If you’ve ever felt a sharp edge of your toenail digging into the skin, you’re not alone. An infected ingrown toenail starts when the nail grows into the surrounding flesh—usually the big toe—and bacteria invade the broken skin. While mild cases cause discomfort, an infection turns this common problem into a medical concern. Left untreated, it can lead to pus, spreading redness, and even serious complications like bone infection or amputation, especially in people with diabetes.
Recognizing the signs of an infected ingrown toenail early is crucial. This guide breaks down the warning signs, when to see a doctor, and how to prevent the condition from worsening. You’ll learn what separates a simple ingrown nail from a full-blown infection—and what steps to take next.
What Causes Ingrown Toenails to Become Infected?
An ingrown toenail begins as a mechanical issue—the nail edge cuts into the soft tissue of the toe. But once the skin breaks, bacteria like Staphylococcus and Streptococcus can enter, turning it into an infection. Several factors increase the risk of this progression.
Cutting Toenails Too Short or at an Angle
Trimming nails too short or rounding the corners encourages the nail to curl downward and pierce the skin. Always cut straight across and leave the nail slightly longer than the tip of your toe to prevent this.
Wearing Tight or Narrow Shoes
Footwear that squeezes the toes—like high heels, narrow dress shoes, or tight athletic sneakers—pushes the nail into the skin. Over time, this pressure alters nail growth and increases the risk of injury and infection.
Toe Injuries or Repetitive Pressure
Stubbing your toe, dropping something on it, or constant pressure from running or kicking can damage the nail bed. This trauma may cause the nail to grow abnormally, increasing the likelihood of ingrowth.
Natural Nail Shape and Genetics
Some people inherit curved or wide toenails that naturally grow into the skin, regardless of care habits. If you’ve had repeated ingrown nails, your anatomy may be a contributing factor.
Poor Foot Hygiene and Moisture Buildup
Sweaty socks and closed shoes create a warm, damp environment where bacteria thrive. Failing to dry your feet thoroughly—especially between the toes—makes it easier for infection to take hold once the skin is broken.
Who Is at Higher Risk for Complications?

Not everyone with an ingrown toenail will develop an infection, but certain health conditions dramatically increase the danger.
Diabetics Face Silent Dangers
People with diabetes often have reduced sensation in their feet (neuropathy) and poor circulation. This means they might not feel the early pain of an ingrown nail, allowing the infection to progress unnoticed until it’s severe.
Poor Blood Flow Slows Healing
Peripheral vascular disease limits blood supply to the feet, weakening the body’s ability to fight infection and repair tissue. Even a small wound can become a major issue without adequate circulation.
Weakened Immune Systems
Conditions like HIV or treatments such as chemotherapy and long-term steroid use impair immune defenses, making infections more aggressive and harder to control.
History of Recurring Ingrown Toenails
Frequent episodes suggest an underlying issue—whether anatomical, behavioral, or both—that raises the risk of infection over time.
High-risk individuals should never ignore foot changes. Even minor redness or swelling warrants immediate attention.
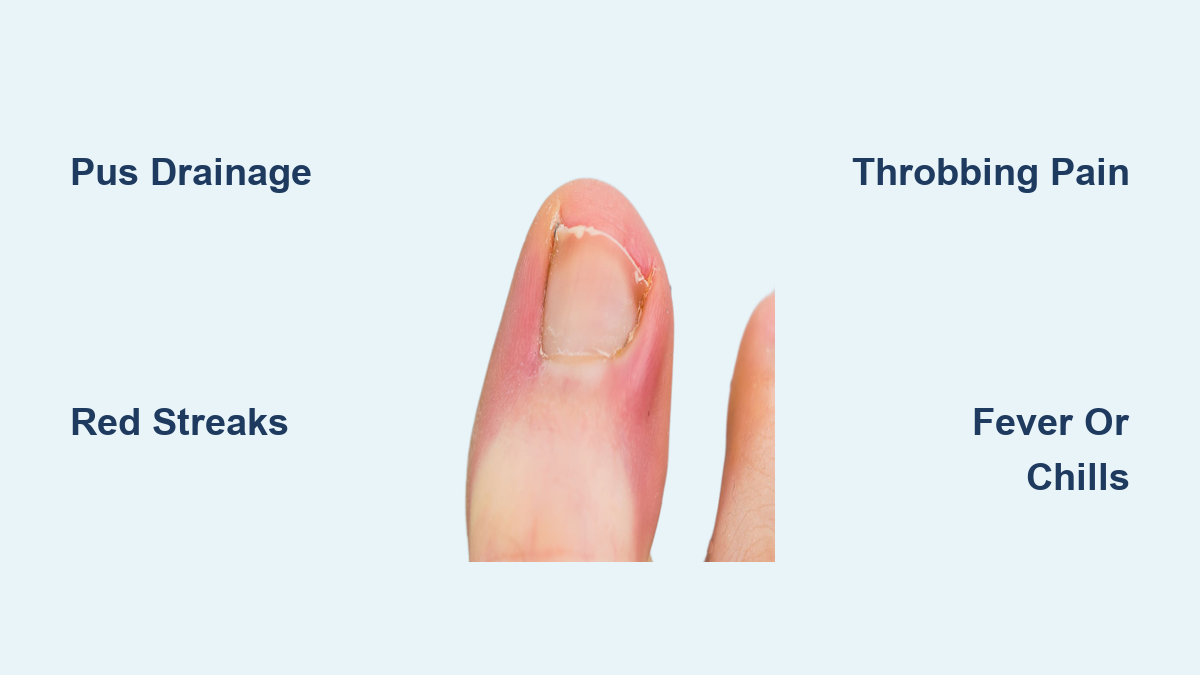
Early Warning Signs of Infection
Knowing the shift from discomfort to infection can prevent serious outcomes.
