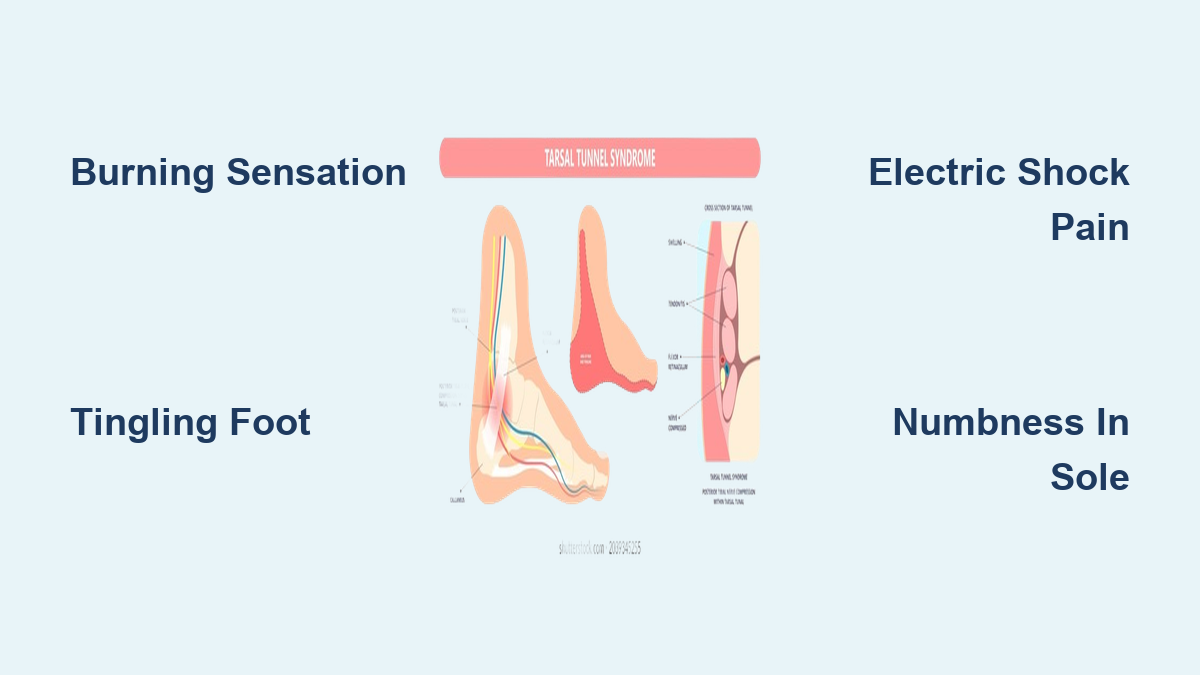
If you’ve ever felt a sharp, electric shock shooting through your ankle when walking, or woken up at night with a burning sensation in the sole of your foot, you might be experiencing signs of tarsal tunnel syndrome (TTS). This lesser-known but painful nerve condition occurs when the posterior tibial nerve—the main nerve supplying sensation to the bottom of your foot—gets compressed as it passes through a tight space on the inside of your ankle. Often mistaken for plantar fasciitis or general foot pain, TTS causes distinct neurological symptoms that shouldn’t be ignored.
Left untreated, tarsal tunnel syndrome can lead to chronic pain, muscle weakness, and even permanent nerve damage. But recognizing the signs early—like numbness, tingling, or shooting pain radiating from your inner ankle down into your foot—can make all the difference in recovery. Whether you’re an athlete, have flat feet, or deal with diabetes, understanding these warning signals helps you take action before symptoms worsen. In this guide, we’ll break down the key signs of tarsal tunnel syndrome, how it differs from similar conditions, and what steps to take next.
Early Warning Signs of Tarsal Tunnel Syndrome
The first signs of tarsal tunnel syndrome often appear subtly and may come and go. Because they’re triggered by activity and relieved by rest, many people dismiss them as fatigue or minor foot strain. But these early symptoms are your body’s way of signaling nerve irritation—and catching them now improves your chances of successful treatment without surgery.
Burning or Tingling in the Foot
One of the earliest and most common signs is a persistent burning sensation along the inner ankle or sole of the foot. This isn’t surface-level skin irritation—it’s a deep, searing feeling that often spreads across the heel, arch, or toes. You might also experience “pins and needles” (paresthesia), especially after standing for long periods or finishing a workout. These sensations follow the path of the posterior tibial nerve, which splits into branches that supply much of the bottom of your foot.
Pro tip: If the tingling wakes you up at night or feels worse when you first start walking, it’s likely neurological—not muscular.
This burning usually starts intermittently but can become constant over time. It’s often described as a “hot wire” running through the foot and may intensify during or after physical activity. Unlike typical muscle soreness, this sensation doesn’t resolve quickly with rest.
