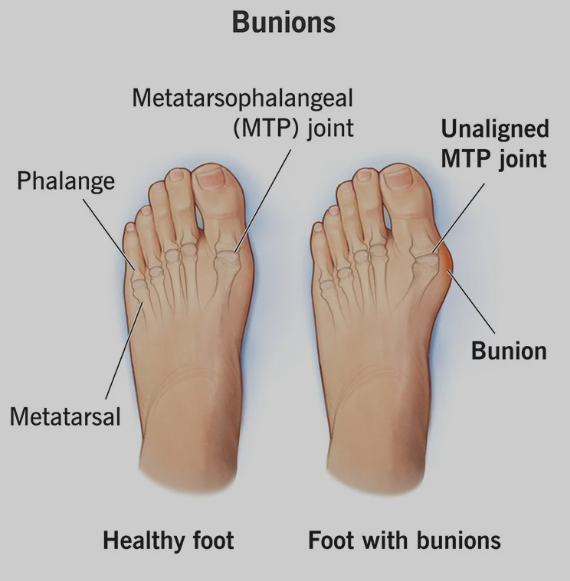
If you’ve noticed a hard, bony bump forming at the base of your big toe, you may be dealing with a bunion—medically known as hallux valgus. This common foot deformity affects millions and goes beyond just a cosmetic issue. It’s a progressive structural misalignment of the metatarsophalangeal (MTP) joint, where the big toe connects to the foot. Over time, the joint shifts, causing the big toe to drift inward toward the second toe while the bone at its base pushes outward, creating the visible bump.
Bunions don’t develop overnight. They evolve gradually, often over years, due to a combination of genetic predisposition, abnormal foot mechanics, and external pressures like ill-fitting shoes. While some people experience no pain, others suffer from swelling, redness, stiffness, and sharp pain—especially when wearing tight footwear. Left untreated, bunions can lead to complications such as hammertoes, bursitis, arthritis, and difficulty walking. Understanding what causes a bunion is the first step toward preventing progression and managing symptoms effectively.
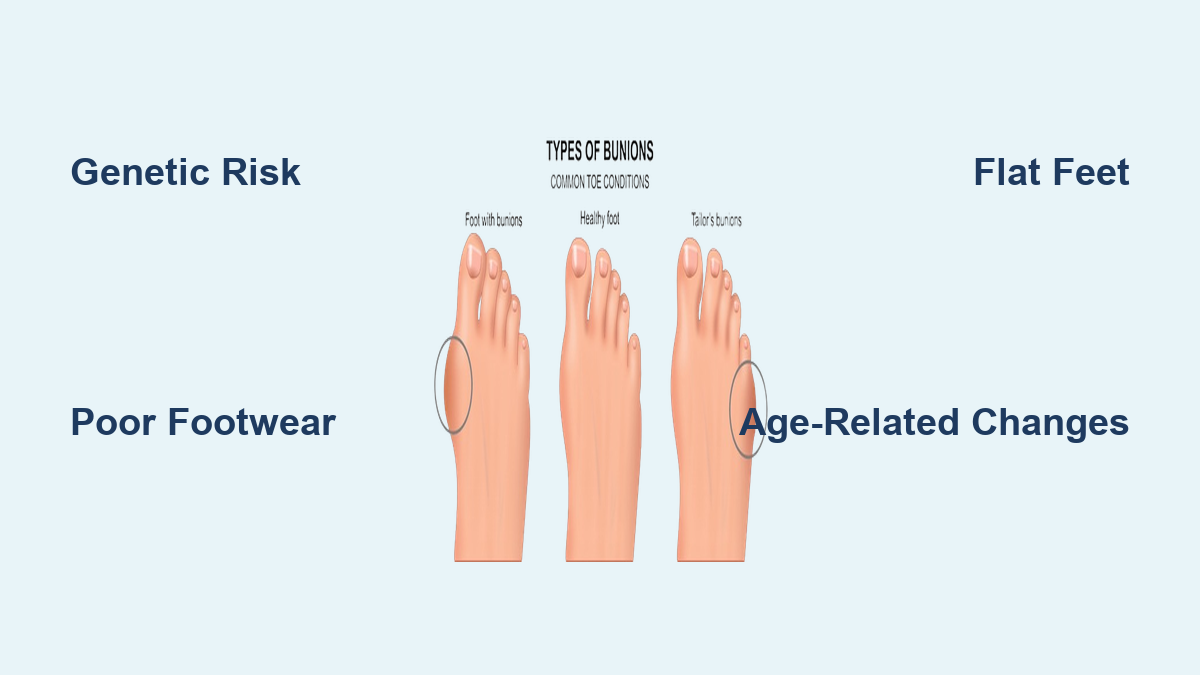
Bunion Types: Not All Bumps Are the Same
Bunions vary in location, cause, and age of onset. Recognizing the type helps determine the best treatment approach.
