Callus removers are specialized tools and treatments designed to reduce or eliminate thickened, hardened patches of skin caused by repeated friction, pressure, or irritation—most commonly on the feet and hands. These products work by softening, exfoliating, or chemically breaking down layers of dead skin cells to improve comfort, appearance, and mobility. With options ranging from medicated creams to electric files, many people turn to callus removers for quick relief from rough, cracked heels or painful pressure spots. But a pressing question remains: Are they safe to use?
While some callus removal methods are effective and low-risk for healthy individuals, others—particularly chemical-based treatments—can lead to serious complications if misused. Chemical burns, infections, and even systemic toxicity are real risks, especially in people with diabetes, poor circulation, or sensitive skin. This guide breaks down what callus removers are, how they work, and which types are safest. You’ll learn the common causes of calluses, how to remove them safely at home, who should avoid self-treatment, and when it’s time to see a professional.
Types of Callus Removers: Tools and Treatments Explained

Callus removers fall into three main categories: chemical, mechanical, and preventive aids. Each has its pros and cons, and understanding the differences is key to choosing a safe, effective method.
Chemical Exfoliants: Dissolving Thick Skin with Active Ingredients
Chemical callus removers use ingredients that break down keratin—the protein in dead skin cells—through a process called keratolysis. While effective, these products require careful use.
Salicylic Acid: Powerful but Potentially Dangerous
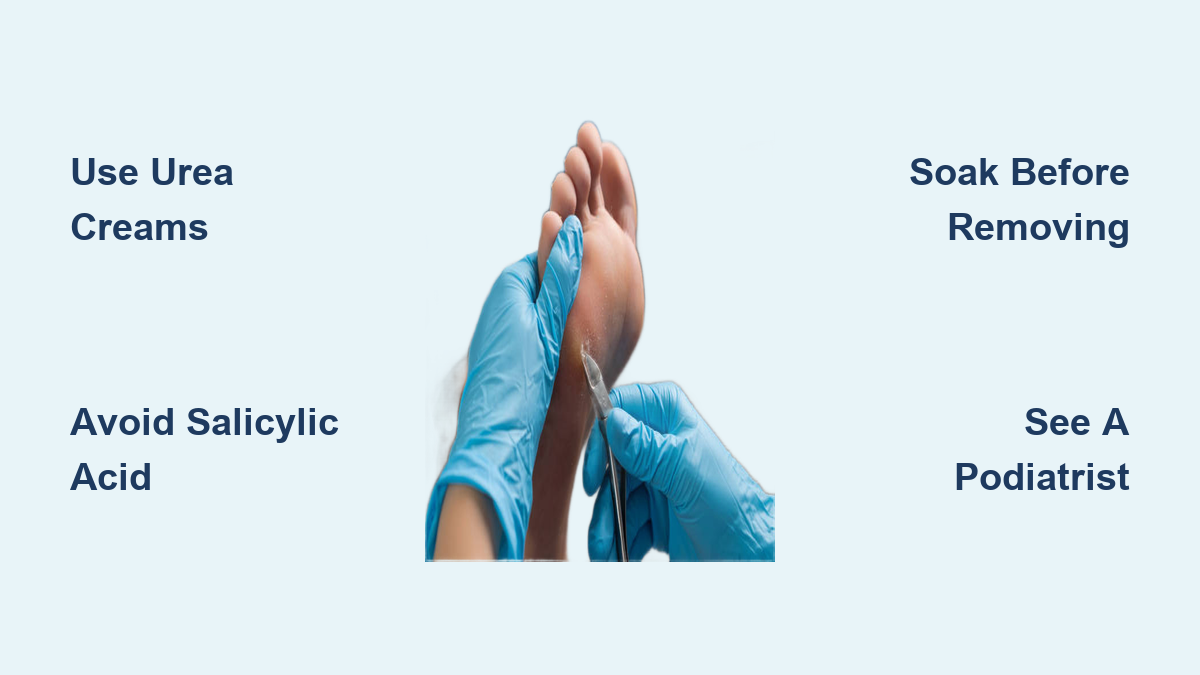
Found in gels, patches, and liquids (like Dr. Scholl’s Clear Away), salicylic acid is one of the most common active ingredients in OTC callus removers. Over-the-counter versions typically contain up to 17%, while medical-grade formulas can go as high as 40%. It works by dissolving the bonds between dead skin cells, allowing them to shed gradually.
