You’ve started noticing a bump forming at the base of your big toe. It rubs against your shoes, becomes red and sore, and now your big toe seems to be drifting inward, pushing against the second toe. This isn’t just a minor irritation—it’s a progressive foot deformity known as hallux valgus, commonly called a bunion. Far more than a cosmetic issue, hallux valgus involves a complex misalignment of the first metatarsophalangeal (MTP) joint, where the big toe (hallux) shifts outward while the first metatarsal bone moves inward. This creates a prominent, often painful bump on the inner side of the foot.
Left untreated, hallux valgus can worsen over time, progressing through distinct stages—from a mild deviation with minimal symptoms to a severe, fixed deformity that impacts walking, shoe fit, and overall foot function. Understanding what hallux valgus is and how it advances through these stages is crucial for timely intervention. Whether through conservative care like footwear changes and orthotics or surgical correction in advanced cases, early recognition can help preserve mobility and prevent long-term complications. In this guide, we’ll explore the causes, symptoms, clinical stages, and treatment options for hallux valgus, empowering you to take informed steps toward relief.
The Anatomy and Mechanics of Hallux Valgus

Hallux valgus is not simply a “bump” but a multiplanar structural deformity involving bones, joints, ligaments, and soft tissues. The term combines hallux (Latin for “big toe”) and valgus (meaning “outward angulation”), describing the lateral deviation of the big toe. The visible bunion forms as the first metatarsal head shifts medially, creating a protrusion that often becomes inflamed due to shoe pressure.
This misalignment disrupts the windlass mechanism—a critical biomechanical process during walking where the plantar fascia tightens as the big toe extends, turning the foot into a rigid lever for push-off. When hallux valgus limits dorsiflexion of the big toe, this mechanism fails, reducing gait efficiency and transferring excessive pressure to the lesser metatarsal heads. Over time, this can lead to transfer metatarsalgia, calluses, hammer toes, and even knee or hip pain due to altered biomechanics.
Unlike temporary foot swelling or blisters, hallux valgus is progressive. Once the structural shift begins, it tends to worsen without intervention. It arises from a combination of genetic predisposition, foot type, and environmental factors like tight footwear.
Who Is at Risk for Developing Hallux Valgus
Hallux valgus affects approximately 23% of adults aged 18–65, with prevalence rising to 16% in those over 60. Women are disproportionately affected, with a 15:1 female-to-male ratio, largely due to narrow footwear and increased ligamentous laxity.
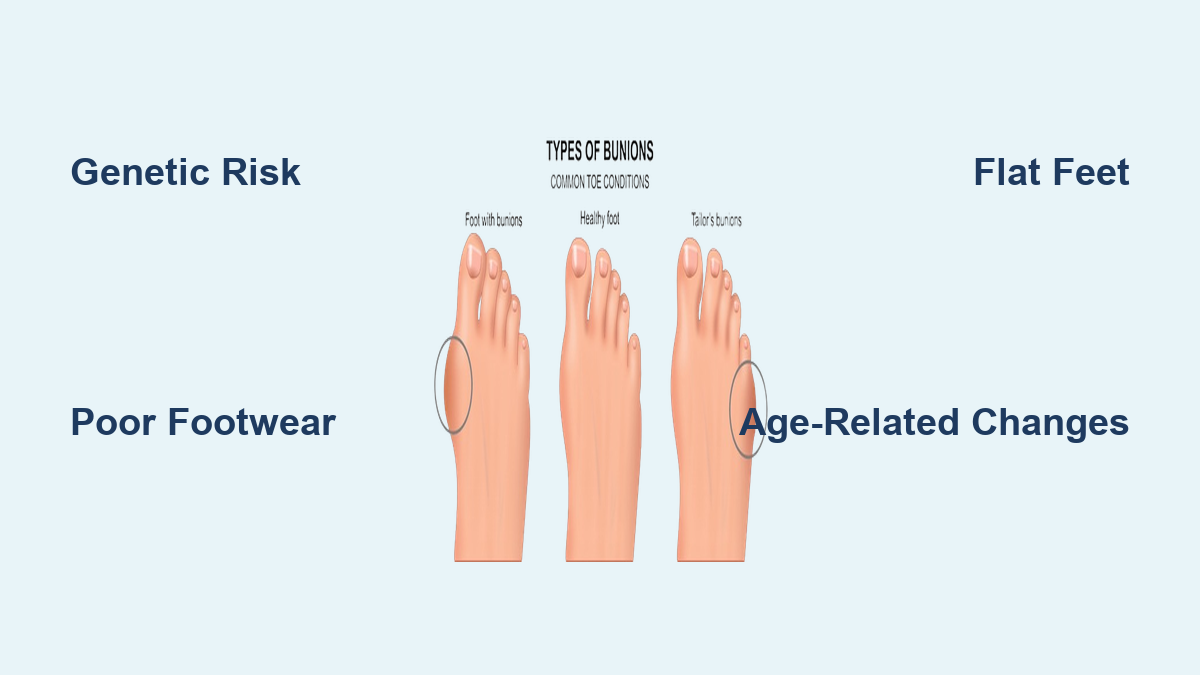
Genetic and Biological Risk Factors
- Family history: Up to 70% of patients report a relative with bunions, indicating strong hereditary influence.
