| Introduction | |
| Forms of Flat | Flexible, Rigid, Acquired, and Congenital Feet |
| Causes of Flat Feet | Genetics, Medical Conditions, Injury and Overuse, Pregnancy, Aging |
| Symptoms of Flat Feet | Pain and Discomfort, Fatigue and Swelling, Balance and Posture Issues, Overpronation Related Symptoms, Limited Mobility |
| Exams and Tests for Flat Feet | Physical Examination, Gait Analysis, Foot Pressure Mapping |
| Treatment for Flat Feet | Non-Surgical Treatment Options, Surgical Treatment Options |
| FAQ Section | |
| Conclusion |
Introduction
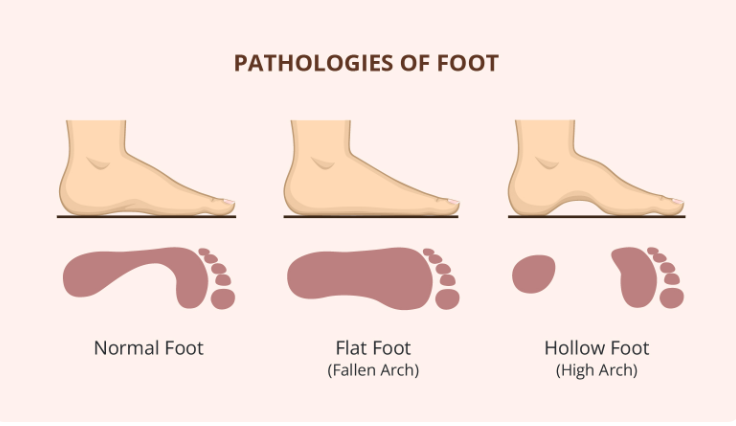
Flat feet, also known as pes planus, is a condition where the arches of the feet touch the ground completely when standing, as opposed to having a slight curve. This can significantly impact your stability and balance during daily activities. In this comprehensive guide, we will explore the different forms of flat feet, delve into underlying causes, discuss symptoms, necessary tests and exams, and present treatment options for effective management.

Forms
Flexible Flat Feet
Flexible flat feet are the most common form, particularly in children. In individuals with flexible flat feet, there is a usual arch when the foot is off the ground, but it flattens when standing or walking. Importantly, this form typically causes minimal or no pain or discomfort. The flexibility of the arch can be observed, making it a common and generally benign condition, especially in the developmental stages of childhood.
Rigid Flat Feet
Contrasting with flexible flatfoot, rigid flat feet present a persistently flat arch even when the foot is off the ground. This can cause significant pain, discomfort, and difficulties in walking or running. The rigidity of the arch makes it less adaptable, leading to more pronounced symptoms. Medical intervention may become necessary to address the discomfort and challenges associated with rigid flat feet.
Acquired Flat Feet
Adult-acquired flatfoot deformity, commonly known as acquired flatfoot, involves the gradual collapse of the arches over time. This condition typically requires attention and potential medical intervention due to the progressive nature of the arch collapse. This can result from various factors such as aging, injury, or underlying medical conditions. Timely identification and proper handling play a pivotal role in averting additional complications.
Congenital Flat Feet
Present at birth and usually hereditary, congenital flat feet are a condition that may not cause discomfort or mobility issues initially. The hereditary aspect implies a genetic predisposition leading to the structural abnormality in the arches. While symptoms may not be immediately apparent, monitoring and, if necessary, early intervention can be important to address potential discomfort or functional limitations as the individual grows.
Causes

Understanding the underlying mechanisms and potential predispositions related to flat feet is crucial.
Genetics
One of the primary causes of flat feet is genetic predisposition. This means that individuals may inherit structural abnormalities in their bones and muscles that contribute to the development of flat feet. The genetic component plays a crucial role in determining the architecture of the feet, influencing the formation of arches. Those with a family history of flat feet are more likely to experience this condition due to inherited structural traits.
Medical Conditions
Conditions like rheumatoid arthritis, diabetes, obesity, cerebral palsy, and muscular dystrophy can weaken foot arches.
– Rheumatoid Arthritis
Rheumatoid arthritis, an autoimmune disorder, can impact the joints, including those in the feet. Inflammation and damage to the joints may compromise the structural integrity of the arches, resulting in flat feet.
– Diabetes
Diabetes, particularly when not well-managed, can affect the nerves and blood vessels in the feet. This can lead to a weakening of the foot arches over time, contributing to the development of flat foott.
– Obesity
Excess body weight places additional stress on the feet, potentially causing the arches to flatten. Obesity is a contributing factor as the feet bear the burden of supporting increased body mass, leading to structural changes.
– Cerebral Palsy
Neurological conditions like cerebral palsy can affect muscle tone and coordination. This imbalance can influence the development of the arches, contributing to the manifestation of flat feet.
– Muscular Dystrophy
Muscular dystrophy, a group of genetic disorders characterized by muscle weakness, can also impact the muscles in the feet. Weakened muscles may be unable to support the arches effectively, resulting in flat feet.
Injury and Overuse
Flat feet can also result from trauma or repetitive stress on the feet, leading to structural changes over time.
– Trauma
Direct trauma, such as fractures or injuries to the tendons, can alter the anatomy of the feet. The healing process may result in changes that contribute to the development of flat feet.
– Repetitive Stress
Activities that involve repetitive stress on the feet, such as prolonged standing or intense physical activities, can lead to wear and tear. Over time, this can weaken the supportive structures of the feet, contributing to the development of flat feet.
Pregnancy
Hormonal changes and weight gain during pregnancy can have a significant impact on the ligaments in the body, including those in the feet.
The release of hormones during pregnancy, particularly relaxin, can relax ligaments, causing them to stretch. This hormonal effect, combined with the increased load on the feet due to weight gain, can lead to a flattening of the arches.
Aging
Natural wear and tear associated with the aging process can affect the elasticity and strength of the ligaments and tendons in the feet.
As we age, the supportive structures of the feet may undergo changes, resulting in reduced elasticity and strength. This gradual process can contribute to the development of flat feet over the years.
Symptoms