Hallux Valgus (Common Bunion)
This is the most frequent form, affecting the inner side of the big toe joint. The big toe gradually angles inward, sometimes overlapping or underlapping the second toe. As the joint protrudes, it becomes inflamed and painful, especially with pressure from shoes.
Bunionette (Tailor’s Bunion)
A smaller bump on the outside of the foot, at the base of the little toe. Like hallux valgus, it results from joint misalignment and is often worsened by tight shoes. The name “tailor’s bunion” comes from historical tailors who sat cross-legged, causing friction on the outer foot edge.
Juvenile and Congenital Bunions
- Juvenile bunions appear in children and teens, typically linked to inherited foot structure.
- Congenital bunions are rare and present at birth, caused by developmental abnormalities in bone alignment.
These early-onset forms can progress quickly during growth spurts and require early monitoring.
Who’s at Risk? Understanding Bunion Demographics
Bunions are surprisingly widespread, with research showing:
- One in three Americans has some degree of bunion deformity.
- 70% of cases have a family history, indicating strong genetic influence.
- Women are far more affected than men, largely due to footwear and hormonal joint laxity.
- Risk increases significantly after age 40, as feet naturally widen and ligaments loosen.
Even if you’re not in a high-risk group, certain traits make you more susceptible.
High-Risk Groups and Why They’re Vulnerable
| Group | Risk Factors |
|---|---|
| Women | High heels, narrow shoes, and estrogen-related joint flexibility increase vulnerability. |
| Adults over 40 | Age-related foot spreading and joint wear promote deformity. |
| People with flat feet | Overpronation shifts weight to the forefoot, straining the MTP joint. |
| Those with family history | Inherited foot structure sets the stage for misalignment. |
| Individuals with RA or neuromuscular disorders | Joint instability and muscle imbalances accelerate bunion formation. |
Early Warning Signs: How to Spot a Bunion
You don’t need an X-ray to suspect a bunion—your feet often give clear signals.
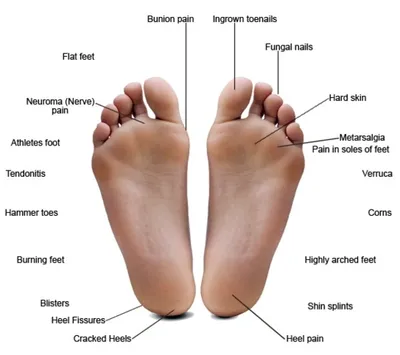
Visible and Physical Symptoms
- Hard bump on the side of the big toe joint
- Big toe leaning toward the second toe
- Redness, swelling, or warmth around the joint
- Pain when walking or wearing shoes
- Calluses or corns from toe rubbing
- Stiffness or limited motion in the big toe
- Numbness due to nerve compression
Pain often flares when wearing narrow or high-heeled shoes. Some people have large bunions with minimal pain, while others feel discomfort from minor misalignment.
When to See a Podiatrist
Seek professional help if you experience:
– Persistent toe or foot pain
– Difficulty finding comfortable shoes
– Reduced big toe mobility
– Signs of infection (redness, heat, pus)
– Early toe drift, especially with family history
Early diagnosis can help preserve joint function and delay or avoid surgery.
Genetic Causes: Why Bunions Run in Families

Genetics play a major role—about 70% of bunion cases have a family link.
Inherited Foot Traits That Increase Risk
- Flat feet (pes planus): Lack of arch causes overpronation, pushing the big toe outward.
- Hypermobility: Loose ligaments allow bones to shift easily.
- Long first metatarsal: A longer bone increases leverage and joint stress.
- Unstable midfoot joints: Weakness in the foot’s arch structure leads to collapse and toe drift.
Key Insight: You inherit the foot structure, not the bunion itself. If your parents had bunions, you likely inherited their foot mechanics—making prevention crucial.
Foot Mechanics: How Your Gait Fuels Bunion Development
Your walking pattern can silently contribute to bunion formation.
Overpronation and Its Role
When your foot rolls inward excessively during walking, it destabilizes the forefoot. This motion forces the big toe joint to bear more pressure, encouraging the first metatarsal to drift outward and the toe to angle inward.
Weak Foot Muscles
The small muscles in your feet help stabilize the toes. If they’re weak—often due to lifelong shoe use—the tendons pull unevenly, worsening toe misalignment.
High-Risk Activities
- Dancers, nurses, teachers, and retail workers who stand for hours
- Runners or athletes with repetitive forefoot loading
- People who walk barefoot on hard surfaces without natural foot strength
These activities amplify existing biomechanical flaws, accelerating bunion progression.
Footwear: How Shoes Make Bunions Worse
Shoes don’t cause bunions in healthy feet—but they’re powerful accelerants in genetically prone individuals.
High Heels and Narrow Toes
- High heels shift up to 75% more pressure to the ball of the foot.
- Pointed toe boxes squeeze toes together, forcing the big toe inward.
- Tight shoes create constant friction, inflaming the joint and speeding deformity.
Women who regularly wear high heels are three times more likely to develop bunions.