Numbness in the Sole or Toes
As nerve compression progresses, areas of reduced sensation develop. You may notice your foot feels “dead” or less responsive, particularly under the heel or ball of the foot. Some patients report feeling like they’re walking on cotton or wearing an invisible sock. This numbness typically affects one foot, though both sides can be involved, especially in systemic conditions like diabetes.
Avoid ignoring this symptom. Persistent numbness increases your risk of injury because you lose protective sensation—stepping on sharp objects or developing pressure sores without realizing it. It also interferes with balance and coordination, increasing fall risk.
Shooting or Electric Shock-Like Pain
Many patients describe sudden, lancinating pain—a jolt of electricity that zips from the ankle into the foot or up toward the calf. This often happens when you flex your foot, stand up quickly, or press on the inner ankle. It’s a hallmark sign of nerve entrapment and differentiates TTS from purely musculoskeletal issues like tendonitis or arthritis.
⚠️ Red flag: If tapping lightly on the inside of your ankle triggers radiating pain or tingling, you’re likely experiencing Tinel’s sign, a strong indicator of nerve irritation.
This type of pain is often unpredictable and can be triggered by simple movements like climbing stairs or rolling your ankle slightly. The shock-like nature of the pain is a clear warning that nerve tissue is under stress.
When Symptoms Begin to Worsen
Tarsal tunnel syndrome symptoms often begin intermittently but can become constant over time. Knowing what makes them worse—and how they evolve—helps confirm whether your discomfort aligns with nerve compression rather than another foot problem.
Pain Increases With Activity
Early-stage TTS usually flares up during or after physical activity. Common triggers include:
- Prolonged standing
- Walking long distances
- Running or jumping
- Starting a new exercise routine
This happens because movement increases pressure within the tarsal tunnel, further compressing the nerve. The pain may ease with rest, reinforcing the idea that it’s just “overuse.” But unlike muscle soreness, nerve pain doesn’t fully resolve—it returns faster and lasts longer with each episode.
Key clue: If your foot feels better in the morning but worsens throughout the day, nerve compression is likely involved.
The cumulative stress of daily activities can gradually worsen nerve irritation, leading to more frequent and intense flare-ups. Over time, even mild activity may trigger symptoms.
Nighttime Symptoms Disrupt Sleep
As the condition advances, symptoms can occur at rest or at night, even without recent activity. You may wake up with:
- Throbbing or burning in the foot
- Cramping or twitching sensations
- Unexplained tingling that keeps you awake
Nocturnal pain is a sign of progressive nerve irritation and suggests more significant compression. It’s also a key differentiator from plantar fasciitis, which causes morning heel pain but typically improves with walking. If your foot pain wakes you up, especially with a burning or electric sensation, it’s time to consider nerve involvement.
Gradual Loss of Foot Strength
Over time, motor nerves can be affected, leading to foot weakness. You might notice:
- Difficulty curling your toes
- A feeling of instability when walking
- Changes in your gait (walking pattern)
In severe cases, weakened muscles can contribute to flat feet or difficulty maintaining balance, creating a cycle that worsens nerve compression. Some people report tripping more often or feeling like their foot “gives out” during activity.
How Tarsal Tunnel Differs From Similar Conditions

Because the symptoms of tarsal tunnel syndrome overlap with other foot problems, it’s frequently misdiagnosed. Understanding the differences ensures you get the right treatment—and avoid wasting time on therapies that won’t help.
Tarsal Tunnel vs Plantar Fasciitis
| Feature | Tarsal Tunnel Syndrome | Plantar Fasciitis |
|---|---|---|
| Pain Location | Inner ankle, sole, heel, toes | Bottom of heel, arch |
| Pain Pattern | Worse with activity, often at night | Worst with first steps in the morning |
| Numbness/Tingling | Common | Absent |
| Tinel’s Sign | Positive (tapping causes shocks) | Negative |
| Nerve Involvement | Yes | No |
While both conditions cause heel and arch pain, only TTS includes neurological symptoms like numbness, tingling, or electric shocks.
Tarsal Tunnel vs Morton’s Neuroma
Morton’s neuroma affects the ball of the foot, usually between the third and fourth toes. It causes:
- Sharp, burning pain in the forefoot
- Feeling like there’s a pebble in your shoe
- Numbness in adjacent toes
Unlike TTS, it doesn’t affect the heel, arch, or inner ankle. It’s also closely linked to tight footwear and high heels—less so to biomechanical issues like flat feet.
