound the problem by compressing nerves and soft tissues, accelerating joint degeneration. Stick to low-heeled, supportive shoes with a heel height under 1 inch. If you must wear dress shoes, use gel spacers or bunion pads to reduce friction and protect sensitive areas.
Prioritize Cushioned Midsoles for Shock Absorption
Impact from walking or standing travels directly to the 1st MTPJ. Shoes with EVA foam or polyurethane (PU) midsoles absorb this shock, reducing joint stress. Look for well-cushioned walking or running shoes with thick, responsive soles. Replace worn-out shoes every 300–500 miles or when the cushioning feels flat—worn soles offer little protection.
Use Orthotics and Support Devices for Targeted Relief

Try Custom-Made Orthotics for Precision Support
Custom orthotics, prescribed by a podiatrist, are tailored to your foot’s unique shape. They can elevate the first metatarsal, correct arch collapse, or shift pressure away from the big toe joint. For hallux rigidus or bunions, a dancer’s pad—a metatarsal pad placed just behind the 1st metatarsal head—can reduce joint compression by up to 30%. These devices improve alignment, enhance gait efficiency, and are ideal for long-term joint protection.
Use High-Quality Prefabricated Insoles
If custom orthotics aren’t an option, over-the-counter insoles can still help. Look for models with rigid arch support and forefoot stiffening. Some include built-in rocker features or metatarsal pads. Brands like Superfeet, Powerstep, or Spenco offer durable, supportive options that mimic custom devices. Replace them every 6–12 months to maintain effectiveness.
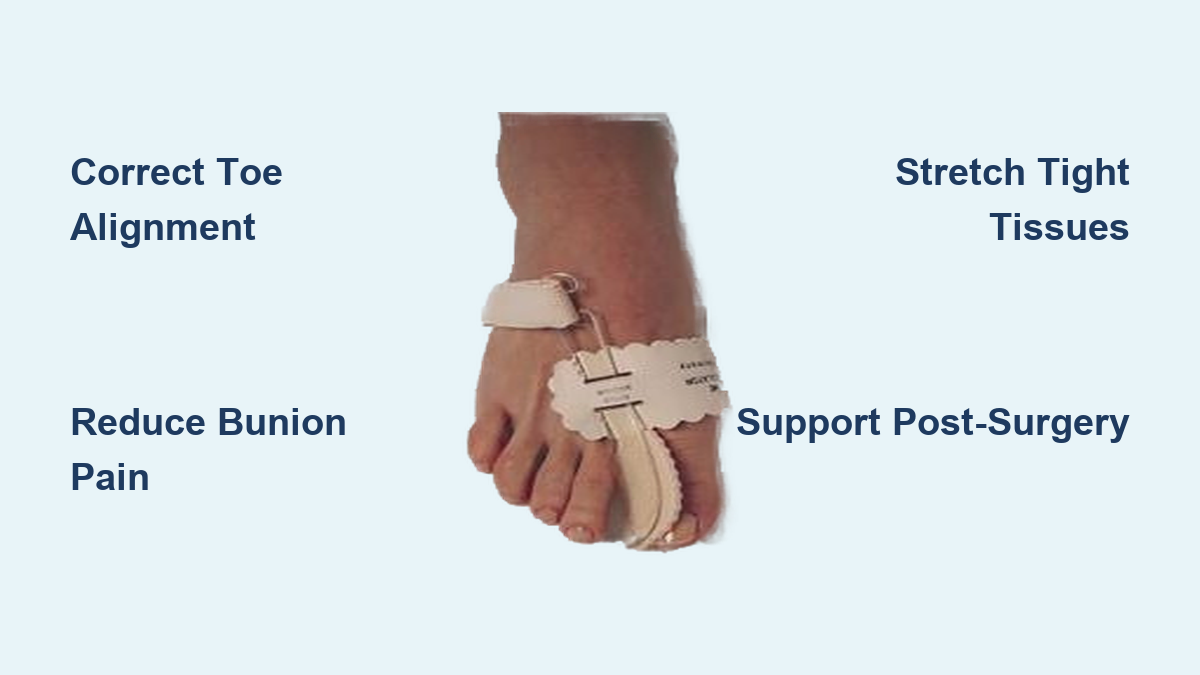
Apply Bunion Pads and Night Splints
Bunion pads made of silicone or gel cushion the medial bump, reducing shoe friction and inflammation. For mild to moderate bunions, they provide all-day comfort. Night splints gently realign the big toe while you sleep, improving joint position and reducing stiffness in hallux rigidus. While they won’t fix severe deformities, they can slow progression and ease discomfort.
Tape the Joint to Limit Painful Motion
Use Rigid Sports Tape for Immediate Stability
Taping stabilizes the 1st MTPJ during flare-ups or after injury. Use zinc oxide or rigid sports tape for best support.
Step-by-Step Taping Method:
- Apply anchor strips above and below the joint (on the foot and big toe).
- From the toe anchor, pull tape diagonally to the foot anchor, gently lifting the toe into dorsiflexion (upward bend).
- For the bottom layer, apply tape while gently pressing the toe into plantarflexion (downward bend).
- Repeat 3–4 times, creating a crisscross pattern that restricts excessive motion.
- Avoid overlapping too tightly—circulation must remain intact.
Check circulation: Press the toe tip. It should blanch and return to pink within 5 seconds. If not, loosen the tape.
Avoid Buddy Taping for the Big Toe
Unlike smaller toes, the big toe has independent nerve and muscle control. Buddy taping (toe-to-toe) can restrict natural motion and increase pressure on the 1st MTPJ. Stick to rigid strapping or bracing instead.
