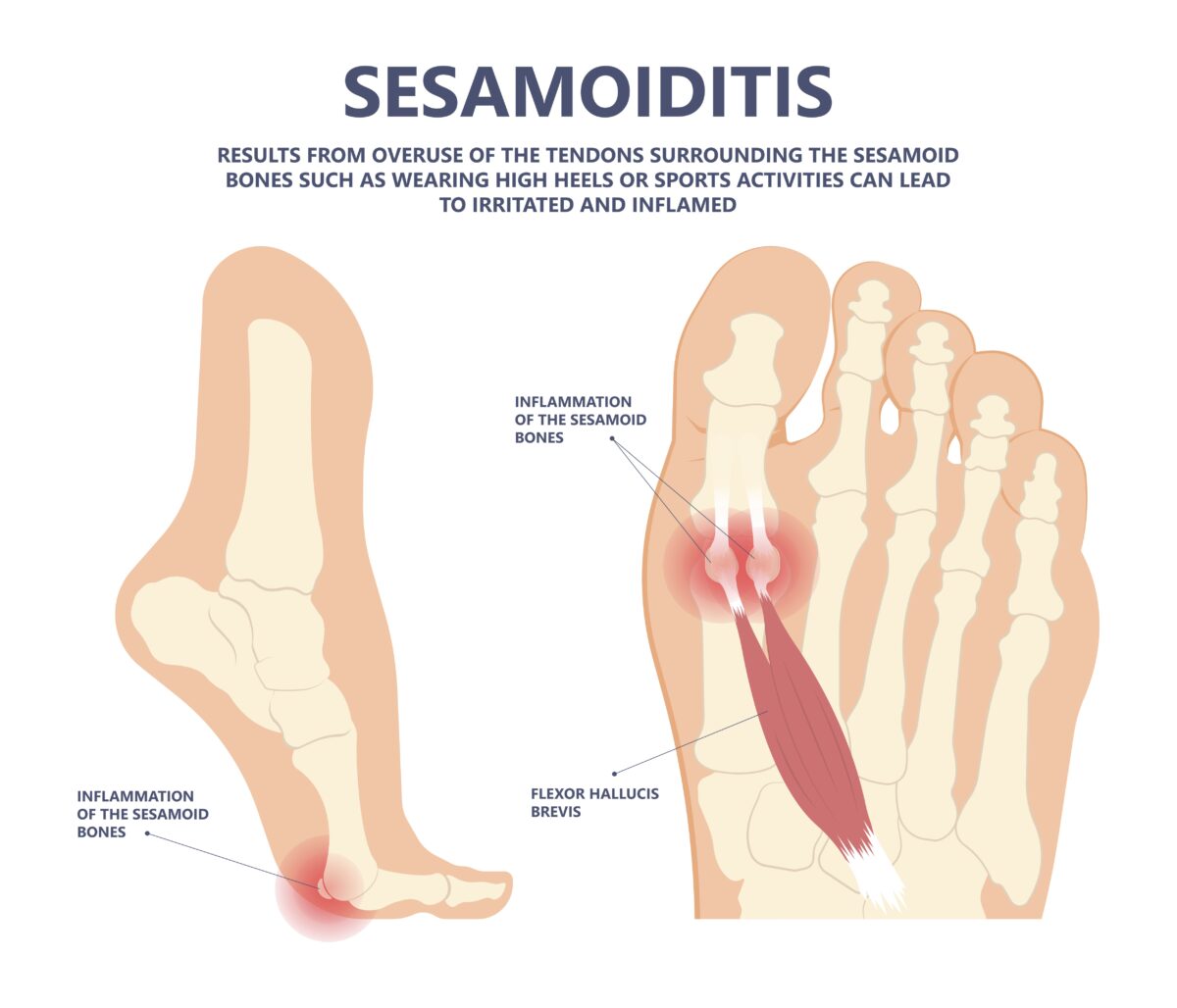
If you’ve been feeling a nagging ache beneath your big toe—especially when walking, running, or pushing off your foot—you may be dealing with sesamoiditis. This condition targets two tiny but powerful bones embedded in the tendons under the ball of your foot, just behind the big toe joint. Known as the sesamoid bones, these pea-sized structures act like pulleys, helping your foot generate force during movement. But when subjected to repetitive stress, they become inflamed, leading to pain that can disrupt daily life and sideline athletes, dancers, and active individuals.