Tarsal Tunnel vs Peripheral Neuropathy
Peripheral neuropathy—common in diabetes—typically causes bilateral, symmetrical symptoms:
- Numbness and tingling starting in the toes
- “Stocking-glove” distribution
- Often affects both feet equally
TTS, in contrast, is usually unilateral and localized to the tarsal tunnel pathway. However, diabetes increases your risk of both conditions, making accurate diagnosis critical.
Confirming the Diagnosis: What to Expect

Diagnosing tarsal tunnel syndrome requires more than just symptom recognition. A healthcare provider will use clinical tests and imaging to confirm nerve compression and rule out mimics.
Positive Tinel’s Sign at the Ankle
Your doctor may perform Tinel’s test by gently tapping over the posterior tibial nerve just behind the medial malleolus (the bony bump on the inside of your ankle). If you feel radiating tingling, buzzing, or shooting pain into your foot, the test is positive—strong evidence of nerve irritation.
🔍 This simple bedside test is one of the most reliable indicators of TTS.
Nerve Conduction Studies (NCV/EMG)
Nerve conduction velocity (NCV) and electromyography (EMG) measure how well electrical signals travel through the nerve and muscles. Slowed conduction in the posterior tibial nerve confirms compression and helps assess severity.
These tests are especially useful when:
- Symptoms are unclear
- Surgery is being considered
- You have diabetes or other neuropathies
Imaging to Rule Out Structural Causes
While X-rays can’t show nerves, they help detect bone spurs or arthritis that might contribute to compression.
More detailed imaging includes:
- MRI: Best for identifying soft tissue masses (e.g., ganglion cysts, lipomas), tenosynovitis, or nerve swelling.
- Ultrasound: Can visualize nerve enlargement and dynamic compression during movement. It’s less expensive and faster than MRI.
✅ Imaging is crucial if symptoms don’t improve with conservative care.
Immediate Actions to Reduce Symptoms
Once you suspect tarsal tunnel syndrome, taking early action can prevent progression and reduce the need for invasive treatments.
Rest and Avoid Aggravating Activities
Stop or modify activities that worsen your symptoms. This means:
- Avoiding prolonged standing or walking
- Taking a break from running or jumping
- Limiting time in unsupportive shoes
Even a few days of reduced stress can give the nerve a chance to recover.
🕒 Recovery tip: Think of nerve healing like a sprained ankle—it needs time and protection.
Apply Ice and Elevate the Foot
Use the RICE method (Rest, Ice, Compression, Elevation):
- Ice: Apply for 15–20 minutes, 3–4 times daily to reduce inflammation.
- Compression: Wear a light elastic bandage or ankle sleeve to minimize swelling.
- Elevation: Prop your foot above heart level when sitting or lying down.
This combo helps decrease pressure in the tarsal tunnel.
Try Over-the-Counter Pain Relief
NSAIDs like ibuprofen or naproxen can reduce inflammation and ease pain. They won’t fix the nerve compression, but they can make daily activities more tolerable while you pursue further evaluation.
⚠️ Don’t rely on painkillers long-term—they mask symptoms without treating the cause.
Long-Term Management Strategies

To fully resolve tarsal tunnel syndrome, especially if it’s linked to biomechanics or chronic conditions, long-term strategies are essential.
Wear Supportive Shoes and Orthotics
Footwear plays a major role. Choose shoes with:
- Firm heel counters
- Good arch support
- Motion control features (especially if you overpronate)
Custom orthotics are often recommended to correct flat feet and reduce nerve strain. Even over-the-counter arch supports can provide relief in mild cases.
✅ Pro tip: Replace worn-out shoes every 300–500 miles of walking or running.
Start Targeted Stretching Exercises
Tight calf muscles increase tension on the posterior tibial nerve. Daily stretching can help:
- Wall stretch: Stand facing a wall, place hands on it, and step one foot back. Keep the back heel down and lean forward until you feel a stretch in the calf.
- Downward dog: A yoga pose that elongates the calves and Achilles tendon.
Do 2–3 sets of 30 seconds per leg, twice daily.
Consider Physical Therapy
A physical therapist can design a program that includes:
- Ankle range-of-motion exercises
- Strengthening for foot and ankle stabilizers
- Gait retraining to reduce nerve strain
Therapy is especially beneficial if you’ve had prior ankle injuries or muscle imbalances.
Final Note
Tarsal tunnel syndrome is more than just foot pain—it’s a warning sign of nerve compression that requires attention. The key signs—burning, tingling, numbness, and electric shock-like pain in the inner ankle and sole of the foot—are distinct from common musculoskeletal issues. Early recognition, proper diagnosis, and targeted treatment can prevent permanent nerve damage and restore full function. If you’re experiencing these symptoms, especially with risk factors like flat feet or a history of ankle injury, don’t wait. See a podiatrist or foot specialist to get the right care and get back on your feet—pain-free.