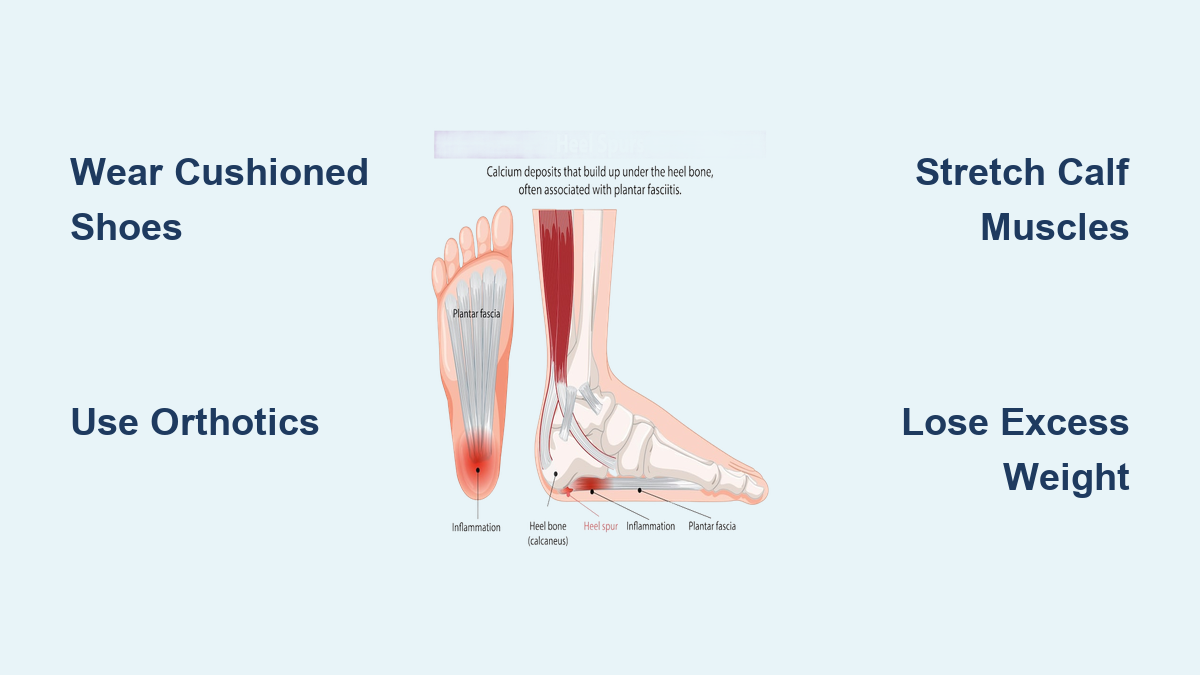
If your heel stings with every step—especially when you first get out of bed—you’re likely dealing with excessive pressure on the calcaneus, the large heel bone that anchors key foot structures. This pain often stems from conditions like plantar fasciitis, Achilles tendinitis, or heel spurs, all of which involve repetitive strain on tissues attached to the heel. The plantar fascia, a thick band running from your heel to your toes, and the Achilles tendon, connecting your calf to the back of the heel, are particularly vulnerable. When overloaded due to poor footwear, tight muscles, or excess body weight, these tissues pull forcefully on the bone, leading to inflammation, microtears, and chronic discomfort.
The good news? Over 90% of heel pain cases resolve with conservative treatment when addressed early. Reducing pressure on the heel bone isn’t about complete rest—it’s about smart load management. This guide breaks down proven, evidence-based strategies to offload the heel, relieve pain, and promote long-term healing. From supportive footwear and targeted stretches to weight management and advanced therapies, you’ll learn how to protect your feet and get back to moving pain-free.
Choose Shoes That Absorb Impact and Support Your Arch

Your footwear plays a crucial role in how much force reaches your heel with each step. Poorly designed or worn-out shoes transfer impact directly to the calcaneus, worsening inflammation and delaying recovery.
Look for These 5 Shoe Features
To reduce heel pressure, prioritize shoes with:
- Cushioned midsoles that absorb shock during heel strike
- Firm arch support to reduce strain on the plantar fascia
- Deep heel cups that cradle the heel and distribute pressure evenly
- Rigid shanks (stiff midsole inserts) that limit excessive foot flexing
- Rocker soles that promote a smooth heel-to-toe transition, lowering peak pressure
Rocker-soled shoes, in particular, can reduce plantar fascia strain by up to 50%, especially when combined with orthotics. Brands like Hoka, Brooks, and New Balance offer models designed for heel pain relief.