Sesamoiditis is a common overuse injury, often mistaken for turf toe or gout. Unlike sudden trauma, it develops gradually—worsening with activity and easing with rest. Left untreated, it can progress to stress fractures or even avascular necrosis, where the bone deteriorates due to poor blood flow. The good news? Most cases respond well to conservative treatment. This guide will walk you through proven, step-by-step strategies to relieve pain, speed recovery, and prevent recurrence—based on clinical insights and real-world effectiveness.
Recognize the Early Signs of Sesamoiditis
Catching sesamoiditis early is key to avoiding long-term complications. Identifying the symptoms helps you take action before inflammation turns into chronic damage.
Understand the Pain Pattern
Sesamoiditis typically causes a dull, persistent ache directly under the big toe joint. The pain intensifies during weight-bearing activities like walking, climbing stairs, or running—especially on hard surfaces. High heels, thin-soled shoes, or minimalist footwear often make it worse by shifting more pressure to the forefoot. While rest usually brings relief, the pain returns once you resume activity.
Unlike turf toe, which results from a sudden hyperextension injury (like stubbing your toe), sesamoiditis develops slowly over days or weeks. There’s no “pop” or immediate swelling. Instead, discomfort builds with repeated strain. You might start limping to avoid putting full weight on the foot or find it painful to bend your big toe upward.
Check for Tenderness and Swelling
Press gently under the ball of your foot, just behind the big toe. If you feel pinpoint tenderness—especially on one side—it’s a strong sign of sesamoid involvement. Some people develop mild swelling or bruising, though these aren’t always visible. Pain when someone lifts your big toe upward (passive dorsiflexion) also points to sesamoid irritation.
If symptoms last more than a few days despite rest, it’s time to act. Early treatment prevents progression to stress fractures or avascular necrosis—a serious condition where the bone begins to die.
Rule Out Other Forefoot Conditions

Not all pain under the big toe is sesamoiditis. Accurate diagnosis ensures you treat the right issue.
Differentiate Sesamoiditis from a Fracture
A sesamoid fracture can mimic sesamoiditis but requires different management. Fractures often result from acute trauma or chronic stress. Pain is sharper and may persist even at rest. X-rays can detect obvious breaks, but stress fractures may not show up initially—requiring an MRI or bone scan for confirmation.
Sesamoiditis, in contrast, doesn’t involve a broken bone. Early X-rays are often normal, though long-term cases may show bone thickening (sclerosis) or fragmentation. If your pain started suddenly after an injury, imaging is essential to rule out a fracture.
Distinguish From Turf Toe, Gout, and Arthritis
Turf toe involves ligament damage from jamming or hyperextending the big toe—common in sports on artificial turf. It causes rapid swelling, instability, and limited motion. Gout strikes suddenly with intense redness, heat, and throbbing pain, often at night, and is linked to high uric acid levels.
Osteoarthritis, bunions, and Morton’s neuroma also cause forefoot pain. A podiatrist can differentiate these through physical exam and imaging. Never self-diagnose—misidentifying the problem delays healing and can worsen the injury.
Stop Aggravating Activities Immediately
The most effective first step in treating sesamoiditis is reducing pressure on the sesamoid bones.
Avoid High-Impact Movements
Running, jumping, dancing, and sprinting must stop until pain subsides. These activities generate forces up to three times your body weight on the forefoot—exactly what the inflamed sesamoids can’t handle. Continuing them risks microfractures or chronic damage.
You don’t need total bed rest, but avoid anything that worsens symptoms. Switch to low-impact alternatives: swimming, cycling, or upper-body strength training help maintain fitness without stressing the foot.
Use Crutches If Walking Hurts
If putting weight on the foot causes significant pain, use crutches to offload pressure. Partial weight-bearing allows healing while preserving mobility. “Pushing through” the pain only prolongs recovery and increases the risk of a stress fracture.
Most people see improvement within 2–3 weeks of activity modification. The key is consistency—returning too soon leads to setbacks.
Ice the Area to Reduce Inflammation
Cold therapy is a simple but powerful tool for calming inflammation and numbing pain.
