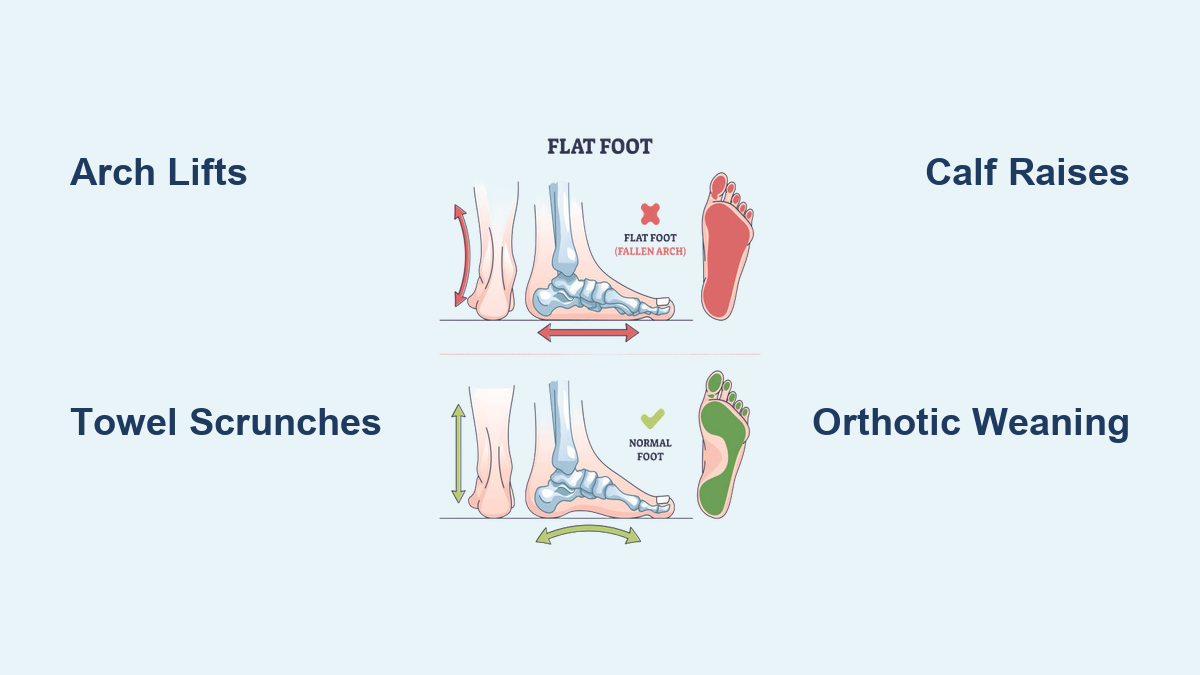
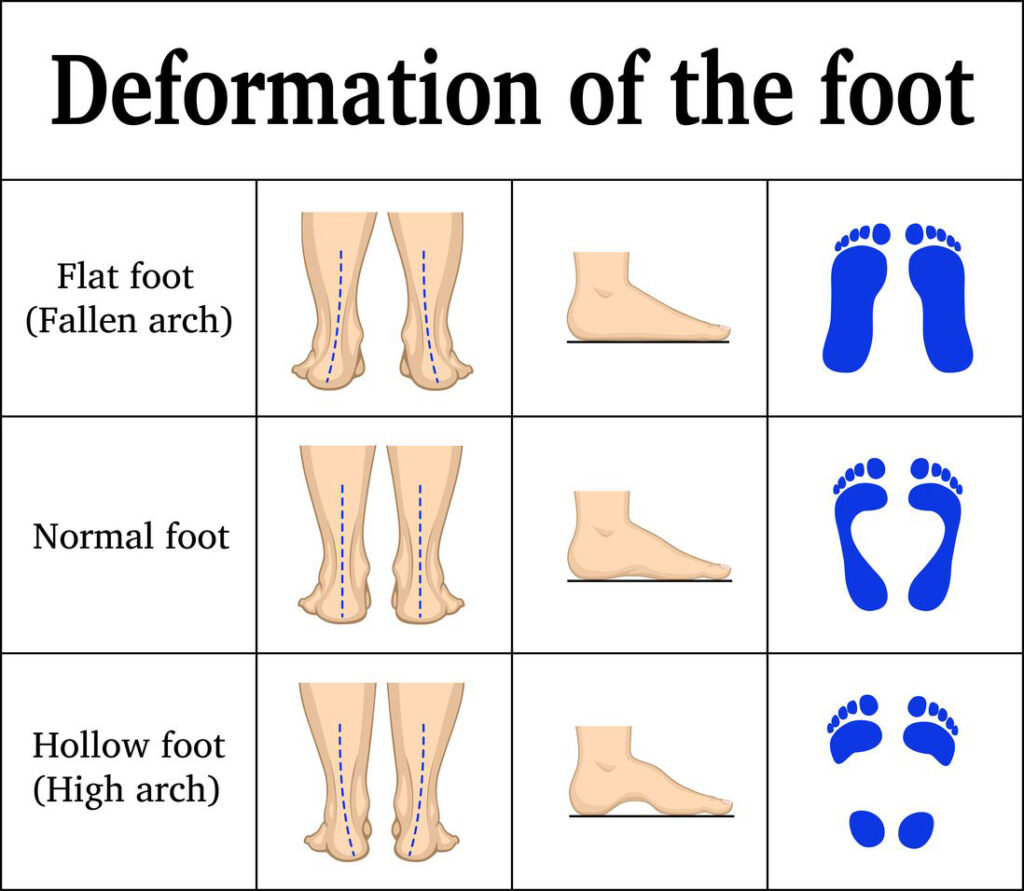
If you’ve noticed your feet flattening when you stand, or you’re experiencing unexplained foot, knee, or lower back pain, fallen arches—also known as flat feet or pes planus—could be the culprit. Affecting up to 14% of adults, this condition occurs when the medial longitudinal arch collapses, leading to overpronation, instability, and discomfort that can ripple up the body. The good news? Most cases—especially flexible flat feet—can be significantly improved with targeted exercises, proper supports, and lifestyle adjustments.
Unlike rigid structural deformities, flexible fallen arches respond well to neuromuscular retraining and strengthening of the foot’s intrinsic muscles and the posterior tibialis tendon, the body’s primary arch supporter. This guide delivers a science-backed, step-by-step approach to fix fallen arches using proven exercises, support strategies, and expert-recommended dos and don’ts. You’ll learn how to rebuild arch strength, reduce pain, and restore natural foot function—without surgery.
Identify Your Flat Foot Type Before Starting
Not all flat feet are the same, and your recovery path depends on whether your arch can still be restored through exercise.
Flexible vs. Rigid Flat Feet
- Flexible flat feet: The arch disappears when standing but reappears when sitting or rising onto your toes. This type responds best to exercise and is the most common form in adults.
- Rigid flat feet: No arch is visible, even when non-weight-bearing. Often caused by bone fusion or congenital issues. Less responsive to conservative care and may require medical evaluation.