Important Warning: Salicylic acid doesn’t differentiate between thickened callus and healthy skin. Overuse or prolonged application can lead to chemical burns, open sores, or scarring—especially on thin or sensitive skin.
These patches are often left on for 48 hours and should be used strictly according to instructions. Never apply over large areas or on broken skin.
Urea Creams: Safe, Hydrating, and Effective
Urea is a humectant that draws moisture into the skin while disrupting keratin structure. Found in concentrations of 10% to 40%, urea-based creams (such as Eucerin Roughness Relief or CeraVe SA Cream) are gentler than salicylic acid and ideal for dry, cracked heels.
They work slowly but safely, making them suitable for daily use. Unlike harsher chemicals, urea helps repair the skin barrier while softening calluses.
Glycolic and Lactic Acids: Mild Exfoliation for Sensitive Skin
As alpha-hydroxy acids (AHAs), glycolic and lactic acids gently loosen dead skin cells. Often included in foot creams, they’re best for mild roughness rather than thick calluses. These acids are less aggressive and more moisturizing, making them a good choice for maintenance.
Mechanical Removal Tools: Physical Exfoliation Done Right
These tools physically file away dead skin and are generally safer when used correctly—especially for healthy individuals.
Pumice Stones: Gentle and Natural
Made from volcanic rock, pumice stones offer a mild abrasive surface. For best results, soak your feet for 10 minutes to soften the skin, then use light, circular motions. Avoid aggressive scrubbing, which can cause micro-tears.
Pro Tip: Clean and dry your pumice stone after each use to prevent bacterial or fungal buildup.
Foot Files and Emery Boards: For Tougher Skin
More aggressive than pumice, metal-grated foot files remove thick skin quickly. Use them only on softened skin—ideally during or after a shower. Apply even, gentle pressure; pressing too hard can damage healthy tissue.
Electric Callus Removers: Fast but Risky if Overused
Battery-powered devices with rotating sanding heads offer quick results. Many have adjustable speeds and safety guards to prevent over-sanding. However, it’s easy to remove too much skin, especially if you don’t stop at the first sign of redness or warmth.
Caution: Never use on inflamed, broken, or numb skin. Discontinue immediately if discomfort occurs.
Protective and Preventive Aids: Stop Calluses Before They Start
These products don’t remove existing calluses but help prevent them by reducing pressure and friction.
Silicone and Gel Pads: Cushion High-Pressure Zones
Donut-shaped pads relieve pressure around calluses, while toe sleeves and heel cups protect vulnerable areas. Reusable and non-irritating, they’re ideal for long-term wear.
Orthotics and Insoles: Fix the Root Cause
Custom or over-the-counter orthotics correct gait imbalances, flat feet, or high arches that contribute to callus formation. By redistributing weight evenly, they reduce friction and prevent recurrence.
Proper Footwear: The First Line of Defense
Shoes with wide toe boxes, low heels, and good arch support prevent calluses from forming. Replace worn-out shoes every 6–12 months, and measure your feet annually—size can change over time.
Why Calluses Form: Addressing the Real Cause

Calluses are your body’s natural defense against repeated stress. Common causes include:
- Tight or ill-fitting shoes that rub against toes or heels
- High-impact activities like running or standing for long hours
- Foot deformities such as bunions, hammertoes, or bone spurs
- Gait abnormalities that shift pressure unevenly
- Dry skin, which cracks and thickens more easily
- Occupational stress, like playing instruments or manual labor
While initially painless, untreated calluses can become painful, split open, or press on nerves. Treating only the surface without addressing the cause leads to recurring problems.