Flat feet can manifest a range of symptoms that have implications for overall foot health and mobility. It is of utmost importance to comprehend these indications in order to promptly identify and efficiently handle them.
Pain and Discomfort
Individuals with flat feet often experience frequent foot pain localized in the arch area. This discomfort tends to worsen with prolonged periods of standing or walking. The absence of proper arch support contributes to strain on the ligaments and muscles, resulting in pain.
Fatigue and Swelling
This can contribute to feelings of tiredness and achiness in the feet. Swelling is commonly observed around the ankles and the inner foot area. The lack of proper arch support puts additional stress on surrounding tissues, leading to discomfort and swelling, especially after extended periods of activity.
Balance and Posture Issues
Challenges in maintaining balance are common among individuals with flat feet. The altered arch structure affects the distribution of weight on the feet, leading to increased clumsiness and poor posture. These issues can have implications for overall body alignment and may contribute to discomfort in various parts of the body.
Overpronation Related Symptoms
Overpronation, the excessive inward rolling of the foot during walking or running, is often associated with flat feet. This can result in a cascade of symptoms, including:
– Heel Pain
The altered foot mechanics can lead to increased pressure on the heels, causing pain and discomfort.
– Plantar Fasciitis
Overpronation can contribute to inflammation of the plantar fascia, the tissue connecting the heel to the toes, resulting in plantar fasciitis.
– Achilles Tendonitis
The Achilles tendon may undergo increased stress and inflammation due to overpronation, leading to Achilles tendonitis.
– Shin Splints
The abnormal foot mechanics associated with flat feet can contribute to shin splints, causing pain along the shinbone.
– Knee Pain
The altered alignment of the feet can affect the knees, leading to pain and discomfort.
Limited Mobility
Individuals with flat feet may experience difficulty engaging in high-impact activities, sports, or exercises. The compromised arch support can result in discomfort and fatigue during such activities. Additionally, standard footwear may cause discomfort, emphasizing the need for proper arch support in footwear choices.
Exams and Tests
The timely identification and accurate assessment play a vital role in effectively managing the condition of fallen arches and alleviating the accompanying agony and unease.
Physical Examination
During a physical examination for flat feet, healthcare professionals assess various aspects related to the musculoskeletal system. This includes evaluating the range of motion in the feet, which helps determine the extent of flexibility and mobility. Muscle strength is examined to identify any weaknesses that may contribute to flat feet. Additionally, the flexibility of the lower limbs is assessed to understand how well the muscles and ligaments support the arches. Visible collapsing of the arch, especially when weight-bearing, is carefully observed during this examination.
Gait Analysis
Gait analysis involves the use of specialized equipment to analyze how an individual walks or runs. In the context of flat feet, this analysis is crucial for detecting abnormalities associated with foot movement. The equipment, such as pressure-sensitive mats and high-speed cameras, captures data on foot placement, timing of steps, and the distribution of weight during each phase of the gait cycle. For flat feet, overpronation (excessive inward rolling of the foot) is a common abnormality identified through gait analysis. This comprehensive assessment aids in understanding the dynamic aspects of foot function.
Imaging Tests
To obtain a detailed view of the internal structures of the feet, imaging tests such as X-rays, magnetic resonance imaging (MRI), and computed tomography (CT) scans are employed.
– X-rays
X-rays provide a two-dimensional image of the bones, allowing healthcare professionals to assess the skeletal structure, identify abnormalities, and visualize any changes in the arches.
– MRI
MRI offers a more comprehensive view by capturing detailed images of soft tissues, muscles, tendons, and ligaments. This is especially valuable in diagnosing conditions that may contribute to flat feet, such as tendon damage or inflammation.
– CT Scans
CT scans provide cross-sectional images, offering a three-dimensional perspective of the foot’s internal structure. This is particularly useful for identifying complex abnormalities and assessing the relationships between bones, muscles, and other tissues.
These imaging tests collectively aid in forming a precise diagnosis by revealing the structural aspects contributing to flat feet and guiding appropriate treatment strategies.
Foot Pressure Mapping
Foot pressure mapping involves the use of pressure-sensitive devices to measure how weight is distributed across the soles of the feet. This technology helps identify imbalances and abnormalities in pressure distribution, highlighting areas of excessive or reduced pressure. In the context of flat feet, pressure mapping can reveal patterns associated with overpronation or uneven weight distribution. This information is valuable for understanding how the feet interact with the ground and guiding interventions such as orthotic inserts or footwear modifications.
Treatment for Flat Feet
Several treatment options are available to alleviate discomfort caused by flat feet.
Non-Surgical Treatment Options
– Orthotic Inserts
Orthotic inserts are specially designed arch supports that are placed inside shoes. These inserts provide crucial support to the arches of the feet, helping to maintain proper alignment. By offering additional support, orthotic inserts can alleviate discomfort associated with flat feet, distribute pressure more evenly, and enhance overall foot function. They are customized to an individual’s foot shape and may be recommended based on the severity of flat feet.
– Physical Therapy
Physical therapy plays a pivotal role in non-surgical treatment for flat feet. Targeted exercises are prescribed to strengthen the muscles and ligaments in the feet and lower limbs. These exercises focus on improving flexibility, enhancing muscle tone, and promoting overall foot stability. Physical therapy aims to address the root causes of flat feet and enhance the ability of the feet to support the arches more effectively.
– Proper Footwear
Wearing properly fitted and supportive shoes is essential in managing flat feet. The right footwear should have a firm sole and arch support to reduce strain on the feet. Supportive shoes help to maintain the natural arch shape and provide stability during various activities. Individuals with flat feet should avoid footwear with inadequate support, such as high heels, which can exacerbate discomfort and contribute to poor foot alignment.
– Maintain a Healthy Weight
Excess body weight can worsen the impact, increasing discomfort and the risk of related issues. Sustaining a healthy weight by means of a well-rounded diet and consistent physical activity can have a positive impact on this condition.
– Medications
Nonsteroidal anti-inflammatory drugs (NSAIDs) may be recommended to reduce pain and inflammation associated with flat feet. While medications do not address the underlying structural issues, they can offer relief from symptoms. NSAIDs, such as ibuprofen, can be beneficial in managing pain and discomfort, especially during periods of increased activity.
Surgical Treatment Options