- Connective tissue disorders: Conditions like Ehlers-Danlos or Marfan syndrome increase joint hypermobility.
- Neuromuscular conditions: Cerebral palsy, Charcot-Marie-Tooth disease, and multiple sclerosis alter muscle balance in the foot.
- Arthritic diseases: Rheumatoid arthritis or gout can mimic or accelerate hallux valgus.
- Structural foot types: Flat feet (pes planus), metatarsus adductus, and an elevated first metatarsal (metatarsus primus elevatus) predispose to instability.
Environmental and Lifestyle Triggers
- Footwear: High heels and narrow toe boxes compress the forefoot, forcing the big toe inward.
- Occupational demands: Jobs requiring prolonged standing increase forefoot loading.
- Obesity and inactivity: Contribute to poor foot mechanics and increased joint stress.
Individuals with both intrinsic and extrinsic risk factors—such as a woman with flat feet who regularly wears high heels—are far more likely to develop moderate to severe hallux valgus.
How Hallux Valgus Progresses: The Pathoanatomic Cascade

Hallux valgus develops gradually through a pathoanatomic cascade:
- First ray hypermobility: Ligament laxity or abnormal joint alignment allows the first metatarsal to drift medially.
- Medial metatarsal shift: This creates a bony prominence at the MTP joint.
- Lateral pull on the hallux: The adductor hallucis tendon pulls the big toe outward.
- Sesamoid displacement: The sesamoid bones, normally centered under the metatarsal head, shift laterally.
- Capsular contracture: The medial capsule stretches while the lateral capsule tightens, locking the toe in a deviated position.
- Joint incongruity and arthritis: Cartilage wears down, potentially leading to hallux rigidus.
As the deformity progresses, the foot loses its ability to function efficiently during gait, often leading to compensatory walking patterns and secondary foot problems.
Recognizing the Symptoms of Hallux Valgus
Symptoms vary by stage but typically begin with mechanical irritation and evolve into functional limitations.
Early Warning Signs
- Mild pain when wearing tight shoes
- Occasional redness or swelling at the MTP joint
- Slight visible shift of the big toe
- Feeling of forefoot tightness
Advanced Symptoms
- Persistent bunion pain, even in wide shoes
- Difficulty finding shoes that fit
- Calluses between the first and second toes
- Stiffness or reduced motion in the big toe
- Secondary deformities like hammer toes or overlapping second toe
- Skin breakdown over the bunion in severe cases
Pain often worsens during activities requiring push-off, such as climbing stairs. Inflammatory flare-ups, like bursitis, can mimic gout or infection.
Clinical and Radiographic Diagnosis

Diagnosis begins with a thorough history and physical exam. A clinician will assess:
– Degree of toe deviation
– Joint mobility (flexible vs. fixed)
– First ray stability
– Presence of arthritis
– Hindfoot and midfoot alignment
Key Physical Findings
- Medial bony prominence at the first MTP joint
- Lateral deviation and pronation of the hallux
- Tenderness over the bunion or sesamoids
- Callus under lesser metatarsal heads
- Associated deformities like flatfoot or hammer toes
Imaging for Accurate Staging
Weight-bearing X-rays are essential. Non-weight-bearing films can underestimate the true deformity.
Critical Radiographic Measurements
| Measurement | Normal | Hallux Valgus Indicator |
|---|---|---|
| HVA (Hallux Valgus Angle) | <15° | >15° indicates deformity |
| IMA (Intermetatarsal Angle) | <9° | >9° shows metatarsal deviation |
| DMAA (Distal Metatarsal Articular Angle) | <15° | >15° suggests joint incongruity |
| HVI (Hallux Valgus Interphalangeus) | <10° | >10° indicates distal phalanx involvement |
These angles guide treatment decisions and surgical planning.