Throbbing, Persistent Pain
Mild ingrown nails hurt when pressed. But infection brings constant, pulsing pain—even when resting. Walking or wearing shoes becomes unbearable.
Expanding Redness Around the Toe
Some redness is normal with an ingrown nail. But if the redness spreads up the toe or foot, it’s a clear sign the infection is advancing.
Noticeable Swelling and Puffiness
The skin around the nail swells, sometimes making the entire toe look bloated. The area may feel tight or shiny due to fluid buildup.
Warmth in the Affected Area
An infected toe feels hotter than the surrounding skin. This warmth comes from increased blood flow and inflammation as your body fights the infection.
Pus or Cloudy Fluid Drainage
Yellow, green, or white fluid oozing from the nail fold is a definitive sign of infection. This pus contains bacteria, dead cells, and tissue debris.
Foul or Rotten Smell
A bad odor coming from the toe signals bacterial breakdown of tissue. Don’t ignore this—it’s a strong indicator of infection.
Nail Changes: Thickening or Discoloration
While often linked to fungus, yellowing, crumbling, or thickening of the nail can also result from chronic irritation and infection near the nail fold.
Danger Signs That Demand Immediate Care

Some symptoms mean the infection is spreading beyond the toe and requires urgent medical treatment.
Red Streaks Moving Up the Foot or Leg
These lines indicate lymphangitis—a serious condition where infection travels through the lymphatic system. This is a medical emergency requiring antibiotics and close monitoring.
Fever or Chills
A temperature above 100.4°F (38°C) or shaking chills means the infection may be entering your bloodstream—raising the risk of sepsis, a life-threatening condition.
Numbness, Tingling, or Loss of Sensation
These feelings may signal nerve damage or poor blood flow, especially in diabetics. Even without pain, tissue could be dying.
Black, Blue, or Gray Toes
Discoloration can indicate tissue death (gangrene), often due to infection combined with poor circulation. This requires emergency care to prevent amputation.
Seek help immediately if you see any of these red flags. Delaying treatment increases the risk of permanent damage.
When to See a Doctor: Don’t Wait
You don’t need to wait for severe symptoms to get help. Early intervention prevents complications.
Call a Healthcare Provider If:
- Pus appears or increases
- Redness spreads beyond the toe
- Pain worsens after 2–3 days of home care
- You develop fever, chills, or red streaks
- You have diabetes and notice any foot change
Diabetics should see a doctor at the first sign of trouble—even if pain is minimal.
Why Acting Fast Matters
Ignoring an infected ingrown toenail can lead to:
– Cellulitis: A spreading skin infection requiring strong antibiotics
– Abscess: A pocket of pus needing surgical drainage
– Osteomyelitis: Bone infection that may require IV antibiotics or surgery
– Gangrene and amputation: In extreme cases, especially among high-risk patients
Safe At-Home Care for Mild, Non-Infected Cases
Home treatment is only appropriate if there are no signs of infection.
Soak in Warm, Soapy Water
Soak the foot 3–4 times daily for 15–20 minutes in warm (not hot) water. Add 1–2 tablespoons of Epsom salt per quart to reduce swelling and draw out fluid.