What to Avoid
- Heels higher than 1 inch (2.5 cm)
- Shoes with pinched or narrow toe boxes
- Slip-on flats or pumps with no arch support
- Ill-fitting footwear (too short or narrow)
Myth Busting: Shoes don’t cause bunions—they exacerbate them in genetically susceptible people.
Medical Conditions That Increase Bunion Risk
Certain health issues destabilize joints, making bunions more likely.
Rheumatoid Arthritis (RA)
RA attacks joint linings, weakening ligaments and cartilage. This leads to rapid joint collapse and severe bunions—even in younger patients.
Osteoarthritis
Develops secondarily in misaligned MTP joints. As cartilage wears down, pain and stiffness increase.
Neuromuscular Disorders
Conditions like Charcot-Marie-Tooth disease or cerebral palsy disrupt muscle balance, causing abnormal foot pressures.
Connective Tissue Diseases
- Lupus
- Ehlers-Danlos syndrome
These increase joint laxity, reducing stability in the foot’s arch and toes.
Injury and Trauma: Hidden Triggers for Bunions
A broken toe or ankle sprain might seem healed—but long-term effects can linger.
How Injuries Trigger Bunions
- Fractures in the midfoot or MTP joint alter bone alignment.
- Ligament damage reduces joint stability.
- Changed gait after injury shifts weight unevenly, increasing forefoot pressure.
Even minor trauma can set off a chain reaction, especially in those already at risk.
Hormonal and Age-Related Factors
Bunions become more common with age—and hormones may explain the gender gap.
Estrogen and Joint Laxity
Higher estrogen levels in women can relax ligaments, making joints more flexible and less stable. This increased mobility raises the risk of joint misalignment under mechanical stress.
Aging Feet
As we age:
– Ligaments weaken, allowing bones to shift
– Fat pads thin, reducing cushioning
– Feet widen and flatten, increasing pressure on the MTP joint
Weight Gain
Extra body weight increases load on the feet by up to 4x per step. In someone with flat feet or poor mechanics, this added pressure speeds up joint deterioration.
The 3D Deformity: How Bunions Actually Form

A bunion isn’t just a bump—it’s a complex, three-dimensional shift.
Step-by-Step Progression
- Joint instability: The first metatarsal bone begins to drift inward.
- Toe deviation: The big toe is pulled outward by tendons and pressure from adjacent toes.
- Bump formation: The metatarsal head becomes prominent.
- Soft tissue changes: Ligaments stretch on one side, tighten on the other.
- Angle widening: The intermetatarsal angle increases, worsening alignment.
This process can take years, often starting subtly in adolescence.
Complications of Untreated Bunions
Ignoring a bunion can lead to a cascade of foot problems.
Common Secondary Conditions
- Bursitis: Inflammation of the fluid sac over the joint.
- Hammertoes: The second toe buckles from crowding.
- Metatarsalgia: Pain under the ball of the foot.
- Osteoarthritis: Joint degeneration from years of misalignment.
- Corns and calluses: From constant friction.
- Gait changes: Altered walking patterns increase fall risk.
Even after surgery, up to 25% of patients develop a recurrence if underlying biomechanics aren’t corrected.
How Doctors Diagnose Bunions
Diagnosis starts with a physical exam but often includes imaging.
Clinical Evaluation
Doctors assess:
– Toe alignment while standing and walking
– Range of motion in the big toe
– Skin condition (calluses, redness)
– Foot posture (flat or high arch)
– Shoe wear patterns
X-Ray Assessment
Weight-bearing X-rays measure:
– Hallux valgus angle (HVA): Big toe deviation (normal <15°)
– Intermetatarsal angle (IMA): Spread between metatarsals (normal <9°)
These angles guide treatment decisions, including surgery.
Preventing Bunions: What Actually Works
You can’t change your genes—but you can change how they express.
Proven Prevention Strategies
- Wear wide-toe-box shoes: Let your toes spread naturally.
- Choose low or zero heels: Keep heel height under 1 inch.
- Use custom orthotics: Especially if you have flat feet.
- Strengthen foot muscles:
- Towel scrunches
- Marble pickups
- Toe spreads
- Arch lifts
- Walk barefoot (safely): Builds intrinsic foot strength.
- Buy shoes late in the day: Feet swell, ensuring a proper fit.
- Maintain a healthy weight: Reduces foot load.
Reality Check: No method guarantees prevention—but these steps can slow or stop progression in early stages.
Key Takeaways: What You Need to Know
- A bunion is a structural deformity, not just a bump.
- Genetics and foot mechanics are the root causes.
- Footwear worsens but doesn’t cause bunions in most cases.
- Women and older adults are at highest risk.
- Symptoms vary widely—some have pain, others don’t.
- Early intervention with shoes, orthotics, and exercises helps.
- Surgery corrects the deformity, but conservative care manages symptoms.
Understanding what causes bunions empowers you to take control. Whether you’re at risk or already seeing changes, the right choices today can protect your feet for years to come.