Quick Test: Stand barefoot on a wet surface or place your foot on paper after wetting the sole. If the entire footprint is visible with no inward curve along the inside, you likely have flat feet.
Common Signs of Fallen Arches
- Foot fatigue after short walks
- Pain along the inner arch or heel
- Swelling near the ankle
- Shoes wearing out on the inner edge
- Knee or hip discomfort during activity
If you experience sudden arch collapse, sharp pain, or swelling, see a podiatrist. These could signal posterior tibial tendon dysfunction (PTTD), a progressive condition requiring early intervention.
Build Arch Strength With Proven Exercises
Exercises are the cornerstone of fixing fallen arches—especially for flexible cases. Done barefoot and consistently, these movements activate underused muscles, improve foot control, and reduce overpronation.
Always Perform Exercises Barefoot
Going barefoot enhances sensory feedback from the soles, boosting muscle activation. Start with 2–3 sessions per week, progressing to daily practice. Most people notice improvements in 6–12 weeks.
Arch Lifts (Short Foot Exercise)
Target: Intrinsic foot muscles, medial arch
This is the gold standard for rebuilding arch control. It strengthens the tiny muscles inside the foot that dynamically support the arch.
How to Do It:
- Sit or stand with feet flat, hip-width apart.
- Keep your heel and toes on the ground.
- Contract the foot to lift the arch, shortening the distance between heel and ball.
- Hold for 3–5 seconds, then release.
- Avoid curling your toes.
Sets & Reps:
- 2–3 sets of 10–15 reps
- Advanced: Work up to 60–80 reps daily
Pro Tip: Practice during daily activities—like standing in line or brushing your teeth.