Avoid These High-Risk Footwear Choices
Stay away from:
– Flip-flops and sandals with no arch support
– Ballet flats and other flat-soled shoes
– Worn-out athletic shoes (replace every 300–500 miles)
– High heels, which shorten calf muscles over time
Pro tip: Keep supportive slippers by your bed. Walking barefoot on hard floors in the morning re-stretches healing tissue, reigniting pain.
Use Insoles and Orthotics to Correct Foot Mechanics

Orthotics are one of the most effective non-invasive tools for reducing heel pressure by improving foot alignment and redistributing load.
Try Over-the-Counter Insoles First
Many people find relief with OTC inserts that include:
– Arch support
– Heel cushioning (gel or memory foam)
– Metatarsal pads (to shift pressure forward)
Studies show 60–70% of users experience reduced heel pain within 6–8 weeks using OTC insoles.
Upgrade to Custom Orthotics for Persistent Pain
If OTC options fail, consult a podiatrist for custom-molded orthotics. These address specific biomechanical issues like:
– Severe overpronation
– High arches (cavus foot)
– Leg length discrepancies
Custom devices can reduce plantar fascia strain by 30–50% and improve gait efficiency with every step.
“A functional orthotic may be prescribed to control excessive pronation and support tendons attaching to the heel bone.” – Podiatric Guidelines
Lose Excess Weight to Reduce Load on the Heel

Carrying extra pounds significantly increases pressure on your heel bone. The mechanics are simple: each pound of body weight multiplies to about 4 pounds of force on your heel during walking.
How Weight Affects Heel Pressure
- Gaining 10 lbs = 40 lbs more pressure per step
- Losing 5–10% of body weight = noticeable pain reduction
- For every 5 kg (11 lbs) lost, plantar fascia load drops by ~20%
Even modest weight loss can eliminate the need for more aggressive treatments.
Choose Low-Impact Exercise While Healing
Protect your heels with:
– Swimming
– Cycling
– Elliptical training
Avoid high-impact activities during flare-ups. Focus on consistency, not intensity.
Modify Daily Activities to Prevent Overuse
You don’t need to stop moving—but you do need to reduce repetitive heel loading.
Swap High-Impact for Low-Impact Exercise
Replace running or jumping with:
– Water aerobics
– Stationary biking
– Walking on soft surfaces (grass, dirt trails)
Gentle movement boosts circulation and speeds healing. As Dr. Steven Goostree, PT, DPT, notes: “Movement encourages blood flow and keeps tissues healthy.”
Limit Prolonged Standing
If your job requires standing:
– Use anti-fatigue mats
– Take seated breaks every 30 minutes
– Rotate tasks to reduce continuous strain
Even 5 minutes off your feet hourly can prevent cumulative damage.
Stretch Tight Calf and Foot Muscles Daily
Tight calf muscles pull on the Achilles tendon, which tugs the heel bone—increasing tension on the plantar fascia.
Perform These Calf Stretches
Wall Stretch (Gastrocnemius)
- Stand facing a wall, hands on wall
- Step one foot forward (knee bent), one back (knee straight, heel down)
- Lean forward until you feel a stretch in the back calf
- Hold 30 seconds, repeat 3 times per leg
Tip: Hold stretches longer than 30 seconds for lasting tissue lengthening.
Seated Soleus Stretch
- Sit with knees bent
- Place a rolled towel under the ball of your foot
- Gently press down to feel a deep calf stretch
- Hold 30 seconds, 3 reps
This targets the soleus, the deeper calf muscle often overlooked.
Stretch the Plantar Fascia Directly
Towel Stretch
- Sit with leg extended
- Loop a towel around the ball of your foot
- Gently pull toes toward your shin
- Keep knee straight
- Hold 30 seconds, 3 reps per foot
Toe Extension Stretch
Gently pull each toe upward to stretch the fascia under the heel.
Strengthen Foot and Calf Muscles for Better Support
Strong muscles support the arch and reduce strain on the heel.
Do Towel Curls
- Place a small towel on the floor
- Use your toes to scrunch it toward you
- Perform 3 sets of 15 reps daily
This strengthens intrinsic foot muscles, improving arch stability.