Are Callus Removers Safe? Key Risks You Must Know

Despite being widely available, many callus removers carry serious risks—especially when used improperly.
Chemical Burns from Salicylic Acid
High-dose patches continue working under occlusion (bandaging), potentially damaging healthy skin. One patch left too long can cause a deep ulcer—particularly dangerous for older adults or those with thin skin.
Infection After Skin Damage
Over-sanding, cutting, or chemical burns create entry points for bacteria and fungi. Staph infections, cellulitis, and athlete’s foot are common. In severe cases, infection can spread to the bone (osteomyelitis) or bloodstream (sepsis)—especially in people with diabetes or poor circulation.
Misdiagnosing Warts as Calluses
Plantar warts (caused by HPV) often look like calluses but bleed when pared down and show tiny black dots (clotted blood vessels). Using salicylic acid on a wart can spread the virus and worsen the infection.
Expert Tip: A podiatrist can pare the lesion to confirm—no bleeding means it’s likely a callus.
Systemic Toxicity from Skin Absorption
Salicylic acid can enter the bloodstream, especially when applied to large or broken skin areas. Symptoms of salicylism include dizziness, nausea, and ringing in the ears. In rare cases, it can cause breathing issues or metabolic imbalances.
Children with viral infections (like chickenpox or flu) are at risk of Reye’s syndrome, a life-threatening condition linked to salicylate absorption.
Harmful Additives in Commercial Products
Many callus creams contain unsafe chemicals. Avoid:
| Chemical | Risk |
|---|---|
| Hydroquinone | Skin darkening, possible carcinogen |
| Formaldehyde | Known carcinogen, irritates skin and lungs |
| Parabens | Hormone disruption, linked to estrogenic effects |
| Phthalates | Reproductive toxicity, hidden in fragrances |
| SLS | Strips natural oils, worsens dryness |
| Synthetic Fragrances | Allergies, hormone interference |
| Ammonium Hydroxide | Causes chemical burns |
| Resorcinol | Thyroid disruption, skin irritation |
Safer Choice: Opt for fragrance-free, paraben-free, and chemical-minimal products.
Who Should Never Self-Treat
Do not use callus removers at home if you have:
- Diabetes (neuropathy means you may not feel injuries)
- Peripheral arterial disease (PAD) (poor blood flow slows healing)
- Neuropathy (loss of sensation increases wound risk)
- Weakened immune system (higher infection risk)
- Elderly skin (thinner, more fragile, slower to heal)
Medical Advice: If you have diabetes or circulation issues, see a podiatrist before using any remover—even a pumice stone.
Safe Callus Removal Steps for Healthy Individuals
Follow this routine to remove calluses safely:
- Soak feet in warm water for 10 minutes
- Gently exfoliate with a pumice stone or foot file—use light, circular motions
- Rinse and pat dry—stop if skin stings, bleeds, or turns red
- Moisturize daily with urea, lactic acid, or petroleum jelly
- Wear cotton socks overnight to lock in moisture
- Use silicone pads to reduce pressure
- Wear proper shoes with good support and wide toe boxes
When to See a Podiatrist
Seek professional help if:
– Callus doesn’t improve in 3 weeks
– You have pain, swelling, or pus
– You have diabetes or circulation issues
– You suspect a wart
– Calluses keep coming back
Podiatrists offer safer treatments, including:
– Debridement (sterile trimming)
– Custom orthotics
– Medical-grade patches (supervised use)
– Surgical correction for bone deformities
Final Verdict: Are Callus Removers Safe?
Yes—but only when used correctly and by the right people.
For healthy adults, urea creams and mechanical tools are safe when used gently. Salicylic acid products can work but carry real risks.
Never self-treat if you have diabetes or poor circulation. A small mistake can lead to serious complications.
The safest approach? Prevent calluses with proper footwear, daily moisturizing, and protective pads. When in doubt, skip the remover and see a podiatrist. Your feet carry you every day—protect them wisely.