Towel Scrunches
Target: Toe flexors, intrinsic foot muscles
Improves fine motor control and mimics the foot’s natural push-off during walking.
How to Do It:
- Sit with a towel under your bare foot.
- Use only your toes to pull the towel toward your heel.
- Keep your heel down.
Variations:
- Marble pickups: Pick up marbles with your toes and place them in a cup.
- Use a thicker towel or resistance band for progression.
Sets & Reps:
- 2–3 sets of 10–15 reps, or 1 minute per foot
Calf Raises
Target: Gastrocnemius, soleus, posterior tibialis
Strong calves support the rear of the arch and improve ankle stability.
How to Do It:
- Stand near a wall for balance.
- Rise onto your toes, lifting heels high.
- Hold for 5 seconds, then lower slowly (3–5 seconds down).
- Keep knees straight for gastrocnemius; slightly bent for soleus.
Progressions:
- Single-leg raises
- Step drops: Lower heels below step level for eccentric loading
Sets & Reps:
- 2–3 sets of 15–20 reps
- For tendon strength: 5 sets of 5 reps with 20-second holds
Key: Slow lowering builds tendon resilience and arch support.
Stair Arch Raises
Target: Posterior tibialis, dynamic arch control
Isolates the muscle that holds up the arch during walking.
How to Do It:
- Stand sideways on a step, one foot on the step, the other hanging off.
- Raise the heel of the lower foot while actively lifting and rotating the arch inward.
- Lower slowly.
Sets & Reps:
- 2–3 sets of 10–15 reps per side
Visual Cue: Imagine screwing your foot into the ground—heel down, arch lifting.
Ankle Inversion with Resistance Band
Target: Posterior tibialis
Directly strengthens the main arch stabilizer.
How to Do It:
- Loop a resistance band around the ball of your foot.
- Anchor the other end to a stable object.
- Sit with leg extended.
- Pull your foot inward (inversion) against the band’s pull.
Sets & Reps:
- 3 sets of 30 reps per foot
Progression: Perform standing for real-world carryover.
Standing Inversion
Target: Medial arch endurance
Builds sustained arch control during daily standing.
How to Do It:
- Stand with feet hip-width apart.
- Engage inner leg muscles to lift the arches slightly.
- Hold for 2–3 seconds, then relax.
- No visible foot roll needed—focus on muscle activation.
Reps:
- 60–80 times per day, spread across the day
Use It: Do reps while waiting, cooking, or talking on the phone.
Heel and Toe Walking
Target: Dynamic foot function, gait balance
Trains both push-off and foot clearance phases.
A. Toe Walking
- Rise onto tiptoes.
- Walk forward 10–20 steps.
- Builds calf and plantar fascia strength.
B. Heel Walking
- Lift toes, walk on heels.
- Strengthens shin muscles (tibialis anterior) to counteract overpronation.
Frequency:
- 2–3 rounds, 2–3 times per week
Surface Tip: Use carpet or mat if hard floors hurt.
Balance Training
Target: Proprioception, ankle stability
Improves foot control and reduces injury risk.
How to Do It:
- Stand on one foot for 20–30 seconds.
- Progress to eyes closed or foam pad.
Frequency:
- Daily, as part of warm-up or cooldown
Bonus: Try Tree Pose in yoga to combine balance and arch activation.
Supination Movement
Target: Push-off phase control
Advanced exercise for dynamic arch control.
How to Do It:
- Stand on one foot.
- Rise onto the ball of the foot.
- Rotate the heel inward (supination).
- Return slowly.
Sets & Reps:
- 3 sets of 10 reps, progress to 20–30
Warning: Only attempt after mastering foundational exercises.
Release and Relax: Foot and Calf Care
Stiff calves and tight plantar fascia can worsen fallen arches. But stretching the arch itself can increase instability—so focus on massage, not stretching.
Tennis or Golf Ball Rolls
Target: Plantar fascia, foot muscles
Releases tension and boosts sensory input.
How to Do It:
- Sit with a ball under your arch.
- Roll for 2–3 minutes, focusing on tender spots.
- Use a frozen ball for inflammation.
Frequency:
- Daily, especially before or after walking
Options: Lacrosse ball (deeper pressure), foam roller, vibrating massager.
Calf and Achilles Massage
Target: Gastrocnemius, soleus, Achilles
Tight calves pull the heel up, flattening the arch.