Always dry thoroughly afterward—moisture fuels bacterial growth.
Gently Lift the Nail Edge
After soaking, use sterilized tweezers to place a tiny piece of cotton, dental floss, or gauze under the ingrown edge. This helps the nail grow above the skin.
Stop if it hurts. Forcing it can worsen the injury.
Wear Loose, Open-Toed Shoes
Reduce pressure by choosing wide-toe-box shoes or sandals. Avoid tight socks or hosiery that press on the toe.
Use Over-the-Counter Pain Relief
- Ibuprofen (Advil, Motrin): Reduces pain and inflammation
- Acetaminophen (Tylenol): For pain relief only
Avoid topical “ingrown toenail” remedies—they can irritate already sensitive skin.
Stop Home Care If Symptoms Worsen
Switch to professional care immediately if:
– Pain increases
– Redness spreads
– Pus develops
– No improvement in 48–72 hours
Professional Treatments for Infection
When infection is present, doctors can resolve it quickly and safely.
Partial Nail Removal (Avulsion)
The most common treatment. After numbing the toe with local anesthesia, the doctor removes the ingrown portion. Most patients feel immediate pain relief and can resume light activity the same day.
Total Nail Removal
Used for severe or recurrent infections. The entire nail is removed to access deeper infection or prepare for permanent correction.
Nail Lifting with Splinting
For early cases, the nail is gently lifted and a small splint inserted to guide growth—no cutting required.
Antibiotics: Fighting the Infection
Medication depends on severity.
Topical Antibiotics
For mild cases with minimal drainage. Applied after cleaning the area.
Oral Antibiotics
Prescribed for pus, swelling, redness, or fever. Common options include cephalexin, dicloxacillin, or clindamycin for those allergic to penicillin.
IV Antibiotics
Needed for deep infections, cellulitis, or systemic illness—usually in hospital settings.
Always finish the full course, even if symptoms improve.
Permanent Solutions for Recurring Ingrown Toenails

If you get ingrown toenails often, long-term fixes are available.
Matrixectomy: Stop the Nail from Growing Back
This procedure destroys the nail root (matrix) so the ingrown part won’t regrow.
Phenolization
- Phenol acid is applied after partial removal.
- Prevents regrowth with over 90% success rate.
Laser Matrixectomy
- Uses laser energy to destroy the matrix.
- Less bleeding and faster healing in some patients.
Surgical Excision
- The nail matrix is physically removed.
- Effective but may involve longer recovery.
These are done in-office with local anesthesia. Most people return to normal activities in days.
Prevention: Your Best Defense
Avoiding ingrown toenails is easier than treating them.
Trim Nails Straight Across
Never round the corners. Cut level with the toe tip and avoid cutting too short.
Choose Proper Footwear
Pick shoes with wide toe boxes. Avoid high heels and tight athletic shoes.
Keep Feet Clean and Dry
Wash daily and dry between toes. Change socks regularly.
Wear Protective Shoes at Work
Use steel-toed boots if your job involves foot hazards.
Inspect Feet Daily (Especially for Diabetics)
Check for:
– Redness
– Swelling
– Cuts
– Nail changes
Use a mirror if needed.
See a Podiatrist Regularly
High-risk individuals benefit from professional nail care and foot exams every 6–12 months.
Quick Reference: Infected vs. Non-Infected
| Symptom | Non-Infected | Infected |
|---|---|---|
| Pain | Mild, only with pressure | Severe, constant, throbbing |
| Redness | Localized | Spreading, red streaks |
| Swelling | Slight | Marked, entire toe puffy |
| Warmth | No | Yes, feels hot |
| Pus | None | Present (yellow/green) |
| Odor | None | Foul smell |
| Fever | No | Possible |
| Progression | Stable or improving | Worsening over 2–3 days |
Red Flags: Red streaks, fever, pus, no improvement in 48 hours, diabetic foot changes.
An infected ingrown toenail is not just a minor foot issue—it’s a warning sign your body needs help. From throbbing pain and pus to red streaks and fever, the symptoms tell a story of escalating infection. For people with diabetes or poor circulation, the stakes are even higher.
While early, non-infected cases may respond to warm soaks and proper trimming, any sign of infection demands professional care. Treatments like partial nail removal and antibiotics work fast. For recurring cases, permanent solutions like matrixectomy can end the cycle for good.
Prevention through proper nail care, footwear, and daily foot checks is your best defense. Catch it early. Treat it right. Protect your feet—because a small problem today can become a major crisis tomorrow.