Practice Toe Yoga
- Sit with feet flat
- Lift only your big toe, keep others down
- Then lift the other four toes, keep big toe grounded
- Alternate 10 times
Improves neuromuscular control and foot coordination.
Use Night Splints to Prevent Morning Pain

Morning heel pain is a hallmark of plantar fasciitis, caused by overnight shortening of the fascia.
Wear a Night Splint
A night splint holds your foot in dorsiflexion (toes pointing up) while you sleep. This:
– Prevents fascia from tightening
– Reduces first-step pain by up to 80%
– Accelerates healing in chronic cases
Options include rigid boot-style splints or soft, sock-like braces.
“Wearing night splints keeps your foot stretched. This helps alleviate morning pain.” – StrideCare Podiatrists
Start slow: Wear for 1–2 hours initially, then work up to all night.
Massage and Release Tight Tissue
Self-massage improves blood flow, reduces adhesions, and decreases fascial sensitivity.
Roll a Frozen Water Bottle
- Fill a bottle, freeze it
- Sit, place under heel or arch
- Roll slowly for 2–5 minutes
Combines ice therapy + massage + stretch—ideal after activity.
Use a Tennis or Lacrosse Ball
- Sit, place ball under foot
- Roll over tender spots (avoid direct pressure on the heel bone)
- Apply moderate pressure for 1–2 minutes per area
Focus on the arch and midfoot.
“Rolling a ball helps decrease sensitivity and increase fascia mobility.” – Austin Kiel, PT
Apply Ice and Reduce Inflammation
Cold therapy prevents inflammation buildup and numbs pain.
Ice After Activity
Apply for 15–20 minutes using:
– Ice pack
– Frozen gel pack
– Frozen water bottle
Do this once daily, especially after walking or standing.
Use NSAIDs Short-Term
Ibuprofen or naproxen can reduce pain and swelling. Use only for 7–10 days and take with food. For localized relief, try diclofenac gel.
Seek Physical Therapy for Lasting Relief
If pain lasts more than 4–6 weeks, see a physical therapist.
What to Expect in PT
- Manual therapy: Joint mobilization, soft tissue release
- Gait analysis: Identify overpronation or imbalances
- Personalized exercises: Stretching and strengthening
- Taping techniques:
- Athletic tape supports the arch
- Kinesiology tape reduces fascial strain
Taping provides immediate relief and improves function.
“A physical therapist can show you exercises to stretch the plantar fascia and strengthen lower leg muscles.” – Mayo Clinic
Consider Advanced Treatments for Chronic Pain
If conservative care fails after 6–12 months, advanced options include:
Corticosteroid Injections
- Provide short-term relief
- Ultrasound-guided for accuracy
- Limit to 1–2 injections due to rupture risk
Platelet-Rich Plasma (PRP)
- Uses your own blood to stimulate healing
- 60–80% improvement in chronic cases
- More effective than steroids long-term
Tenex Procedure
- Minimally invasive
- Removes scar tissue via ultrasound-guided device
- No stitches, faster recovery than surgery
Avoid Surgery If Possible
Surgery is a last resort—only 5% of cases require it.
Common Procedures
-
Plantar Fascia Release:
– Partially cuts fascia to relieve tension
– Success rate: 70–80%
– Risks: Nerve injury, arch collapse -
Gastrocnemius Recession:
– Lengthens tight calf muscle
– Preferred when only gastrocnemius is tight
Recovery Timeline
- 6–10 weeks for initial healing
- ~3 months before returning to running
- Physical therapy required post-op
Prevent Future Heel Pain
Once healed, protect your heels with lifelong habits.
Wear Supportive Shoes Always
Never walk barefoot on hard floors—even at home. Keep supportive slippers nearby.
Replace Shoes Regularly
Discard athletic shoes every 300–500 miles or when soles show wear.
Follow the 10% Rule
When increasing activity, boost duration or intensity by no more than 10% per week.
Do Daily Maintenance
- Stretch calves and feet every morning
- Perform towel curls 3x/week
- Use a roller or ball weekly
Reducing pressure on the heel bone starts with early action. Combine supportive footwear, targeted stretches, and activity modification to heal faster and prevent chronic pain. Most cases resolve within 10 months with consistent care—no surgery needed. Listen to your body, avoid pushing through pain, and prioritize foot health as part of your overall wellness.