If you’ve noticed a tender, swollen bump at the back or bottom of your heel, you’re not alone. Localized swelling on the heel bone—specifically involving the calcaneus—can stem from a range of issues, from overuse injuries to systemic diseases. This swelling often develops gradually or appears suddenly after trauma, and it typically worsens with activity or shoe pressure. Whether you’re an athlete, on your feet all day, or dealing with an underlying health condition, understanding the root cause is essential for effective treatment. Left unaddressed, heel swelling can lead to chronic pain, altered gait, and long-term tissue damage.
This guide breaks down the most common and serious causes of heel bone swelling, including bursitis, structural deformities, trauma, tendon problems, and inflammatory diseases. You’ll learn how each condition develops, what symptoms to watch for, and what factors increase your risk. We’ll also cover key diagnostic tools and why accurate identification matters—because treating a gout flare like a simple bruise can delay healing and worsen outcomes. By the end, you’ll be equipped to recognize warning signs and take informed steps toward recovery.
Heel Bursitis: Inflammation Behind the Heel
Swelling at the back of the heel is frequently due to bursitis, an inflammation of small fluid-filled sacs that cushion tendons and bones. Two types affect the heel: retrocalcaneal and subcutaneous calcaneal bursitis. Both cause localized puffiness, pain, and discomfort in shoes, but they occur in different locations and have distinct triggers.
Retrocalcaneal Bursitis Causes
This form involves the bursa between the Achilles tendon and heel bone. Repetitive motion—like running uphill or jumping—creates friction, irritating the bursa and triggering fluid buildup. It’s common in athletes and active individuals who push through pain without adequate rest.
- Pain is deep and located just above the heel bone, worsening when the foot bends upward.
- Swelling may feel firm and is often invisible at first but becomes noticeable over time.
- Walking barefoot or in flat shoes can aggravate symptoms due to increased dorsiflexion.
- Often coexists with Achilles tendinopathy, making diagnosis tricky without imaging.
Without intervention, chronic irritation can thicken the bursa and lead to persistent swelling that resists conservative care. Early management includes rest, ice, heel lifts, and avoiding activities that provoke pain.
Subcutaneous Calcaneal Bursitis Signs
Also called superficial bursitis, this affects the bursa between the skin and Achilles tendon. It’s usually caused by shoe pressure, especially from stiff heels or tight footwear like dress shoes, ice skates, or high heels.
- Swelling appears as a soft, red, warm lump at the top back of the heel.
- Direct pressure from shoes intensifies pain—many patients report relief when switching to open-back footwear.
- Frequently linked to Haglund’s deformity, where a bony bump aggravates the area.
- Unlike deeper bursitis, this type is often visible and easily palpable.
✅ Pro Tip: If your heel swells only when wearing certain shoes and improves when barefoot, subcutaneous bursitis is likely.
Haglund’s Deformity: The “Pump Bump”

A hard, protruding lump at the back of the heel that hurts in shoes may be Haglund’s deformity, often nicknamed the “pump bump” because it’s commonly triggered by wearing pumps or stiff-heeled shoes. This bony enlargement on the upper rear edge of the calcaneus mechanically irritates soft tissues, leading to secondary inflammation and swelling.
Why the Bony Bump Forms
The deformity develops due to a combination of genetics and biomechanics. Some people inherit a heel bone shape that angles outward, creating natural pressure points. Over time, repetitive rubbing against shoe counters causes chronic irritation.
- High arches (cavus foot) shift the heel backward, increasing contact with shoes.
- Tight calf muscles pull the Achilles tendon taut, pressing it harder against the bone.
- Overpronation or flat feet alter gait mechanics, indirectly contributing to strain.
Even minor daily friction can turn into significant inflammation if the bony prominence isn’t addressed. The result? A cycle of swelling, pain, and skin breakdown.
Symptoms and Diagnosis
- A hard, immovable bump at the posterior-superior heel.
- Overlying soft tissue swelling, redness, and warmth—signs of reactive bursitis.
- Pain when wearing closed shoes, especially during walking or running.
- X-ray confirms the abnormal bone contour; MRI or ultrasound assesses soft tissue damage.
⚠️ Warning: Ignoring this condition can lead to chronic bursitis, tendon degeneration, or even Achilles rupture in severe cases.
Heel Bone Bruise: Trauma-Induced Swelling

A sudden jolt or repeated pounding can cause a calcaneal contusion, commonly known as a bruised heel bone. This injury leads to localized swelling, pain, and sometimes discoloration, especially after landing hard from a jump or falling on your feet.
Acute vs. Repetitive Trauma
- Acute trauma (e.g., fall from height) causes immediate pain and swelling, often with bruising.