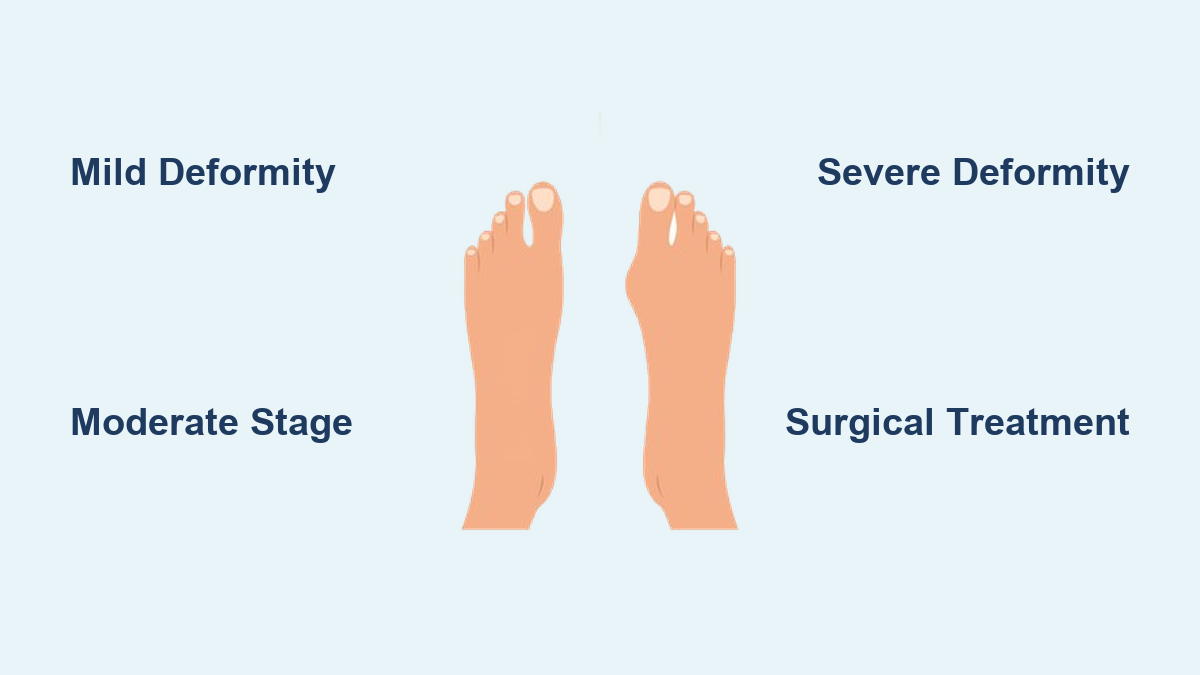
Three Stages of Hallux Valgus Progression
Hallux valgus is commonly classified into three stages based on clinical and radiographic findings.
Stage I: Mild Deformity
Clinical Features
– Slight inward shift of the hallux
– No visible bunion or minimal bump
– Often asymptomatic or mild discomfort with narrow shoes
Radiographic Findings
– HVA: 15–20°
– IMA: 9–13°
– Joint congruent, sesamoids normal
Management
– Wide-toe-box footwear
– Custom orthotics for flat feet
– Toe spacers and stretching exercises
Early intervention can slow or halt progression.
Stage II: Moderate Deformity
Clinical Features
– Clear lateral deviation of the big toe
– Visible, painful bunion
– Callus under second metatarsal
– Possible overlapping of second toe
Radiographic Findings
– HVA: 20–30°
– IMA: 13–16°
– Mild sesamoid subluxation
Management
– Continue conservative care
– Consider surgery if pain persists: Chevron osteotomy, McBride procedure
Surgical outcomes are excellent at this stage.
Stage III: Severe Deformity
Clinical Features
– Hallux overlaps or underlaps second toe
– Large, painful bunion
– Difficulty walking
– Secondary hammer toes
Radiographic Findings
– HVA: >30–50°
– IMA: >16–20°
– Significant sesamoid displacement, possible arthritis
Management
– Surgery typically required: Scarf osteotomy, Lapidus procedure, Keller resection
Recovery is longer, but patient satisfaction remains high (81–90%).
Four-Stage Classification (Alternative Model)
Some clinicians use a four-stage system:
| Stage | Description |
|---|---|
| 1 | Hallux begins to deviate; no bunion |
| 2 | Bunion forms; deviation increases |
| 3 | Hallux overlaps second toe; fixed |
| 4 | Arthritis develops; multiple deformities |
This model emphasizes arthritis, aiding surgical decision-making.