Apply Ice the Right Way
Use ice for 15–20 minutes, 3–4 times daily—especially after standing or walking. Wrap a gel pack or frozen peas in a thin towel to protect your skin. Never apply ice directly.
Focus the cold on the tender spot under the big toe joint. Elevate your foot while icing to help reduce swelling. Many find evening icing especially helpful after a full day on their feet.
Avoid heat during the acute phase—it increases blood flow and can worsen inflammation. Save warm soaks for later, during rehabilitation.
Use Anti-Inflammatory Medications Wisely
Medications can help control pain and reduce swelling, supporting other treatments.
Take NSAIDs for Pain and Inflammation
Over-the-counter NSAIDs like ibuprofen (Advil) or naproxen (Aleve) reduce both pain and inflammation. Take them with food to protect your stomach. Limit use to 7–10 days unless directed by a doctor.
If NSAIDs aren’t safe for you (due to kidney issues or stomach ulcers), acetaminophen (Tylenol) offers pain relief—though it doesn’t reduce inflammation.
Try Topical Pain Relievers
Gels or creams containing diclofenac or menthol provide localized relief with fewer side effects. Apply directly to the painful area under the big toe. Some people combine topical treatments with oral meds for better control.
Always follow dosage guidelines and consult your healthcare provider if symptoms persist.
Wear Shoes That Reduce Forefoot Pressure
Footwear plays a major role in both causing and curing sesamoiditis.
Choose Supportive, Low-Heeled Shoes
Wear shoes with:
– Low heels (under 1 inch) to shift weight backward
– Cushioned soles to absorb impact
– Stiff midsoles that limit big toe flexion
– Wide toe boxes to avoid squeezing the forefoot
Avoid high heels, flip-flops, and worn-out athletic shoes—they increase pressure on the sesamoids. Replace running shoes every 300–500 miles or 6 months.
Dansko-style clogs or orthopedic shoes with rocker bottoms are excellent choices. They reduce push-off force and protect the sesamoid area.
Use Orthotics and Insoles to Offload Pressure

Custom or over-the-counter inserts help redistribute weight away from the painful spot.
Get Custom Orthotics for Long-Term Relief
Custom orthotics are the gold standard. Made from a mold of your foot, they include a sesamoid cutout—a small hole under the sesamoid bones—surrounded by a supportive ring that shifts pressure away.
They also correct biomechanical issues like high arches or overpronation. A podiatrist can prescribe them after gait analysis.
Try OTC Insoles with Metatarsal Support
If custom orthotics aren’t an option, use over-the-counter insoles with a metatarsal bar or donut pad. These lift and spread the metatarsal heads, reducing pressure on the sesamoids.
Test different brands—some offer immediate relief, while others may need adjustment.
Apply Padding and Tape to Limit Motion
External support helps reduce strain on the tendons pulling on the sesamoids.
Use Donut Pads to Offload the Sesamoids
A donut-shaped pad with a hole over the painful area shifts pressure to the surrounding tissue. Place it inside your shoe or on your foot under a sock.
Foam, gel, or felt pads work well. Cut the hole slightly larger than the tender spot to avoid direct pressure. Replace pads when they compress or lose shape.
Tape the Big Toe to Reduce Tendon Pull
Taping limits motion and reduces stress on the sesamoids. One effective method:
1. Sit with your foot flat.
2. Apply anchor strips above and below the joint.
3. Use a strip to gently compress the big toe toward the second toe.
4. Add stabilizing strips to hold position.
Kinesiology or athletic tape works. Learn the technique from a physical therapist to ensure proper tension.
Immobilize the Foot with a Walking Boot if Needed
For moderate to severe cases, immobilization gives the sesamoids time to heal.
Wear a CAM Walker for 4–8 Weeks
If rest, ice, and padding don’t help within 2–3 weeks, consider a CAM walker (walking boot). It limits motion and prevents toe flexion, reducing stress on the sesamoids.
Wear it for 4–8 weeks, depending on severity. You can bear weight on it, but avoid prolonged standing. Remove it at night and for hygiene.
This is especially important if a stress fracture is suspected.
Try a Stiff-Soled Surgical Shoe
If a boot feels too restrictive, a stiff-soled shoe with a rigid shank offers similar protection. It stops the foot from bending at the forefoot, minimizing push-off forces.