- Repetitive microtrauma (e.g., long-distance running on concrete) builds up over time, leading to chronic heel discomfort.
Unlike a fracture, a bruised heel allows partial weight-bearing, though walking is painful. X-rays show no break, but MRI reveals bone marrow edema—a key diagnostic sign.
Risk Factors for Heel Bruising
- High-impact sports: basketball, track, gymnastics.
- Obesity: increases force on the heel with each step.
- Poorly cushioned shoes: fail to absorb shock during activity.
- Hard surfaces: concrete, asphalt, or hardwood floors.
✅ Quick Fix: Rest, ice, and cushioned insoles often resolve mild cases within 1–3 weeks.
Achilles Tendinopathy: Swelling at the Tendon Insertion
Pain and swelling at the back of the heel are hallmark signs of insertional Achilles tendinopathy, a degenerative condition affecting the tendon where it attaches to the heel bone. While often confused with bursitis, this issue originates in the tendon itself.
How Tendon Damage Causes Swelling
Chronic overuse leads to microtears and failed healing, resulting in tendon thickening and inflammation. The area becomes swollen, tender, and stiff—especially in the morning or after sitting.
- Swelling is along the tendon, not just behind it.
- Palpable lump or nodule may form at the insertion site.
- Pain improves slightly with movement (“warm-up” phenomenon).
- Often coexists with retrocalcaneal bursitis, creating a dual-source pain problem.
Common Triggers
- Rapid increase in training intensity or mileage.
- Poor calf flexibility: tight gastrocnemius or soleus muscles.
- Biomechanical issues: flat feet, overpronation, leg length differences.
- Age: degeneration is more common in adults over 40.
✅ Pro Tip: Heel lifts in shoes can reduce strain during early recovery.
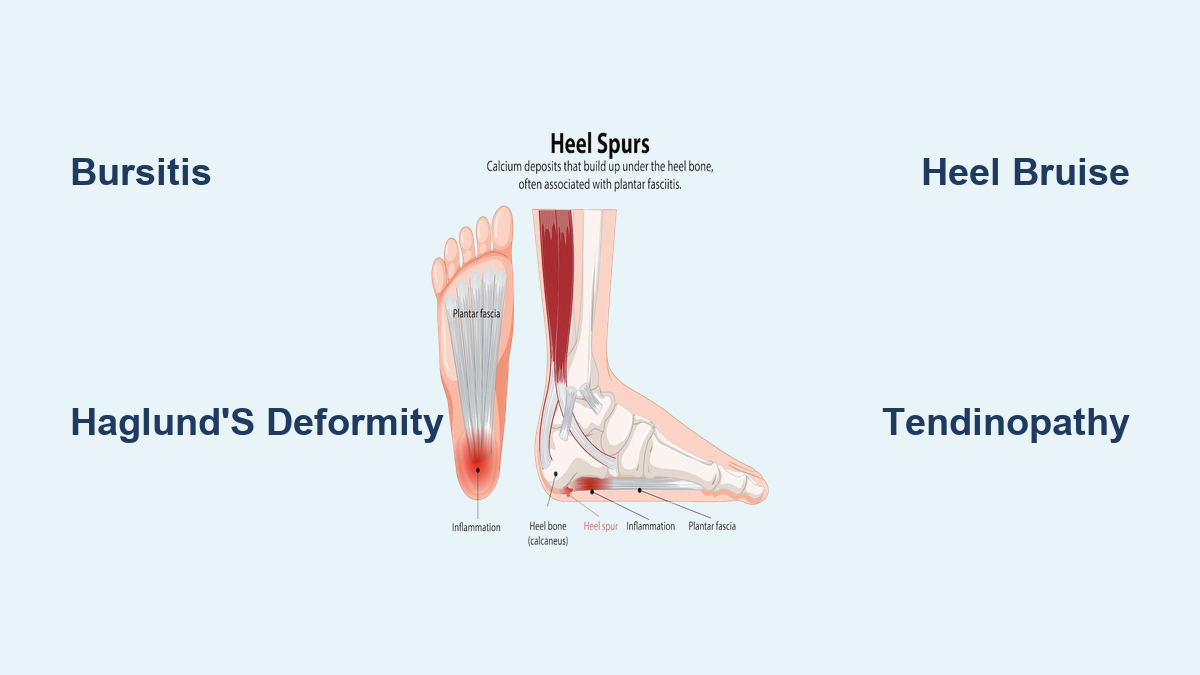
Heel Spurs and Their Role in Swelling
Heel spurs are bony projections that form on the underside (plantar) or back (posterior) of the heel bone. While the spur itself doesn’t swell, it acts like a splinter—irritating surrounding tissues and causing inflammation.