Perform Daily Exercises to Improve Joint Function
Stretch to Restore Big Toe Mobility
Stiffness limits push-off and increases strain. Daily stretching improves dorsiflexion.
Key Stretches:
- Toe Pull: Cross one leg, gently pull the big toe toward you. Hold 15 seconds, 3 sets.
- All-in-One Big Toe Opener: Place a tennis ball under the MTPJ. Press down while keeping the heel grounded. Hold 15–20 seconds, 3–5 reps.
- Door Frame Stretch: Place a ball under the foot, press the big toe into a door frame, and lunge forward. Hold 15–20 seconds.
Stop if pain occurs—stretching should feel like tension, not sharp pain.
Strengthen Intrinsic Foot Muscles
Weak foot muscles contribute to instability. Strengthening improves load distribution.
Effective Exercises:
- Towel Scrunch: Scrunch a towel toward you with your toes. Pinch between big and second toe. 10–15 reps.
- Marble Pickup: Pick up marbles with your toes and place them in a cup. 10–15 marbles per foot.
- Toe Raises: Lift only the big toe while keeping other toes down. 10–15 reps.
- Resistance Band Work: Loop a band around the big toe. Slowly flex and extend against resistance. 10–15 reps.
Do these daily for best results.
Improve Ankle and Joint Mobility
Restricted ankle motion forces the big toe to overwork.
Try These:
- Ankle Alphabet: Sit and trace the alphabet (A–Z) in the air with your big toe.
- Calf Stretch: Stand facing a wall, place the affected foot back, and press heel down. Hold 30 seconds.
Apply Joint Mobilization and Pain Relief Techniques
Perform First Knuckle Mobilization
This self-mobilization improves joint glide.
How to Do It:
- Pinch the base of the big toe between thumb and fingers.
- Apply gentle upward pressure with fingers, downward with thumb.
- Hold for 2–3 seconds, then release.
- Repeat up to 5 times. A “pop” may occur—this is normal.
Use daily, especially in early-stage hallux rigidus.
Mobilize the Metatarsal Bone
Misalignment increases joint pressure.
For a Dropped Metatarsal:
- Press down on the head of the first metatarsal with both thumbs. Hold 5 seconds. Repeat 3–5 times.
For an Elevated Metatarsal:
- Press down on the top of the bone with the palm. Use gentle, sustained pressure.
Perform 1–2 times daily.
Manage Pain and Inflammation Effectively
Use NSAIDs for Short-Term Relief
Ibuprofen or naproxen reduce inflammation in gout, bursitis, or sprains. Use only as needed and for no more than 7–10 days due to stomach and heart risks. Consult your doctor if you have kidney issues.
Try Acetaminophen for Pain
If NSAIDs aren’t safe, acetaminophen (Tylenol) offers pain relief. Ideal for mild to moderate discomfort.
Consider Corticosteroid Injections
When oral meds fail, a corticosteroid injection into the 1st MTPJ can provide fast relief for gout flares or arthritis. Limited to 2–3 per year to avoid cartilage damage. Administered by a podiatrist.
Explore PRP Injections
Platelet-rich plasma (PRP) uses your blood to promote healing. Emerging evidence supports its use in moderate hallux rigidus. Still under research, but promising for those avoiding surgery.
Apply Ice and Contrast Therapy
Ice After Activity or Flare-Ups
Use an ice pack or frozen water bottle for 15–20 minutes after walking or during a gout flare. Wrap in a thin towel to avoid skin damage.
Best for acute pain, not chronic stiffness.
Try Contrast Bath Therapy
Alternating hot and cold improves circulation.
How to Do It:
- Fill two basins: one with cold water (50–60°F), one with warm water (90–100°F).
- Soak foot in cold for 5 minutes, then warm for 5 minutes.
- Repeat 3–4 cycles, ending with cold.
Use for chronic swelling or recovery.
Lose Weight to Reduce Joint Load
Every pound of body weight adds up to 8 pounds of pressure on the big toe joint. Losing just 5–10% of body weight can significantly reduce strain and slow arthritis progression. Combine balanced nutrition with low-impact exercise like swimming or cycling.
Modify Activities and Rest When Needed
Avoid running, jumping, or squatting during pain flares. Switch to non-weight-bearing activities. After injury, use a CAM walker (moon boot) for 4–6 weeks to protect the joint. Athletes should modify training and use rigid-soled shoes during recovery.
Consider Surgery as a Last Resort
Cheilectomy for Early Arthritis
Removes bone spurs in Stage 1–2 hallux rigidus. Restores motion. Recovery: 6–8 weeks.
Arthrodesis for Severe Arthritis
Fuses the joint in Stage 3 hallux rigidus. Eliminates pain but sacrifices motion. Over 90% satisfaction.
Arthroplasty for Joint Replacement
Artificial joint implant for older, less active patients. Preserves some motion but may wear over time.
Bunion Surgery
Corrects hallux valgus and prevents secondary arthritis.
Surgery is only considered after 3–6 months of failed conservative care.
Final Note: Reducing pressure on the big toe joint requires a multifaceted approach: proper footwear, targeted exercises, orthotics, and lifestyle changes. Start with shoe modifications and daily stretching, then add orthotics or taping as needed. Address weight, inflammation, and activity levels for long-term success. If pain persists beyond 2–3 weeks, consult a podiatrist or foot specialist. With consistent care, most people can relieve pain, improve mobility, and protect their big toe joint for years to come.