Differential Diagnosis: Conditions That Mimic Hallux Valgus
Several disorders resemble hallux valgus:
– Hallux rigidus: Stiff, arthritic big toe
– Gout: Acute, red, hot joint
– Rheumatoid arthritis: Symmetric swelling
– Turf toe: Trauma-induced sprain
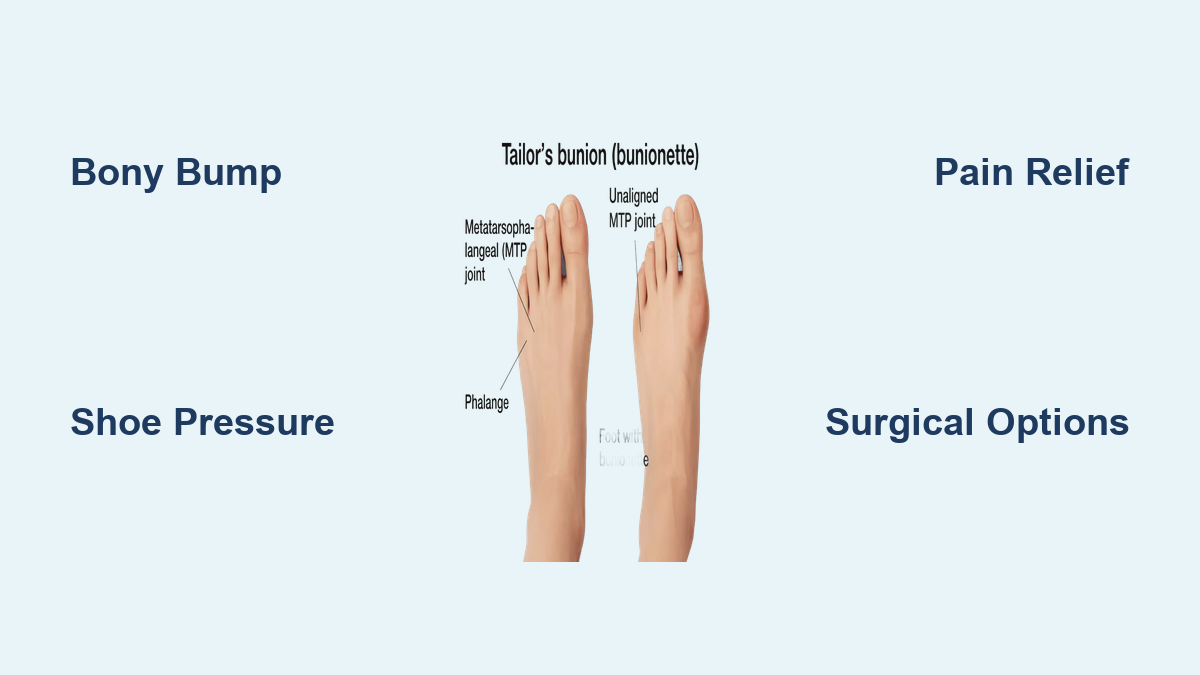
– Bunionette: Fifth MTP deformity
Accurate diagnosis ensures proper treatment.
Conservative Treatment Options by Stage
Non-surgical care focuses on symptom relief and slowing progression.
Stage I and II: Effective Conservative Strategies
- Footwear: Wide toe box, low heel (<2 inches)
- Devices: Silicone sleeves, custom orthotics
- Exercises: Towel scrunches, calf stretches
- Medications: NSAIDs, topical analgesics
Avoid ineffective products like over-the-counter splints.
When Conservative Care Fails
If pain persists for 3–6 months or deformity worsens, surgical evaluation is recommended.
Surgical Treatment Based on Severity
Over 100 procedures exist, tailored to severity and patient factors.
Mild (HVA <30°, IMA <13°)
- Chevron osteotomy
- Modified McBride
- Akin osteotomy
Moderate (HVA 30–40°, IMA 13–20°)
- Scarf osteotomy
- Ludloff osteotomy
Severe (HVA >40°, IMA >20°)
- Lapidus procedure (fusion)
- Double osteotomy
- Keller resection (elderly, low-demand patients)
Postoperative Recovery and Complications
Recovery Timeline
- 0–6 weeks: Surgical shoe
- 6 weeks: Begin motion exercises
- 8–12 weeks: Return to regular shoes
- 6–12 months: Full recovery
Common Complications
- Recurrence (10–47%)
- Transfer metatarsalgia (~5%)
- Hallux varus (overcorrection)
- Nonunion, neuropathy
Smoking and diabetes increase risks.
Prognosis and Long-Term Outcomes
- Success rate: >95% with experienced surgeons
- Patient satisfaction: 81–90%
- Functional improvement: AOFAS scores rise by 30+ points
Unmet expectations, not surgical failure, are the main cause of dissatisfaction.
Prevention and When to Seek Help
Prevention Tips
- Wear wide, low-heeled shoes
- Use orthotics if you have flat feet
- Strengthen intrinsic foot muscles
- Seek care at first sign of deviation
When to See a Specialist
Consult a foot and ankle specialist if:
– Pain limits daily activities
– You can’t wear normal shoes
– The toe overlaps
– Conservative measures fail
Early evaluation improves outcomes.
Final Note: Hallux valgus is a progressive, multifactorial deformity that advances through identifiable stages. Recognizing the signs early allows for conservative management and potential delay of surgery. As the condition worsens, surgical correction becomes necessary to restore function and relieve pain. With proper diagnosis, staging, and treatment selection, most patients achieve excellent outcomes and return to active, pain-free lives.