Plantar vs. Posterior Spurs
| Type | Location | Associated Condition | Swelling Pattern |
|---|---|---|---|
| Plantar Heel Spur | Bottom of heel | Plantar fasciitis | Tender, swollen spot on the sole |
| Posterior Heel Spur | Back of heel | Insertional Achilles tendinopathy | Swelling at tendon insertion |
Spurs develop due to chronic traction from the plantar fascia or Achilles tendon. They’re visible on X-ray, but treatment focuses on the inflamed soft tissue, not the bone spur.
❗ Myth Busting: Removing a heel spur surgically rarely resolves pain—the real issue is usually soft tissue inflammation.
Systemic Conditions That Cause Heel Swelling

Not all heel swelling stems from overuse or injury. Inflammatory and metabolic diseases can target the heel, mimicking mechanical injuries but requiring entirely different treatment.
Rheumatoid Arthritis (RA) Effects
RA is an autoimmune disease that attacks joint linings. It can affect the subtalar or ankle joints, leading to bilateral heel pain, morning stiffness lasting over 30 minutes, and soft tissue swelling.
- Often accompanied by fatigue, fever, and joint swelling elsewhere.
- Ultrasound or MRI shows synovitis or tenosynovitis around the Achilles or plantar regions.
Gout in the Heel
Gout occurs when uric acid crystals deposit in tissues. Though more common in the big toe, it can flare in the Achilles tendon or retrocalcaneal bursa.
- Sudden, severe pain, redness, and swelling—often waking patients at night.
- Fever and extreme tenderness; may mimic infection.
- Diagnosed via blood tests (elevated uric acid) or joint fluid analysis.
Septic Bursitis: Infection Risk
A rare but dangerous cause, infectious bursitis happens when bacteria enter the bursa through a cut, blister, or injection.
- Signs: intense redness, heat, pus, fever, and systemic illness.
- Requires urgent medical care: bursal fluid aspiration, antibiotics, possibly surgery.
- High-risk groups: diabetics, immunocompromised individuals, IV drug users.
⚠️ Red Flag: If heel swelling comes with fever or spreading redness, seek care immediately—this could be septic bursitis.
Key Risk Factors for Heel Swelling
Certain habits and health conditions make you more prone to heel problems. Identifying these can help prevent recurrence.
Footwear and Activity Triggers
- Stiff-backed shoes: Ice skates, dress shoes, and high heels rub against the heel, causing bursitis.
- Lack of cushioning: Thin-soled shoes increase impact on the calcaneus.
- Sudden activity spikes: Starting a new workout routine too aggressively causes microtrauma.
Biomechanical Contributors
- Flat feet (pes planus): Stretch the plantar fascia and strain the Achilles.
- High arches (pes cavus): Concentrate pressure on the heel and ball of the foot.
- Overpronation: Rolls the foot inward, twisting the Achilles and irritating the heel.
Physical and Medical Risks
- Tight calf muscles: Limit ankle motion, increasing tendon tension.
- Obesity: Adds up to 3–4 times body weight in force on the heel with each step.
- Age: Tendons lose elasticity over time, making degeneration more likely.
✅ Prevention Tip: Stretch calves daily and wear supportive, well-fitted shoes.
Diagnosing the Cause of Heel Swelling
Accurate diagnosis is crucial—because treatments for bursitis, gout, and infection are vastly different. A combination of clinical exam and imaging helps pinpoint the issue.
Clinical Evaluation Steps
- Medical history: Onset, duration, footwear, activity level, systemic symptoms.
- Palpation: Determines if tenderness is deep (retrocalcaneal) or superficial (subcutaneous).
- Range of motion test: Pain with dorsiflexion suggests bursitis or Achilles issues.
- Gait analysis: Reveals overpronation, limb length discrepancy, or limping.
Imaging for Confirmation
| Test | What It Shows |
|---|---|
| X-ray | Detects Haglund’s deformity, heel spurs, fractures |
| Ultrasound | Real-time view of bursae, tendons, fluid; guides injections |
| MRI | Best for soft tissue: shows bursitis, tendinopathy, bone edema, infection |
✅ When to Get Imaging: If pain lasts over 2–3 weeks despite rest, or if infection is suspected.
Final Note
Localized swelling on the heel bone is not a single condition—it’s a symptom with multiple possible causes. From bursitis and Haglund’s deformity to trauma, tendinopathy, and systemic diseases, each has unique triggers and treatments. Early recognition of patterns—like shoe-related pain, bilateral involvement, or sudden red-hot swelling—can guide timely care. Addressing risk factors like footwear, calf tightness, and activity level can prevent recurrence. When in doubt, consult a foot specialist and consider imaging to avoid misdiagnosis. With the right approach, most causes of heel swelling are manageable and often preventable.