– Arthrodesis
Arthrodesis involves fusing the bones of the foot and ankle to provide stability and support. This surgical procedure is considered in cases where non-surgical interventions have not provided sufficient relief. By fusing specific joints, arthrodesis aims to create a more stable arch structure, preventing excessive motion and reducing discomfort. It is a permanent solution that alters the mechanics of the foot to improve overall function.
– Osteotomy
Osteotomy is a surgical procedure that involves cutting and reshaping bones to improve alignment and function. In the context of flat feet, osteotomy may be performed to correct deformities, redistribute pressure, and enhance the arch structure. This procedure is tailored to the individual’s specific anatomical needs and aims to optimize foot mechanics.
– Tendon Transfer
Tendon transfer is a surgical option where a healthy tendon is transferred to restore the arch and improve foot function. This procedure addresses imbalances in muscle and tendon function, helping to re-establish the natural arch shape. Tendon transfer is particularly beneficial for individuals with flat feet due to tendon dysfunction or weakness.
FAQ Section
Q1: Do my symptoms align with the characteristics of flat feet?
A1: If you experience arch pain, visible flattening, and difficulties in balance, your symptoms may indicate flat feet.
Q2: Are flat feet hereditary?
A2: Yes, congenital flat feet are usually hereditary, but acquired flat feet can result from various factors.
Q3: Do I need imaging tests for flat feet?
A3: Imaging tests like X-rays and MRI can provide a comprehensive understanding of the severity and extent of flat feet.
Q4: What treatment options are available for flat feet?
A4: Non-surgical options include orthotic inserts, physical therapy, proper footwear, and medications. Surgical options include arthrodesis, osteotomy, and tendon transfer.
Q5: Are there specific exercises to reduce pain?
A5: Targeted exercises can strengthen supporting muscles, alleviate tightness, and improve overall foot health.
Q6: Is surgery necessary in severe cases?
A6: Surgery may be considered for severe cases, with options like arthrodesis, osteotomy, or tendon transfer.
Q7: How can I manage pain on a daily basis?
A7: Nonsteroidal anti-inflammatory drugs can help reduce pain, along with proper footwear and orthotic inserts.
Q8: Are there specific shoes for better arch support?
A8: Supportive shoes with a firm sole and arch support are crucial. High heels should be avoided.
Q9: Are there lifestyle adjustments for flat feet?
A9: Lifestyle adjustments may include avoiding high-impact activities and choosing appropriate footwear.
Q10: Are there potential complications of flat feet?
A10: Complications may include limited mobility, discomfort, and long-term effects if not addressed.
WHERE TO BUY
Conclusion
Flat feet shouldn’t hinder your quality of life. Implementing appropriate solutions, such as orthotic inserts, exercises, and suitable footwear, can minimize discomfort and prevent further complications. Early detection and consultation with healthcare professionals are crucial for effective management.










Tremendous things here. I am very glad to peer your article. Thanks a lot and I’m looking ahead to contact you. Will you please drop me a mail?