Use either option consistently—partial compliance delays healing.
Explore Advanced Treatments for Stubborn Pain

When conservative care fails, newer therapies can help.
Try Shockwave Therapy for Chronic Cases
Extracorporeal shockwave therapy (ESWT) uses sound waves to stimulate healing. Studies show 90% of patients report pain reduction after 6 sessions.
Treatment schedule:
– First 3 sessions: weekly
– Next 3: spaced over 6 weeks
Peak benefit occurs at 12–16 weeks. Each session costs ~$200 and is rarely covered by insurance. But it’s non-invasive and promotes actual tissue repair.
Best for chronic sesamoiditis unresponsive to 3+ months of standard care.
Consider PRP or Laser Therapy
Platelet-rich plasma (PRP) injections deliver growth factors to the injured area. Though not widely studied for sesamoiditis, it’s used for chronic tendon issues.
Low-level laser therapy (LLLT) reduces inflammation and may speed recovery. Administered in multiple clinic visits, it’s painless and safe.
These are second-line options—discuss with a foot specialist.
Begin Rehab Exercises Once Pain Subsides
Once pain decreases, physical therapy rebuilds strength and prevents relapse.
Stretch Tight Calf Muscles
Tight calves increase forefoot pressure. Stretch daily:
Gastrocnemius stretch:
– Stand facing a wall, back leg straight, heel down
– Lean forward, hold 30 seconds, 3 reps per side
Soleus stretch:
– Same position, but bend the back knee
– Hold 30 seconds, 3 reps
Do both twice daily.
Strengthen Foot and Calf Muscles
Towel crunches: Scrunch a towel toward you with your toes—10–15 reps per foot.
Calf raises: Rise onto toes slowly, lower with control—start with 10–15 reps.
Single-leg balance: Stand on one foot, hold 30 seconds, progress by closing your eyes.
Perform exercises barefoot on a firm surface. Stop if pain increases.
Follow a Realistic Recovery Timeline
Healing takes time—rushing back leads to setbacks.
Expect 6–12 Weeks for Full Recovery
Most people improve within 6–12 weeks with consistent care. Athletes may take 3–6 months to return to full sport.
Phases:
– Weeks 1–3: Rest, ice, NSAIDs, shoe changes
– Weeks 4–8: Begin orthotics, padding, PT
– Weeks 8–12+: Gradual return to activity
Listen to your body. If pain returns, scale back.
Return to Activity Safely
Start with non-weight-bearing exercise. Then add:
– Walking in supportive shoes
– Low-impact cardio (bike, elliptical)
– Short runs on soft surfaces
Increase by no more than 10% per week. Wear orthotics and consider taping during early return.
Reserve Surgery for Severe, Unresponsive Cases
Surgery is rare—only considered after 6–12 months of failed conservative treatment.
Sesamoidectomy: Removal of the Damaged Bone
Removal of the affected sesamoid (sesamoidectomy) is the only surgical option. Only one sesamoid should be removed—taking both risks big toe instability or deformity.
Indications:
– Chronic pain disabling daily life
– Confirmed non-healing stress fracture
– Avascular necrosis
Recovery includes 4–6 weeks of limited weight-bearing, then physical therapy. Full return to activity takes 3–6 months.
Weigh risks carefully—surgery alters foot mechanics permanently.
Prevent Future Episodes with Smart Habits
Once healed, prevent recurrence with proactive care.
Wear Supportive Shoes Daily
Make cushioned, low-heeled shoes your default. Avoid high heels and flip-flops. Rotate athletic shoes regularly.
Keep Doing Foot Strengthening Exercises
Continue towel crunches, calf raises, and balance drills 2–3 times per week. Strong feet resist overload.
Warm Up and Progress Gradually
Always warm up before activity. Increase training intensity slowly—no sudden spikes in mileage or hill work.
Use taping or padding during high-risk activities like dance or sprinting.
Final Note: Sesamoiditis is treatable with early, consistent care. Focus on offloading the sesamoids, reducing inflammation, and correcting biomechanics. Most people recover fully without surgery. If pain persists, consult a podiatrist for personalized management. With the right approach, you can get back on your feet—pain-free.