How to Do It:
- Use a foam roller or massage ball on calves.
- Or perform seated towel stretch: Loop towel around foot, gently pull toes toward you.
Hold:
- 30 seconds per leg, 4 sets
Avoid: Aggressive arch stretches—they may worsen ligament laxity.
Support Strategies: Orthotics and Footwear
Exercises are essential, but pairing them with proper support speeds recovery and reduces pain.
Use Orthotics Wisely

Purpose: Provide temporary alignment, shock absorption.
Types:
- OTC insoles: Affordable, good for mild symptoms.
- Custom orthotics: Tailored to your foot, prescribed by a podiatrist.
When to Use:
- For long walks or standing
- As a bridge while building strength
Critical Rule:
- Do not rely on orthotics long-term.
- Overuse weakens foot muscles.
- Wean off gradually as strength improves.
Dr. Michael Bogden, Cleveland Clinic: “Orthotics should not be relied on long-term. Use them as a bridge while building intrinsic strength—then gradually phase them out.”
Wear Proper Footwear

Your shoes can either support recovery or make it worse.
What to Look For:
- Wide toe box: Allows toes to splay, improving balance and arch function.
- Low heel-to-toe drop: Reduces calf tightness.
- Stability or motion-control shoes: Ideal for overpronators.
- Avoid: High heels, narrow shoes, flip-flops.
Recommended:
- Walking shoes with arch support
- Minimalist shoes (only after building strength)
- Hiking boots (for ankle support if needed)
Lifestyle and Activity Tips
Smart movement choices protect your feet and support healing.
Safe Aerobic Activities
- Swimming
- Cycling
- Rowing
- Elliptical training
These are low-impact and won’t overload your arches.
Walking Programs
- Start with 10–15 minutes on flat surfaces.
- Follow a Couch-to-5K or walk-to-run plan.
- Include recovery weeks.
Dr. Bogden: “Any increase in activity dramatically more than usual puts someone at risk for soreness, tightness, or injury.”
Avoid High-Impact Overload
- Running, jumping, basketball should be introduced slowly.
- Only start if you’re pain-free and have built foot strength.
What to Avoid With Fallen Arches
- ❌ Stretching the arch directly—may increase instability
- ❌ Overusing orthotics—leads to muscle dependency
- ❌ Narrow or high-heeled shoes—restrict natural foot motion
- ❌ Sudden increases in activity—risk of injury
- ❌ Ignoring pain—stop any exercise that causes sharp discomfort
When to See a Professional
Not all flat feet improve with home care. Seek help if:
– Pain persists after 8–12 weeks of exercise
– You have swelling, redness, or warmth (possible tendonitis)
– Your arch collapse is sudden or rigid
– You suspect PTTD or a structural issue
– You want custom orthotics or gait analysis
Surgery is rare and only considered for:
– Tendon tears
– Severe deformities
– Chronic, disabling pain
Expected Timeline and Realistic Goals
You won’t wake up with perfect arches—but you can expect real functional gains.
| Timeframe | What to Expect |
|---|---|
| 2–4 weeks | Better foot awareness, less fatigue |
| 6–12 weeks | Stronger arches, reduced pain, improved balance |
| 3–6 months | Less reliance on supports, better gait, increased endurance |
Reality Check: The goal isn’t a “perfect” arch—it’s less pain, better movement, and stronger feet.
Final Tips for Long-Term Success
- Strengthen, don’t stretch the foot.
- Go barefoot when safe—grass, sand, hardwood floors.
- Be consistent—3–5 days per week minimum.
- Combine foot work with balance and core training.
- Progress slowly—no aggressive loading.
- Listen to your body—pain means stop.
- Wean off supports as strength improves.
- Wear wide, low shoes that let your foot move naturally.
Equipment You’ll Need
| Item | Purpose |
|---|---|
| Chair | Support for seated or standing exercises |
| Tennis/golf ball | Foot massage and release |
| Towel | Towel scrunches, calf stretches |
| Marbles | Toe dexterity training |
| Step or stair | Calf and arch raises |
| Resistance band | Ankle strengthening |
| Foam pad | Balance training |
Bottom Line: You can fix fallen arches—not by relying on supports, but by activating and strengthening your foot’s natural architecture. With consistent exercise, smart footwear, and the right mindset, you can walk pain-free and build feet that are stronger than ever.